Abstract
Objectives
To retrospectively evaluate the ability of multiparametric magnetic resonance (MR) imaging to differentiate renal tumours.
Methods
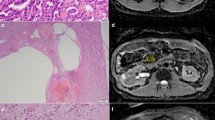
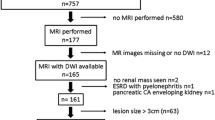
MR images from 100 consecutive pathologically proven solid renal tumours without macroscopic fat [57 clear cell, 16 papillary and 7 chromophobe renal cell carcinomas (RCCs), 16 oncocytomas and 4 minimal fat angiomyolipomas (AMLs)] between 2009 and 2012 were evaluated. Two radiologists blinded to pathology results independently reviewed double-echo chemical shift, dynamic contrast-enhanced T1- and T2-weighted images and apparent diffusion coefficient (ADC) maps. Signal intensity index (SII), tumour-to-spleen SI ratio (TSR), ADC ratio, wash-in (WiI) and wash-out indices (WoI) between different phases were calculated.
Results
There were significant differences between papillary RCCs and other renal tumours for arterial WiI (P < 0.001), initial WoI (P = 0.006) and ADC ratio (P < 0.001); between chromophobe RCCs and oncocytomas for TSR (P = 0.02), parenchymal WiI (P = 0.03), late WiI (P = 0.02), initial WoI (P = 0.03) and late WoI (P = 0.04); and between clear cell RCCs and oncocytomas for SII (P = 0.01) and parenchymal WiI (P = 0.01). Papillary RCCs were distinguished from other tumours (sensitivity 37.5 %, specificity 100 %) and oncocytomas from chromophobe RCCs (sensitivity 25 %, specificity 100 %) and clear cell RCCs (sensitivity 100 %, specificity 94.2 %).
Conclusion
MR imaging provides criteria able to accurately distinguish papillary RCCs from other tumours and oncocytomas from chromophobe and clear cell RCCs.
Key Points
• Multiparametric MR parameters accurately distinguish papillary RCCs with high specificity (100 %).
• Oncocytomas can be distinguished from chromophobe RCCs with high specificity (100 %).
• Oncocytomas can be distinguished from clear cell RCCs with high specificity (94.2 %).
• In oncocytomatosis, imaging follow-up with such parameters analysis could be promoted.





Similar content being viewed by others
Abbreviations
- ADC:
-
Apparent diffusion coefficient
- au:
-
Arbitrary units
- CT:
-
Computed tomography
- DCE:
-
Dynamic contrast-enhanced
- Gd:
-
Gadolinium
- GE:
-
Gradient echo
- mpMRI:
-
Multiparametric magnetic resonance imaging
- MR:
-
Magnetic resonance
- RCC:
-
Renal cell carcinoma
- ROC:
-
Receiver operating characteristic
- ROI:
-
Region of interest
- SII:
-
Signal intensity index
- SIR:
-
Signal intensity ratio
- TSR:
-
Tumor-to-spleen ratio
- WiI:
-
Wash-in index
- WoI:
-
Wash-out index
References
Lechevallier E, Andre M, Barriol D et al (2000) Fine-needle percutaneous biopsy of renal masses with helical CT guidance. Radiology 216:506–510
Eshed I, Elias S, Sidi AA (2004) Diagnostic value of CT-guided biopsy of indeterminate renal masses. Clin Radiol 59:262–267
Fujii Y, Komai Y, Saito K et al (2008) Incidence of benign pathologic lesions at partial nephrectomy for presumed RCC renal masses: Japanese dual-center experience with 176 consecutive patients. Urology 72:598–602
Snyder ME, Bach A, Kattan MW, Raj GV, Reuter VE, Russo P (2006) Incidence of benign lesions for clinically localized renal masses smaller than 7 cm in radiological diameter: influence of sex. J Urol 176:2391–2395
Breda A, Treat EG, Haft-Candell L et al (2010) Comparison of accuracy of 14-, 18- and 20-G needles in ex-vivo renal mass biopsy: a prospective, blinded study. BJU Int 105:940–945
Herts BR, Baker ME (1995) The current role of percutaneous biopsy in the evaluation of renal masses. Semin Urol Oncol 13:254–261
Heilbrun ME, Zagoria RJ, Garvin AJ et al (2007) CT-guided biopsy for the diagnosis of renal tumors before treatment with percutaneous ablation. AJR 188:1500–1505
Milner J, McNeil B, Alioto J et al (2006) Fat poor renal angiomyolipoma: patient, computerized tomography and histological findings. J Urol 176:905–909
Bosniak MA, Megibow AJ, Hulnick DH, Horii S, Raghavendra BN (1988) CT diagnosis of renal angiomyolipoma: the importance of detecting small amounts of fat. AJR 151:497–501
Kim JK, Kim SH, Jang YJ et al (2006) Renal angiomyolipoma with minimal fat: differentiation from other neoplasms at double-echo chemical shift FLASH MR imaging. Radiology 239:174–180
Hindman N, Ngo L, Genega EM et al (2012) Angiomyolipoma with minimal fat: can it be differentiated from clear cell renal cell carcinoma by using standard MR techniques? Radiology 265:468–477
Yoshimitsu K, Irie H, Tajima T et al (2004) MR imaging of renal cell carcinoma: its role in determining cell type. Radiat Med 22:371–376
