Abstract
Objective
To determine whether radiomics analysis of pericoronary adipose tissue (PCAT) captured by coronary computed tomography angiography (CCTA) could discriminate acute myocardial infarction (MI) from unstable angina (UA).
Methods
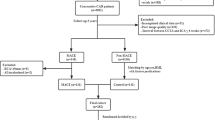
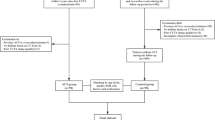
In a single-center retrospective case-control study, patients with acute MI (n = 105) were matched to patients with UA (n = 105) and all patients were randomly divided into training and validation cohorts with a ratio of 7:3. Fat attenuation index (FAI) and PCAT radiomics features selected by Max-Relevance and Min-Redundancy (mRMR) and least absolute shrinkage and selection operator (LASSO) around the proximal three major epicardial coronary vessels (LAD [left anterior descending artery], LCx [left circumflex artery], and RCA [right coronary artery]) were used to build logistic regression models. Finally, a FAI model, three radiomics models of PCAT (LAD, LCx, and RCA), and a combined model that used the scores of these independent models were constructed. The performance of the models was evaluated by identification, calibration, and clinical application.
Results
In training and validation cohorts, compared with the FAI model (AUC = 0.53, 0.50), the combined model achieved superior performance (AUC = 0.97, 0.95) while there was a significant difference of AUC between two models (p < 0.05). The calibration curves of the combined model demonstrated the smallest Brier score loss. Decision curve analysis suggested that the combined model provided higher clinical benefit than the FAI model.
Conclusions
The CCTA–based radiomics phenotype of PCAT outperforms the FAI model in discriminating acute MI from UA. The combination of PCAT radiomics and FAI could further enhance the performance of acute MI identification.
Key Points
• Fat attenuation index based on CCTA can detect inflammation-induced changes in the ratio of lipid to aqueous phase in pericoronary adipose tissue.
• Fat attenuation index cannot distinguish acute MI patients from UA patients, suggesting that the two groups have the same degree of ratio of lipid to aqueous phase in pericoronary adipose tissue.
• Radiomics features of PCAT have the potential to distinguish acute MI patients from UA patients.






Similar content being viewed by others
Abbreviations
- ACE-I:
-
Angiotensin-converting enzyme inhibitor
- ACS:
-
Acute coronary syndrome
- ARB:
-
Angiotensin receptor blocker
- BMI:
-
Body mass index
- BP:
-
Blood pressure
- CAD:
-
Coronary artery disease
- CCTA:
-
Coronary computed tomography angiography
- DLP:
-
Dose-length product
- ECG:
-
Electrocardiogram
- FAI:
-
Fat attenuation index
- HDL:
-
High-density lipoprotein
- HIS:
-
Hospital information system
- LAD:
-
Left anterior descending artery
- LASSO:
-
Least absolute shrinkage and selection operator
- LCx:
-
Left circumflex artery
- LDL:
-
Low-density lipoprotein
- MI:
-
Myocardial infarction
- mRMR:
-
Max-Relevance and Min-Redundancy
- PCAT:
-
Pericoronary adipose tissue
- RCA:
-
Right coronary artery
- UA:
-
Unstable angina
References
Timmis A, Townsend N, Gale C et al (2018) European Society of Cardiology: cardiovascular disease statistics 2017. Eur Heart J 39:508–579
Benjamin EJ, Virani SS, Callaway CW et al (2018) Heart disease and stroke statistics-2018 update: a report from the American Heart Association. Circulation 137:e67–e492
Koskinas KC, Ughi GJ, Windecker S, Tearney GJ, Räber L (2016) Intracoronary imaging of coronary atherosclerosis: validation for diagnosis, prognosis and treatment. Eur Heart J 37:524–535a-c
Douglas PS, Hoffmann U, Patel MR et al (2015) Outcomes of anatomical versus functional testing for coronary artery disease. N Engl J Med 372:1291–1300
