Abstract
Aims/hypothesis
Glucagon-like peptide 1 (GLP-1) receptors are expressed by pancreatic beta cells and GLP-1 receptor signalling promotes insulin secretion. GLP-1 receptor agonists have neural effects and are therapeutically promising for mild cognitive impairment and Alzheimer’s disease. Our previous results showed that insulin is released by neurogliaform neurons in the cerebral cortex, but the expression of GLP-1 receptors on insulin-producing neocortical neurons has not been tested. In this study, we aimed to determine whether GLP-1 receptors are present in insulin-containing neurons.
Methods
We harvested the cytoplasm of electrophysiologically and anatomically identified neurogliaform interneurons during patch-clamp recordings performed in slices of rat neocortex. Using single-cell digital PCR, we determined copy numbers of Glp1r mRNA and other key genes in neurogliaform cells harvested in conditions corresponding to hypoglycaemia (0.5 mmol/l glucose) and hyperglycaemia (10 mmol/l glucose). In addition, we performed whole-cell patch-clamp recordings on neurogliaform cells to test the effects of GLP-1 receptor agonists for functional validation of single-cell digital PCR results.
Results
Single-cell digital PCR revealed GLP-1 receptor expression in neurogliaform cells and showed that copy numbers of mRNA of the Glp1r gene in hyperglycaemia exceeded those in hypoglycaemia by 9.6 times (p < 0.008). Moreover, single-cell digital PCR confirmed co-expression of Glp1r and Ins2 mRNA in neurogliaform cells. Functional expression of GLP-1 receptors was confirmed with whole-cell patch-clamp electrophysiology, showing a reversible effect of GLP-1 on neurogliaform cells. This effect was prevented by pre-treatment with the GLP-1 receptor-specific antagonist exendin-3(9-39) and was absent in hypoglycaemia. In addition, single-cell digital PCR of neurogliaform cells revealed that the expression of transcription factors (Pdx1, Isl1, Mafb) are important in beta cell development.
Conclusions/interpretation
Our results provide evidence for the functional expression of GLP-1 receptors in neurons known to release insulin in the cerebral cortex. Hyperglycaemia increases the expression of GLP-1 receptors in neurogliaform cells, suggesting that endogenous incretins and therapeutic GLP-1 receptor agonists might have effects on these neurons, similar to those in pancreatic beta cells.
Similar content being viewed by others
Avoid common mistakes on your manuscript.

Introduction
Glucagon-like peptide 1 (GLP-1), produced by L cells of the intestine, is important in blood glucose homeostasis, acting through several classic mechanisms including the inhibition of gastric emptying, suppression of pancreatic glucagon secretion and enhancement of insulin release in the pancreas [1]. Direct action of circulating GLP-1 on G-protein-coupled GLP-1 receptors located on pancreatic beta cells leads to glucose-dependent closure of ATP-sensitive K+ channels, with subsequent depolarisation and Ca2+ influx, and Ca2+-dependent release of Ca2+ from intracellular Ca2+ stores, resulting in Ca2+-dependent insulin secretion [1]. It is of high clinical importance that GLP-1 reduces the concentrations of blood glucose only postprandially, when blood glucose levels exceed fasting concentrations [2]. Such glucose-dependent action means that intravenously administered GLP-1 does not result in hypoglycaemia and, consequently, the current treatment of type 2 diabetes mellitus includes GLP-1 receptor agonists as therapeutic agents.
Outside of the pancreas, circulating GLP-1 has additional targets that are linked to insulin synthesis. Native GLP-1 crosses the blood–brain barrier [1, 3] and, thus, it is possible for incretins arriving from the periphery, including GLP-1 produced by intestinal L cells and GLP-1 analogues prescribed in type 2 diabetes mellitus [4], to act on neurons of the hippocampus and the neocortex, which are known to express GLP-1 receptors [5, 6]. In addition, neurons in the brain might also receive GLP-1 from central sources, according to results showing GLP-1 expression in neurons located in the nucleus of the solitary tract in the brainstem [7, 8]. On the other hand, accumulating evidence based on experiments performed mostly in rats shows that insulin is synthesised by neurons of the cerebral cortex [9,10,11,12,13]. Neuron-derived insulin is effective in regulating synaptic and microcircuit activity in the rat neocortex [13] and is suggested to regulate on-demand energy homeostasis of neural networks [14].
