Abstract
Purpose
To evaluate patients with resolved versus confirmed ARDS, identify subgroups with substantial mortality risk, and to determine the utility of day 2 ARDS reclassification.
Methods
Our primary objective, in this secondary LUNG SAFE analysis, was to compare outcome in patients with resolved versus confirmed ARDS after 24 h. Secondary objectives included identifying factors associated with ARDS persistence and mortality, and the utility of day 2 ARDS reclassification.
Results
Of 2377 patients fulfilling the ARDS definition on the first day of ARDS (day 1) and receiving invasive mechanical ventilation, 503 (24%) no longer fulfilled the ARDS definition the next day, 52% of whom initially had moderate or severe ARDS. Higher tidal volume on day 1 of ARDS was associated with confirmed ARDS [OR 1.07 (CI 1.01–1.13), P = 0.035]. Hospital mortality was 38% overall, ranging from 31% in resolved ARDS to 41% in confirmed ARDS, and 57% in confirmed severe ARDS at day 2. In both resolved and confirmed ARDS, age, non-respiratory SOFA score, lower PEEP and P/F ratio, higher peak pressure and respiratory rate were each associated with mortality. In confirmed ARDS, pH and the presence of immunosuppression or neoplasm were also associated with mortality. The increase in area under the receiver operating curve for ARDS reclassification on day 2 was marginal.
Conclusions
ARDS, whether resolved or confirmed at day 2, has a high mortality rate. ARDS reclassification at day 2 has limited predictive value for mortality. The substantial mortality risk in severe confirmed ARDS suggests that complex interventions might best be tested in this population.
Trial Registration
ClinicalTrials.gov NCT02010073.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
All patients that develop ARDS have a high risk for mortality, even when the syndrome resolves quickly. Higher tidal volume is associated with ARDS persistence. Patients with severe ARDS on the second day constitute a group at substantially increased risk for mortality. In contrast, the predictive value of ARDS reclassification at day 2 for mortality was relatively limited. |
Introduction
ARDS carries a high mortality, especially in observational studies, but with a relatively wide variability across studies [1,2,3]. The definition of ARDS has been repeatedly considered as one of the reasons for this heterogeneity. Because ARDS severity may change significantly in the first 24 h after fulfillment of the diagnostic criteria as the underlying mechanisms leading to lung injury progress or resolve, it has been proposed to reassess patients at 24 h (i.e., day 2) [4], in order to ‘confirm' fulfillment of the ARDS definition [5]. In addition, considerable optimization of management, particularly in regard to mechanical ventilatory support, may take place in the first 24 h, and impact on ARDS severity as captured by the definition.
The Berlin definition for ARDS [6] was designed primarily to make the diagnosis and has high sensitivity in this regard [7]. However, concerns exist regarding the specificity of the Berlin definition. In the LUNG SAFE study a significant portion of patients who initially fulfilled clinical criteria for ARDS did not do so 24 h later [1]. Some of these “resolved ARDS” patients may constitute false positives, transiently fulfilling clinical criteria for ARDS but not possessing the underlying pathophysiologic processes seen in ARDS, and consequently should have a much better outcome. In contrast, patients with confirmed ARDS, i.e., in whom ARDS criteria remain present 24 h later, may constitute a particularly high-risk patient cohort.
Reapplication of ARDS diagnostic criteria on day 2 following fulfillment of the ARDS definition may enhance our understanding of the impact of resolved versus confirmed ARDS, and predict important patient-centered outcomes from ARDS [4, 8, 9]. It may be possible to gain additional insights regarding the influence of management factors on the risk of ARDS persistence and on outcomes in these patients. Identification of ARDS subpopulations at highest risk for mortality might facilitate early consideration of these patients for adjunctive therapeutic strategies that have the potential for greater side effects (e.g., extracorporeal membrane oxygenation). Should reclassification at day 2 markedly improve outcome prognostication, this would have important implications for clinical trials, as another 24 h of confirmation may be necessary before enrolling patients into therapeutic trials.
We wished to address these issues in this secondary analysis of the LUNG SAFE cohort [1]. Our primary objective was to compare outcome in patients with resolved versus confirmed ARDS assessed on the day following ARDS onset. Secondary objectives included identifying factors associated with resolved and confirmed ARDS, determining the factors on the second day that predict hospital mortality, identifying subpopulations with high mortality risk, and determining the predictive value for patient outcome of reclassification of ARDS severity on the day following ARDS onset.
Methods and materials
The detailed methods and protocol have been published elsewhere [1]. In brief, LUNG SAFE was an international, multicenter, prospective cohort study, with a 4-week enrollment window in the winter season [1]. The study, funded by the European Society of Intensive Care Medicine (ESICM), was endorsed by multiple national societies/networks (Online Appendix 1). All participating ICUs obtained ethics committee approval, and either patient consent or ethics committee waiver of consent, as appropriate. National coordinators (Online Appendix 1) and site investigators (Online Appendix 2) were responsible for obtaining ethics committee approval and for ensuring data integrity and validity.
Patients, study design, and data collection
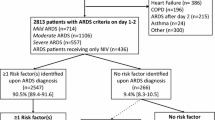
Inclusion criteria were admission to a study ICU (including ICU transfers) within the 4-week enrollment window; and receipt of invasive or noninvasive ventilation. Exclusion criteria were age less than 16 years or inability to obtain informed consent (where required). Patients were classified as having ARDS on the basis of fulfillment of all of the Berlin criteria rather than by clinician determination, as previously described [1]. This analysis was restricted to patients (93%) that fulfilled ARDS criteria within 48 h of the onset of acute hypoxemic respiratory failure (AHRF) and who received invasive mechanical ventilation (Fig. 1) at ARDS onset. All data were recorded for each patient at the same time each day within participating ICUs, normally as close as possible to 10 a.m. each day. Data on ventilatory settings were recorded simultaneously with arterial blood gas analysis.
Stratification and outcomes of patients classified for ARDS severity on day 1 and 2 of ARDS. Of 2377 patients that developed ARDS on day 1 or 2 following the development of AHRF, and were invasively ventilated, 263 (11.1%) were excluded from the analysis due to death (63 patients), or ICU discharge (16 patients) within 2 days, or because it was not possible to determine whether they still had ARDS (according to Berlin definition) on day 2 due to missing data (184 patients). The number of patients with ARDS evaluable for 2 days from onset was 2114, of which 1611 (76%) had confirmed ARDS and 503 (24%) had resolved ARDS at the second day. Patients are classified into three groups according to ARDS severity (mild, moderate, or severe) assessed at day 1, and then each group is stratified on the basis of their severity evaluated at day 2 (mild, moderate, severe, and resolved ARDS). In each group identified by day 1, the proportion of deaths varies among severity subgroups evaluated at day 2. Outcome is similar for each ARDS severity group on day 2, irrespective of their severity status on day 1
Definitions
Our definitions have been previously reported [1, 10, 11]. Day 1 refers to the first day on which the patient fulfilled all of the Berlin criteria for ARDS, while day 2 is the day following ARDS onset. For the purposes of this analysis patients were considered to have “resolved ARDS” when they initially fulfilled the Berlin ARDS criteria but did not fulfill at least one criterion on day 2. Patients were considered to have “confirmed ARDS” when they continued to fulfill the Berlin definition when reassessed on day 2. Where chest radiography was not present at day 2, patients could only be considered to have confirmed ARDS if the other criteria were still present. Where data on positive end-expiratory pressure (PEEP) were missing at day 2, patients were considered to have confirmed ARDS if (a) the other criteria were fulfilled, and (b) there were data on the third day indicating ongoing assisted ventilation with a PEEP of 5 cmH2O or greater (Table e1, Supplementary Material). Patients could not be deemed to have resolved ARDS if any of the day 2 data was missing. If ARDS status could not be determined on the second day, despite the aforementioned assumptions, they were excluded from further analysis, as were patients that were not in the ICU on day 2 (i.e., were discharged or dead).
Duration of invasive mechanical ventilation was calculated as the number of days between the date of intubation and the date of extubation in ICU (or death, if the patient died under invasive mechanical ventilation). Survival was evaluated at hospital discharge, or at day 90, whichever occurred first.
Data management and statistical analyses
Descriptive statistics included proportions for categorical variables and mean (standard deviation) or median (interquartile range) for continuous variables. The study population was stratified according to the fulfillment of the Berlin definition on day 2 (resolved versus confirmed ARDS). Comparisons between groups were performed using Chi-squared test (or Fisher exact test) for discrete variables or Student’s t test (or Wilcoxon-Mann–Whitney test) for continuous variables. The Shapiro–Wilk test was used to assess normality in data distribution. Moreover, differences in discrete or continuous distributions of variables measured at day 1 and 2 were tested using McNemar’s test or Wilcoxon signed-rank test, respectively.
To evaluate factors associated with persistence of ARDS, we applied a multivariable logistic regression model and the independent predictors (demographic characteristics and clinical parameters measured at the first day of ARDS) were identified through stepwise regression approach. This approach combines forward and backward selection methods in an iterative procedure to select predictors in the final multivariable model. This approach was also applied to identify factors associated with hospital mortality in patients with resolved and with confirmed ARDS. Moreover, as a result of missing values in the clinical variables measured at the second day of ARDS (Table e2, Supplementary Material), we assessed the same model for hospital mortality, assuming a random distribution of missing data [12]. We applied a multiple imputation approach to handle missing information and the Markov chain Monte Carlo method was used to create 20 imputed datasets [13]. The estimates of each multivariable logistic model were combined using Rubin’s rules to estimate odds ratio (ORs) and corresponding 95% confidence intervals (CIs) [14].
To compare the predictive value for hospital mortality of day 2 and day 1 ARDS classification (Berlin definition), we estimated the area under the receiver operating curve (AUROC) using two different multivariable logistic regression models performed on the whole study population. The first model considered as independent variables all significant factors (demographic and clinical) measured at day 1 and identified by stepwise regression approach, plus ARDS severity at day 1 (mild, moderate, severe). The second model was similar, except for ARDS severity measured at day 2 (resolved, mild, moderate, and severe). The two AUROCs were estimated fitting the two models on the subset of patients without missing values in the covariates, in order to compare them with the non-parametric approach of DeLong, DeLong, and Clarke-Pearson [15].
We analyzed the survival time in patients with resolved and confirmed ARDS using the Kaplan–Meier approach with patients stratified according to ARDS severity at day 1 and/or day 2. When the survival curve involved ARDS severity at day 2, time and probabilities were calculated starting from the second day of ARDS. We assumed that patients discharged alive from hospital before 90 days were alive on day 90. Differences in survival curves were assessed by the log-rank test.
