Abstract
An unprecedented expansion of antifungal therapy failure incidences in healthcare settings of Candida glabrata is the matter of global concern that needs to be addressed efficiently and effectively. In this pursuit, the present study has investigated the antifungal mechanism of benzylisoquinoline alkaloid berberine using biochemical, metabolic, and gene expression analysis, with the aim to delineate its therapeutic activity against C. glabrata and differentially fluconazole-responsive clinical isolates. Interestingly, the clinical isolates were found to be highly susceptible to berberine. Berberine was found to control the surface properties like hydrophobicity and charge of the cells. The cell membrane composition was altered by berberine, where the ergosterol and fatty acids were affected. The efflux pump activity was inhibited, and osmotic stress was generated in C. glabrata cells upon berberine exposure. The berberine has also generated oxidative stress and activated antioxidant system in C. glabrata cells. Furthermore, these observations were supported by the transcriptional expression study of C. glabrata cell genes (CDR1, RLM1, SLT2, SUR4, KRE1) and metabolomics analysis. Based on fold change analysis, the study identified 20 differential metabolites upon berberine treatment, which belong to central carbon, amino acids, and nucleotide pathways. The checkerboard analysis revealed the potentiation of some classically used antifungal drugs by berberine, thus suggesting it as a combinatorial nutraceutical adjuvant for the eradication of fungal infections.
Key points
• Berberine exhibited better potency against azole-resistant clinical isolates
• Berberine modulated metabolites of different pathways
• Berberine generated oxidative stress and blocked efflux pump activity
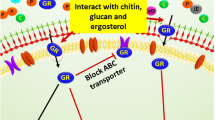
Graphical abstract







Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Ai X, Yu P, Peng L, Luo L, Liu J, Li S, Lai X, Luan F, Meng X (2021) Berberine: a review of its pharmacokinetics properties and therapeutic potentials in diverse vascular diseases. Front Pharmacol 12:762654
Alarcon-Barrera JC, Kostidis S, Ondo-Mendez A, Giera M (2022) Recent advances in metabolomics analysis for early drug development. Drug Discov Today 27(6):1763–1773
Ashok A, Mangalore RP, Morrissey CO (2022) Azole therapeutic drug monitoring and its use in the management of invasive fungal disease. Curr Fungal Infect Rep 16(2):55–69
Chakrabarti A, Mohamed N, Capparella MR, Townsend A, Sung AH, Yura R, Muñoz P (2022) The role of diagnostics-driven antifungal stewardship in the management of invasive fungal infections: a systematic literature review. In: Open forum infectious diseases. Oxford University Press, 9(7):ofac234
Chaudhary CR, Kavitake D, Jaiswal KK, Jaiswal KS, Reddy GB, Agarwal V, Shetty PH (2023) NMR-based metabolomics as a significant tool for human nutritional research and health applications. Food Biosci 53:102538
Chavda VP, Patel AB, Vihol D, Vaghasiya DD, Ahmed KMSB, Trivedi KU, Dave DJ (2022) Herbal remedies, nutraceuticals, and dietary supplements for COVID-19 management: an update. Clin Complement Med Pharmacol 2(1):100021
Chen C, Dickman MB (2005) Proline suppresses apoptosis in the fungal pathogen Colletotrichum trifolii. Proc Natl Acad Sci 102(9):3459–3464
Clarke CJ, Haselden JN (2008) Metabolic profiling as a tool for understanding mechanisms of toxicity. Toxicol Pathol 36(1):140–147
CLSI C (2008) Reference method for broth dilution antifungal susceptibility testing of filamentous fungi; Approved standard—second edition—document M38-A2
Colletti A, Cicero AFG (2021) Nutraceutical approach to chronic osteoarthritis: from molecular research to clinical evidence. Int J Mol Sci 22(23):12920
