Abstract
Background
Some indications for revision total knee arthroplasty (TKA), e.g. arthrofibrosis, have been identified to yield inferior results. The aim of this study was to analyse the results of revision TKA according to aetiology of TKA failure.
Patients and methods
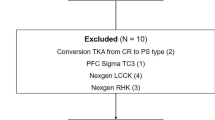
The results of 97 consecutive revision TKA in 97 patients stratified according to the aetiology of primary TKA failure (periprosthetic infection, aseptic loosening, instability and arthrofibrosis), were compared using the Knee Society Score (KSS). The effect of patient age, gender, BMI, American Society of Anesthesiologists (ASA) classification, interval to revision and the occurrence of complications on the outcome were also analysed.
Results
After a mean follow-up of 29 months, the KSS had significantly improved in all patient groups (p < 0.001). The analysis of variance among patient groups depicted no significant differences between preoperative KSS (p = 0.618) and postoperative KSS (p = 0.915), while the magnitude of pre- to postoperative improvement showed significant differences between the groups (p = 0.006). The aetiology of primary TKA failure had an independent influence on pre- to postoperative improvement (p = 0.014). Of the other factors analysed, only the ASA classification had an independent impact on postoperative KSS (p = 0.045).
Conclusion
The aetiology of TKA failure has an effect on the improvement in knee function from revision TKA. As no difference was observed between patient groups postoperatively, similar clinical results can be expected independent of the aetiology of primary TKA failure.
Similar content being viewed by others
References
Emmerson KP, Moran CG, Pinder IM (1996) Survivorship analysis of the Kinematic Stabilizer total knee replacement: a 10- to 14-year follow-up. J Bone Joint Surg Br 78:441–445
Baker P, Cowling P, Kurtz S, Jameson S, Gregg P, Deehan D (2012) Reason for revision influences early patient outcomes after aseptic knee revision. Clin Orthop Relat Res. doi:10.1007/s11999-012-2278-7
Greidanus NV, Peterson RC, Masri BA, Garbuz DS (2010) Quality of life outcomes in revision versus primary total knee arthroplasty. J Arthroplasty. doi:10.1016/j.arth.2010.04.026
Saleh KJ, Rand JA, McQueen DA (2003) Current status of revision total knee arthroplasty: how do we assess results? J Bone Joint Surg Am A 85(Suppl 1):S18–S20
Callaghan JJ, O’Rourke MR, Saleh KJ (2004) Why knees fail: lessons learned. J Arthroplasty 19:31–34 [Pii] S0883540304001330
Jacobs MA, Hungerford DS, Krackow KA, Lennox DW (1988) Revision total knee arthroplasty for aseptic failure. Clin Orthop Relat Res 226:78–85
Lidgren L, Robertson O, Dahl A (2009) The Swedish National Knee Arthroplasty Register: annual report 2009. Lund University Hospital
Meek RM, Dunlop D, Garbuz DS, McGraw R, Greidanus NV, Masri BA (2004) Patient satisfaction and functional status after aseptic versus septic revision total knee arthroplasty using the PROSTALAC articulating spacer. J Arthroplasty 19:874–879 [Pii] S0883540304003493
Barrack RL, Engh G, Rorabeck C, Sawhney J, Woolfrey M (2000) Patient satisfaction and outcome after septic versus aseptic revision total knee arthroplasty. J Arthroplasty 15:990–993. doi:10.1054/arth.2000.16504
Ghanem E, Restrepo C, Joshi A, Hozack W, Sharkey P, Parvizi J (2007) Periprosthetic infection does not preclude good outcome for revision arthroplasty. Clin Orthop Relat Res 461:54–59. doi:10.1097/BLO.0b013e318073c246
Pun SY, Ries MD (2008) Effect of gender and preoperative diagnosis on results of revision total knee arthroplasty. Clin Orthop Relat Res 466:2701–2705. doi:10.1007/s11999-008-0451-9
Hardeman F, Londers J, Favril A, Witvrouw E, Bellemans J, Victor J (2012) Predisposing factors which are relevant for the clinical outcome after revision total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc Off J ESSKA 20:1049–1056. doi:10.1007/s00167-011-1624-8
Malviya A, Brewster NT, Bettinson K, Holland JP, Weir DJ, Deehan DJ (2011) Functional outcome following aseptic single-stage revision knee arthroplasty. Knee Surg Sports Traumatol Arthrosc Off J ESSKA. doi:10.1007/s00167-011-1786-4
Haidukewych GJ, Jacofsky DJ, Pagnano MW, Trousdale RT (2005) Functional results after revision of well-fixed components for stiffness after primary total knee arthroplasty. J Arthroplasty 20:133–138
Ritter MA, Eizember LE, Fechtman RW, Keating EM, Faris PM (1991) Revision total knee arthroplasty. A survival analysis. J Arthroplasty 6:351–356
Saleh KJ, Dykes DC, Tweedie RL, Mohamed K, Ravichandran A, Saleh RM, Gioe TJ, Heck DA (2002) Functional outcome after total knee arthroplasty revision: a meta-analysis. J Arthroplasty 17:967–977. doi:10.1054/arth.2002.35823
Dahm DL, Barnes SA, Harrington JR, Berry DJ (2007) Patient reported activity after revision total knee arthroplasty. J Arthroplasty 22:106–110. doi:10.1016/j.arth.2007.03.030
Singh JA, Gabriel SE, Lewallen DG (2011) Higher body mass index is not associated with worse pain outcomes after primary or revision total knee arthroplasty. J Arthroplasty 26(3):366–374. doi: 10.1016/j.arth.2010.02.006
Ritter MA, Berend ME, Harty LD, Davis KE, Meding JB, Keating EM (2004) Predicting range of motion after revision total knee arthroplasty: clustering and log-linear regression analyses. J Arthroplasty 19:338–343 [Pii] S0883540303005783
Singh JA, O’Byrne MM, Harmsen WS, Lewallen DG (2010) Predictors of moderate–severe functional limitation 2 and 5 years after revision total knee arthroplasty. J Arthroplasty 25:1091–1095, 1095, e1091–1094. doi: 10.1016/j.arth.2009.07.020
Callaghan JJ, O’Rourke MR, Liu SS (2005) The role of implant constraint in revision total knee arthroplasty: not too little, not too much. J Arthroplasty 20:41–43. doi:S0883540305001580
Vince KG (2003) Why knees fail. J Arthroplasty 18:39–44. doi:10.1054/arth.2003.50102
Suarez J, Griffin W, Springer B, Fehring T, Mason JB, Odum S (2008) Why do revision knee arthroplasties fail? J Arthroplasty 23:99–103. doi:10.1016/j.arth.2008.04.020
Patil N, Lee K, Huddleston JI, Harris AH, Goodman SB Aseptic versus septic revision total knee arthroplasty: patient satisfaction, outcome and quality of life improvement. Knee 17:200–203. doi: 10.1016/j.knee.2009.09.001
Peters CL, Erickson JA, Gililland JM (2009) Clinical and radiographic results of 184 consecutive revision total knee arthroplasties placed with modular cementless stems. J Arthroplasty 24:48–53. doi:10.1016/j.arth.2009.04.033
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bieger, R., Kappe, T., Fraitzl, C.R. et al. The aetiology of total knee arthroplasty failure influences the improvement in knee function. Arch Orthop Trauma Surg 133, 237–241 (2013). https://doi.org/10.1007/s00402-012-1647-8
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-012-1647-8