Abstract
Purpose
Greater neighborhood greenspace has been associated with brain health, including better cognition and lower odds of Alzheimer’s disease in older adults. We investigated associations between neighborhood greenspace and brain-based magnetic resonance imaging (MRI) measures and potential effect modification by sex or apolipoprotein E genotype (APOE), a risk factor for Alzheimer’s disease.
Methods
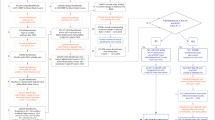
We obtained a sample of non-demented participants 65 years or older (n = 1125) from the longitudinal, population-based Cardiovascular Health Study (CHS). Greenspace data were derived from the National Land Cover Dataset. Adjusted multivariable linear regression estimated associations between neighborhood greenspace five years prior to the MRI and left and right hippocampal volume and 10-point grades of ventricular size and burden of white matter hyperintensity. Interaction terms tested effect modification by APOE genotype and sex. CHS data (1989–1999) were obtained/analyzed in 2020.
Results
Participants were on average 79 years old [standard deviation (SD) = 4], 58% were female, and 11% were non-white race. Mean neighborhood greenspace was 38% (SD = 28%). Greater proportion of greenspace in the neighborhood five years before MRI was borderline associated with lower ventricle grade (estimate: − 0.30; 95% confidence interval: − 0.61, 0.00). We observed no associations between greenspace and the other MRI outcome measures and no evidence of effect modification by APOE genotype and sex.
Conclusion
This study suggests a possible association between greater greenspace and less ventricular enlargement, a measure reflecting global brain atrophy. If confirmed in other longitudinal cohort studies, interventions and policies to improve community greenspaces may help to maintain brain health in older age.

Similar content being viewed by others
Code availability
Not applicable.
References
Clarke PJ, Ailshire JA, House JS, Morenoff JD, King K, Melendez R, Langa KM (2012) Cognitive function in the community setting: the neighbourhood as a source of “cognitive reserve”? J Epidemiol Community Health 66(8):730–736. https://doi.org/10.1136/jech.2010.128116
Wu YT, Prina AM, Jones AP, Barnes LE, Matthews FE, Brayne C, Study MRCCF, Ageing (2015) Community environment, cognitive impairment and dementia in later life: results from the Cognitive Function and Ageing Study. Age Ageing 44(6):1005–1011. https://doi.org/10.1093/ageing/afv137
Brown SC, Perrino T, Lombard J, Wang K, Toro M, Rundek T, Gutierrez CM, Dong C, Plater-Zyberk E, Nardi MI, Kardys J, Szapocznik J (2018) Health disparities in the relationship of neighborhood greenness to mental health outcomes in 249,405 U.S. medicare beneficiaries. Int J Environ Res Public Health. https://doi.org/10.3390/ijerph15030430
Cherrie MPC, Shortt NK, Mitchell RJ, Taylor AM, Redmond P, Thompson CW, Starr JM, Deary IJ, Pearce JR (2018) Green space and cognitive ageing: A retrospective life course analysis in the Lothian Birth Cohort 1936. Soc Sci Med 196:56–65. https://doi.org/10.1016/j.socscimed.2017.10.038
de Keijzer C, Gascon M, Nieuwenhuijsen MJ, Dadvand P (2016) Long-term green space exposure and cognition across the life course: a systematic review. Curr Environ Health Rep 3(4):468–477. https://doi.org/10.1007/s40572-016-0116-x
de Keijzer C, Tonne C, Basagana X, Valentin A, Singh-Manoux A, Alonso J, Anto JM, Nieuwenhuijsen MJ, Sunyer J, Dadvand P (2018) Residential surrounding greenness and cognitive decline: a 10-year follow-up of the Whitehall II Cohort. Environ Health Perspect 126(7):077003. https://doi.org/10.1289/ehp2875