Insulin delivered intranasally to the brain is therapeutically promising against mild cognitive impairment and Alzheimer’s disease [15], and the GLP-1 analogues used in diabetes treatment have preventive effects in the early stage of Alzheimer’s disease development [16, 17], Parkinson’s disease [16, 18] and traumatic brain injury [19, 20]. It has been recently hypothesised that novel therapeutic strategies might include modulation of neural insulin production in the brain by GLP-1 agonists in order to counteract diabetes, obesity and neurodegenerative diseases [14]. Therefore, it is of potential importance to determine whether GLP-1 of intestinal or neural origin or therapeutically applied GLP-1 receptor agonists find targets on neurons capable of insulin production. In the current study, we tested whether neurogliaform cells of the rat neocortex, shown to release insulin locally in the brain [13], have the molecular components to be involved in GLP-1 signalling.
Methods
Animals
All procedures were performed with the approval of the University of Szeged (no. I-74-8/2016) and in accordance with the Guide for the Care and Use of Laboratory Animals (2011) (http://grants.nih.gov/grants/olaw/guide-for-the-care-and-use-of-laboratory-animals.pdf). Male Wistar rats (n = 106, postnatal day 28–35, 190–220 g; Charles River, Isaszeg, Hungary) were kept in individually ventilated cages (0.25 m2) with biological bedding and ad libitum dry food and water.
Electrophysiology
Animals were anaesthetized by intraperitoneal injection of ketamine (30 mg/kg) and xylazine (10 mg/kg) and, following checking of the cessation of pain reflexes and decapitation, coronal slices (350 μm) were prepared from the somatosensory cortex. Animals used for this study also provided brain slices for other projects performed in parallel in the laboratory. Slice preparation and recordings were performed as previously described [13, 21]. Recordings were obtained at approximately 36°C from cells visualised in layers I–III by infrared differential interference contrast videomicroscopy, at depths 60–130 μm from the surface of the slice. Micropipettes (5–7 MΩ) were filled with an intracellular solution containing 126 mmol/l K-gluconate, 4 mmol/l KCl, 10 mmol/l HEPES, 10 mmol/l creatine phosphate and 8 mmol/l biocytin (pH 7.25, 300 mOsm), supplemented with RNase Inhibitor (1 U/μl, Life Technologies, Budapest, Hungary) to prevent any RNA degradation. Slices were preincubated in 0.5 mmol/l glucose for 4 h prior to recording sessions under hypoglycaemic conditions. Pre-treatment with exendin-3(9-39) (1 μmol/l; Tocris, Bristol, UK) was applied for 4 h prior to recording sessions under hyperglycaemic (10 mmol/l glucose) conditions. Access resistance was monitored with −10 mV voltage steps in between experimental epochs and neurons were excluded from data analysis if access resistance exceeded 35 MΩ. Signals were filtered at 8 kHz, digitised at 16 kHz and analysed with PULSE software (HEKA, Lambrecht/Pfalz, Germany). Traces shown are single sweeps for firing patterns.