SCOT-HEART investigators. (2015) CT coronary angiography in patients with suspected angina due to coronary heart disease (SCOT-HEART): an open-label, parallel-group, multicentre trial. Lancet 385:2383–2391
Greenland P, LaBree L, Azen SP, Doherty TM, Detrano RC (2004) Coronary artery calcium score combined with Framingham score for risk prediction in asymptomatic individuals. JAMA 291:210–215
Cury RC, Abbara S, Achenbach S et al (2016) CAD-RADS™: coronary artery disease - reporting and data system: an expert consensus document of the Society of Cardiovascular Computed Tomography (SCCT), the American College of Radiology (ACR) and the North American Society for Cardiovascular Imaging (NASCI). Endorsed by the American College of Cardiology. J Am Coll Radiol 13:1458–1466.e1459
Momiyama Y, Adachi H, Fairweather D, Ishizaka N, Saita E (2014) Inflammation, atherosclerosis and coronary artery disease. Clin Med Insights Cardiol 8:67–70
Joshi NV, Vesey AT, Williams MC et al (2014) 18F-fluoride positron emission tomography for identification of ruptured and high-risk coronary atherosclerotic plaques: a prospective clinical trial. Lancet 383:705–713
Popescu BA, Petersen SE, Maurovich-Horvat P et al (2018) The year 2017 in the European Heart Journal-Cardiovascular Imaging: Part I. Eur Heart J Cardiovasc Imaging 19:1099–1106
Camici PG, Rimoldi OE, Gaemperli O, Libby P (2012) Non-invasive anatomic and functional imaging of vascular inflammation and unstable plaque. Eur Heart J 33:1309–1317
Antonopoulos AS, Sanna F, Sabharwal N et al (2017) Detecting human coronary inflammation by imaging perivascular fat. Sci Transl Med 9:eaal2658
Margaritis M, Antonopoulos AS, Digby J et al (2013) Interactions between vascular wall and perivascular adipose tissue reveal novel roles for adiponectin in the regulation of endothelial nitric oxide synthase function in human vessels. Circulation 127:2209–2221
Antonopoulos AS, Margaritis M, Coutinho P et al (2015) Adiponectin as a link between type 2 diabetes and vascular NADPH oxidase activity in the human arterial wall: the regulatory role of perivascular adipose tissue. Diabetes 64:2207–2219
Lin A, Nerlekar N, Yuvaraj J et al (2021) Pericoronary adipose tissue computed tomography attenuation distinguishes different stages of coronary artery disease: a cross-sectional study. Eur Heart J Cardiovasc Imaging 22:298–306
Oikonomou EK, Antoniades C (2019) The role of adipose tissue in cardiovascular health and disease. Nat Rev Cardiol 16:83–99
Crewe C, An YA, Scherer PE (2017) The ominous triad of adipose tissue dysfunction: inflammation, fibrosis, and impaired angiogenesis. J Clin Invest 127:74–82
Gillies RJ, Kinahan PE, Hricak H (2016) Radiomics: images are more than pictures, they are data. Radiology 278:563–577
Aerts HJ, Velazquez ER, Leijenaar RT et al (2014) Decoding tumour phenotype by noninvasive imaging using a quantitative radiomics approach. Nat Commun 5:4006
Kolossváry M, Karády J, Kikuchi Y et al (2019) Radiomics versus visual and histogram-based assessment to identify atheromatous lesions at coronary CT angiography: an ex vivo study. Radiology 293:89–96
Oikonomou EK, Williams MC, Kotanidis CP et al (2019) A novel machine learning-derived radiotranscriptomic signature of perivascular fat improves cardiac risk prediction using coronary CT angiography. Eur Heart J 40:3529–3543
Lin A, Kolossváry M, Yuvaraj J et al (2020) Myocardial infarction associates with a distinct pericoronary adipose tissue radiomic phenotype: a prospective case-control study. JACC Cardiovasc Imaging 13:2371–2383
Thygesen K, Alpert JS, Jaffe AS et al (2018) Fourth universal definition of myocardial infarction (2018). J Am Coll Cardiol 72:2231–2264
