Abstract
Purpose
Cerebrospinal fluid (CSF) hypoglycorrhachia and elevated protein is well-described in bacterial meningitis, but evidence for its differential diagnostic value in tuberculous meningitis (TBM) is lacking. We aimed to assess the diagnostic utility of CSF glucose, CSF to serum glucose ratio and CSF protein in children with suspected TBM.
Methods
We describe CSF glucose and protein values as well as CSF to serum glucose ratios in a prospective evaluation of TBM suspects seen at Tygerberg Children’s Hospital, Cape Town, South Africa, from January 1985 to January 2014.
Results
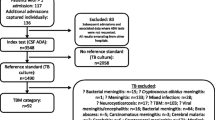
Of 615 TBM suspects, 88 (14 %) had microbiologically confirmed TBM, 381 (62 %) ‘probable’ TBM and 146 (24 %) ‘non-TBM’. Mean absolute CSF glucose concentration was significantly lower in the microbiologically confirmed (1.87 ± 1.15 mmol/L) and ‘probable’ TBM (1.82 ± 1.19 mmol/L) groups compared to non-TBM (3.66 ± 0.88 mmol/L). A CSF glucose concentration of <2.2 mmol/L diagnosed TBM with sensitivity 0.68 and specificity 0.96. Sensitivity using a CSF to serum glucose ratio of <0.5 was 0.90. Mean CSF protein was significantly elevated in the microbiologically confirmed TBM (1.91 ± 1.44 g/L) and ‘probable’ TBM (2.01 ± 1.49 g/L) groups compared to the non-TBM (0.31 ± 0.31 g/L). A CSF protein >1 g/L diagnosed TBM with sensitivity 0.78 and specificity 0.94.
Conclusion
Absolute CSF glucose values of <2.2 mmol/L and protein values of >1 g/L differentiated between TBM and non-bacterial meningitis with good specificity, although sensitivity was poor. A CSF to serum glucose ratio is more informative than the absolute value.

Similar content being viewed by others
References
World Health Organization (2013) Global tuberculosis report, Geneva. http://apps.who.int/iris/bitstream/10665/91355/1/9789241564656_eng.pdf. Accessed 6 Oct 2014
Rock RB, Olin M, Baker CA, Molitor TW, Peterson PK (2008) Central nervous system tuberculosis: pathogenesis and clinical aspects. Clin Microbiol Rev 21:243–261
Thwaites G, Chau TTH, Mai NTH, Drobniewski F, McAdam K, Farrar J (2000) Tuberculous meningitis. J Neurol Neurosurg Psychiatry 68:289–299
Jönsson B, Ridell M (2003) The Cobas Amplicor MTB test for detection of Mycobacterium tuberculosis complex from respiratory and non-respiratory clinical specimens. Scand J Infect Dis 35(6-7):372–377
Hosoglu S, Geyik MF, Balik I et al (2002) Predictors of outcome in patients with tuberculous meningitis. Int J Tuberc Lung Dis 6(1):64–70
Solomons RS, van Elsland SL, Visser DH et al (2014) Commercial nucleic acid amplification tests in tuberculous meningitis—a meta-analysis. Diagn Microbiol Infect Dis 78(4):398–403
Thwaites G, Fisher M, Hemingway C, Scott G, Solomon T, Innes J (2009) British Infection Society guidelines for the diagnosis of tuberculosis of the central nervous system in adults and children. J Infect 59:167–187
Torok ME, Chau TTH, Mai PP et al (2008) Clinical and microbiological features of HIV-associated tuberculous meningitis in Vietnamese adults. PLoS ONE 3(3), e1772
van Well GT, Paes BF, Terwee CB et al (2009) Twenty years of pediatric tuberculous meningitis: a retrospective cohort study in the western cape of South Africa. Pediatrics 123(1):1–8
Youssef FG, Afifi SA, Azab AM et al (2006) Differentiation of tuberculous meningitis from acute bacterial meningitis using simple clinical and laboratory parameters. Diagn Microbiol Infect Dis 55(4):275–278
Cecchini D, Ambrosioni J, Brezzo C et al (2009) Tuberculous meningitis in HIV-infected and non-infected patients: comparison of cerebrospinal fluid findings. Int J Tuberc Lung Dis 13(2):269–271
Griggs RC, Jozefowicz RF, Aminoff MJ (2011) Approach to the patient with neurologic disease. In: Goldman L, Schafer AI (eds) Goldman’s Cecil medicine, 24th edn. Elsevier Saunders, Philadelphia, chapter 403, pp 2228–2235
Prober CG, Dyner L (2011) Central nervous system infections. In: Kliegman RM, Stanton BF, Gemelli JWS, Schor NF (eds) Nelson textbook of pediatrics, 19th edn. Elsevier Saunders, Philadelphia, chapter 595, pp 2086–2097
Swaiman KF, Ashwal S (2011) Pediatric neurology: principles and practice, 5th edn. Elsevier Saunders, Philadelphia
