Abstract
Introduction
Lymphopenia has been correlated with poorer survival in patients with metastatic cancers treated with anti-PD-1 immunotherapy. Treatments such as chemotherapy, surgery or radiotherapy can induce lymphopenia. Radiation-induced lymphopenia is common and prolonged in head and neck cancer (HNSCC) patients. We evaluated the impact of lymphopenia, on efficacy of anti PD-1 nivolumab immunotherapy in HNSCC patients.
Methods
a multicenter retrospective study included consecutive patients treated with nivolumab for recurrent/metastatic (R/M) HNSCC between January 2017 and June 2019. Lymphopenia was defined as lymphocyte counts below 1000 cells/mm3 upon initiation of nivolumab. Logistical regression was performed on factors associated with lymphopenia and ROC analyses assessed association between lymphopenia and survival.
Results
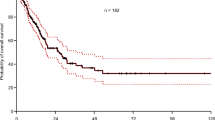
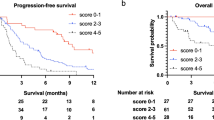
median age was 65. Of the 100 included patients, 60% had been treated by surgery, 67% had had first-line chemotherapy, and 89% loco-regional radiotherapy, 65% had concurrent chemotherapy with radiotherapy. Lymphopenia occurred in 56 (56%) patients upon initiation of nivolumab, with 29 (29%) patients having radiation-related lymphopenia. Prior locoregional radiotherapy was the only factor associated with lymphopenia upon initiation of nivolumab by logistical regression (OR 0.144 [0.029–0.706], p − 0.017). Lymphopenia upon initiation of nivolumab did not affect progression-free survival (PFS) (p − 0.815), overall survival (OS) (p − 0.783) or disease control rate (DCR) (p − 0.125). Locoregional symptomatology (HR − 2.37 [1.24–4.54], p − 0.009), metastatic symptomatology (HR − 4.74 [2.21–10.15], and persistent lymphopenia under nivolumab (HR 3.96 [1.19–13.17] p − 0.034) were associated with poorer OS in multivariate analysis.
Conclusions
Lymphopenia upon initiation of nivolumab was not associated with poorer survival in R/M HNSCC patients, but persistence of lymphopenia during immunotherapy might be a prognostic marker of patient survival.



Similar content being viewed by others
Data availability
The participants of this study did not give written consent for their data to be shared publicly, so due to the sensitive nature of the research supporting data is not available.
Abbreviations
- 5-FU:
-
5-Fluoro-uracile
- BMI:
-
Body mass index
- CPS:
-
Combined positive score
- DCR:
-
Disease control rate
- HNSCC:
-
Head and neck cancer
- ICI:
-
Immune check-point inhibitors
- NLR:
-
Neutrophil-to-lymphocyte ratio
- OS:
-
Overall survival
- PD-1:
-
Programmed cell death protein 1
- PD-L1:
-
Programmed cell death ligand 1
- PFS:
-
Progression-free survival
- R/M:
-
Recurrent/metastatic
- WHO:
-
World Health Organization
References
Defossez G, Le Guyader‑Peyrou S, Uhry Z,, Grosclaude P, Colonna M, Dantony E, et al (2019) Estimations nationales de l’incidence et de la mortalité par cancer en France métropolitaine entre 1990 et 2018. Volume 1 – Tumeurs solides. Saint‑Maurice (Fra) : Santé publique France, 2019. 372 p.