Single-cell reverse transcription and digital PCR
At the end of electrophysiological recordings, the intracellular content was aspirated into recording pipettes by applying a gentle negative pressure while maintaining a tight seal [13, 21]. The pipettes were then delicately removed to allow outside-out patch formation and the content of the pipettes (~1.5 μl) was expelled into a low-adsorption test tube (Axygen, Corning, NY, USA) containing 0.5 μl SingleCellProtect (Avidin, Szeged, Hungary) solution in order to prevent nucleic acid degradation and to be compatible with direct reverse transcription reactions. Samples were snap-frozen in liquid nitrogen and stored or immediately used for reverse transcription. Reverse transcription of the harvested cytoplasm was carried out in two steps. The first step was performed for 5 min at 65°C in a total reaction volume of 5 μl, containing 2 μl intracellular solution and SingleCellProtect, mixed with the cytoplasmic contents of the neuron, 0.3 μl TaqMan reagent, 0.3 μl 10 mmol/l deoxynucleotide triphosphates (dNTPs), 1 μl 5X first-strand buffer, 0.3 μl 0.1 mol/l dithiothreitol, 0.3 μl RNase Inhibitor (Life Technologies) and 100 U reverse transcriptase (SuperScript III; Invitrogen, Carlsbad, CA, USA). The second step of the reaction was carried out at 55°C for 1 h, following which the reaction was stopped by heating at 75°C for 15 min. The reverse transcription reaction mix was stored at −20°C until PCR amplification.
For digital PCR analysis, half of the reverse transcription reaction mixture (2.5 μl), 2 μl TaqMan reagent (Life Technologies), 10 μl OpenArray Digital PCR Master Mix (Life Technologies) and nuclease-free water (5.5 μl) were mixed, for a total volume of 20 μl. Processing of the OpenArray slide, cycling in the OpenArray NT cycler and data analysis were performed as previously described [13, 21]. For our digital PCR protocol for amplification, reactions with Ct confidence values <100 were considered not different from background noise and were excluded from the dataset. In addition, reactions with Ct values <23 were considered primer dimers and those >33 were considered false reactions originated from non-template amplifications and were excluded from the dataset.
Histology and reconstruction of neurons
Following electrophysiological recordings, slices were immersed in fixative containing 4% (wt/vol.) paraformaldehyde, 15% (vol./vol.) saturated picric acid and 1.25% (vol./vol.) glutaraldehyde in 0.1 mol/l phosphate buffer (pH 7.4; Sigma-Aldrich, Saint Louis, MO, USA), at 4°C for at least 12 h. After several washes with 0.1 mol/l phosphate buffer, slices were frozen in liquid nitrogen and then thawed in 0.1 mol/l phosphate buffer, embedded in 10% (wt/vol.) gelatine and further sectioned into 60 μm slices. Sections were incubated in a solution of conjugated avidin–biotin horseradish peroxidase (1:100; Vector Labs, Burlingame, CA, USA) in Tris-buffered saline (pH 7.4) at 4°C overnight. The enzyme reaction was revealed by 3′3-diaminobenzidine tetrahydrochloride (0.05% wt/vol.) as the chromogen and 0.01% (vol./vol.) H2O2 as the oxidant. Sections were post-fixed with 1% OsO4 (wt/vol.) in 0.1 mol/l phosphate buffer. After several washes in distilled water, sections were stained in 1% (wt/vol.) uranyl acetate and dehydrated using an ascending series of ethanol. Sections were infiltrated with epoxy resin (Durcupan; Sigma-Aldrich) overnight and embedded on glass slides. Three-dimensional light microscopic reconstructions were carried out using the Neurolucida system (MicroBrightField, Williston, VT, USA) with a ×100 objective.
Statistical analysis
Data are given as means ± SD. Datasets were statistically compared using one-way ANOVA or the Kruskal–Wallis or Wilcoxon tests. The Mann–Whitney U test was used for electrophysiological measurements with SPSS software (IBM, Armonk, NY, USA). Differences were accepted as significant if p < 0.05. Randomisation of samples and blinding was not carried out for outcome assessment.