All P values were two-sided, with P values less than 0.05 considered as statistically significant.
Statistical analyses were performed with R, version 3.3.3. (R Project for Statistical Computing, http://www.R-project.org) and SAS software, version 9.4 (SAS Institute, Cary, NC, USA).
Results
Of 2377 patients that developed ARDS within 48 h of the occurrence of AHRF, and were invasively ventilated, we excluded from the main analysis 263 patients (11.1%) because of death (63 patients) or ICU discharge (16 patients) by day 2, or because it was not possible to determine whether they still had ARDS on day 2 according to the Berlin definition, as a result of missing data (184 patients) (Fig. 1 and Tables e1–2, Supplementary Material).
Evolution of ARDS over first 24 h
ARDS severity profile varied significantly from day 1 to day 2. Of 2114 patients fulfilling ARDS criteria on day 1 and included in this study, 503 (24%) patients had resolved ARDS, no longer fulfilling ARDS criteria on day 2, while 1611 (76%) patients had confirmed ARDS (Table 1 and Fig. 1). Among confirmed ARDS patients, 31% improved to a less severe ARDS category, 55% were unchanged, while 14% progressed to a more severe ARDS category (Table e3, Supplementary Material).
Resolved ARDS
Patients with resolved ARDS were less severely ill, with higher PaO2/FiO2 (P/F) ratio and lower SOFA score, compared to those with confirmed ARDS (Table 1); 52% of the resolved ARDS patients had moderate or severe ARDS. Resolved ARDS patients had a lower prevalence of pneumonia and a higher prevalence of non-cardiogenic shock (Table e4). Clinicians were less likely to recognize ARDS on day 1 in patients with resolved ARDS compared to patients with confirmed ARDS (24% vs 35%, P < 0.0001). Patients with resolved ARDS received significantly higher tidal volumes and lower PEEP on day 2 compared to day 1 (Fig. e1, Supplementary Material).
Mortality was 31% in these patients (Table 1). Factors associated with mortality in patients with resolved ARDS were higher age, higher respiratory SOFA score, higher respiratory rate, lower P/F ratio, lower PEEP, and higher PIP (Table 2).
Confirmed ARDS
Confirmed ARDS patients had higher day 1 driving pressures (mean value 14.9 vs. 13.3 cmH2O, P < 0.0001),and received higher PEEP (mean value 8.6 vs. 7.8 cmH2O, P = 0.0016) compared to patients with resolved ARDS (Table 1). Mechanical ventilation-related changes from day 1 to day 2 were modest, with no change in tidal volume (Fig. e1A), a small increase in PEEP (in moderate or severe ARDS) (Fig. e1B), and a decrease in peak inspiratory pressure (PIP) (mild or moderate ARDS) (Fig. e1C, Supplementary Material). Sixty-nine percent of patients with confirmed ARDS received protective mechanical ventilation on day 2 compared to 65% on day 1 (P = 0.41), defined as a tidal volume of 8 mL/kg of predicted body weight or less and a plateau pressure of 30 cmH2O or less (Fig. e2, Supplementary Material).
In the multivariable model, pneumonia was a risk factor for confirmed ARDS (Table 3). Other factors measured on day 1 significantly associated with confirmed ARDS were lower P/F ratio, higher PIP, higher non-respiratory SOFA score, and higher tidal volume.
On day 2, tidal volume decreased modestly, while PEEP increased (mean values from 8.1 cmH2O in mild to 10.5 cmH2O in severe ARDS) with greater ARDS severity category (Table e3). Median inspired fractional oxygen use increased substantially, from 0.4 in mild, to 0.5 in moderate and 0.9 in severe ARDS (Table e3, Supplementary Material).
Hospital mortality of patients with confirmed ARDS was 41%: this increased from 36% with mild, to 39% with moderate and 57% with severe ARDS at day 2 (P < 0.0001) (Table 1 and Table e3, Supplementary Material). In multivariable analyses, age, the presence of immunosuppression and/or neoplasm and chronic liver failure were each associated with increased hospital mortality (Table 2). Illness severity factors on day 2 significantly associated with increased mortality were lower P/F ratio, lower pH, and higher non-respiratory SOFA score. In regard to ventilation-related factors, the use of higher respiratory rate and lower PEEP, and the presence of higher PIP were each associated with higher hospital mortality.
Reclassification of ARDS severity on day 2
Hospital mortality in patients with ARDS severity classified as mild on day 1 was 34%, compared to 36% in mild ARDS patients on day 2 (Fig. 1 and Table e3, Supplementary Material). Mortality rates were unchanged at 39% in patients classified as moderate ARDS severity on day 1 or 2. In contrast, in patients classified as severe ARDS, mortality increased from 43% in patients classified on day 1 to 57% in patients classified on day 2. Kaplan–Meier curves for outcome based on ARDS severity on day 1 versus day 2 confirm these findings, with mortality significantly higher for severe confirmed ARDS compared to all other severity categories on day 2 (Fig. 2a, b).
Hospital survival probability in patients with ARDS classified on day 1 and day 2 (Kaplan–Meier approach). Kaplan–Meier curves for survival during hospital stay in patients with ARDS stratified by ARDS severity on day 1 (a) or day 2 (b). In b, time and probabilities were calculated starting from the second day of ARDS. *P < 0.05 versus mild ARDS. †P < 0.05 versus resolved ARDS. ‡P < 0.05 versus moderate ARDS
Kaplan–Meier curves for each category of ARDS severity on day 1 demonstrated a significantly different survival probability when stratified by ARDS severity on day 2 (Fig. e3A–C). In contrast, survival probability observed in patients with ARDS severity assessed at day 2 demonstrated similar probability when stratified by ARDS severity on day 1 (Fig. e3D–F, Supplementary Material).
Reclassification of ARDS severity on day 2 demonstrated a marginal (though statistically significant) increase in predictive value for mortality compared to day 1 (estimated difference between AUROCs was 0.0089, P = 0.045) (Fig. e4). Of interest, day 2 non-pulmonary SOFA demonstrated greater accuracy to predict mortality (AUROC 0.67, 95% CI 0.65–0.70) than P/F ratio (AUROC 0.57, 95% CI 0.55–0.60), while the combination of both variables did not improve AUROC (0.68, 95% CI 0.65–0.70) over SOFA score alone (Table e5, Supplementary Material).
Discussion
Almost one quarter of patients that fulfill ARDS criteria demonstrate resolution of one or more criteria 24 h later, while ARDS is confirmed or persists for at least 24 h in the other three quarters of patients. All patients with ARDS, whether resolved or confirmed at day 2, had a high mortality. Of concern, higher tidal volume on day 1 was independently associated with persistence of ARDS at day 2, while higher respiratory rate was associated with increased mortality. Reclassification of ARDS severity on day 2 identified patients with severe confirmed ARDS as a group with substantially increased mortality. In contrast, the predictive value of ARDS reclassification at day 2 for mortality was relatively limited.
Evolution of ARDS severity over first 24 h
Substantial changes were seen in the ARDS severity profile over the first 24 h, with ARDS resolving or decreasing in severity in over half of patients, while ARDS severity worsened in only 14%. ARDS resolved in 17% of patients classified as severe ARDS on day 1. Perhaps not surprisingly, greater day 1 severity of ARDS and higher non-respiratory SOFA score both increased the likelihood of ARDS persistence. Of interest, ARDS duration and the severity of hypoxemia have been identified in post-mortem studies as being predictive of the presence of diffuse alveolar damage [16]. Higher tidal volume use on day 1 was associated with ARDS persistence, supporting concerns raised regarding higher tidal volume use [17, 18], especially in early ARDS [19]. Given the extent of evolution of the clinical condition over the first 24 h, specifically the clinical improvement of most patients, selection of patients for clinical trials based on day 1 data—particularly where the intervention may have significant side effects (e.g., higher PEEP or extracorporeal membrane oxygenation)—may not be optimal.
Impact of ventilator management
The role of ventilator-induced lung injury in worsening outcomes from ARDS is clear from multiple studies [17, 18]. Our findings emphasize the need for continued focus on ventilator management to minimize iatrogenic injury and improve outcome in patients with ARDS. The use of higher tidal volume on day 1 of ARDS was associated with ARDS persistence. In patients with resolved and confirmed ARDS, the use of higher respiratory rate and lower PEEP, and the presence of higher PIP were each associated with higher hospital mortality.
Overall, we found relatively limited changes in ventilator management from day 1 to 2. There was no overall change in tidal volume in patients with confirmed (whether mild, moderate, or severe) ARDS from day 1 to 2. Patients with resolved ARDS actually received higher tidal volumes and lower PEEP on day 2 than on day 1. While potentially a reflection of an improvement in the patients’ condition, with increased spontaneous ventilation, this remains a concern [20].
Resolved versus confirmed ARDS
Patients with resolved ARDS had similar mortality to patients with mild confirmed ARDS, underlining the fact that this constitutes a patient group with ongoing critical illness. Older age, non-respiratory SOFA score, and day 1 ventilator parameters including respiratory rate, PEEP, and PIP were each associated with outcome in these patients. Our data provide novel insights into this poorly characterized patient group, and emphasize the requirement for careful attention to ventilator parameters and ongoing critical care to optimize clinical outcomes in these patients.
Consistent with previous studies, persistence of ARDS was associated with longer ICU and hospital stay, fewer ventilator-free days, and lower hospital survival [4, 8, 9]. The high mortality (57%) in patients with severe ARDS on day 2 suggests that these patients may warrant early consideration for alternative approaches, such as extracorporeal membrane oxygenation, to improve outcomes.
Predictive value of reapplication of ARDS criteria on day 2
Accurately predicting patient outcome, while not the primary role of diagnostic criteria such as the Berlin definition, is an important aspect of validity in the absence of a “gold standard” [6]. While the Berlin definition demonstrates somewhat better predictive value for mortality compared to the older American-European Consensus Conference definition [6], it remains low which is a potential limitation [7].
Reapplication of ARDS criteria on day 2 of ARDS provided greater discriminatory capacity for patient outcome, with greater separation in mortality rates by ARDS severity compared to classification on day 1. Of interest, patients with confirmed ARDS did not have a uniformly worse outcome, such as might be explained by the removal of patients with resolved ARDS from the analysis. Hospital mortality was substantially increased in patients with severe ARDS on day 2, suggesting that this approach identifies a higher-risk patient cohort.