da Silva AR, de Andrade Neto JB, da Silva CR, de Sousa Campos R, Costa Silva RA, Freitas DD, do Nascimento FBSA, de Andrade LND, Sampaio LS, Grangeiro TB (2016) Berberine antifungal activity in fluconazole-resistant pathogenic yeasts: action mechanism evaluated by flow cytometry and biofilm growth inhibition in Candida spp. Antimicrob Agents Chemother 60(6):3551–3557
Denning DW (2022) Antifungal drug resistance: an update. Eur J Hosp Pharm 29(2):109–112
Eissa LA, Kenawy HI, El-Karef A, Elsherbiny NM, El-Mihi KA (2018) Antioxidant and anti-inflammatory activities of berberine attenuate hepatic fibrosis induced by thioacetamide injection in rats. Chem Biol Interact 294:91–100
Eleutherio E, Panek A, De Mesquita JF, Trevisol E, Magalhães R (2015) Revisiting yeast trehalose metabolism. Curr Genet 61(3):263–274
Esch BM, Limar S, Bogdanowski A, Gournas C, More T, Sundag C, Walter S, Heinisch JJ, Ejsing CS, André B (2020) Uptake of exogenous serine is important to maintain sphingolipid homeostasis in Saccharomyces cerevisiae. PLoS Genet 16(8):e1008745
Fisher MC, Denning DW (2023) The WHO fungal priority pathogens list as a game-changer. Nat Rev Microbiol 21(4):211–212
Fisher MC, Alastruey-Izquierdo A, Berman J, Bicanic T, Bignell EM, Bowyer P, Bromley M, Brüggemann R, Garber G, Cornely OA (2022) Tackling the emerging threat of antifungal resistance to human health. Nat Rev Microbiol 20(9):557–571
Flynn NE, Patyrak ME, Seely JB, Wu G (2010) Glycine oxidation and conversion into amino acids in Saccharomyces cerevisiae and Candida albicans. Amino Acids 39(2):605–608
Fogacci F, Fogacci S (2021) Cardiovascular risk factors management in pregnancy: a role for nutraceuticals? Nutraceuticals Cardiovasc Dis An Evidence-based Approach Clin Pract 245–253. https://springer.longhoe.net/chapter/10.1007/978-3-030-62632-7_12
Gharibpour F, Shirban F, Bagherniya M, Nosouhian M, Sathyapalan T, Sahebkar A (2021) The effects of nutraceuticals and herbal medicine on Candida albicans in oral candidiasis: a comprehensive review. Pharmacol Prop Plant-Derived Nat Prod Implic Hum Health 1308:225–248
Gupta P, Poluri KM (2021) Elucidating the eradication mechanism of perillyl alcohol against Candida glabrata biofilms: insights into the synergistic effect with azole drugs. ACS Bio Med Chem Au 2(1):60–72
Gupta P, Gupta S, Sharma M, Kumar N, Pruthi V, Poluri KM (2018) Effectiveness of phytoactive molecules on transcriptional expression, biofilm matrix, and cell wall components of Candida glabrata and its clinical isolates. ACS Omega 3(9):12201–12214
Gupta P, Gupta H, Poluri KM (2021a) Geraniol eradicates Candida glabrata biofilm by targeting multiple cellular pathways. Appl Microbiol Biotechnol 105(13):5589–5605
Gupta P, Mishra P, Mehra L, Rastogi K, Prasad R, Mittal G, Poluri KM (2021b) Eugenol-acacia gum-based bifunctional nanofibers as a potent antifungal transdermal substitute. Nanomedicine 16(25):2269–2289
Gupta H, Gupta P, Kairamkonda M, Poluri KM (2022a) Molecular investigations on Candida glabrata clinical isolates for pharmacological targeting. RSC Adv 12(27):17570–17584
Gupta P, Gupta H, Kairamkonda M, Kumar N, Poluri KM (2022b) Elucidating the lactic acid tolerance mechanism in vaginal clinical isolates of Candida glabrata. Med Mycol 60(6):myac042
Holmes AR, Cardno TS, Strouse JJ, Ivnitski-Steele I, Keniya MV, Lackovic K, Monk BC, Sklar LA, Cannon RD (2016) Targeting efflux pumps to overcome antifungal drug resistance. Future Med Chem 8(12):1485–1501
Huang X, Zheng D, Yong J, Li Y (2022) Antifungal activity and potential mechanism of berberine hydrochloride against fluconazole-resistant Candida albicans. J Med Microbiol 71(6):1542