Results
Morphophysiological characteristics of identified neurogliaform cells in hyper- and hypoglycaemia
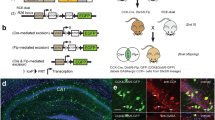
We searched for interneurons showing characteristics of neurogliaform cells in layers 1–3 using the whole-cell patch-clamp mode of brain slices prepared from the somatosensory cortex of male rats (P28-35). Acute brain slices were maintained in artificial cerebrospinal fluid containing glucose either in the concentration used as standard for in vitro brain slices (10 mmol/l, hyperglycaemia) or at a concentration of 0.5 mmol/l, determined as the hypoglycaemic external glucose concentration in the rat brain [22], but still suitable for whole-cell recordings from interneurons [13]. Differential interference contrast microscopy was used to select putative interneurons based on perisomatic morphology, and the identity of neurogliaform cells was first confirmed according to their late-spiking firing characteristics in response to depolarising current pulses (Fig. 1a–d) [13]. The use of biocytin in the patch-clamp recording pipettes allowed us to recover the morphology of the recorded cells, and the identity of each neurogliaform cell included in this study (n = 87) was additionally confirmed by post hoc anatomical assessment of axonal morphology (Fig. 1a–d). Quantitative morphological analysis was beyond the scope of this study; however, an extremely dense axonal arborisation with small and frequently spaced boutons, the hallmark of neurogliaform cells [13], could be readily observed in samples recorded and biocytin filled in hyper- and hypoglycaemic conditions. In addition, no somatodendritic differences seemed to emerge between the two experimental groups and no morphological features considered pathological were observed.
Anatomical and electrophysiological features of neurogliaform cells harvested for transcriptomic analysis. (a–d) Three-dimensional reconstructions (a,c) and somatically recorded firing patterns (b,c) of neurogliaform cells that were recorded by whole-cell patch-clamp and subsequently harvested for molecular analysis in brain slices of the rat frontal cortex. The neurogliaform cell in (a) was recorded as having hyperglycaemic external glucose concentration (10 mmol/l) in the artificial cerebrospinal fluid. This is standard in brain-slice experiments. Red, soma and dendrites; orange, axons. The neurogliaform cell in (c) was recorded in artificial cerebrospinal fluid containing 0.5 mmol/l glucose (similar to that reported during hypoglycaemia in the brain [22]). Blue, soma and dendrites; light blue, axons. (e–m) Electrophysiological variables of neurogliaform cells measured in hyperglycaemia (10 mmol/l external glucose [glucoseext]; red) and hypoglycaemia (0.5 mmol/l glucoseext; blue). Basic membrane variables were not significantly different; however, the amplitude of action potentials (APs) decreased during a train at a significantly higher rate in neurogliaform cells recorded in hypoglycaemia (l, p<0.010) and the half width of their successive action potentials increased more rapidly compared with neurogliaform cells measured in hyperglycaemia (m, p<0.019). *p<0.05
We compared the basic electrophysiological properties of neurogliaform cells recorded in 10 mmol/l (n = 10) and 0.5 mmol/l (n = 10) external glucose concentrations (Fig. 1e–m). Hyper- vs hypoglycaemic conditions had no significant effect on the resting membrane potential (−67.08 ± 2.66 mV vs −69.52 ± 5.28 mV; p = 0.35, Mann–Whitney U test), input resistance (113.15 ± 34.03 mΩ vs 85.82 ± 17.91 mΩ; p = 0.079), amplitude of action potentials (75.76 ± 6.84 mV vs 72.30 ± 6.1 mV; p = 0.39), interspike interval (0.103 ± 0.030 ms vs 0.078 ± 0.033 ms; p = 0.094), half width of action potentials (0.82 ± 0.27 ms vs 0.56 ± 0.12 ms; p = 0.079), action potential threshold (−30.89 ± 1.77 mV vs −30.9 ± 4.8 mV; p = 0.71) or action potential accommodation (131.86 ± 56.51% vs 155.25 ± 43.51%; p = 0.15). However, significant differences emerged between neurogliaform cells recorded in 10 mmol/l vs 0.5 mmol/l glucose when measuring accommodation in the amplitudes of successive action potentials (90.04 ± 6.18% vs 81.44 ± 6.47%; p = 0.010; Fig. 1l) and accommodation in the half widths of successive action potentials (129.73 ± 10.75% vs 145.53 ± 12.96%; p = 0.019; Fig. 1m). Thus, apart from minor differences possibly due to the relatively lower metabolic supply in hypoglycaemia slightly affecting the amplitude and duration of action potentials during sustained activity, electrophysiological and morphological features of neurogliaform cells appeared stable in our experimental conditions.