In contrast, the overall increase in the predictive value for outcome of reclassification of ARDS severity on day 2, while statistically significant, was only marginal. This is perhaps not surprising, given all the other factors known to be important (including age, comorbid disease, other organ dysfunction, vasopressor requirement, etc.) in determining outcome from critical illnesses, including ARDS [11, 21, 22]. In fact, it is well recognized that many patients die with, rather than of, ARDS, i.e., they die from other complications of their critical illness such as vasopressor-resistant shock due to sepsis [23]. This is supported by our finding that the predictive value of the non-pulmonary SOFA score was slightly higher than the P/F ratio in the patient population with confirmed ARDS. Including all variables identified in the model further increased predictive value. This may have important implications for clinical trials since it has been claimed that waiting for “confirmed ARDS” to enroll patients results in a patient population with higher severity and/or greater homogeneity.
Limitations
This study has several limitations. Our patient cohort, while large and geographically diverse, may not be representative of actual clinical practice in ICUs across the globe. We did not have access to the source data for the patients in the enrolling ICUs, and it is possible that not all patients with ARDS in participating centers were enrolled. However, enrollment of patients with ARDS from participating ICUs met expectations based on their recorded 2013 admission rates, while data from lower-recruiting ICUs was not different from that from higher-enrolling ICUs, suggesting the absence of reporting biases.
We instituted a robust data quality control program in which all centers were requested to verify data that appeared inconsistent or erroneous. Despite our data quality control, missing data meant that we had to apply two assumptions regarding chest radiography and PEEP settings to classify one-fifth of patients. Missing radiologic data for day 2 likely reflects the fact that routine daily chest radiographs are no longer justified [24, 25]. We were unable to classify 8% of patients because of missing day 2 oxygenation data. Analysis of the clinical characteristics and presence of other Berlin criteria of this latter group demonstrate a similar profile to included patients, suggesting their exclusion does not bias this analysis. Use of a multiple imputation approach to assess the possible influence of missing data demonstrated similar results for predictors associated with mortality to that seen with the study population. Taken together, these findings support the robustness of our analytic approach.
While we have adjusted our analyses to account for known measured confounders, the possibility remains that some of our findings may arise from unmeasured or residual confounding. Moreover, we cannot make causal inferences for the associations seen, given the observational nature of our study. In this is an observational dataset, we are unable to test promising approaches to determining persistence of ARDS that involve standardization of ventilator settings, such as those proposed by Villar et al. [26]. Given the size of our database, small differences between groups may achieve statistical significance but be of uncertain clinical significance. Lastly, our assumption that inpatients at day 90 survived to hospital discharge is a further limitation.
Conclusions
All patients with ARDS, whether resolved or confirmed on the second day after onset, had a high mortality. Reclassification of ARDS severity on day 2 identified patients with severe confirmed ARDS as constituting a group at substantially increased risk for mortality. Clinical trials of complex interventions, especially those with significant side effects, might best be focused on this population. In contrast, the predictive value of ARDS reclassification at day 2 for mortality was relatively limited.
References
Bellani G, Laffey JG, Pham T, Fan F, Brochard L, Esteban A, Gattinoni L, van Haren F, Larsson A, McAuley DF, Ranieri M, Rubenfeld GD, Thompson BT, Wrigge H, Slutsky AS, Pesenti A, LUNG SAFE Investigators, ESICM Trials Group (2016) Epidemiology, patterns of care, and mortality for patients with acute respiratory distress syndrome in intensive care units in 50 countries. JAMA 315:788–800
Bersten AD, Edibam C, Hunt T, Moran J, Australian, New Zealand Intensive Care Society Clinical Trials Group (2002) Incidence and mortality of acute lung injury and the acute respiratory distress syndrome in three Australian states. Am J Respir Crit Care Med 165:443–448
Villar J, Blanco J, Anon JM, Santos-Bouza A, Blanch L, Ambros A, Gandia F, Carriedo D, Mosteiro F, Basaldua S, Fernandez RL, Kacmarek RM (2011) The ALIEN study: incidence and outcome of acute respiratory distress syndrome in the era of lung protective ventilation. Intensive Care Med 37:1932–1941
Villar J, Fernandez RL, Ambros A, Parra L, Blanco J, Dominguez-Berrot AM, Gutierrez JM, Blanch L, Anon JM, Martin C, Prieto F, Collado J, Perez-Mendez L, Kacmarek RM, Acute Lung Injury Epidemiology and Natural History Network (2015) A clinical classification of the acute respiratory distress syndrome for predicting outcome and guiding medical therapy. Crit Care Med 43:346–353
Guerin C, Reignier J, Richard JC, Beuret P, Gacouin A, Boulain T, Mercier E, Badet M, Mercat A, Baudin O, Clavel M, Chatellier D, Jaber S, Rosselli S, Mancebo J, Sirodot M, Hilbert G, Bengler C, Richecoeur J, Gainnier M, Bayle F, Bourdin G, Leray V, Girard R, Baboi L, Ayzac L (2013) Prone positioning in severe acute respiratory distress syndrome. N Engl J Med 368:2159–2168
ARDS Definition Task Force, Ranieri VM, Rubenfeld GD, Thompson BT, Ferguson ND, Caldwell E, Fan E, Camporota L, Slutsky AS (2012) Acute respiratory distress syndrome: the Berlin Definition. JAMA 307:2526–2533
Frohlich S, Murphy N, Boylan JF (2013) ARDS: progress unlikely with non-biological definition. Br J Anaesth 111:696–699
Villar J, Blanco J, del Campo R, Andaluz-Ojeda D, Diaz-Dominguez FJ, Muriel A, Corcoles V, Suarez-Sipmann F, Tarancon C, Gonzalez-Higueras E, Lopez J, Blanch L, Perez-Mendez L, Fernandez RL, Kacmarek RM, Spanish Initiative for Epidemiology, Stratification & Therapies for ARDS (SIESTA) Network (2015) Assessment of PaO(2)/FiO(2) for stratification of patients with moderate and severe acute respiratory distress syndrome. BMJ Open 5:e006812
Bos LD, Cremer OL, Ong DS, Caser EB, Barbas CS, Villar J, Kacmarek RM, Schultz MJ, MARS Consortium (2015) External validation confirms the legitimacy of a new clinical classification of ARDS for predicting outcome. Intensive Care Med 41:2004–2005
Bellani G, Laffey JG, Pham T, Madotto F, Fan E, Brochard L, Esteban A, Gattinoni L, Bumbasirevic V, Piquilloud L, van Haren F, Larsson A, McAuley DF, Bauer PR, Arabi YM, Ranieri M, Antonelli M, Rubenfeld GD, Thompson BT, Wrigge H, Slutsky AS, Pesenti A, LUNG SAFE Investigators, ESICM Trials Group (2017) Non-invasive ventilation of patients with ARDS: insights from the LUNG SAFE study. Am J Respir Crit Care Med 195:67–77
Laffey JG, Bellani G, Pham T, Fan E, Madotto F, Bajwa EK, Brochard L, Clarkson K, Esteban A, Gattinoni L, van Haren F, Heunks LM, Kurahashi K, Laake JH, Larsson A, McAuley DF, McNamee L, Nin N, Qiu H, Ranieri M, Rubenfeld GD, Thompson BT, Wrigge H, Slutsky AS, Pesenti A, LUNG SAFE Investigators, ESICM Trials Group (2016) Potentially modifiable factors contributing to outcome from acute respiratory distress syndrome: the LUNG SAFE study. Intensive Care Med 42:1865–1876
Sterne JA, White IR, Carlin JB, Spratt M, Royston P, Kenward MG, Wood AM, Carpenter JR (2009) Multiple imputation for missing data in epidemiological and clinical research: potential and pitfalls. BMJ 338:b2393
Schafer JL (1997) Analysis of incomplete multivariate data. Chapman & Hall, New York
Rubin DB (2004) Multiple imputation for nonresponse in surveys. Wiley, New York
DeLong ER, DeLong DM, Clarke-Pearson DL (1988) Comparing the areas under two or more correlated receiver operating characteristic curves: a nonparametric approach. Biometrics 44:837–845
Thille AW, Esteban A, Fernandez-Segoviano P, Rodriguez JM, Aramburu JA, Penuelas O, Cortes-Puch I, Cardinal-Fernandez P, Lorente JA, Frutos-Vivar F (2013) Comparison of the Berlin definition for acute respiratory distress syndrome with autopsy. Am J Respir Crit Care Med 187:761–767
Network ARDS (2000) Ventilation with lower tidal volumes as compared with traditional tidal volumes for acute lung injury and the acute respiratory distress syndrome. The Acute Respiratory Distress Syndrome Network. N Engl J Med 342:1301–1308
Amato MB, Barbas CS, Medeiros DM, Magaldi RB, Schettino GP, Lorenzi-Fihlo G, Kairalla RA, Deheinzelin D, Munoz C, Oliveira R, Takagaki TY, Carvalho CR (1998) Effect of a protective-ventilation strategy on mortality in the acute respiratory distress syndrome. N Engl J Med 338:347–354
Needham DM, Yang T, Dinglas VD, Mendez-Tellez PA, Shanholtz C, Sevransky JE, Brower RG, Pronovost PJ, Colantuoni E (2015) Timing of low tidal volume ventilation and intensive care unit mortality in acute respiratory distress syndrome. A prospective cohort study. Am J Respir Crit Care Med 191:177–185
Gajic O, Frutos-Vivar F, Esteban A, Hubmayr RD, Anzueto A (2005) Ventilator settings as a risk factor for acute respiratory distress syndrome in mechanically ventilated patients. Intensive Care Med 31:922–926
Brun-Buisson C, Doyon F, Carlet J, Dellamonica P, Gouin F, Lepoutre A, Mercier JC, Offenstadt G, Regnier B (1995) Incidence, risk factors, and outcome of severe sepsis and septic shock in adults. A multicenter prospective study in intensive care units. French ICU Group for Severe Sepsis. JAMA 274:968–974
Brun-Buisson C, Minelli C, Bertolini G, Brazzi L, Pimentel J, Lewandowski K, Bion J, Romand JA, Villar J, Thorsteinsson A, Damas P, Armaganidis A, Lemaire F (2004) Epidemiology and outcome of acute lung injury in European intensive care units. Results from the ALIVE study. Intensive Care Med 30:51–61
Stapleton RD, Wang BM, Hudson LD, Rubenfeld GD, Caldwell ES, Steinberg KP (2005) Causes and timing of death in patients with ARDS. Chest 128:525–532
Hejblum G, Chalumeau-Lemoine L, Ioos V, Boelle PY, Salomon L, Simon T, Vibert JF, Guidet B (2009) Comparison of routine and on-demand prescription of chest radiographs in mechanically ventilated adults: a multicentre, cluster-randomised, two-period crossover study. Lancet 374:1687–1693
Resnick S, Inaba K, Karamanos E, Skiada D, Dollahite JA, Okoye O, Talving P, Demetriades D (2017) Clinical relevance of the routine daily chest X-ray in the surgical intensive care unit. Am J Surg 214:19–23
Villar J, Perez-Mendez L, Lopez J, Belda J, Blanco J, Saralegui I, Suarez-Sipmann F, Lopez J, Lubillo S, Kacmarek RM, HELP Network (2007) An early PEEP/FIO2 trial identifies different degrees of lung injury in patients with acute respiratory distress syndrome. Am J Respir Crit Care Med 176:795–804
Acknowledgments
LUNG SAFE Investigators A complete list of LUNG SAFE steering committee, national coordinators, site investigators, and national societies endorsing the study can be found in the Supplementary Material.