Dadvand P, Nieuwenhuijsen MJ, Esnaola M, Forns J, Basagana X, Alvarez-Pedrerol M, Rivas I, Lopez-Vicente M, De Castro PM, Su J, Jerrett M, Querol X, Sunyer J (2015) Green spaces and cognitive development in primary schoolchildren. Proc Natl Acad Sci USA 112(26):7937–7942. https://doi.org/10.1073/pnas.1503402112
Dadvand P, Pujol J, Macia D, Martinez-Vilavella G, Blanco-Hinojo L, Mortamais M, Alvarez-Pedrerol M, Fenoll R, Esnaola M, Dalmau-Bueno A, Lopez-Vicente M, Basagana X, Jerrett M, Nieuwenhuijsen MJ, Sunyer J (2018) The association between lifelong greenspace exposure and 3-dimensional brain magnetic resonance imaging in Barcelona schoolchildren. Environ Health Perspect 126(2):027012. https://doi.org/10.1289/ehp1876
Dadvand P, Tischer C, Estarlich M, Llop S, Dalmau-Bueno A, Lopez-Vicente M, Valentin A, de Keijzer C, Fernandez-Somoano A, Lertxundi N, Rodriguez-Dehli C, Gascon M, Guxens M, Zugna D, Basagana X, Nieuwenhuijsen MJ, Ibarluzea J, Ballester F, Sunyer J (2017) lifelong residential exposure to green space and attention: a population-based prospective study. Environ Health Perspect 125(9):097016. https://doi.org/10.1289/ehp694
Hartig T, Mitchell R, de Vries S, Frumkin H (2014) Nature and health. Annu Rev Public Health 35:207–228. https://doi.org/10.1146/annurev-publhealth-032013-182443
Crowe CL, Kannoth S, Andrews H, Strogatz D, Li G, DiGuiseppi C, Hill L, Eby DW, Molnar LJ, Mielenz TJ (2020) Associations of frailty status with low-mileage driving and driving cessation in a cohort of older drivers. Geriatrics (Basel). https://doi.org/10.3390/geriatrics5010019
Cherrie MPC, Shortt NK, Ward Thompson C, Deary IJ, Pearce JR (2019) Association between the activity space exposure to parks in childhood and adolescence and cognitive aging in later life. Int J Environ Res Public Health. https://doi.org/10.3390/ijerph16040632
Yuchi W, Sbihi H, Davies H, Tamburic L, Brauer M (2020) Road proximity, air pollution, noise, green space and neurologic disease incidence: a population-based cohort study. Environ Health Glob Access Sci Source 19(1):8. https://doi.org/10.1186/s12940-020-0565-4
Zhu A, Yan L, Shu C, Zeng Y, Ji JS (2020) APOE epsilon4 modifies effect of residential greenness on cognitive function among older adults: a longitudinal analysis in China. Sci Rep 10(1):82. https://doi.org/10.1038/s41598-019-57082-7
Zijlema WL, Triguero-Mas M, Smith G, Cirach M, Martinez D, Dadvand P, Gascon M, Jones M, Gidlow C, Hurst G, Masterson D, Ellis N, van den Berg M, Maas J, van Kamp I, van den Hazel P, Kruize H, Nieuwenhuijsen MJ, Julvez J (2017) The relationship between natural outdoor environments and cognitive functioning and its mediators. Environ Res 155:268–275. https://doi.org/10.1016/j.envres.2017.02.017
Besser LM, Hirsch J, Galvin JE, Renne J, Park J, Evenson KR, Kaufman JD, Fitzpatrick AL (2020) Associations between neighborhood park space and cognition in older adults vary by US location: the multi-ethnic study of atherosclerosis. Health Place 66:102459
Slawsky E (2019) An evaluation of greenspace exposure as a protective factor in dementia risk among U.S. adults 75 years or older. University of Washington, Seattle, WA
Wang D, Lau KK, Yu R, Wong SYS, Kwok TTY, Woo J (2017) Neighbouring green space and mortality in community-dwelling elderly Hong Kong Chinese: a cohort study. BMJ open 7(7):e015794. https://doi.org/10.1136/bmjopen-2016-015794
Wu YT, Prina AM, Jones A, Matthews FE, Brayne C, Collaboration MRCCF, Study A (2017) The built environment and cognitive disorders: results from the cognitive function and ageing study II. Am J Prev Med. https://doi.org/10.1016/j.amepre.2016.11.020
Wu YT, Prina AM, Jones AP, Barnes LE, Matthews FE, Brayne C, Medical Research Council Cognitive F, Ageing S (2015) Community environment, cognitive impairment and dementia in later life: results from the Cognitive Function and Ageing Study. Age Ageing 44(6):1005–1011. https://doi.org/10.1093/ageing/afv137
