Abstract
Objectives
To identify the CT features in differentiating grade 3 neuroendocrine carcinomas from grade 1/2 neuroendocrine tumours.
Methods
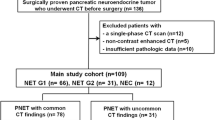
This study included 161 patients with surgically confirmed pancreatic neuroendocrine neoplasms. Pathology slides were reviewed to determine the tumour grade. CT image analysis included size, pattern, calcification, margin, pancreatic duct dilatation, bile duct dilatation, vascular invasion, arterial enhancement ratio, and portal enhancement ratio. We used 2 cm, 3 cm, and 4 cm as cutoff values of tumour size and 0.9 and 1.1 of enhancement ratio to determine the sensitivity and specificity.
Results
Pathology analysis identified 167 lesions in 161 patients. 154 lesions (92 %) were grade 1/2 and 13 (8 %) were grade 3. Portal enhancement ratio (< 1.1) showed high sensitivity and specificity 92.3 % and 80.5 %, respectively in differentiating grade 3 from grade 1/2. It showed the highest odds ratio (49.60), followed by poorly defined margin, size (> 3 cm), bile duct dilatation, and vascular invasion. When at least two of these five criteria were used in combination, the sensitivity and specificity for diagnosing grade 3 were 92.3 % (12/13) and 87.7 % (135/154), respectively.
Conclusions
By using specific CT findings, grade 3 can be differentiated from grade 1/2 with a high diagnostic accuracy leading to an appropriate imaging staging.
Key points
• Neuroendocrine carcinomas should be differentiated from neuroendocrine tumours.
• Neuroendocrine carcinomas can be differentiated from neuroendocrine tumours on dynamic CT.
• Neuroendocrine carcinomas show iso- or hypo-enhancement on portal venous phase CT.






Similar content being viewed by others
Abbreviations
- PanNEN:
-
Pancreatic neuroendocrine neoplasm
- NET:
-
Neuroendocrine tumour
- NEC:
-
Neuroendocrine carcinoma
- G1:
-
Grade 1
- G2:
-
Grade 2
- G3:
-
Grade 3
- ROI:
-
region of interest
- WHO:
-
World Health Organization
- HU:
-
Hounsfield unit
- MVD:
-
Microvascular density
References
Ramage JK, Ahmed A, Ardill J et al (2012) Guidelines for the management of gastroenteropancreatic neuroendocrine (including carcinoid) tumours (NETs). Gut 61:6–32
Kim KW, Krajewski KM, Nishino M et al (2013) Update on the management of gastroenteropancreatic neuroendocrine tumors with emphasis on the role of imaging. AJR 201:811–824
Bosman FT, Carneiro F, Hruban RH, Theise ND (2010) WHO classification of tumours of the digestive system, 4th edn. International Agency for Research on Cancer, Lyon
Kulke MH, Shah MH, Benson Al B, et al. (2014) NCCN guidelines Neuroendocrine tumors version 2. Accessed March, 2014
Horton KM, Hruban RH, Yeo C, Fishman EK (2006) Multi–detector row CT of pancreatic islet cell tumors1. Radiographics 26:453–464
Gore RM, Levine MS. (2008) Textbook of gastrointestinal radiology volume 2 Saunders, Philadelphia
Lu DS, Reber HA, Krasny RM, Kadell BM, Sayre J (1997) Local staging of pancreatic cancer: criteria for unresectability of major vessels as revealed by pancreatic-phase, thin-section helical CT. AJR 168:1439–1443
Rindi G (2010) The ENETS guidelines: the new TNM classification system. Tumori 96:806–809
Baron RL (1994) Understanding and optimizing use of contrast material for CT of the liver. AJR 163:323–331
Kim JH, Park SH, Yu ES et al (2010) Visually isoattenuating pancreatic adenocarcinoma at dynamic-enhanced CT: frequency, clinical and pathologic characteristics, and diagnosis at imaging examinations. Radiology 257:87–96
Rodallec M, Vilgrain V, Couvelard A et al (2006) Endocrine pancreatic tumours and helical CT: contrast enhancement is correlated with microvascular density, histoprognostic factors and survival. Pancreatology 6:77–85
