Abstract
Introduction
In sepsis, severe reduction of afterload may often mask cardiac impairment. By establishing the parameter “afterload-related cardiac performance (ACP)” we wanted to determine the extent, frequency, and prognostic relevance of septic cardiomyopathy.
Methods
Over a 12 months period, all patients of our medical intensive care ward were included into the study when they were classified as having “septic MODS” (sepsis score ≥12 as long as APACHE II score was ≥20). Hemodynamic assessments were performed using a pulmonary artery catheter.
Results
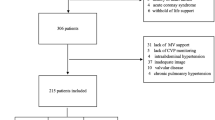
A total of 524 patients were screened, and from these 39 had septic MODS. In survivors, APACHE II score values declined from day 0 (day of diagnosis, 27.6 ± 8.0) to day 4 (17.8 ± 8.0), while in non-survivors, score values remained high (day 0: 31.8 ± 5.7; day 4: 33.2 ± 6.7; p < 0.001). Hemodynamic measurements showed an inverse correlation of cardiac output (COmeasured) and SVR which can be described as CO = β 0 × SVRβ1. The upper limit of 80% tolerance range of CO was defined as the “normal” CO values (COnormal). The parameter “afterload-related cardiac performance (ACP)” was calculated as ACP (%) = COmeasured/COnormal × 100. It turned out that ACP shows a stronger correlation with APACHE II- and sepsis-score than CO, cardiac index (CI), cardiac power (CPO), or cardiac power index (CPI). Furthermore, ACP correlated with sepsis-induced myocardial damage as indicated by elevations of troponin I and significantly differed between surviving (86.9 ± 1.6%) and non-surviving patients (69.2 ± 1.4%; p < 0.0001). While 75% of the surviving patients showed an ACP >60%, 38% of the non-survivors had a moderate (ACP 40–60%) and 25% a severe impairment of cardiac function (ACP < 40%).
Conclusion
By using the parameter “afterload-related cardiac performance, ACP”, the impairment of cardiac function can be reliably quantified showing that septic cardiomyopathy occurs frequently and is of prognostic relevance in patients with septic MODS.





Similar content being viewed by others
References
Reinhart K, Brunkhorst F, Bone Hg et al (2006) Diagnose und Therapie der Sepsis. Clin Res Cardiol 95:429–454
Parrillo Je (1989) The cardiovascular pathophysiology of sepsis. Ann Rev Med 40:469–485
Werdan K, Schmidt H, Ebelt H et al (2009) Impaired regulation of cardiac function in sepsis, SIRS, and MODS. Can J Physiol Pharmacol 87:266–274
Kindermann M, Seeland U, Ruhnke P (2010) Functional effects of beta(1)-adrenoceptor polymorphisms on the hemodynamic response to dobutamine with and without beta-blocker administration. Clin Res Cardiol. doi:10.1007/s00392-00010-00221-z
Vieillard-Baron A, Prin S, Chergui K et al (2003) Hemodynamic instability in sepsis: bedside assessment by Doppler echocardiography. Am J Respir Crit Care Med 168:1270–1276
Elebute Ea, Stoner Hb (1983) The grading of sepsis. Br J Surg 70:29–31
Werdan K, Pilz G, Bujdoso O et al (2007) Score-based immunoglobulin G therapy of patients with sepsis: the SBITS study. Crit Care Med 35:2693–2701
Elliott P, Andersson B, Arbustini E et al (2008) Classification of the cardiomyopathies: a position statement from the European Society Of Cardiology Working Group on Myocardial and Pericardial Diseases. Eur Heart J 29:270–276
Bouhemad B, Nicolas-Robin A, Arbelot C et al (2009) Acute left ventricular dilatation and shock-induced myocardial dysfunction. Crit Care Med 37:441–447
Merx Mw, Weber C (2007) Sepsis and the heart. Circulation 116:793–802
Werdan K, Muller-Werdan U (1996) Elucidating molecular mechanisms of septic cardiomyopathy–the cardiomyocyte model. Mol Cell Biochem 163–164:291–303
Zorn-Pauly K, Pelzmann B, Lang P et al (2007) Endotoxin impairs the human pacemaker current If. Shock 28:655–661
Fincke R, Hochman Js, Lowe Am et al (2004) Cardiac power is the strongest hemodynamic correlate of mortality in cardiogenic shock: a report from the SHOCK trial registry. J Am Coll Cardiol 44:340–348
Pilz G, Mcginn P, Boekstegers P et al (1994) Pseudomonas sepsis does not cause more severe cardiovascular dysfunction in patients than non-Pseudomonas sepsis. Circ Shock 42:174–182
Levy Rj, Piel Da, Acton Pd et al (2005) Evidence of myocardial hibernation in the septic heart. Crit Care Med 33:2752–2756
Spies C, Haude V, Fitzner R et al (1998) Serum cardiac troponin T as a prognostic marker in early sepsis. Chest 113:1055–1063
Wu Ah (2001) Increased troponin in patients with sepsis and septic shock: myocardial necrosis or reversible myocardial depression? Intensive Care Med 27:959–961
Brueckmann M, Huhle G, Lang S et al (2005) Prognostic value of plasma N-terminal pro-brain natriuretic peptide in patients with severe sepsis. Circulation 112:527–534
Charpentier J, Luyt Ce, Fulla Y et al (2004) Brain natriuretic peptide: a marker of myocardial dysfunction and prognosis during severe sepsis. Crit Care Med 32:660–665
Witthaut R, Busch C, Fraunberger P et al (2003) Plasma atrial natriuretic peptide and brain natriuretic peptide are increased in septic shock: impact of interleukin-6 and sepsis-associated left ventricular dysfunction. Intensive Care Med 29:1696–1702
Mclean As (1996) Echocardiography assessment of left ventricular function in the critically ill. Anaesth Intensive Care 24:60–65
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Werdan, K., Oelke, A., Hettwer, S. et al. Septic cardiomyopathy: hemodynamic quantification, occurrence, and prognostic implications. Clin Res Cardiol 100, 661–668 (2011). https://doi.org/10.1007/s00392-011-0292-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00392-011-0292-5