Inamadar A, Rengasamy M, Charugulla SN (2022) Treatment approach for superficial dermatophytosis infections and factors contributing for noncompliance to antifungal therapy in India: an epidemiological survey. Clin Dermatology Rev 6(1):15–21
Jiang C, Li Z, Shi Y, Guo D, Pang B, Chen X, Shao D, Liu Y, Shi J (2020) Bacillus subtilis inhibits Aspergillus carbonarius by producing iturin A, which disturbs the transport, energy metabolism, and osmotic pressure of fungal cells as revealed by transcriptomics analysis. Int J Food Microbiol 330:108783
Jong CJ, Sandal P, Schaffer SW (2021) The role of taurine in mitochondria health: more than just an antioxidant. Molecules 26(16):4913
Katragkou A, Williams M, Sternberg S, Pantazatos D, Roilides E, Walsh TJ (2017) Micafungin alters the amino acid, nucleic acid and central carbon metabolism of Candida albicans at subinhibitory concentrations: novel insights into mechanisms of action. J Antimicrob Chemother 72(3):712–716
Kaur R, Domergue R, Zupancic ML, Cormack BP (2005) A yeast by any other name: Candida glabrata and its interaction with the host. Curr Opin Microbiol 8(4):378–384
Kobayashi D, Kondo K, Uehara N, Otokozawa S, Tsuji N, Yagihashi A, Watanabe N (2002) Endogenous reactive oxygen species is an important mediator of miconazole antifungal effect. Antimicrob Agents Chemother 46(10):3113–3117
Kontoyiannis DP (2000) Modulation of fluconazole sensitivity by the interaction of mitochondria and erg3p in Saccharomyces cerevisiae. J Antimicrob Chemother 46(2):191–197
Lee J, Dawes IW, Roe J-H (1995) Adaptive response of Schizosaccharomyces pombe to hydrogen peroxide and menadione. Microbiology 141(12):3127–3132
Martins-Santana L, Rezende CP, Rossi A, Martinez-Rossi NM, Almeida F (2023) Addressing microbial resistance worldwide: challenges over controlling life-threatening fungal infections. Pathogens 12(2):293
Moni M, Sidharthan N, Sudhir S, Prabhu B, Nampoothiri V, James J, Philip JM, Thomas J, Antony R, Mohamed ZU (2022) A quality improvement initiative to improve the appropriateness of candidemia management by the implementation of a comprehensive candidemia care bundle at a tertiary care hospital in South India: results of a quasi-experimental study. Medicine (Baltimore) 101(13):e28906
Och A, Podgórski R, Nowak R (2020) Biological activity of berberine—a summary update. Toxins (Basel) 12(11):713
Peghin M, Vena A, Graziano E, Giacobbe DR, Tascini C, Bassetti M (2022) Improving management and antimicrobial stewardship for bacterial and fungal infections in hospitalized patients with COVID-19. Ther Adv Infect Dis 9:20499361221095732
Perfect JR, Tenor JL, Miao Y, Brennan RG (2017) Trehalose pathway as an antifungal target. Virulence 8(2):143–149
Poopedi E, Marimani M, AlOmar SY, Aldahmash B, Ahmad A (2021) Modulation of antioxidant defence system in response to berberine in Candida albicans. Yeast 38(2):157–169
Puri V, Nagpal M, Singh I, Singh M, Dhingra GA, Huanbutta K, Dheer D, Sharma A, Sangnim T (2022) A comprehensive review on nutraceuticals: therapy support and formulation challenges. Nutrients 14(21):4637
Quan H, Cao Y-Y, Xu Z, Zhao J-X, Gao P-H, Qin X-F, Jiang Y-Y (2006) Potent in vitro synergism of fluconazole and berberine chloride against clinical isolates of Candida albicans resistant to fluconazole. Antimicrob Agents Chemother 50(3):1096–1099
Shao J, Shi G, Wang T, Wu D, Wang C (2016) Antiproliferation of berberine in combination with fluconazole from the perspectives of reactive oxygen species, ergosterol and drug efflux in a fluconazole-resistant Candida tropicalis isolate. Front Microbiol 7:1516
Silva S, Rodrigues CF, Araújo D, Rodrigues ME, Henriques M (2017) Candida species biofilms’ antifungal resistance. J Fungi 3(1):8
Souyoul SA, Saussy KP, Lupo MP (2018) Nutraceuticals: a review. Dermatol Ther (Heidelb) 8(1):5–16