Collaborating Authors. LUNG SAFE Steering Committee: Antonio Pesenti, John G. Laffey, Laurent Brochard, Andres Esteban, Luciano Gattinoni, Frank van Haren, Anders Larsson, Daniel F. McAuley, Marco Ranieri, Gordon Rubenfeld, B. Taylor Thompson, Hermann Wrigge, Arthur S. Slutsky. LUNG SAFE National Coordinators: Argentina: Fernando Rios; Australia/New Zealand: Frank Van Haren; Belgium: Sottiaux T, Depuydt P; Bolivia: Fredy S Lora; Brazil: Luciano Cesar Azevedo; Canada: Eddy Fan; Chile: Guillermo Bugedo; China: Haibo Qiu; Colombia: Marcos Gonzalez; Costa Rica: Juan Silesky; Czech Republic: Vladimir Cerny; Denmark: Jonas Nielsen; Ecuador: Manuel Jibaja; France: Tài Pham; Germany: Hermann Wrigge; Greece: Dimitrios Matamis; Guatemala: Jorge Luis Ranero; India: Pravin Amin; Iran: S.M. Hashemian; Ireland: Kevin Clarkson; Italy: Giacomo Bellani; Japan: Kiyoyasu Kurahashi; Mexico: Asisclo Villagomez; Morocco: Amine Ali Zeggwagh; Netherlands: Leo M Heunks; Norway: Jon Henrik Laake; Philippines: Jose Emmanuel Palo; Portugal: Antero do Vale Fernandes; Romania: Dorel Sandesc; Saudi Arabia: Yaasen Arabi; Serbia: Vesna Bumbasierevic; Spain: Nicolas Nin, Jose A Lorente; Sweden: Anders Larsson; Switzerland: Lise Piquilloud; Tunisia: Fekri Abroug; UK: Daniel F McAuley, Lia McNamee; Uruguay: Javier Hurtado; USA: Ed Bajwa; Venezuela: Gabriel Démpaire.
LUNG SAFE Site Investigators (by Country):
ALBANIA: Uhc Mother Theresa (Tirana): Hektor Sula, Lordian Nunci; University Hospital Shefqet Ndroqi (Tirana): Alma Cani; ARGENTINA: Clinica De Especialidades (Villa Maria): Alan Zazu; Hospital Dr Julio C. Perrando (Resistencia): Christian Dellera, Carolina S Insaurralde; Sanatorio Las Lomas (San Isidro, Buenos Aires): Risso V Alejandro; Sanatorio De La Trinidad San Isidro (San Isidro): Julio Daldin, Mauricio Vinzio; Hospital Español De Mendoza (Godoy Cruz - Mendoza): Ruben O Fernandez; Hospital Del Centenario (Rosario): Luis P Cardonnet, Lisandro R Bettini; San Antonio (Gualeguay (Entre Rios)): Mariano Carboni Bisso, Emilio M Osman; Cemic (Buenos Aires): Mariano G Setten, Pablo Lovazzano; Hospital Universitrario Austral (Pilar): Javier Alvarez, Veronica Villar; Hospital Por + Salud (Pami) Dr. Cesar Milstein (Buenos Aires): Norberto C Pozo, Nicolas Grubissich; Sanatorio Anchorena (Buenos Aires): Gustavo A Plotnikow, Daniela N Vasquez; Sanatorio De La Trinidad Mitre (Buenos Aires): Santiago Ilutovich, Norberto Tiribelli; Hospital Luis Lagomaggiore (Mendoza): Ariel Chena, Carlos A Pellegrini; H.I.G.A San Martín (La Plata): María G Saenz, Elisa Estenssoro; Hospital Misericordia (Cordoba): Matias Brizuela, Hernan Gianinetto; Sanatorio Juncal (Temperley): Pablo E Gomez, Valeria I Cerrato; Hospital D. F. Santojanni (Buenos Aires): Marco G Bezzi, Silvina A Borello; Hospital Alejandro Posadas (Buenos Aires): Flavia A Loiacono, Adriana M Fernandez; AUSTRALIA: St. Vincent’s Hospital, Sydney (Darlinghurst): Serena Knowles, Claire Reynolds; St George Public Hospital (Kogarah): Deborah M Inskip, Jennene J Miller; Westmead Hospital (Westmead): **g Kong, Christina Whitehead; Flinders Medical Centre (Bedford Park, South Australia): Shailesh Bihari; John Hunter Hospital (Newcastle): Aylin Seven, Amanda Krstevski; Canberra Hospital (Garran): Helen J Rodgers, Rebecca T Millar; Calvary Mater Newcastle (Waratah): Toni E Mckenna, Irene M Bailey; Cabrini Hospital (Melbourne): Gabrielle C Hanlon; Liverpool Hospital (Liverpool): Anders Aneman, Joan M Lynch; Coffs Harbour Health Campus (Coffs Harbour): Raman Azad, John Neal; Sir Charles Gairdner Hospital (Nedlands): Paul W Woods, Brigit L Roberts; Concord Hospital (Concord): Mark R Kol, Helen S Wong; AUSTRIA: General Hospital of Vienna/Medical University of Vienna (Vienna): Katharina C Riss, Thomas Staudinger; BELGIUM: Cliniques universitaires St Luc, UCL (Brussels): Xavier Wittebole, Caroline Berghe; CHU Dinant-Godinne (Yvoir): Pierre A Bulpa, Alain M Dive; AZ Sint Augustinus Veurne (Veurne): Rik Verstraete, Herve Lebbinck; Ghent University Hospital (Ghent): Pieter Depuydt, Joris Vermassen; University Hospitals Leuven (Leuven): Philippe, Meersseman, Helga Ceunen; BRAZIL: Hospital Renascentista (Pouso Alegre): Jonas I Rosa, Daniel O Beraldo; Vitoria Apart Hospital (Serra): Claudio Piras, Adenilton M Rampinelli; Hospital Das Clinicas (São Paulo): Antonio P Nassar Jr; Hospital Geral Do Grajaù (São Paulo): Sergio Mataloun, Marcelo Moock; Evangelical Hospital (Cachoeiro De Itapemirim/Espírito Santo): Marlus M Thompson, Claudio H Gonçalves; Hospital Moinhos De Vento (Porto Alegre): Ana Carolina P Antônio, Aline Ascoli; Hospital Alvorada Taguatinga (Taguatinga): Rodrigo S Biondi, Danielle C Fontenele; Complexo Hospitalar Mngabeira Tarcisio Burity (Joao Pessoa): Danielle Nobrega, Vanessa M Sales; BRUNEI DARUSSALAM: Raja Isteri Pengiran Anak Saleha (Ripas) Hospital (Bandar Seri Begawan): Dr Suresh Shindhe, Dr Dk Maizatul Aiman B Pg Hj Ismail; CANADA: Medical-Surgical ICU of St Michael’s Hospital (Toronto): John Laffey, Francois Beloncle; St. Josephs Health Centre (Toronto): Kyle G Davies, Rob Cirone; Sunnybrook Health Sciences Center (Toronto): Venika Manoharan, Mehvish Ismail; Toronto Western Hospital (Toronto): Ewan C Goligher, Mandeep Jassal; Medical Surgical ICU of the Toronto General Hospital (Toronto): Erin Nishikawa, Areej Javeed; Cardiovascular ICU of St Michael’s Hospital (Toronto): Gerard Curley, Nuttapol Rittayamai; Cardiovascular ICU of the Toronto General Hospital (Toronto): Matteo Parotto, Niall D Ferguson; Mount Sinai Hospital (Toronto): Sangeeta Mehta, Jenny Knoll; Trauma-Neuro ICU of St Michael’s Hospital (Toronto): Antoine Pronovost, Sergio Canestrini; CHILE: Hospital Clínico Pontificia Universidad Católica De Chile (Santiago): Alejandro R Bruhn, Patricio H Garcia; Hospital Militar De Santiago (Santiago): Felipe A Aliaga, Pamela A Farías; Clinica Davila (Santiago): Jacob S Yumha; Hospital Guillermo Grant Benavente (Concepcion): Claudia A Ortiz, Javier E Salas; Clinica Las Lilas (Santiago): Alejandro A Saez, Luis D Vega; Hospital Naval Almirante Nef (Viña Del Mar): Eduardo F Labarca, Felipe T Martinez; Hospital Luis Tisné Brousse (Penanolen): Nicolás G Carreño, Pilar Lora; CHINA: The Second Affiliated Hospital of Harbin Medical University (Harbin): Haitao Liu; Nan**g Zhong-Da Hospital, Southeast University (Nan**g): Haibo Qiu, Ling Liu; The First Affiliated Hospital of Anhui Medical University (Hefei): Rui Tang, **aoming Luo; Peking University People’s Hospital (Bei**g): Youzhong An, Huiying Zhao; Fourth Affiliated Hospital of Harbin Medical University (Harbin): Yan Gao, Zhe Zhai; Nan**g Jiangbei Peoples Hospital Affiliated To Medical School of Southeast University (Nan**g): Zheng L Ye, Wei Wang; The First Affiliated Hospital of Dalian Medical University (Dalian): Wenwen Li, Qingdong Li; Subei Peoples Hospital of Jiangsu Province (Yanghzou): Ruiqiang Zheng; **ling Hospital (Nan**g): Wenkui Yu, Juanhong Shen; Urumqi General Hospital (Urumqi): **nyu Li; Intensive Care Unit, First Affiliated Hospital of Wanna Medical College, Yijishan Hospital, (Wuhu): Tao Yu, Weihua Lu; Sichuan Provincial Peoples Hospital (Chengdu): Ya Q Wu, **ao B Huang; Hainan Province Peoples Hospital (Haikou): Zhenyang He; Peoples Hospital of Jiangxi Province (Nanchang): Yuanhua Lu; Qilu Hospital of Shandong University (**an): Hui Han, Fan Zhang; Zhejiang Provincial Peoples Hospital (Hangzhou): Renhua Sun; The First Affiliated Hospital of Bengbu Medical College (Bengbu, Anhui): Hua X Wang, Shu H Qin; Nan**g Municipal Government Hospital (Nan**g): Bao H Zhu, Jun Zhao; The First Hospital of Lanzhou University (Lanzhou): Jian Liu, Bin Li; The First Affiliated Hospital of Chongqing University of Medical Science (Chongqing): **g L Liu, Fa C Zhou; Xuzhou Central Hospital, Jiangsu Province, China (Xuzhou): Qiong J Li, **ng Y Zhang; The First Peoples Hospital of Foshan (Foshan): Zhou Li-**n, Qiang **n-Hua; The First Affiliated Hospital of Guangxi Medical University (Nanning): Liangyan Jiang; Renji Hospital,Shanghai Jiao Tong University School of Medicine (Shanghai): Yuan N Gao, **an Y Zhao; First Hospital of Shanxi Medical University (Taiyuan): Yuan Y Li, **ao L Li; Shandong