Abstract
Introduction
Mobile-bearing unicompartmental knee arthroplasty (UKA) was designed so that flexion and extension gap adjustments could achieve isometric function of the ligaments throughout ROM to prevent complications. However, achieving accurate knee balancing using a spacer block technique remains difficult since determination of the thickness of the spacer block is determined according to the feeling of the individual surgeon’s hand. The objective of the study was to investigate flexion and extension medial unicompartmental knee gap kinematics in mobile-bearing UKA and to reveal the accuracy of spacer block measurement technique using a gap tensor device.
Materials and methods
Mobile-bearing UKA was performed in 40 knees of 31 subjects using generally accepted spacer block technique so that the extension gap was made equal to the flexion gap. The extension and flexion gaps of the medial knee compartment were measured using the tensor device with 25, 50, 75, 100, 125, and 150 N of joint distraction force. The interplay gap was calculated by subtracting the thickness of the tibial prosthesis and the thickness of the selected size of bearing from the measured extension and flexion gaps. Medial compartmental joint interplay gap differences were compared among flexion and extension gaps.
Results
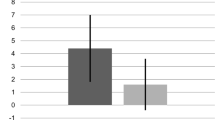
The mean flexion interplay gap was 25 N: 0.5 mm, 50 N: 1.5 mm, 75 N: 2.4 mm, 100 N: 3.1 mm, 125 N: 3.6 mm, 150 N: 4.0 mm. The mean extension interplay gap was 25 N: −0.2 mm, 50 N: 0.81 mm, 75 N: 1.7 mm, 100 N: 2.5 mm, 125 N: 3.1 mm, 150 N: 3.5 mm. The measured extension gap was shown to be significantly smaller compared with the flexion gap at every joint distraction force (P < 0.01).
Conclusions
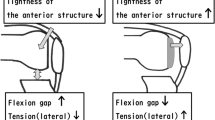
These results suggest that gap measurement using a spacer block in UKA has the potential risk that the resulting extension gap may be smaller than the flexion gap. Surgeons should adjust the flexion and extension gaps with caution to achieve good ligament function when performing mobile-bearing UKA.




Similar content being viewed by others
References
Asano H, Hoshino A, Wilton TJ (2004) Soft-tissue tension total knee arthroplasty. J Arthroplast 19(5):558–561
Asano H, Muneta T, Sekiya I (2008) Soft tissue tension in extension in total knee arthroplasty affects postoperative knee extension and stability. Knee Surg Sports Traumatol Arthrosc 16(11):999–1003
Attfield SF, Warren-Forward M, Wilton T, Sambatakakis A (1994) Measurement of soft tissue imbalance in total knee arthroplasty using electronic instrumentation. Med Eng Phys 16(6):501–505
Dorr LD, Boiardo RA (1986) Technical considerations in total knee arthroplasty. Clin Orthop Relat Res 205:5–11
Gleeson RE, Evans R, Ackroyd CE, Webb J, Newman JH (2004) Fixed or mobile bearing unicompartmental knee replacement? A comparative cohort study. Knee 11(5):379–384
Hananouchi T, Yamamoto K, Ando W, Fudo K, Ohzono K (2012) The intraoperative gap difference (flexion gap minus extension gap) is altered by insertion of the trial femoral component. Knee 19(5):601–605
Insall JN, Binazzi R, Soudry M, Mestriner LA (1985) Total knee arthroplasty. Clin Orthop Relat Res 192:13–22
Kellgren JH, Lawrence JS (1957) Radiological assessment of osteo-arthrosis. Ann Rheum Dis 16(4):494–502
Krackow KA, Mihalko WM (1999) The effect of medial release on flexion and extension gaps in cadaveric knees: implications for soft-tissue balancing in total knee arthroplasty. Am J Knee Surg 12(4):222–228
Matsumoto T, Mizuno K, Muratsu H, Tsumura N, Fukase N, Kubo S, Yoshiya S, Kurosaka M, Kuroda R (2007) Influence of intra-operative joint gap on post-operative flexion angle in osteoarthritis patients undergoing posterior-stabilized total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 15(8):1013–1018