Functional expression of GLP-1 receptors and related molecular characteristics of identified neurogliaform cells
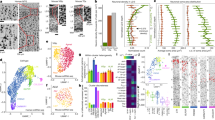
Previous experiments have suggested modulations of the Ins2 gene in neurogliaform cells in response to changes in the extracellular glucose concentration [13], indicating that these neurons of the cerebral cortex might have partially similar molecular and functional predispositions to those of pancreatic beta cells. Thus, we used the highly sensitive and quantitative method of single-cell digital PCR [21] to test whether genes important in beta cell function and development are expressed in neurogliaform cells of the neocortex. In particular, GLP-1 receptors promote insulin secretion on pancreatic beta cells, and expression of these receptors on insulin-releasing neurons has been suggested to have therapeutic implications [14]. We detected the expression of GLP-1 receptors in electrophysiologically and anatomically identified neurogliaform cells using single-cell digital PCR (n = 11, Fig. 2a) with the homeostatic gene S18 (also known as Rps18) as a reference. Moreover, we compared copy numbers of Glp1r mRNA in neurogliaform cells (n = 5) in hypoglycaemia, and found that copy numbers in hyperglycaemia exceeded those in hypogycaemia by 9.6 times when normalised to copy numbers of the homeostatic S18 gene (0.0457 ± 0.0427 and 0.0048 ± 0.0066; p < 0.008, Mann–Whitney U test; Fig. 2a).
Functional expression of GLP-1 receptors in neurogliaform cells. (a) Expression of GLP-1 receptors in electrophysiologically and anatomically identified neurogliaform cells detected by single-cell digital PCR. Copy numbers of Glp1r mRNA were higher in hyperglycaemia compared with hypoglycaemia when normalised to copy numbers of the homeostatic S18 gene (p<0.008). (b) Co-expression of GLP-1 receptors and insulin in individual neurogliaform cells. Neurogliaform cells tested for co-expression under hyperglycaemic conditions contained higher numbers of mRNA of both Ins2 and Glp1r compared with neurogliaform cells under hypoglycaemic conditions (p<0.037 and p<0.016, respectively). (c–g) Functional expression of GLP-1 on neurogliaform cells. (c,d) Example of an experiment testing the effect of GLP-1 (100 nmol/l) on identified neurogliaform cells. (c) Firing pattern of a neurogliaform cell recorded as having a hyperglycaemic external glucose concentration (10 mmol/l) in the artificial cerebrospinal fluid. (d) The application of 100 nmol/l GLP-1 to the same neurogliaform cell as in (c) altered the current required for a –90 mV holding potential. (e) Population data confirmed a decrease in the holding current (p<0.003) with GLP-1 treatment, which was reversible upon washout (p<0.022). Four out of 11 experiments were terminated before washout because of unstable access resistance. (f) Pre-treatment with the GLP-1 receptor-specific antagonist exendin-3(9-39) (1 μmol/l) blocked the response to GLP-1 application in identified neurogliaform cells (n=7). (g) Changes in the holding current in neurogliaform cells (n=6) did not occur with the application of GLP-1 in hypoglycaemia. *p<0.05, **p<0.01
We next asked whether GLP-1 receptors and insulin can be co-detected in individual neurogliaform cells (Fig. 2b). Our single-cell digital PCR method allows the exact measurement of mRNA copy numbers of no more than two genes, thus we replaced the homeostatic gene S18 with the Ins2 gene in our protocol so as to test GLP-1 receptor and insulin co-expression. Similar to pancreatic beta cells, neurogliaform cells co-expressed mRNA of the Ins2 and Glp1r genes. Neurogliaform cells tested for co-expression in hyperglycaemia (n = 5) contained higher numbers of mRNA of both Ins2 (8.60 ± 3.97) and Glp1r (8.40 ± 4.47) genes, compared with neurogliaform cells in hypoglycaemia (n = 5; 2.60 ± 1.34 and 0.80 ± 1.30, respectively; p < 0.037 and p < 0.016, respectively, Mann–Whitney U test; Fig. 2b). In showing that the external glucose concentration modulates the co-expression of insulin and GLP-1 receptors in neurogliaform cells, these results confirm our earlier report on insulin expression [13] and its glucose modulation in neurogliaform cells and corroborate the results shown above for Glp1r referenced to a homeostatic gene.