Provincial Hospital (**an): Chunting Wang, Qingchun Yao; Fujian Provincial Hospital (Fuzhou): Rongguo Yu, Kai Chen; Henan Provincial People’s Hospital (Zhengzhou): Huanzhang Shao, Bingyu Qin; The Second Affiliated Hospital of Kunming Medical University (Kunming City): Qing Q Huang, Wei H Zhu; ** Qin; Jiangsu Province Hospital (Nan**g): Yi Han, Suming Zhou; COLOMBIA: Fundación Valle Del Lili (Cali): Monica P Vargas; COSTA RICA: Hospital San Juan De Dios (San José): Juan I Silesky Jimenez, Manuel A González Rojas; Hospital San Juan De Dios (San José): Jaime E Solis-Quesada, Christian M Ramirez-Alfaro; CZECH REPUBLIC: University Hospital of Ostrava (Ostrava): Jan Máca, Peter Sklienka; DENMARK: Aarhus Universitetshospital (Aarhus N): Jakob Gjedsted, Aage Christiansen; Rigshopitalet: Jonas Nielsen; ECUADOR: Hospital Militar (Quito): Boris G Villamagua, Miguel Llano; FRANCE: Clinique du Millenaire (Montpellier): Philippe Burtin, Gautier Buzancais; Centre Hospitalier (Roanne): Pascal Beuret, Nicolas Pelletier; CHU d’Angers (Angers): Satar Mortaza, Alain Mercat; Hôpital Marc Jacquet (Melun): Jonathan Chelly, Sébastien Jochmans; CHU Caen (Caen): Nicolas Terzi, Cédric Daubin; Henri Mondor Hospital (Créteil): Guillaume Carteaux, Nicolas de Prost; Cochin Hospital (Paris): Jean-Daniel Chiche, Fabrice Daviaud; Hôpital Tenon (Paris): Tai Pham, Muriel Fartoukh; CH Mulhouse-Emile Muller (Mulhouse): Guillaume Barberet, Jerome Biehler; Archet 1 University Hospital (Nice): Jean Dellamonica, Denis Doyen; Hopital Sainte Musse (Toulon): Jean-Michel Arnal, Anais Briquet; Hopital Nord - Réanimation des Détresses Respiratoires et Infections Sévères (Marseille): Sami Hraiech, Laurent Papazian; HEGP (Paris): Arnaud Follin; Louis Mourier Hospital (Colombes): Damien Roux, Jonathan Messika; Centre Hospitalier de Dax (Dax): Evangelos Kalaitzis; Réanimation Médicale, GH Pitié-Salpêtrière (Paris) : Laurence Dangers, Alain Combes; Ap-Hp Ambroise Paré (Boulogne-Billancourt): Siu-Ming Au; University Hospital Rouen (Rouen): Gaetan Béduneau, Dorothée Carpentier; CHU Amiens (Amiens - Salouel): Elie H Zogheib, Herve Dupont; Centre Hospitalier Intercommunal Robert Ballanger (Aulnay Sous Bois): Sylvie Ricome, Francesco L Santoli; Centre Hospitalier René Dubos (Pontoise): Sebastien L Besset; CHI Portes de l’Oise (Beaumont Sur Oise): Philippe Michel, Bruno Gelée; Archet 2 University Hospital (Nice): Pierre-Eric Danin, Bernard Goubaux; Centre Hospitalier Pierre Oudot (Bourgoin Jallieu): Philippe J Crova, Nga T Phan; CH Dunkerque (Dunkerque): Frantz Berkelmans; Centre Hospitalier de Belfort Montbéliard (Belfort): Julio C Badie, Romain Tapponnier; Centre Hospitalier Emile Muller (Mulhouse): Josette Gally, Samy Khebbeb; Hôpital de Hautepierre-Hôpitaux Universitaires de Strasbourg (Strasbourg): Jean-Etienne Herbrecht, Francis Schneider; Centre Hospitalier de Dieppe (Dieppe): Pierre-Louis M Declercq, Jean-Philippe Rigaud; Bicetre (Le Kremin-Bicetre): Jacques Duranteau, Anatole Harrois; CHU Gabriel Montpied (Clermont-Ferrand): Russell Chabanne, Julien Marin; CHU Estaing (Clermont-Ferrand): Charlene Bigot, Sandrine Thibault; CHI Eure-Seine Evreux (Evreux): Mohammed Ghazi, Messabi Boukhazna; Centre Hospitalier de Châlons en Champagne (Châlons en Champagne): Salem Ould Zein; CH Beauvais (Beauvais): Jack R Richecoeur, Daniele M Combaux; Centre Hospitalier Le Mans (Le Mans): Fabien Grelon, Charlene Le Moal; Hôpital Fleyriat (Bourg en Bresse): Elise P Sauvadet, Adrien Robine; Hôpital Saint Louis (Paris): Virginie Lemiale, Danielle Reuter; Service de Pneumologie Pitié-Salpétrière (Paris): Martin Dres, Alexandre Demoule; Centre Hospitalier Gonesse (Gonesse): Dany Goldgran-Toledano; Hôpital Croix Rousse (Lyon): Loredana Baboi, Claude Guérin; GERMANY: St. Nikolaus-Stiftshospital (Andernach): Ralph Lohner; Fachkrankenhaus Coswig GmbH (Coswig): Jens Kraßler, Susanne Schäfer; University Hospital Frankfurt (Frankfurt am Main): Kai D Zacharowski, Patrick Meybohm; Department of Anaesthesia & Intensive Care Medicine, University Hospital of Leipzig (Leipzig): Andreas W Reske, Philipp Simon; Asklepios Klinik Langen (Langen): Hans-Bernd F Hopf, Michael Schuetz; Städtisches Krankenhaus Heinsberg (Heinsberg): Thomas Baltus; GREECE: Hippokrateion General Hospital of Athens (Athens): Metaxia N Papanikolaou, Theonymfi G Papavasilopoulou; Gh Ahepa (Thessaloniki): Giannis A Zacharas, Vasilis Ourailogloy; Hippokration General Hospital of Thessaloniki (Thessaloniki): Eleni K Mouloudi, Eleni V Massa; Hospital General of Kavala (Kavala): Eva O Nagy, Electra E Stamou; Papageorgiou General Hospital (Thessaloniki): Ellada V Kiourtzieva, Marina A Oikonomou; GUATEMALA: Hospital General De Enfermedades, Instituto Guatemalteco De Seguridad Social (Ciudad De Guatemala): Luis E Avila; Centro Médico Militar (Guatemala): Cesar A Cortez, Johanna E Citalán; INDIA: Deenanath Mangeshkar Hospital and Research Center (Pune): Sameer A Jog, Safal D Sable; Care Institute of Medical Sciences (CIMS) Hospital (Ahmedabad): Bhagyesh Shah; Sanjay Gandhi Postgraduate Institute of Medical Sciences (SGPGIMS) (Lucknow): Mohan Gurjar, Arvind K Baronia; Rajasthan Hospital (Ahmedabad): Mohammedfaruk Memon; National Institute of Mental Health and Neuro Sciences (NIMHANS) (Bangalore): Radhakrishnan Muthuchellappan, Venkatapura J Ramesh; Anaesthesiology Unit of the Kasturba Medical College & Dept of Respiratory Therapy, SHOAS, Manipal University (Manipal): Anitha Shenoy, Ramesh Unnikrishnan; Sanjeevan Hospital (Pune): Subhal B Dixit, Rachana V Rhayakar; Apollo Hospitals (Chennai): Nagarajan Ramakrishnan, Vallish K Bhardwaj; Medicine Unit of the Kasturba Medical College & Dept of Respiratory Therapy, SHOAS, Manipal University (Manipal): Heera L Mahto, Sudha V Sagar; G Kuppuswamy Naidu Memorial Hospital (Coimbatore): Vijayanand Palaniswamy, Deeban Ganesan; IRAN: NRITLD/Masih Daneshvari (Tehran): Seyed Mohammadreza Hashemian, Hamidreza Jamaati; Milad Hospital (Tehran): Farshad Heidari; IRELAND: St Vincent’s University Hospital (Dublin): Edel A Meaney, Alistair Nichol; Mercy University Hospital (Cork): Karl M Knapman, Donall O’Croinin; Cork University Hospital (Cork): Eimhin S Dunne, Dorothy M Breen; Galway University Hospital (Galway): Kevin P Clarkson, Rola F Jaafar; Beaumont Hospital (Dublin): Rory Dwyer, Fahd Amir; Mater Misericordiae University Hospital (Dublin): Olaitan O Ajetunmobi, Aogan C O’Muircheartaigh; Tallaght Hospital (Dublin): Colin S Black, Nuala Treanor; Saint James’s Hospital (Dublin): Daniel V Collins, Wahid Altaf; ITALY: Santa Maria delle Croci Hospital (Ravenna): Gianluca Zani, Maurizio Fusari; Arcispedale Sant’Anna Ferrara (Ferrara): Savino Spadaro, Carlo A Volta; Ospedale Profili (Fabriano) (An): Romano Graziani, Barbara Brunettini; Umberto I Nocera Inferiore (Nocera Inferiore Salerno): Salvatore Palmese; Azienda Ospedaliera San Paolo – Polo Universitario- Università degli Studi di Milano (Milan): Paolo Formenti, Michele Umbrello; Sant’Anna (San Fermo Della Battaglia (Co)): Andrea Lombardo; Spedali Civili Brescia (Brescia): Elisabetta Pecci, Marco Botteri; Fondazione Irccs Ca Granda, Ospedale Maggiore Policlinico (Milan): Monica Savioli, Alessandro Protti; University Campus Bio-Medico of Rome (Rome): Alessia Mattei, Lorenzo Schiavoni; Azienda Ospedaliera “Mellino Mellini” (Chiari (Bs)): Andrea Tinnirello, Manuel Todeschini; Policlinico P. Giaccone, University of Palermo (Palermo): Antonino Giarratano, Andrea Cortegiani; Niguarda Cà Granda Hospital (Milan): Sara Sher, Anna Rossi; A. Gemelli University Hospital (Rome): Massimo M Antonelli, Luca M Montini; Ospedale “Sandro Pertini” (Rome): Paolo Casalena, Sergio Scafetti; ISMeTT IRCCS UPMC (Palermo): Giovanna Panarello, Giovanna Occhipinti; Ospedale San Gerardo (Monza): Nicolò Patroniti, Matteo Pozzi; Santa Maria Della Scaletta (Imola): Roberto R Biscione, Michela M Poli; Humanitas Research Hospital (Rozzano): Ferdinando Raimondi, Daniela Albiero; Ospedale Desio - Ao Desio-Vimercate (Desio): Giulia Crapelli, Eduardo Beck; Pinetagrande Private Hospital (Castelvolturno): Vincenzo Pota, Vincenzo Schiavone; Irccs San Martino Ist (Genova): Alexandre Molin, Fabio Tarantino; Ospedale San