Matsumoto T, Muratsu H, Kubo S, Kuroda R, Kurosaka M (2013) Intra-operative joint gap kinematics in unicompartmental knee arthroplasty. Clin Biomech (Bristol, Avon) 28(1):29–33
Matsumoto T, Muratsu H, Kubo S, Matsushita T, Kurosaka M, Kuroda R (2012) Intraoperative soft tissue balance reflects minimum 5-year midterm outcomes in cruciate-retaining and posterior-stabilized total knee arthroplasty. J Arthroplast 27(9):1723–1730
Muratsu H, Matsumoto T, Kubo S, Maruo A, Miya H, Kurosaka M, Kuroda R (2010) Femoral component placement changes soft tissue balance in posterior-stabilized total knee arthroplasty. Clin Biomech (Bristol, Avon) 25(9):926–930
O’Connor JJ, Goodfellow JW (1996) Theory and practice of meniscal knee replacement: designing against wear. Proc Inst Mech Eng H 210(3):217–222
O’Connor JJ, Shercliff TL, Biden E, Goodfellow JW (1989) The geometry of the knee in the sagittal plane. Proc Inst Mech Eng H 203(4):223–233
Okamoto S, Okazaki K, Mitsuyasu H, Matsuda S, Mizu-Uchi H, Hamai S, Tashiro Y, Iwamoto Y (2014) Extension gap needs more than 1-mm laxity after implantation to avoid post-operative flexion contracture in total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 22(12):3174–3180
Pandit H, Jenkins C, Gill HS, Barker K, Dodd CA, Murray DW (2011) Minimally invasive Oxford phase 3 unicompartmental knee replacement: results of 1000 cases. J Bone Joint Surg Br 93(2):198–204
Pang HN, Yeo SJ, Chong HC, Chin PL, Ong J, Lo NN (2011) Computer-assisted gap balancing technique improves outcome in total knee arthroplasty, compared with conventional measured resection technique. Knee Surg Sports Traumatol Arthrosc 19(9):1496–1503
Parmaksizoglu AS, Kabukcuoglu Y, Ozkaya U, Bilgili F, Aslan A (2010) Short-term results of the Oxford phase 3 unicompartmental knee arthroplasty for medial arthritis. Acta Orthop Traumatol Turc 44(2):135–142
Price AJ, O’Connor JJ, Murray DW, Dodd CA, Goodfellow JW (2007) A history of Oxford unicompartmental knee arthroplasty. Orthopedics 30(5 Suppl):7–10
Price AJ, Svard U (2011) A second decade lifetable survival analysis of the Oxford unicompartmental knee arthroplasty. Clin Orthop Relat Res 469(1):174–179
Sambatakakis A, Attfield SF, Newton G (1993) Quantification of soft-tissue imbalance in condylar knee arthroplasty. J Biomed Eng 15(4):339–343
Svard UC, Price AJ (2001) Oxford medial unicompartmental knee arthroplasty. A survival analysis of an independent series. J Bone Joint Surg Br 83(2):191–194
Ten Ham AM, Heesterbeek PJ, van der Schaaf DB, Jacobs WC, Wymenga AB (2013) Flexion and extension laxity after medial, mobile-bearing unicompartmental knee arthroplasty: a comparison between a spacer- and a tension-guided technique. Knee Surg Sports Traumatol Arthrosc 21(11):2447–2452
Unitt L, Sambatakakis A, Johnstone D, Briggs TW (2008) Short-term outcome in total knee replacement after soft-tissue release and balancing. J Bone Joint Surg Br 90(2):159–165
Watanabe T, Muneta T, Sekiya I, Banks SA (2013) Intraoperative joint gaps affect postoperative range of motion in TKAs With posterior-stabilized prostheses. Clin Orthop Relat Res 471(4):1326–1333
Whiteside LA, Saeki K, Mihalko WM (2000) Functional medical ligament balancing in total knee arthroplasty. Clin Orthop Relat Res 380:45–57
Winemaker MJ (2002) Perfect balance in total knee arthroplasty: the elusive compromise. J Arthroplasty 17(1):2–10
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Suzuki, T., Ryu, K., Kojima, K. et al. Evaluation of spacer block technique using tensor device in unicompartmental knee arthroplasty. Arch Orthop Trauma Surg 135, 1011–1016 (2015). https://doi.org/10.1007/s00402-015-2231-9
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-015-2231-9