Yu R, Wang D, Leung J, Lau K, Kwok T, Woo J (2018) Is Neighborhood Green Space Associated With Less Frailty? Evidence From the Mr. and Ms. Os (Hong Kong) Study. J Am Med Directors Assoc 19(6):528–534. https://doi.org/10.1016/j.jamda.2017.12.015
Kirk-Sanchez NJ, McGough EL (2014) Physical exercise and cognitive performance in the elderly: current perspectives. Clin Interv Aging 9:51–62. https://doi.org/10.2147/CIA.S39506
Lupien SJ, Maheu F, Tu M, Fiocco A, Schramek TE (2007) The effects of stress and stress hormones on human cognition: Implications for the field of brain and cognition. Brain Cogn 65(3):209–237. https://doi.org/10.1016/j.bandc.2007.02.007
Barnes DE, Alexopoulos GS, Lopez OL, Williamson JD, Yaffe K (2006) Depressive symptoms, vascular disease, and mild cognitive impairment: findings from the Cardiovascular Health Study. Arch Gen Psychiatry 63(3):273–279. https://doi.org/10.1001/archpsyc.63.3.273
Ribeiro AI, Pires A, Carvalho MS, Pina MF (2015) Distance to parks and non-residential destinations influences physical activity of older people, but crime doesn’t: a cross-sectional study in a southern European city. BMC Public Health 15:593. https://doi.org/10.1186/s12889-015-1879-y
Sugiyama T, Shibata A, Koohsari MJ, Tanamas SK, Oka K, Salmon J, Dunstan DW, Owen N (2015) Neighborhood environmental attributes and adults’ maintenance of regular walking. Med Sci Sports Exerc 47(6):1204–1210. https://doi.org/10.1249/MSS.0000000000000528
Wu YT, Prina AM, Jones A, Matthews FE, Brayne C, Mrc C (2015) Older people, the natural environment and common mental disorders: cross-sectional results from the Cognitive Function and Ageing Study. BMJ Open 5(9):e007936. https://doi.org/10.1136/bmjopen-2015-007936
Pun VC, Manjourides J, Suh HH (2018) Association of neighborhood greenness with self-perceived stress, depression and anxiety symptoms in older U.S adults. Environ Health 17(1):39. https://doi.org/10.1186/s12940-018-0381-2
Sarkar C, Webster C, Gallacher J (2018) Residential greenness and prevalence of major depressive disorders: a cross-sectional, observational, associational study of 94 879 adult UK Biobank participants. Lancet Planet Health 2(4):e162–e173. https://doi.org/10.1016/S2542-5196(18)30051-2
Cleary EG, Cifuentes M, Grinstein G, Brugge D, Shea TB (2018) Association of low-level ozone with cognitive decline in older adults. J Alzheimers Dis 61(1):67–78. https://doi.org/10.3233/JAD-170658
Tonne C, Elbaz A, Beevers S, Singh-Manoux A (2014) Traffic-related air pollution in relation to cognitive function in older adults. Epidemiology 25(5):674–681. https://doi.org/10.1097/EDE.0000000000000144
Barwise Y, Kumar P (2020) Designing vegetation barriers for urban air pollution abatement: a practical review for appropriate plant species selection. Npj Clim Atmos Sci. https://doi.org/10.1038/s41612-020-0115-3
Cerin E, Baranowski T, Barnett A, Butte N, Hughes S, Lee RE, Mendoza JA, Thompson D, O’Connor TM (2016) Places where preschoolers are (in)active: an observational study on Latino preschoolers and their parents using objective measures. Int J Behav Nutr Phys Act 13:29. https://doi.org/10.1186/s12966-016-0355-0
Chaddock-Heyman L, Erickson KI, Voss MW, Powers JP, Knecht AM, Pontifex MB, Drollette ES, Moore RD, Raine LB, Scudder MR, Hillman CH, Kramer AF (2013) White matter microstructure is associated with cognitive control in children. Biol Psychol 94(1):109–115. https://doi.org/10.1016/j.biopsycho.2013.05.008