Raffaele (Milano): Giacomo Monti, Elena Frati; Ospedali Riuniti Di Foggia (Foggia): Lucia Mirabella, Gilda Cinnella; Azienda Ospedaliera Luigi Sacco - Polo Universitario (Milano): Tommaso Fossali, Riccardo Colombo; A.O.U. Città della Salute e della Scienza di Torino (Turin): Pierpaolo Terragni Ilaria Pattarino; Università degli Studi di Pavia-Fondazione IRCCS Policlinico San Matteo (Pavia): Francesco Mojoli, Antonio Braschi; Ao Ospedale Civile Legnano (Legnano): Erika E Borotto; Arnas Ospedale Civico Di Cristina Benfratelli (Palermo): Andrea N Cracchiolo, Daniela M Palma; Azienda Ospedaliera Della Provincia Di Lecco - Ospedale “A. Manzoni” (Lecco): Francesco Raponi, Giuseppe Foti; A.O. Provincia Di Lecco - Ospedale Alessandro Manzoni (Lecco): Ettore R Vascotto, Andrea Coppadoro; Cliniche Universitarie Sassari (Sassari): Luca Brazzi, Leda Floris; IRCCS Policlinico San Matteo (Pavia): Giorgio A Iotti, Aaron Venti; JAPAN: Yokohama City University Hospital (Yokohama): Osamu Yamaguchi, Shunsuke Takagi; Toyooka Hospital (Toyooka City, Hyogo Prefecture): Hiroki N Maeyama; Chiba University Hospital (Chiba City): Eizo Watanabe, Yoshihiro Yamaji; Okayma University Hospital (Okayama): Kazuyoshi Shimizu, Kyoko Shiozaki; Japanese Foundation for Cancer Research, Cancer Institute Hospital, Department of Emergency Medicine and Critical Care (Tokyo): Satoru Futami; Ibaraki Prefectural Central Hospital (Kasama): Sekine Ryosuke; Tohoku University Hospital (Sendai-Shi): Koji Saito, Yoshinobu Kameyama; Tokyo Medical University Hachioji Medical Center (Hachioji, Tokyo): Keiko Ueno; Tokushima University Hospital (Tokushima): Masayo. Izawa, Nao Okuda; Maebashi Red Cross Hospital (Gunma Maebashi): Hiroyuki Suzuki, Tomofumi Harasawa; Urasoe General Hospital (Urasoe): Michitaka Nasu, Tadaaki Takada; Ohta General Hospital Foundation Ohta Nishinouchi Hospital (Fukushima): Fumihito Ito; Jichi Medical University Hospital (Shimotsuke): Shin - Nunomiya, Kansuke - Koyama; Mito Kyodo General Hospital, Tsukuba University Hospital Mito Medical Center (Mito): Toshikazu Abe; Sendai City Hospital (Sendai): Kohkichi Andoh, Kohei Kusumoto; Ja Hiroshima General Hospital (Hatsukaichi City, Hiroshima): Akira Hirata, Akihiro Takaba; Yokohama Rosai Hospital (Yokohama): Hiroyasu Kimura; Nagasaki University Hospital (Nagasaki): Shuhei Matsumoto, Ushio Higashijima; Niigata University Medical & Dental Hospital (Niigata): Hiroyuki Honda, Nobumasa Aoki; Mie University Hospital (Tsu, Mie): Hiroshi Imai; Yamaguchi University Hospital (Ube, Yamaguchi): Yasuaki Ogino, Ichiko Mizuguchi; Saiseikai Kumamoto Hospital (Kumamoto City): Kazuya Ichikado; Shinshu University School of Medecine (Matsumoto City): Kenichi Nitta, Katsunori Mochizuki; Kuki General Hospital (Kuki): Tomoaki Hashida; Kyoto Medical Center (Kyoto): Hiroyuki Tanaka; Fujita Health University (Toyoake): Tomoyuki Nakamura, Daisuke Niimi; Rakwakai Marutamachi Hospital (Kyoto): Takeshi Ueda; Osaka University Hospital (Suita City, Osaka Prefecture): Yozo Kashiwa, Akinori Uchiyama; LATVIA: Paul Stradins Clinical University Hospital (Riga): Olegs Sabelnikovs, Peteris Oss; LEBANON: Kortbawi Hospital (Jounieh): Youssef Haddad; MALAYSIA: Hospital Kapit (Kapit): Kong Y Liew; MEXICO: Instituto Nacional De Cancerología, México (Mexico City): Silvio A Ñamendys-Silva, Yves D Jarquin-Badiola; Hospital De Especialidades “Antonio Fraga Mouret” Centro Medico Nacional La Raza IMSS (Mexico City): Luis A Sanchez-Hurtado, Saira S Gomez-Flores; Hospital Regional 1° De Octubre (Mexico City): Maria C Marin, Asisclo J Villagomez; Hospital General Dr Manuel Gea Gonzalez (Mexico City): Jordana S Lemus, Jonathan M Fierro; Hospital General De Zona No. 1 Instituto Mexicano Del Seguro Social Tepic Nayarit (Tepic): Mavy Ramirez Cervantes, Francisco Javier Flores Mejia; Centro Medico Dalinde (Mexico D.F.): Dulce Dector, Dulce M Dector; Opd Hospital Civil De Guadalajara Hospital Juan I Menchaca (Guadalajara): Daniel R Gonzalez, Claudia R Estrella; Hospital Regional De Ciudad Madero Pemex (Ciudad Madero): Jorge R Sanchez-Medina, Alvaro Ramirez-Gutierrez; Centro Médico ABC (Mexico D.F.): Fernando G George, Janet S Aguirre; Hospital Juarez De Mexico (Mexico City): Juan A Buensuseso, Manuel Poblano; MOROCCO: Mohammed V University, University Teaching Ibn Sina Hospital (Rabat): Tarek Dendane, Amine Ali Zeggwagh; Hopital Militaire D’Instruction Mohammed V (Rabat): Hicham Balkhi; Errazi (Marrakech): Mina Elkhayari, Nacer Samkaoui; University Teaching Hospital Ibn Rushd (Casablanca): Hanane Ezzouine, Abdellatif Benslama; Hôpital des Spécialités de Rabat (HSR) (Rabat): Mourad Amor, Wajdi Maazouzi. NETHERLANDS: Tjongerschans (Heerenveen): Nedim Cimic, Oliver Beck; Cwz (Nijmegen): Monique M Bruns, Jeroen A Schouten; Rijnstate Hospital (Arnhem): Myra - Rinia, Monique Raaijmakers; Radboud Umc (Nijmegen): Leo M Heunks, Hellen M Van Wezel; Maastricht University Medical Centre (Maastricht): Serge J Heines, Ulrich Strauch; Catharinaziekenhuis (Eindhoven): Marc P Buise; Academic Medical Center (Amsterdam): Fabienne D Simonis, Marcus J Schultz; NEW ZEALAND: Tauranga Hospital (Tauranga): Jennifer C Goodson, Troy S Browne; Wellington Hospital (Wellington): Leanlove Navarra, Anna Hunt; Dunedin Hospital (Dunedin): Robyn A Hutchison, Mathew B Bailey; Auckland City Hospital (Auckland): Lynette Newby, Colin Mcarthur; Whangarei Base Hospital (Whangarei): Michael Kalkoff, Alex Mcleod; North Shore Hospital (Auckland): Jonathan Casement, Danielle J Hacking; NORWAY: Ålesund Hospital (Ålesund): Finn H Andersen, Merete S Dolva; Oslo University Hospital - Rikshospitalet Medical Centre (Oslo): Jon H Laake, Andreas Barratt-Due; Stavanger University Hospital (Stavanger): Kim Andre L Noremark, Eldar Søreide; Haukeland University Hospital (Bergen): Brit Å Sjøbø, Anne B Guttormsen; PERU: Hospital Nacional Edgardo Rebagliati Martins (Lima): Hector H Leon Yoshido; Clínica Ricardo Palma (Lima): Ronald Zumaran Aguilar, Fredy A Montes Oscanoa; PHILIPPINES: The Medical City (Pasig): Alain U Alisasis, Joanne B Robles; Chong Hua Hospital (Cebu): Rossini Abbie B Pasanting-Lim, Beatriz C Tan; POLAND: Warsaw University Hospital (Warsaw): Pawel Andruszkiewicz, Karina Jakubowska; PORTUGAL: Centro Hospitalar Da Cova Da Beira (Covilhã): Cristina M Coxo; Hospital Santa Maria, Chln (Lisboa): António M Alvarez, Bruno S Oliveira; Centro Hospitalar Trás-Os-Montes E Alto Douro - Hospital De S. Pedro -Vila Real (Vila Real): Gustavo M Montanha, Nelson C Barros; Hospital Beatriz Ângelo (Loures): Carlos S Pereira, António M Messias; Hospital De Santa Maria (Lisboa): Jorge M Monteiro; Centro Hospitalar Médio Tejo - Hospital De Abrantes (Abrantes): Ana M Araujo, Nuno T Catorze; Instituto Português De Oncologia De Lisboa (Lisboa): Susan M Marum, Maria J Bouw; Hospital Garcia De Orta (Almada): Rui M Gomes, Vania A Brito; Centro Hospitalar Do Algarve (Faro): Silvia Castro, Joana M Estilita; Hpp Hospital De Cascais (Alcabideche): Filipa M Barros; Hospital Prof. Doutor Fernando Fonseca Epe (Amadora): Isabel M Serra, Aurelia M Martinho; ROMANIA: Fundeni Clinical Institute (Bucharest): Dana R Tomescu, Alexandra Marcu; Emergency Clinical County Hospital Timisoara (Timisoara): Ovidiu H Bedreag, Marius Papurica; Elias University Emergency Hospital (Bucharest): Dan E Corneci, Silvius Ioan Negoita; RUSSIAN FEDERATION: University Hospital (Kemerovo): Evgeny Grigoriev; Krasnoyarsk Regional Hospital, Krasnoyarsk State Medical University (Krasnoyarsk): Alexey I Gritsan, Andrey A Gazenkampf; SAUDI ARABIA: GICU of PSMMC (Riyadh): Ghaleb Almekhlafi, Mohamad M Albarrak; SICU of PSMMC (Riyadh): Ghanem M Mustafa; King Faisal Hospital And Research Center (Riyadh): Khalid A Maghrabi, Nawal Salahuddin; King Fahad Hospital (Baha): Tharwat M Aisa; King Abdulaziz Medical City (Riyadh): Ahmed S Al Jabbary, Edgardo Tabhan; King Abdulaziz Medical City (Riyadh): Yaseen M Arabi, Olivia A Trinidad; King Abdulaziz Medical City (Riyadh): Hasan M Al Dorzi, Edgardo E Tabhan; SOUTH AFRICA: Charlotte Maxeke Johannesburg Academic Hospital (Johannesburg): Stefan Bolon, Oliver Smith; SPAIN: Hospital Sant Pau (Barcelona): Jordi Mancebo, Hernan Aguirre-Bermeo; Hospital