Rosenberg GA (2012) Brain edema and disorders of cerebrospinal fluid circulation. In: Daroff RB, Fenichel GM, Jankovic J, Mazziotta JC (eds) Bradley’s neurology in clinical practice, 6th edn. Elsevier Saunders, Philadelphia, chapter 59, pp 1377–1395
Silver TS, Todd JK (1976) Hypoglycorrhachia in pediatric patients. Pediatrics 58(1):67–71
Donald PR, Malan C, van der Walt A (1983) Simultaneous determination of cerebrospinal fluid glucose and blood glucose concentrations in the diagnosis of bacterial meningitis. J Pediatr 103(3):413–415
Hristea A, Olaru ID, Baicus C, Moroti R, Arama V, Ion M (2012) Clinical prediction rule for differentiating tuberculous from viral meningitis. Int J Tuberc Lung Dis 16(6):793–798
Marais S, Thwaites G, Schoeman JF et al (2010) Tuberculous meningitis: a uniform case definition for use in clinical research. Lancet Infect Dis 10(11):803–812
Solomons RS, Wessels M, Visser DH et al (2014) Uniform research case definition criteria differentiate tuberculous and bacterial meningitis in children. Clin Infect Dis. doi:10.1093/cid/ciu781
British Medical Research Council (1948) Streptomycin treatment of tuberculous meningitis. Br Med J 1(6503):582–596
van Toorn R, Springer P, Laubscher JA, Schoeman JF (2012) Value of different staging systems for predicting neurological outcome in childhood tuberculous meningitis. Int J Tuberc Lung Dis 16(5):628–632
van Toorn R, Schaaf HS, Laubscher JA, van Elsland SL, Donald PR, Schoeman JF (2014) Short intensified treatment in children with drug-susceptible tuberculous meningitis. Pediatr Infect Dis J 33(3):248–252
Huy NT, Thao NT, Diep DT, Kikuchi M, Zamora J, Hirayama K (2010) Cerebrospinal fluid lactate concentration to distinguish bacterial from aseptic meningitis: a systemic review and meta-analysis. Crit Care 14(6):R240
Thwaites GE, Simmons CP, Than Ha Quyen N et al (2003) Pathophysiology and prognosis in Vietnamese adults with tuberculous meningitis. J Infect Dis 188(8):1105–1115
Ho J, Marais BJ, Gilbert GL, Ralph AP (2013) Diagnosing tuberculous meningitis—have we made any progress? Trop Med Int Health 18(6):783–793
Metcalfe JZ, Everett CK, Steingart KR et al (2011) Interferon-gamma release assays for active pulmonary tuberculosis diagnosis in adults in low- and middle-income countries: systematic review and meta-analysis. J Infect Dis 204(S4):S1120–S1129
Kim SH, Cho OH, Park SJ et al (2010) Rapid diagnosis of tuberculous meningitis by T cell-based assays on peripheral blood and cerebrospinal fluid mononuclear cells. Clin Infect Dis 50:1349–1358
Patel VB, Singh R, Connolly C et al (2010) Cerebrospinal T-cell responses aid in the diagnosis of tuberculous meningitis in a human immunodeficiency virus- and tuberculosis-endemic population. Am J Respir Crit Care Med 182:569–577
Vidhate MR, Singh MK, Garg RK et al (2011) Diagnostic and prognostic value of Mycobacterium tuberculosis complex specific interferon gamma release assay in patients with tuberculous meningitis. J Infect 62:400–403
Park KH, Cho OH, Lee EM et al (2012) T-cell-based assays on cerebrospinal fluid and PBMCs for rapid diagnosis of TB meningitis in non-HIV patients. Eur Respir J 39:768–770
Thwaites GE (2013) Advances in the diagnosis and treatment of tuberculous meningitis. Curr Opin Neurol 26(3):295–300
van Toorn R, Solomons R (2014) Update on the diagnosis and management of tuberculous meningitis in children. Semin Pediatr Neurol 21(1):12–18
Visser DH, Solomons RS, Ronacher K et al (2015) Host immune response to tuberculous meningitis. Clin Infect Dis. doi:10.1093/cid/ciu781
Marais S, Wilkinson KA, Lesosky M et al (2014) Neutrophil-associated central nervous system inflammation in tuberculous meningitis immune reconstitution inflammatory syndrome. Clin Infect Dis. doi:10.1093/cid/ciu641
Karande S, Gupta V, Kulkarni M, Joshi A, Rele M (2005) Tuberculous meningitis and HIV. Indian J Pediatr 72(9):755–760
Funding
This study was supported by a Vrije University-National Research Foundation Desmond Tutu Phd scholarship.
Conflict of interest
The authors declare that they have no competing interests.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Solomons, R.S., Visser, D.H., Donald, P.R. et al. The diagnostic value of cerebrospinal fluid chemistry results in childhood tuberculous meningitis. Childs Nerv Syst 31, 1335–1340 (2015). https://doi.org/10.1007/s00381-015-2745-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-015-2745-z