Pignon J-P, le Maître A, Maillard E et al (2009) Meta-analysis of chemotherapy in head and neck cancer (MACH-NC): an update on 93 randomised trials and 17,346 patients. Radiother Oncol J Eur Soc Ther Radiol Oncol 92:4–14. https://doi.org/10.1016/j.radonc.2009.04.014
Duprez F, Berwouts D, De Neve W et al (2017) Distant metastases in head and neck cancer. Head Neck 39:1733–1743. https://doi.org/10.1002/hed.24687
Topalian SL, Hodi FS, Brahmer JR et al (2012) Safety, activity, and immune correlates of anti-PD-1 antibody in cancer. N Engl J Med 366:2443–2454. https://doi.org/10.1056/NEJMoa1200690
Ferris RL, Blumenschein G, Fayette J et al (2016) Nivolumab for recurrent squamous-cell carcinoma of the head and neck. N Engl J Med 375:1856–1867. https://doi.org/10.1056/NEJMoa1602252
Burtness B, Harrington KJ, Greil R et al (2019) Pembrolizumab alone or with chemotherapy versus cetuximab with chemotherapy for recurrent or metastatic squamous cell carcinoma of the head and neck (KEYNOTE-048): a randomised, open-label, phase 3 study. Lancet Lond Engl 394:1915–1928. https://doi.org/10.1016/S0140-6736(19)32591-7
Psyrri A, Gavrielatou N, Spathis A et al (2019) Predictive biomarkers for response to nivolumab in head and neck squamous cell carcinoma (HNSCC) (NCT#03652142). J Clin Oncol 37:6060–6060. https://doi.org/10.1200/JCO.2019.37.15_suppl.6060
Ho WJ, Yarchoan M, Hopkins A et al (2018) Association between pretreatment lymphocyte count and response to PD1 inhibitors in head and neck squamous cell carcinomas. J Immunother Cancer 6:84. https://doi.org/10.1186/s40425-018-0395-x
Goodman AM, Kato S, Bazhenova L et al (2017) Tumor mutational burden as an independent predictor of response to immunotherapy in diverse cancers. Mol Cancer Ther 16:2598–2608. https://doi.org/10.1158/1535-7163.MCT-17-0386
Saâda-Bouzid E, Defaucheux C, Karabajakian A et al (2017) Hyperprogression during anti-PD-1/PD-L1 therapy in patients with recurrent and/or metastatic head and neck squamous cell carcinoma. Ann Oncol Off J Eur Soc Med Oncol 28:1605–1611. https://doi.org/10.1093/annonc/mdx178
Suzuki C, Kiyota N, Imamura Y et al (2020) Effect of tumor burden and growth rate on treatment outcomes of nivolumab in head and neck cancer. Int J Clin Oncol. https://doi.org/10.1007/s10147-020-01669-y
Campian JL, Sarai G, Ye X et al (2014) Association between severe treatment-related lymphopenia and progression-free survival in patients with newly diagnosed squamous cell head and neck cancer. Head Neck 36:1747–1753. https://doi.org/10.1002/hed.23535
Lin AJ, Rao YJ, Chin R-I et al (2018) Post-operative radiation effects on lymphopenia, neutrophil to lymphocyte ratio, and clinical outcomes in palatine tonsil cancers. Oral Oncol 86:1–7. https://doi.org/10.1016/j.oraloncology.2018.08.008
Dai D, Tian Q, Shui Y et al (2022) The impact of radiation induced lymphopenia in the prognosis of head and neck cancer: a systematic review and meta-analysis. Radiother Oncol J Eur Soc Ther Radiol Oncol 168:28–36. https://doi.org/10.1016/j.radonc.2022.01.003
Verastegui EL, Morales RB, Barrera-Franco JL et al (2003) Long-term immune dysfunction after radiotherapy to the head and neck area. Int Immunopharmacol 3:1093–1104. https://doi.org/10.1016/S1567-5769(03)00013-4
Sun R, Champiat S, Dercle L et al (1990) 2017) Baseline lymphopenia should not be used as exclusion criteria in early clinical trials investigating immune checkpoint blockers (PD-1/PD-L1 inhibitors. Eur J Cancer Oxf Engl 84:202–211. https://doi.org/10.1016/j.ejca.2017.07.033