Universitari Bellvitge (L Hospitalet De Llobregat (Barcelona)): Juan C Lopez-Delgado, Francisco Esteve; Hospital Son Llatzer (Palma De Mallorca): Gemma Rialp, Catalina Forteza; Sabadell Hospital, CIBER Enfermedades Respiratorias (Sabadell): Candelaria De Haro, Antonio Artigas; Hospital Universitario Central De Asturias (Oviedo): Guillermo M Albaiceta, Sara De Cima-Iglesias; Complejo Hospitalario Universitario A Coruña (A Coruña): Leticia Seoane-Quiroga, Alexandra Ceniceros-Barros; Hospital Universitario Miguel Servet (Zaragoza): Antonio L Ruiz-Aguilar, Luis M Claraco-Vega; Morales Meseguer University Hospital (Murcia): Juan Alfonso Soler, Maria del Carmen Lorente; Hospital Universitario del Henares (Coslada): Cecilia Hermosa, Federico Gordo; Complejo Asistencial De Palencia. Hospital Rio Carrión (Palencia): Miryam - Prieto-González, Juan B López-Messa; Fundación Jiménez Díaz (Madrid): Manuel P Perez, Cesar P Perez; Hospital Clínico Universitario Lozano Blesa (Zaragoza): Raquel Montoiro Allue; Hospital Verge de la Cinta (Tortosa): Ferran Roche-Campo, Marcos Ibañez-Santacruz; Hospital Universitario 12 De Octubre (Madrid): Susana - Temprano; Hospital Universitario Príncipe De Asturias (Alcalá De Henares, Madrid): Maria C Pintado, Raul De Pablo; Hospital Universitari Germans Trias I Pujol (Badalona): Pilar Ricart Aroa Gómez; Hospital Universitario Arnau De Vilanova De Lleida (Lleida): Silvia Rodriguez Ruiz, Silvia Iglesias Moles; Cst Terrassa (Barcelona): Mª Teresa Jurado, Alfons Arizmendi; Hospital Universitari Mútua Terrassa (Terrassa): Enrique A Piacentini; Hospital Universitario De Móstoles (Mostoles): Nieves Franco, Teresa Honrubia; Complejo Asistencial De Salamanca (Salamanca): Meisy Perez Cheng, Elena Perez Losada; Hospital General Universitario De Ciudad Real (Ciudad Real): Javier - Blanco, Luis J Yuste; Torrecardenas (Almeria): Cecilia Carbayo-Gorriz, Francisca G Cazorla-Barranquero; Hospital Universitario Donostia (San Sebastian): Javier G Alonso, Rosa S Alda; Hospital Universitario De Torrejón (Madrid): Ángela Algaba, Gonzalo Navarro; Hospital Universitario De La Princesa (Madrid): Enrique Cereijo, Esther Diaz-Rodriguez; Hospital Universitario Lucus Augusti (Lugo): Diego Pastor Marcos, Laura Alvarez Montero; Hospital Universitario Santa Lucia (Cartagena): Luis Herrera Para, Roberto Jimenez Sanchez; Hospital Universitario Severo Ochoa, Leganes (Madrid): Miguel Angel Blasco Navalpotro, Ricardo Diaz Abad; University Hospital of Ntra. Sra. De Candelaria (Santa Cruz De Tenerife): Raquel Montiel Gonz á lez, D á cil Parrilla Toribio; Hospital Universitario Marques De Valdecilla (Santander): Alejandro G Castro, Maria Jose D Artiga; Hospital Infanta Cristina (Parla, Madrid): Oscar Penuelas; Hospital General De Catalunya (Sant Cugat Del Valles): Tomas P Roser, Moreno F Olga; San Pedro De Alcántara (Cáceres): Elena Gallego Curto, Rocío Manzano Sánchez; Sant Joan De Reus (Reus): Vallverdu P Imma, Garcia M Elisabet; Hospital Joan XXIII (Tarragona): Laura Claverias, Monica Magret; Hospital Universitario De Getafe (Madrid): Ana M Pellicer, Lucia L Rodriguez; Hospital Universitario Río Hortega (Valladolid): Jesús Sánchez-Ballesteros, Ángela González-Salamanca; Hospital Arquitecto Marcide (Ferrol, La Coruña): Antonio G Jimenez, Francisco P Huerta; Hospital General Universitario Gregorio Marañón (Madrid): Juan Carlos J Sotillo Diaz, Esther Bermejo Lopez; Hospital General De Segovia (Segovia): David D Llinares Moya, Alec A Tallet Alfonso; Hospital General Universitario Reina Sofia (Murcia): Palazon Sanchez Eugenio Luis, Palazon Sanchez Cesar; Complejo Hospitalario Universitario De Albacete (Albacete): Sánchez I Rafael, Corcoles G Virgilio; Hospital Infanta Elena (Valdemoro): Noelia N Recio; SWEDEN: Sahlgrenska University Hospital (Gothenburg): Richard O Adamsson, Christian C Rylander; Karolinska University Hospital (Stockholm): Bernhard Holzgraefe, Lars M Broman; Akademiska Sjukhuset Uppsala (Uppsala): Joanna Wessbergh, Linnea Persson; Vrinnevisjukhuset (Norrkö**): Fredrik Schiöler, Hans Kedelv; Linko** University Hospital (Linkö**): Anna Oscarsson Tibblin, Henrik Appelberg; Skellefteå Lasarett (Skellefteå): Lars Hedlund, Johan Helleberg; Karolinska University Hospital Solna (Stockholm): Karin E Eriksson, Rita Glietsch; Umeå University Hospital (Umeå): Niklas Larsson, Ingela Nygren; Danderyd Hospital (Stockholm): Silvia L Nunes, Anna-Karin Morin; Lund University Hospital (Lund): Thomas Kander, Anne Adolfsson; SWITZERLAND: Chuv (Centre Hospitalier Universitaire Vaudois) (Lausanne): Lise Piquilloud; Hôpital neuchâtelois - La Chaux-De-Fonds (La Chaux-De-Fonds): Hervé O. Zender, Corinne Leemann-Refondini; TUNISIA: Hopital Taher Sfar Mahdia (Mahdia): Souheil Elatrous; University Hospital Farhat Hached Sousse (Sousse): Slaheddine Bouchoucha, Imed Chouchene; CHU F. Bourguiba (Monastir): Islem Ouanes; Mongi Slim University Hospital, La Marsa (La Marsa): Asma Ben Souissi, Salma Kamoun; TURKEY: Cerrahpasa Medical Faculty Emergency Intensive Care Unit (Istanbul): Oktay Demirkiran; Cerrahpasa Medical Faculty Sadi Sun Intensive Care Unit (Istanbul): Mustafa Aker, Emre Erbabacan; Uludag University Medical Faculty (Bursa): Ilkay Ceylan, Nermin Kelebek Girgin; Ankara University Faculty of Medicine, Reanimation 3rd level ICU (Ankara): Menekse Ozcelik, Necmettin Ünal; Ankara University Faculty of Medicine, 2nd level ICU-postoperative ICU (Ankara): Basak Ceyda Meco; Istanbul Kartal Egitim Ve Arastirma Hastanesi (Istanbul): Onat O Akyol, Suleyman S Derman; UK: Papworth Hospital (Cambridge): Barry Kennedy, Ken Parhar; Royal Glamorgan Hospital (Llantrisant): Latha Srinivasa; Royal Victoria Hospital-Belfast (Belfast): Lia McNamee, Danny McAuley; Jack Steinberg ICU of King’s College (London): Phil Hopkins, Clare Mellis; Frank Stansil ICU of King’s College Hospital (London): Vivek Kakar; Liver ICU of King’s College (London): Dan Hadfield; Christine Brown ICU of King’s College (London): Andre Vercueil; West Suffolk Hospital (Bury St Edmunds): Kaushik Bhowmick, Sally K Humphreys; Craigavon Area Hospital (Portadown): Andrew Ferguson, Raymond Mckee; Barts Health NHS Trust, Whipps Cross Hospital (Leytonstone): Ashok S Raj, Danielle A Fawkes; Kettering General Hospital, Foundation NHS Trust (Northamptonshire): Philip Watt, Linda Twohey; Barnet General Hospital (Barnet): Rajeev R JhaMatthew Thomas, Alex Morton, Varsha Kadaba; Rotherham General Hospital (Rotherham): Mark J Smith, Anil P Hormis; City Hospital, (Birmingham): Santhana G Kannan, Miriam Namih; Poole Hospital NHS Foundation Trust (Poole): Henrik Reschreiter, Julie Camsooksai; Weston General Hospital (Weston-Super-Mare): Alek Kumar, Szabolcs Rugonfalvi; Antrim Area Hospital (Antrim): Christopher Nutt, Orla O’Neill; Aintree University Hospital (Liverpool): Colette Seasman, Ged Dempsey; Northern General Hospital (Sheffield): Christopher J Scott, Helen E Ellis; John Radcliffe Hospital (Oxford): Stuart Mckechnie, Paula J Hutton; St Georges Hospital (London): Nora N Di Tomasso, Michela N Vitale; Hillingdon Hospital (Uxbridge): Ruth O Griffin, Michael N Dean; The Royal Bournemouth & Christchurch NHS Foundation Trust (Bournemouth, Dorset): Julius H Cranshaw, Emma L Willett; Guys and St Thomas NHS Foundation Trust (London): Nicholas Ioannou, Gstt Severe Respiratory Failure Service; Whittington Hospital (London): Sarah Gillis; Wexham Park Hospital (Slough): Peter Csabi; Western General Hospital (Edinburgh): Rosaleen Macfadyen, Heidi Dawson; Royal Preston Hospital (Preston): Pieter D Preez, Alexandra J Williams; Brighton and Sussex University Hospitals NHS Trust (Brighton): Owen Boyd, Laura Ortiz-Ruiz De Gordoa; East And North Herts NHS Trust (Stevenage): Jon Bramall, Sophie Symmonds; Barnsley Hospital (Barnsley): Simon K Chau, Tim Wenham; Prince Charles Hospital (Merthyr Tydfil): Tamas Szakmany, Piroska Toth-Tarsoly; University Hospital of South Manchester NHS Foundation Trust (Manchester): Katie H Mccalman, Peter Alexander; Harrogate District Hospital (Harrogate): Lorraine Stephenson, Thomas Collyer; East And North Herts NHS Trust (Welwyn Garden City): Rhiannon Chapman, Raphael Cooper; Western Infirmary (Glasgow): Russell M