Krafft CE, Schaeffer DJ, Schwarz NF, Chi L, Weinberger AL, Pierce JE, Rodrigue AL, Allison JD, Yanasak NE, Liu T, Davis CL, McDowell JE (2014) Improved frontoparietal white matter integrity in overweight children is associated with attendance at an after-school exercise program. Dev Neurosci 36(1):1–9. https://doi.org/10.1159/000356219
Chandrabose M, Rachele JN, Gunn L, Kavanagh A, Owen N, Turrell G, Giles-Corti B, Sugiyama T (2019) Built environment and cardio-metabolic health: systematic review and meta-analysis of longitudinal studies. Obes Rev 20(1):41–54. https://doi.org/10.1111/obr.12759
Fletcher E, Gavett B, Harvey D, Farias ST, Olichney J, Beckett L, DeCarli C, Mungas D (2018) Brain volume change and cognitive trajectories in aging. Neuropsychology 32(4):436–449. https://doi.org/10.1037/neu0000447
Nestor SM, Rupsingh R, Borrie M, Smith M, Accomazzi V, Wells JL, Fogarty J, Bartha R, Alzheimer’s Disease Neuroimaging I (2008) Ventricular enlargement as a possible measure of Alzheimer’s disease progression validated using the Alzheimer’s disease neuroimaging initiative database. Brain 131(Pt 9):2443–2454. https://doi.org/10.1093/brain/awn146
Cerin E, Rainey-Smith SR, Ames D, Lautenschlager NT, Macaulay SL, Fowler C, Robertson JS, Rowe CC, Maruff P, Martins RN, Masters CL, Ellis KA (2017) Associations of neighborhood environment with brain imaging outcomes in the Australian Imaging Biomarkers and Lifestyle cohort. Alzheimers Dement 13(4):388–398. https://doi.org/10.1016/j.jalz.2016.06.2364
Kuhn S, Duzel S, Eibich P, Krekel C, Wustemann H, Kolbe J, Martensson J, Goebel J, Gallinat J, Wagner GG, Lindenberger U (2017) In search of features that constitute an “enriched environment” in humans: associations between geographical properties and brain structure. Sci Rep. https://doi.org/10.1038/s41598-017-12046-7
Apostolova LG, Green AE, Babakchanian S, Hwang KS, Chou YY, Toga AW, Thompson PM (2012) Hippocampal atrophy and ventricular enlargement in normal aging, mild cognitive impairment (MCI), and Alzheimer Disease. Alzheimer Dis Assoc Disord 26(1):17–27. https://doi.org/10.1097/WAD.0b013e3182163b62
Bangen KJ, Preis SR, Delano-Wood L, Wolf PA, Libon DJ, Bondi MW, Au R, DeCarli C, Brickman AM (2018) Baseline white matter hyperintensities and hippocampal volume are associated with conversion from normal cognition to mild cognitive impairment in the framingham offspring study. Alzheimer Dis Assoc Disord 32(1):50–56. https://doi.org/10.1097/WAD.0000000000000215
Fried LP, Borhani NO, Enright P, Furberg CD, Gardin JM, Kronmal RA, Kuller LH, Manolio TA, Mittelmark MB, Newman A et al (1991) The Cardiovascular Health Study: design and rationale. Ann Epidemiol 1(3):263–276. https://doi.org/10.1016/1047-2797(91)90005-w
Yue NC, Arnold AM, Longstreth WT Jr, Elster AD, Jungreis CA, O’Leary DH, Poirier VC, Bryan RN (1997) Sulcal, ventricular, and white matter changes at MR imaging in the aging brain: data from the cardiovascular health study. Radiology 202(1):33–39. https://doi.org/10.1148/radiology.202.1.8988189
Bryan RN, Manolio TA, Schertz LD, Jungreis C, Poirier VC, Elster AD, Kronmal RA (1994) A method for using MR to evaluate the effects of cardiovascular disease on the brain: the cardiovascular health study. AJNR Am J Neuroradiol 15(9):1625–1633
Kuller LH, Arnold AM, Longstreth WT Jr, Manolio TA, O’Leary DH, Burke GL, Fried LP, Newman AB (2007) White matter grade and ventricular volume on brain MRI as markers of longevity in the cardiovascular health study. Neurobiol Aging 28(9):1307–1315. https://doi.org/10.1016/j.neurobiolaging.2006.06.010
Raji CA, Lopez OL, Kuller LH, Carmichael OT, Becker JT (2009) Age, Alzheimer disease, and brain structure. Neurology 73(22):1899–1905. https://doi.org/10.1212/WNL.0b013e3181c3f293