In order to confirm the functional expression of GLP-1 receptors, we tested the effect of GLP-1 on electrophysiologically and anatomically identified neurogliaform cells using the hyperglycaemic extracellular glucose concentration (Fig. 2c–e), similar to previous experiments [5]. Measuring the current required for −90 mV holding potential in whole-cell recordings before (−228 ± 39 pA, n = 11), during (−194 ± 49 pA, n = 11) and after (−214 ± 55 pA, n = 7) bath application of GLP-1 (100 nmol/l) [5], we detected a decrease in the holding current (p < 0.003, Wilcoxon test), which was reversible upon washout (p < 0.022; Fig. 2c–e). Moreover, pre-treatment with the GLP-1 receptor-specific antagonist exendin-3(9-39) (1 μmol/l) was effective in blocking the response in identified neurogliaform cells (n = 7) to GLP-1 application (−171 ± 39 pA vs −166 ± 32 pA; p = 0.205, Wilcoxon test; Fig. 2f). Furthermore, changes in the holding current in neurogliaform cells (n = 6) did not occur during the application of GLP-1 in hypoglycaemic conditions (−201 ± 59 pA vs −204 ± 58 pA; p = 0.401, Wilcoxon test; Fig. 2g). Accordingly, the moderate copy numbers relative to a homeostatic gene detected by single-cell digital PCR in neurogliaform cells appear sufficient for a functional GLP-1 response in neurogliaform interneurons.
The co-expression of GLP-1 receptors and insulin in neurogliaform cells gives rise to a potentially broader molecular similarity between pancreatic beta cells and neurogliaform neurons of the cerebral cortex. Indeed, the developmental lineage for pancreatic endocrine cells and neurons has been suggested to be related [23]. Following these ideas, our final series of experiments using single-cell digital PCR on identified neurogliaform cells revealed the expression of transcription factors important in beta cell development (Pdx1, Isl1 and Mafb copy numbers relative to S18: 0.0755 ± 0.0395, 0.0218 ± 0.0057 and 0.0279 ± 0.0254, respectively; Fig. 3) [24, 25]. In addition, we detected a significantly lower normalised mRNA copy numbers of Pdx1 and Isl1 in hypoglycaemia (0.0073 ± 0.0163, 0.0051 ± 0.0072; p < 0.037 and p < 0.016 vs hyperglycaemia, respectively, Mann–Whitney U test; Fig. 3).
Single-cell digital PCR of neurogliaform cells confirms the expression of transcription factors important in beta cells. Changes in extracellular glucose concentrations modulated the copy number of Isl1 and Pdx1 mRNA (normalised to the homeostatic gene S18) in electrophysiologically and anatomically identified neurogliaform cells (p<0.037 and p<0.016, respectively). *p<0.05
Discussion
Our results provide evidence for GLP-1 receptor expression in neurons known to release insulin in the cerebral cortex. Hyperglycaemia increases the expression of GLP-1 receptors in neurogliaform cells, suggesting that endogenous incretins and therapeutic GLP-1 receptor agonists might have effects on these neurons, similar to those on pancreatic beta cells. In addition, we detected transcription factors (Pdx1, Isl1, Mafb) in neurogliaform cells known to be important in beta cell development.