Collet JP, Thiele H, Barbato E et al (2021) 2020 ESC guidelines for the management of acute coronary syndromes in patients presenting without persistent ST segment elevation. Eur Heart J 42:1289–1367
Oikonomou EK, Marwan M, Desai MY et al (2018) Non-invasive detection of coronary inflammation using computed tomography and prediction of residual cardiovascular risk (the CRISP CT study): a post-hoc analysis of prospective outcome data. Lancet 392:929–939
Segmentation of CT thoracic organs by multi-resolution VB-nets (2019) Challenge on Segmentation of Thoracic Organs at Risk in CT Images, France. Available via http://ceur-ws.org/Vol-2349/SegTHOR2019_paper_1.pdf. Accessed 23 Apr 2019
Yao L, Jiang P, Xue Z et al (2020) Machine learning in medical imaging. Springer, Berlin Heidelberg
Zhao Z, Anand R, Wang M (2019) 2019 IEEE International Conference on Data Science and Advanced Analytics (DSAA). IEEE, Washington, DC
Yang L, Gu D, Wei J et al (2019) A radiomics nomogram for preoperative prediction of microvascular invasion in hepatocellular carcinoma. Liver Cancer 8:373–386
Libby P (2012) Inflammation in atherosclerosis. Arterioscler Thromb Vasc Biol 32:2045–2051
Kolossváry M, Kellermayer M, Merkely B, Maurovich-Horvat P (2018) Cardiac computed tomography radiomics: a comprehensive review on radiomic techniques. J Thorac Imaging 33:26–34
Mauriello A, Sangiorgi G, Fratoni S et al (2005) Diffuse and active inflammation occurs in both vulnerable and stable plaques of the entire coronary tree: a histopathologic study of patients dying of acute myocardial infarction. J Am Coll Cardiol 45:1585–1593
Kubo T, Imanishi T, Kashiwagi M et al (2010) Multiple coronary lesion instability in patients with acute myocardial infarction as determined by optical coherence tomography. Am J Cardiol 105:318–322
Asakura M, Ueda Y, Yamaguchi O et al (2001) Extensive development of vulnerable plaques as a pan-coronary process in patients with myocardial infarction: an angioscopic study. J Am Coll Cardiol 37:1284–1288
Shang J, Ma S, Guo Y et al (2021) Prediction of acute coronary syndrome within 3 years using radiomics signature of pericoronary adipose tissue based on coronary computed tomography angiography. Eur Radiol. https://doi.org/10.1007/s00330-021-08109-z
Acknowledgements
Thanks to **g**g Cui and Fan Yang for their help in the processing of PCAT segmentation and radiomics feature extraction.
Funding
The authors state that this work has not received any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Tong Zhang.
Conflict of interest
Two of the authors of this manuscript (Yan Guo, Jiesi Hu) are employees of GE Healthcare. Two of the authors of this manuscript (**g**g Cui, Fan Yang) are employees of Shanghai United Imaging Intelligence, Co., Ltd. The remaining authors declare no relationships with any companies whose products or services may be related to the subject matter of the article.
Statistics and biometry
Yan Guo and Jiesi Hu kindly provided statistical advice for this manuscript.
Informed consent
Written informed consent was obtained from all subjects (patients) in this study.
Ethical approval
Institutional Review Board approval was obtained.
Methodology
• retrospective
• case-control study
• performed at one institution
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 686 kb)
Rights and permissions
About this article
Cite this article
Si, N., Shi, K., Li, N. et al. Identification of patients with acute myocardial infarction based on coronary CT angiography: the value of pericoronary adipose tissue radiomics. Eur Radiol 32, 6868–6877 (2022). https://doi.org/10.1007/s00330-022-08812-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-022-08812-5