Capone M, Giannarelli D, Mallardo D et al (2018) Baseline neutrophil-to-lymphocyte ratio (NLR) and derived NLR could predict overall survival in patients with advanced melanoma treated with nivolumab. J Immunother Cancer 6:74. https://doi.org/10.1186/s40425-018-0383-1
Park JC, Durbeck J, Clark JR (2020) Predictive value of peripheral lymphocyte counts for immune checkpoint inhibitor efficacy in advanced head and neck squamous cell carcinoma. Mol Clin Oncol 13:87. https://doi.org/10.3892/mco.2020.2157
Diehl A, Yarchoan M, Hopkins A et al (2017) Relationships between lymphocyte counts and treatment-related toxicities and clinical responses in patients with solid tumors treated with PD-1 checkpoint inhibitors. Oncotarget 8:114268–114280. https://doi.org/10.18632/oncotarget.23217
Campian JL, Ye X, Brock M, Grossman SA (2013) Treatment-related lymphopenia in patients with stage III non-small-cell lung cancer. Cancer Invest 31:183–188. https://doi.org/10.3109/07357907.2013.767342
Sfikakis PP, Gourgoulis GM, Moulopoulos LA et al (2005) Age-related thymic activity in adults following chemotherapy-induced lymphopenia. Eur J Clin Invest 35:380–387. https://doi.org/10.1111/j.1365-2362.2005.01499.x
Kumar BV, Connors T, Farber DL (2018) Human T cell development, localization, and function throughout life. Immunity 48:202–213. https://doi.org/10.1016/j.immuni.2018.01.007
Cho Y, Kim JW, Yoon HI et al (2018) The prognostic significance of neutrophil-to-lymphocyte ratio in head and neck cancer patients treated with radiotherapy. J Clin Med. https://doi.org/10.3390/jcm7120512
Péron J, Cropet C, Tredan O et al (1990) (2013) CD4 lymphopenia to identify end-of-life metastatic cancer patients. Eur J Cancer Oxf Engl 49:1080–1089. https://doi.org/10.1016/j.ejca.2012.11.003
Eberst G, Vernerey D, Laheurte C et al (2022) Prognostic value of CD4+ T lymphopenia in non-small cell lung Cancer. BMC Cancer 22:529. https://doi.org/10.1186/s12885-022-09628-8
Ray-Coquard I, Cropet C, Van Glabbeke M et al (2009) Lymphopenia as a prognostic factor for overall survival in advanced carcinomas, sarcomas, and lymphomas. Cancer Res 69:5383–5391. https://doi.org/10.1158/0008-5472.CAN-08-3845
Takenaka Y, Oya R, Takemoto N, Inohara H (2022) Neutrophil-to-lymphocyte ratio as a prognostic marker for head and neck squamous cell carcinoma treated with immune checkpoint inhibitors: Meta-analysis. Head Neck 44:1237–1245. https://doi.org/10.1002/hed.26997
Balázs K, Kis E, Badie C et al (2019) Radiotherapy-induced changes in the systemic immune and inflammation parameters of head and neck cancer patients. Cancers. https://doi.org/10.3390/cancers11091324
Oliva M, Spreafico A, Taberna M et al (2019) Immune biomarkers of response to immune-checkpoint inhibitors in head and neck squamous cell carcinoma. Ann Oncol Off J Eur Soc Med Oncol 30:57–67. https://doi.org/10.1093/annonc/mdy507
Hanna GJ, Lizotte P, Cavanaugh M et al (2018) Frameshift events predict anti-PD-1/L1 response in head and neck cancer. JCI Insight. https://doi.org/10.1172/jci.insight.98811
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declared no conflicts of interest.
Ethical approval
Our study has received the approval of the CNIL and the Ethics Committee of the François Baclesse Center. A non-opposition briefing note for patients living at the time of inclusion was issued to the various participating centers.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Césaire, M., Rambeau, A., Clatot, F. et al. Impact of lymphopenia on efficacy of nivolumab in head and neck cancer patients. Eur Arch Otorhinolaryngol 280, 2453–2461 (2023). https://doi.org/10.1007/s00405-022-07800-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-022-07800-1