The crucial gene in the GLP-1–insulin interaction, Ins2, shows significant variations under similar experimental conditions from cell type to cell type in the cerebral cortex [13]; therefore, identifying the interneuron type(s) involved in an analysis is essential for appropriately interpreting the results. Our combined electrophysiological, neuroanatomical and molecular techniques allowed us to monitor transcriptional changes associated with experimentally controlled alterations in extracellular glucose concentrations, and to determine the identity of each neuron included in our dataset. Previous analyses of transcriptional changes in identified neurons in response to variable glucose concentrations are scarce [13], but are consistent regarding the functional effectiveness of approximately ten copies of the Ins2 and Glp1r genes per neuron. The expression threshold for functional GLP-1 receptor response seems to be more than two copies of Glp1r mRNA in low external glucose concentrations. This suggests that genes with moderate expression levels detected by microarray or next-generation techniques [26,27,28,29,30] and potentially interesting in insulin/incretin action are worth testing in functional experiments.
Conjoint modulation of the expression of the Ins2 and Glp1r genes reported here in identified neurogliaform interneurons suggests that mechanisms classically described in the pancreas for GLP-1-induced enhancement of insulin release might also operate in the brain. Application of glibenclamide, which is known to promote insulin release from pancreatic beta cells, has been successful in triggering insulin release from neurogliaform cells [13]. Although the direct action of endogenous incretins or other GLP-1 receptor agonists in neuronal insulin release requires further experiments, the mode of GLP-1 action and the polarity of responses might be cell-type-specific [5]. We speculate that the outward current in response to GLP-1 in neurogliaform cells at the holding potential applied in this study supports that activation of GLP-1 receptors leads to the opening of somatic K-channels possibly linked to gamma-aminobutyric acid (GABA) type B (GABAB) receptors and, as suggested in response to GLP-1 in hypothalamic neurons [31], to increased presynaptic GABA release. Moreover, considering the effect of GLP-1 in enhancing synaptic and tonic inhibitory currents arriving at hippocampal pyramidal cells [32], and taking into account the high expression of extrasynaptic GABA type A (GABAA) receptor delta subunits found on intermediate and distal dendrites of neurogliaform cells [33], we cannot exclude the possibility that our results also reflect the activation of GABAA channels located on distal dendrites and detected with suboptimal space-clamp due to the relatively low input resistance of neurogliaform cells and somatically placed electrodes [33, 34]. Possible tonic GABAA currents induced by GLP-1 on neurogliaform cells are in line with the involvement of neurogliaform cells shown to provide synaptic and extrasynaptic inhibition [33], and are further supported by insulin-triggered tonic inhibition through GABAA receptors [35]. It is not yet clear whether neurogliaform cells receive innervation from GLP-1-releasing neurons of the brainstem [5, 7, 8]; however, it is possible that intestinal-derived GLP-1 or therapeutic GLP-1 receptor agonists reach the cerebral cortex through the blood–brain barrier, similar to native GLP-1 [3, 4], and could modulate insulin release from neurogliaform cells. The inhibition of gastric emptying is considered a potential factor leading to weight loss caused by GLP-1 receptor agonist therapy [2]. However, an alternative mechanism might emerge when considering imaging studies suggesting that the prefrontal cortex is important in the inhibitory control of food intake in humans [36,37,38] and human brain-slice experiments showing that neurogliaform cells provide widespread inhibition in prefrontal microcircuits [39]. Selective involvement of GABAergic interneuron subpopulations is likely in neurodegenerative diseases [40]. Given that GLP-1 receptor agonists promise therapeutic effectiveness against neurodegeneration in models of traumatic brain injury and Alzheimer’s and Parkinson’s disease [16,17,18,19,20], the scenario of GLP-1 receptor-mediated insulin synthesis in the brain could be extended to the therapy of these diseases.