Spigoni V, Aldigeri R, Antonini M, Micheli MM, Fantuzzi F, Fratter A, Pellizzato M, Derlindati E, Zavaroni I, Bonadonna RC (2017) Effects of a new nutraceutical formulation (berberine, red yeast rice and chitosan) on non-HDL cholesterol levels in individuals with dyslipidemia: results from a randomized, double blind, placebo-controlled study. Int J Mol Sci 18(7):1498
Swamy MK, Akhtar MS, Sinniah UR (2016) Antimicrobial properties of plant essential oils against human pathogens and their mode of action: an updated review. Evidence-Based Complement Altern Med 2016:3012462
Takagi H (2008) Proline as a stress protectant in yeast: physiological functions, metabolic regulations, and biotechnological applications. Appl Microbiol Biotechnol 81(2):211–223
World Health Organization (2023) WHO fungal priority pathogens list to guide research, development and public health action. 2022. Available https://www.who.int/publications/i/item/9789240060241
**e Y, Liu X, Zhou P (2020) In vitro antifungal effects of berberine against Candida spp. in planktonic and biofilm conditions. Drug Des Devel Ther 14:87–101
Xu Y, Wang Y, Yan L, Liang R-M, Dai B-D, Tang R-J, Gao P-H, Jiang Y-Y (2009) Proteomic analysis reveals a synergistic mechanism of fluconazole and berberine against fluconazole-resistant Candida albicans: endogenous ROS augmentation. J Proteome Res 8(11):5296–5304
Xu C, Wang J, Gao Y, Lin H, Du L, Yang S, Long S, She Z, Cai X, Zhou S (2010) The anthracenedione compound bostrycin induces mitochondria-mediated apoptosis in the yeast Saccharomyces cerevisiae. FEMS Yeast Res 10(3):297–308
Xu Y, Quan H, Wang Y, Zhong H, Sun J, Xu J, Jia N, Jiang Y (2017) Requirement for ergosterol in berberine tolerance underlies synergism of fluconazole and berberine against fluconazole-resistant Candida albicans isolates. Front Cell Infect Microbiol 7:491
Yan L, Zhang J-D, Cao Y-B, Gao P-H, Jiang Y-Y (2007) Proteomic analysis reveals a metabolism shift in a laboratory fluconazole-resistant Candida albicans strain. J Proteome Res 6(6):2248–2256
Zhu S, Yan L, Zhang Y, Jiang Z, Gao P, Qiu Y, Wang L, Zhao M, Cai Z, Tian S (2014) Berberine inhibits fluphenazine-induced up-regulation of CDR1 in Candida albicans. Biol Pharm Bull 37(2):268–273
Zorić N, Kosalec I, Tomić S, Bobnjarić I, Jug M, Vlainić T, Vlainić J (2017) Membrane of Candida albicans as a target of berberine. BMC Complement Altern Med 17(1):1–10
Acknowledgements
PG acknowledges financial support from the Department of Biotechnology (DBT), Government of India, under DBT-RAship scheme. HG acknowledges All India Council for Technical Education (AICTE) for support through QIP scheme. KMP acknowledge the receipt of Grant CRG/2022/003028 and STR/2022/000008 from SERB-DST, from Government of India. Both PG and KMP also acknowledge the technical and financial support under the collaborative alliance of IITR@175 from IIT-Roorkee. The authors are thankful to the NMR and analytical facilities at Institute Instrumentation Centre (IIC) at IIT Roorkee.
Author information
Authors and Affiliations
Contributions
KMP conceived the research plan. PG, HG, and ST performed the experiments; PG and HG analyzed the data; PG, HG, and KMP wrote the manuscript. All the authors have read and confirmed the final version of the manuscript. Both the authors PG and HG have contributed equally to the manuscript.
Corresponding author
Ethics declarations
Ethics approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Gupta, P., Gupta, H., Tripathi, S. et al. Biochemical and metabolomic insights into antifungal mechanism of berberine against Candida glabrata. Appl Microbiol Biotechnol 107, 6085–6102 (2023). https://doi.org/10.1007/s00253-023-12714-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00253-023-12714-x