Allan, Malcolm Sim; Dumfries and Galloway Royal Infirmary (Dumfries): David W Wrathall, Donald A Irvine; Charing Cross Hospital (London): Kim S Zantua, John C Adams; Worcestershire Royal Hospital (Worcester): Andrew J Burtenshaw, Gareth P Sellors; Royal Liverpool University Hospital (Liverpool): Ingeborg D Welters, Karen E Williams; Royal Alexandra Hospital (Glasgow): Robert J Hessell, Matthew G Oldroyd; Morriston Hospital (Swansea): Ceri E Battle, Suresh Pillai; Frimley Park Hospital (Frimley): Istvan Kajtor, Mageswaran Sivashanmugavel; Altnagelvin Hospital (Derry): Sinead C O’Kane, Adrian Donnelly; Buckinghamshire Healthcare NHS Trust (High Wycombe, Buckinghamshire): Aniko D Frigyik, Jon P Careless; Milton Keynes Hospital (Milton Keynes): Martin M May, Richard Stewart; Ulster Hospital (Belfast): T John Trinder, Samantha J Hagan; University Hospital of Wales (Cardiff): Matt P Wise, Jade M Cole; Freeman Hospital (Newcastle Upon Tyne): Caroline C MacFie, Anna T Dowling; URUGUAY: Hospital Español (Montevideo): Javier Hurtado, Nicolás Nin; Cudam (Montevideo): Javier Hurtado; Sanatorio Mautone (Maldonado): Edgardo Nuñez; Sanatorio Americano (Montevideo): Gustavo Pittini, Ruben Rodriguez; Hospital De Clínicas (Montevideo): María C Imperio, Cristina Santos; Circulo Católico Obreros Uruguay- Sanatorio JPII (Montevido: Ana G. França, Alejandro EBEID; CASMU (Montevideo): Alberto Deicas, Carolina Serra; USA: Saint Louis University Hospital (St.Louis): Aditya Uppalapati, Ghassan Kamel; Beth Israel Deaconess Medical Center (Boston): Valerie M Banner-Goodspeed, Jeremy R Beitler; Memorial Medical Center (Springfield): Satyanarayana Reddy Mukkera, Shreedhar Kulkarni; Massachusetts General Hospital (Boston): Jarone Lee, Tomaz Mesar; University of Cincinnati Medical Center (Cincinnati): John O Shinn 3rd, Dina - Gomaa; Massachusetts General Hospital (Boston): Christopher Tainter, Jarone Lee; Massachusetts General Hospital (Boston): Tomaz Mesar, Jarone Lee; R Adams Cowley Shock Trauma Center (Baltimore): Dale J Yeatts, Jessica Warren; Intermountain Medical Center (Murray, Utah): Michael J Lanspa, Russel R Miller; Intermountain Medical Center (Murray, Utah): Colin K Grissom, Samuel M Brown; Mayo Clinic (Rochester): Philippe R Bauer; North Shore Medical Center (Salem): Ryan J Gosselin, Barrett T Kitch; Albany Medical Center (Albany): Jason E Cohen, Scott H Beegle; John H Stoger Hospital of Cook County (Chicago, Il): Renaud M Gueret, Aiman Tulaimat; Albany Medical Center (Albany): Shazia Choudry; University of Alabama at Birmingham (UAb) (Birmingham, AL): William Stigler, Hitesh Batra; Duke University Hospital (Durham): Nidhi G Huff; Iowa Methodist Medical Center (Des Moines, Iowa): Keith D Lamb, Trevor W Oetting; Surgical & Neurosciences Intensive Care Unit of the University of Iowa Hospitals and Clinics (Iowa City, Iowa): Nicholas M Mohr, Claine Judy; Medical Center of Louisiana at New Orleans (New Orleans, Louisiana): Shigeki Saito, Fayez M Kheir; Tulane University (New Orleans): Fayez Kheir; Critical Care Unit of the University of Iowa Hospitals And Clinics (Iowa City, Iowa): Adam B Schlichting, Angela Delsing; University of California, San Diego Medical Center (San Diego, Ca): Daniel R Crouch, Mary Elmasri; Uc San Diego Thornton Hospital (La Jolla): Daniel R Crouch, Dina Ismail; University Hospital (Cincinnati): Kyle R Dreyer, Thomas C Blakeman; University Hospital (Cincinnati): Kyle R Dreyer, Dina Gomaa; Tower 3B Medical ICU of Brigham and Women’s Hospital (Boston): Rebecca M Baron, Carolina Quintana Grijalba; Tower 8C Burn/Trauma ICU of Brigham and Women’s Hospital (Boston): Peter C Hou; Tower 8D Surgical ICU of Brigham and Women’s Hospital (Boston): Raghu Seethala; Tower 9C Neurosurgical ICU of Brigham and Women’s Hospital (Boston): Imo Aisiku; Tower 9D Neurological ICU of Brigham and Women’s Hospital (Boston): Galen Henderson; Tower 11C Thoracic ICU of Brigham and Women’s Hospital (Boston): Gyorgy Frendl; Shapiro 6W Cardiac Surgery ICU of Brigham and Women’s Hospital (Boston): Sen-Kuang Hou; Shapiro 9E Coronary Care Unit of Brigham and Women’s Hospital (Boston): Robert L Owens, Ashley Schomer; SERBIA: Clinical Center of Serbia (Belgrade): Vesna Bumbasirevic, Bojan Jovanovic; Military Medical Academy (Belgrade): Maja Surbatovic, Milic Veljovic.
Funding
This work was funded and supported by the European Society of Intensive Care Medicine (ESICM), Brussels, Belgium, by St Michael’s Hospital, Toronto, Canada, and by the University of Milan-Bicocca, Monza, Italy.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Role of the funders
The ESICM provided support in data collection and study coordination. ESICM, St Michael’s Hospital, and University of Milan-Bicocca had no role in the design and conduct of the study; management, analysis, and interpretation of the data; preparation, review, or approval of the manuscript; or decision to submit the manuscript for publication.
Conflicts of interest
The authors attest that they have no conflicts of interest in regard to the subject of this manuscript.
Additional information
Marcus J. Schultz and John G. Laffey are the Joint senior Authors.
LUNG SAFE Investigators and the ESICM Trials Group collaborators members are listed in the Acknowledgments section.
Electronic supplementary material
Below is the link to the electronic supplementary material.
134_2018_5152_MOESM2_ESM.jpg
Fig. e1: Evolution of ventilator management from day 1 to day 2 of ARDS. Boxplots of the tidal volume (A), PEEP (B), and PIP (C) on day 1 compared to day 2 of ARDS. The study population is stratified according to ARDS severity at day 2.* P < 0.05, day 2 compared to day 1
134_2018_5152_MOESM3_ESM.jpg
Fig. e2: Use of protective ventilation on day 1 and day 2 of ARDS. Distribution of day 1 (A) and day 2 (B) for tidal volume and plateau pressure for each patient with confirmed ARDS. Patients with mild, moderate, and severe ARDS were represented with green, orange, and red dots, respectively. ARDS severity was assessed to day 1 in A and to day 2 in B
134_2018_5152_MOESM4_ESM.jpg
Fig. e3: Hospital survival probability in ARDS patients classified by ARDS severity on day 1 and on day 2 (Kaplan–Meier approach). A–C represents survival probability during hospital stay in patients with mild, moderate, and severe ARDS, respectively, as classified on day 1, with each panel then stratified according to ARDS severity assessed at day 2. The survival probability of patients with mild (n = 635, A), moderate (n = 993, B), and severe (n = 486, C) ARDS on day 1 was significantly different on the basis of their severity classification on day 2. D–F represents survival probability during hospital stay in patients with mild, moderate, and severe ARDS, respectively, as classified on day 2, with each panel stratified according to severity assessed on day 1. No statistically significant difference is demonstrated in patients with mild (n = 546, D), moderate (n = 825, E), or severe (n = 240, F) ARDS. Note: time and probabilities were calculated starting from the second day of ARDS
134_2018_5152_MOESM5_ESM.jpg
Fig. e4: Receiver operating curves to evaluate ARDS classification on day 1 and on day 2 as a predictor of hospital mortality. To compare the predictive value for hospital mortality of day 2 and day 1 ARDS classification using the Berlin definition, the area under the receiver operating curve (AUROC) was estimated by two logistic regression models, adjusted for demographical and clinical factors measured at day 1. First model (black line) considered ARDS classification on day 1 (mild, moderate, severe) as independent variables. Second model (red line) considered ARDS classification on day 2 as independent variables (resolved, mild, moderate, and severe). There was a small, but statistically significant, increase in the AUROC for day 2 compared to day 1
Rights and permissions
About this article
Cite this article
Madotto, F., Pham, T., Bellani, G. et al. Resolved versus confirmed ARDS after 24 h: insights from the LUNG SAFE study. Intensive Care Med 44, 564–577 (2018). https://doi.org/10.1007/s00134-018-5152-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-018-5152-6