Raji CA, Lopez OL, Kuller LH, Carmichael OT, Longstreth WT, Jr., Gach HM, Boardman J, Bernick CB, Thompson PM, Becker JT (2012) White matter lesions and brain gray matter volume in cognitively normal elders. Neurobiol Aging 33 (4):834 e837–816. doi:https://doi.org/10.1016/j.neurobiolaging.2011.08.010
Wickham J, Homer C, Vogelmann J, McKerrow A, Mueller R, Herold N, Coulston J (2014) The multi-resolution land characteristics (mrlc) consortium-20 years of development and integration of USA national land cover data. Remote Sens-Basel 6(8):7424–7441. https://doi.org/10.3390/rs6087424
Multi-Resolution Land Characteristics (MRLC) Consortium. https://www.mrlc.gov/. Accessed 03/28/2020
Yang Y, Diez-Roux AV (2012) Walking distance by trip purpose and population subgroups. Am J Prev Med 43(1):11–19. https://doi.org/10.1016/j.amepre.2012.03.015
Talen E (1998) Visualizing Fairness: Equity Maps for Planners. Journal of the American Planning Association 64:22–38
Kuller LH, Shemanski L, Manolio T, Haan M, Fried L, Bryan N, Burke GL, Tracy R, Bhadelia R (1998) Relationship between ApoE, MRI findings, and cognitive function in the Cardiovascular Health Study. Stroke 29(2):388–398. https://doi.org/10.1161/01.str.29.2.388
Taylor HL, Jacobs DR Jr, Schucker B, Knudsen J, Leon AS, Debacker G (1978) A questionnaire for the assessment of leisure time physical activities. J Chronic Dis 31(12):741–755. https://doi.org/10.1016/0021-9681(78)90058-9
Radloff LS (1977) The CES-D scale: a self-report depression scale for research in the general population. Appl Psychol Meas 1:385–401
Ives DG, Fitzpatrick AL, Bild DE, Psaty BM, Kuller LH, Crowley PM, Cruise RG, Theroux S (1995) Surveillance and ascertainment of cardiovascular events. Cardiovasc Health Study Ann Epidemiol 5(4):278–285. https://doi.org/10.1016/1047-2797(94)00093-9
Carmichael OT, Kuller LH, Lopez OL, Thompson PM, Dutton RA, Lu A, Lee SE, Lee JY, Aizenstein HJ, Meltzer CC, Liu Y, Toga AW, Becker JT (2007) Ventricular volume and dementia progression in the Cardiovascular Health Study. Neurobiol Aging 28(3):389–397. https://doi.org/10.1016/j.neurobiolaging.2006.01.006
Coupé P, Manjón JV, Lanuza E, Catheline G (2019) Lifespan changes of the human brain In Alzheimer’s Disease. Scientific reports 9:3998
Gernes R, Brokamp C, Rice GE, Wright JM, Kondo MC, Michael YL, Donovan GH, Gatziolis D, Bernstein D, LeMasters GK, Lockey JE, Khurana Hershey GK, Ryan PH (2019) Using high-resolution residential greenspace measures in an urban environment to assess risks of allergy outcomes in children. Sci Total Environ 668:760–767. https://doi.org/10.1016/j.scitotenv.2019.03.009
Graziose MM, Gray HL, Quinn J, Rundle AG, Contento IR, Koch PA (2016) Association between the built environment in school neighborhoods with physical activity among New York City Children, 2012. Prev Chronic Dis 13:E110. https://doi.org/10.5888/pcd13.150581
Sheline YI, Wang PW, Gado MH, Csernansky JG, Vannier MW (1996) Hippocampal atrophy in recurrent major depression. Proc Natl Acad Sci U S A 93(9):3908–3913. https://doi.org/10.1073/pnas.93.9.3908
Zhang W, He X, Liu S, Li T, Li J, Tang X, Lai S (2019) Neural correlates of appreciating natural landscape and landscape garden: Evidence from an fMRI study. Brain Behav 9(7):e01335. https://doi.org/10.1002/brb3.1335
Markevych I, Schoierer J, Hartig T, Chudnovsky A, Hystad P, Dzhambov AM, de Vries S, Triguero-Mas M, Brauer M, Nieuwenhuijsen MJ, Lupp G, Richardson EA, Astell-Burt T, Dimitrova D, Feng X, Sadeh M, Standl M, Heinrich J, Fuertes E (2017) Exploring pathways linking greenspace to health: Theoretical and methodological guidance. Environ Res 158:301–317. https://doi.org/10.1016/j.envres.2017.06.028
Hunter AJ, Luck GW (2015) Defining and measuring the social-ecological quality of urban greenspace: a semi-systematic review. Urban Ecosyst 18(4):1139–1163. https://doi.org/10.1007/s11252-015-0456-6