Oliva MR, Glickman JN, Zou KH et al (2009) Renal cell carcinoma: t1 and t2 signal intensity characteristics of papillary and clear cell types correlated with pathology. AJR 192:1524–1530
Roy C, Sauer B, Lindner V, Lang H, Saussine C, Jacqmin D (2007) MR imaging of papillary renal neoplasms: potential application for characterization of small renal masses. Eur Radiol 17:193–200
Rosenkrantz AB, Niver BE, Fitzgerald EF, Babb JS, Chandarana H, Melamed J (2010) Utility of the apparent diffusion coefficient for distinguishing clear cell renal cell carcinoma of low and high nuclear grade. AJR 195:W344–351
Zhang JL, Sigmund EE, Chandarana H et al (2010) Variability of renal apparent diffusion coefficients: limitations of the monoexponential model for diffusion quantification. Radiology 254:783–792
Cornelis F, Lasserre AS, Tourdias T et al (2013) Combined late gadolinium-enhanced and double-echo chemical-shift MRI help to differentiate renal oncocytomas with high central t2 signal intensity from renal cell carcinomas. AJR 200:830–838
Sasiwimonphan K, Takahashi N, Leibovich BC, Carter RE, Atwell TD, Kawashima A (2012) Small (<4 cm) renal mass: differentiation of angiomyolipoma without visible fat from renal cell carcinoma utilizing MR imaging. Radiology 263:160–168
Busing KA, Kilian AK, Schaible T, Debus A, Weiss C, Neff KW (2008) Reliability and validity of MR image lung volume measurement in fetuses with congenital diaphragmatic hernia and in vitro lung models. Radiology 246:553–561
Shrout PE, Fleiss JL (1979) Intraclass correlations: uses in assessing rater reliability. Psychol Bull 86:420–428
Bland JM, Altman DG (1995) Multiple significance tests: the Bonferroni method. BMJ 310:170
Youden WJ (1950) Index for rating diagnostic tests. Cancer 3:32–35
Pedrosa I, Sun MR, Spencer M et al (2008) MR imaging of renal masses: correlation with findings at surgery and pathologic analysis. Radiographics 28:985–1003
Sun MRM, Ngo L, Genega EM et al (2009) Renal cell carcinoma: dynamic contrast-enhanced MR imaging for differentiation of tumor subtypes–correlation with pathologic findings. Radiology 250:793–802
Vargas HA, Chaim J, Lefkowitz RA et al (2012) Renal cortical tumors: use of multiphasic contrast-enhanced MR imaging to differentiate benign and malignant histologic subtypes. Radiology 264:779–788
Wang H, Cheng L, Zhang X et al (2010) Renal cell carcinoma: diffusion-weighted MR imaging for subtype differentiation at 3.0 T. Radiology 257:135–143
Pedrosa I, Alsop DC, Rofsky NM (2009) Magnetic resonance imaging as a biomarker in renal cell carcinoma. Cancer 115:2334–2345
Schatz SM, Lieber MM (2003) Update on oncocytoma. Curr Urol Rep 4:30–35
Rosenkrantz AB, Hindman N, Fitzgerald EF, Niver BE, Melamed J, Babb JS (2010) MRI features of renal oncocytoma and chromophobe renal cell carcinoma. AJR 195:W421–427
Dodelzon K, Mussi TC, Babb JS, Taneja SS, Rosenkrantz AB (2012) Prediction of growth rate of solid renal masses: utility of MR imaging features–preliminary experience. Radiology 262:884–893
Harmon WJ, King BF, Lieber MM (1996) Renal oncocytoma: magnetic resonance imaging characteristics. J Urol 155:863–867
Millet I, Doyon FC, Hoa D et al (2011) Characterization of small solid renal lesions: can benign and malignant tumors be differentiated with CT? AJR 197:887–896
Vargas HA, Delaney HG, Delappe EM et al (2013) Multiphasic contrast-enhanced MRI: single-slice versus volumetric quantification of tumor enhancement for the assessment of renal clear-cell carcinoma fuhrman grade. J Magn Reson Imaging 37:1160–1167
Acknowledgements
The authors thank Pippa McKelvie-Sebileau for medical editorial services.
The scientific guarantor of this publication is Professor Nicolas Grenier. The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article. The authors state that this work has not received any funding. One of the authors has significant statistical expertise. No complex statistical methods were necessary for this paper. Institutional review board approval was obtained. Written informed consent was waived by the institutional review board. Methodology: retrospective, diagnostic or prognostic study, performed at one institution.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cornelis, F., Tricaud, E., Lasserre, A.S. et al. Routinely performed multiparametric magnetic resonance imaging helps to differentiate common subtypes of renal tumours. Eur Radiol 24, 1068–1080 (2014). https://doi.org/10.1007/s00330-014-3107-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-014-3107-z