d’Assignies G, Couvelard A, Bahrami S et al (2009) Pancreatic endocrine tumors: tumor blood flow assessed with perfusion CT reflects angiogenesis and correlates with prognostic factors. Radiology 250:407–416
Manfredi R, Bonatti M, Mantovani W et al (2013) Non-hyperfunctioning neuroendocrine tumours of the pancreas: MR imaging appearance and correlation with their biological behaviour. Eur Radiol 23:3029–3039
Ellis LM, Takahashi Y, Fenoglio CJ, Cleary KR, Bucana CD, Evans DB (1998) Vessel counts and vascular endothelial growth factor expression in pancreatic adenocarcinoma. Eur J Cancer 34:337–340
Duarte IG, Bufkin BL, Pennington MF et al (1998) Angiogenesis as a predictor of survival after surgical resection for stage I non-small-cell lung cancer. J Thorac Cardiovasc Surg 115:652–658
Vermeulen PB, Verhoeven D, Hubens G et al (1995) Microvessel density, endothelial cell proliferation and tumour cell proliferation in human colorectal adenocarcinomas. Ann Oncol 6:59–64
Weidner N, Folkman J, Pozza F et al (1992) Tumor angiogenesis: a new significant and independent prognostic indicator in early-stage breast carcinoma. J Natl Cancer Inst 84:1875–1887
Marion-Audibert AM, Barel C, Gouysse G et al (2003) Low microvessel density is an unfavorable histoprognostic factor in pancreatic endocrine tumors. Gastroenterology 125:1094–1104
Dong M, Phan AT, Yao JC (2012) New strategies for advanced neuroendocrine tumors in the era of targeted therapy. Clin Cancer Res 18:1830–1836
Bae KT (2010) Intravenous contrast medium administration and scan timing at CT: considerations and approaches. Radiology 256:32–61
Kawamoto S, Johnson PT, Shi C et al (2013) Pancreatic neuroendocrine tumor with cystlike changes: evaluation with MDCT. AJR 200:W283–W290
Singhi AD, Chu LC, Tatsas AD et al (2012) Cystic pancreatic neuroendocrine tumors: a clinicopathologic study. Am J Surg Pathol 36:1666–1673
Rha SE, Jung SE, Lee KH, Ku YM, Byun JY, Lee JM (2007) CT and MR imaging findings of endocrine tumor of the pancreas according to WHO classification. Eur J Radiol 62:371–377
Noone TC, Hosey J, Firat Z, Semelka RC (2005) Imaging and localization of islet-cell tumours of the pancreas on CT and MRI. Best Pract Res Clin Endocrinol Metab 19:195–211
Panzuto F, Merola E, Rinzivillo M et al (2014) Advanced digestive neuroendocrine tumors: metastatic pattern is an independent factor affecting clinical outcome. Pancreas 43:212–218
d’Assignies G, Fina P, Bruno O et al (2013) High sensitivity of diffusion-weighted MR imaging for the detection of liver metastases from neuroendocrine tumors: comparison with T2-weighted and dynamic gadolinium-enhanced MR imaging. Radiology 268:390–399
Sutcliffe R, Maguire D, Ramage J, Rela M, Heaton N (2004) Management of neuroendocrine liver metastases. Am J Surg 187:39–46
Acknowledgments
The scientific guarantor of this publication is Hyoung Jung Kim. The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article. The authors state that this work has not received any funding. No complex statistical methods were necessary for this paper. Institutional Review Board approval was obtained. Written informed consent was waived by the Institutional Review Board. Methodology: retrospective, observational, performed at one institution.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kim, D.W., Kim, H.J., Kim, K.W. et al. Neuroendocrine neoplasms of the pancreas at dynamic enhanced CT: comparison between grade 3 neuroendocrine carcinoma and grade 1/2 neuroendocrine tumour. Eur Radiol 25, 1375–1383 (2015). https://doi.org/10.1007/s00330-014-3532-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-014-3532-z