Acknowledgments
This research was supported by contracts HHSN268201200036C, HHSN268200800007C, HHSN268201800001C, N01HC55222, N01HC85079, N01HC85080, N01HC85081, N01HC85082, N01HC85083, N01HC85086, N01HC15103, and grants U01HL080295 and U01HL130114 from the National Heart, Lung, and Blood Institute (NHLBI), with additional contribution from the National Institute of Neurological Disorders and Stroke (NINDS). Additional support was provided by R01AG023629 and R01AG15928 from the National Institute on Aging (NIA). A full list of principal CHS investigators and institutions can be found at CHS-NHLBI.org. This work was supported by the National Institute of Aging (grants 1R01AG049970, 3R01AG049970-04S1), Commonwealth Universal Research Enhancement (C.U.R.E) program funded by the Pennsylvania Department of Health—2015 Formula award—SAP #4100072543, the Urban Health Collaborative at Drexel University, and the Built Environment and Health Research Group at Columbia University. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health. No authors have conflicts of interest to disclose and the following authors have funding support: Dr. Besser (NIH/NIA K01AG063895), Yvonne Michael (NIH/NIA 3R01AG049970-04S1), Phil Hurvitz NIH grants R01DK076608, R01CA178343, R01AG049970, R01DK114196, R01HD091089, R01NR016942), James Galvin (NIA/NIH Grants R01AG040211, R01NS101483.William Longstreth is co-investigator on several NIH-funded studies, including the CHS, and serves as a co-PI for the NIH-funded ARCADIA trial, which receives in-kind study drug from the BMS-Pfizer Alliance and ancillary funding from Roche Diagnostics
Funding
Lilah Besser is supported by NIH/NIA award K01AG063895. Yvonne Michael is supported by National Institute on Aging (3R01AG049970-04S1). Phil Hurvitz is supported by NIH grants R01DK076608, R01CA178343, R01AG049970, R01DK114196, R01HD091089, and R01NR016942. James Galvin is supported by NIA/NIH Grants R01AG040211 and R01NS101483. William Longstreth co-investigator on several NIH-funded studies, including the CHS, and serves as a co-PI for the NIH-funded ARCADIA trial. Jana Hirsch and Gina Lovasi are supported by the National Institute on Aging (1R01AG049970, 3R01AG049970-04S1), Commonwealth Universal Research Enhancement (C.U.R.E) program funded by the Pennsylvania Department of Health—2015 Formula award—SAP #4100072543, the Urban Health Collaborative at Drexel University, and the Built Environment and Health Research Group at Columbia University. The remaining authors have no funding to disclose.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest:
Lilah Besser has no conflict of interest. Gina Lovasi has no conflict of interest. Yvonne Michael has no conflict of interest. Parveen Garg has no conflict of interest. Jana Hirsch has no conflict of interest. David Siscovick has no conflict of interest. Phil Hurvitz has no conflict of interest. Mary Lou Biggs has no conflict of interest. James Galvin has no conflict of interest. Traci Bartz has no conflict of interest. William Longstreth serves as a co-PI for the NIH-funded ARCADIA trial, which receives in-kind study drug from the BMS-Pfizer Alliance and ancillary funding from Roche Diagnostics.
Availability of data
Researchers can request access to CHS data through the Cardiovascular Health Study, at https://chs-nhlbi.org/.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Besser, L.M., Lovasi, G.S., Michael, Y. et al. Associations between neighborhood greenspace and brain imaging measures in non-demented older adults: the Cardiovascular Health Study. Soc Psychiatry Psychiatr Epidemiol 56, 1575–1585 (2021). https://doi.org/10.1007/s00127-020-02000-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-020-02000-w