A related developmental lineage for pancreatic endocrine cells and neurons has been implicated [23], and our results on the limited number of transcription factors tested in neurogliaform cells here support this idea. Pdx1 is central in the regulation of pancreatic development and in the differentiation of beta cells from progenitor cells [24]. The effects of GLP-1 on beta cell proliferation and secretory function depend on crosstalk with proteins in the insulin-signalling pathway and modulation of transcription factors including pancreatic and duodenal homeobox 1 (PDX1) [24]; thus, the co-expression of Glp1r and Pdx1 found in neurogliaform cells suggests potential functional homology of neurogliaform and beta cells beyond development. Along the same vein, expression of the LIM homeodomain protein ISL1 (insulin gene enhancer binding protein, islet factor 1) is known from the develo** pancreas and the central nervous system [41, 42]. Synergistically with the basic helix-loop-helix transcription factor BETA2, ISL1 activates the insulin promoter in beta cells [43] and promotes pancreatic islet cell proliferation [44], and is required for the differentiation of interneurons in the spinal cord [45]. The role of Mafa and Mafb genes is crucial in beta cells during development (Mafb) and adulthood (Mafa in mice and MAFA and MAFB in humans) [46] and our results in neurogliaform cells confirm the widespread expression of MAFB reported earlier in develo** and differentiated neocortical interneurons [47]. Our results suggest that insulin and GLP-1 receptor-expressing neurogliaform interneurons of the cerebral cortex partially possess the transcription toolkit known to be instrumental in the development of insulin-synthesising pancreatic beta cells.
Data availability
The data are available on request from the authors.
Abbreviations
- GABA:
-
Gamma-aminobutyric acid
- GABAA:
-
Gamma-aminobutyric acid type A
- GABAB:
-
Gamma-aminobutyric acid type B
- GLP-1:
-
Glucagon-like peptide 1
- ISL1:
-
Insulin gene enhancer binding protein, islet factor 1
References
Holst JJ (2007) The physiology of glucagon-like peptide 1. Physiol Rev 87(4):1409–1439. https://doi.org/10.1152/physrev.00034.2006
Lovshin JA, Drucker DJ (2009) Incretin-based therapies for type 2 diabetes mellitus. Nat Rev Endocrinol 5(5):262–269. https://doi.org/10.1038/nrendo.2009.48
Kastin AJ, Akerstrom V, Pan W (2002) Interactions of glucagon-like peptide-1 (GLP-1) with the blood-brain barrier. J Mol Neurosci 18(1-2):7–14. https://doi.org/10.1385/JMN:18:1-2:07
Hunter K, Hölscher C (2012) Drugs developed to treat diabetes, liraglutide and lixisenatide, cross the blood brain barrier and enhance neurogenesis. BMC Neurosci 13(1):33. https://doi.org/10.1186/1471-2202-13-33
Cork SC, Richards JE, Holt MK, Gribble FM, Reimann F, Trapp S (2015) Distribution and characterisation of glucagon-like peptide-1 receptor expressing cells in the mouse brain. Mol Metab 4(10):718–731. https://doi.org/10.1016/j.molmet.2015.07.008
Hamilton A, Hölscher C (2009) Receptors for the incretin glucagon-like peptide-1 are expressed on neurons in the central nervous system. Neuroreport 20(13):1161–1166. https://doi.org/10.1097/WNR.0b013e32832fbf14
Trapp S, Richards JE (2013) The gut hormone glucagon-like peptide-1 produced in brain: is this physiologically relevant? Curr Opin Pharmacol 13(6):964–969. https://doi.org/10.1016/j.coph.2013.09.006
Llewellyn-Smith IJ, Reimann F, Gribble FM, Trapp S (2011) Preproglucagon neurons project widely to autonomic control areas in the mouse brain. Neuroscience 180:111–121. https://doi.org/10.1016/j.neuroscience.2011.02.023
Devaskar SU, Singh BS, Carnaghi LR et al (1993) Insulin II gene expression in rat central nervous system. Regul Pept 48(1-2):55–63. https://doi.org/10.1016/0167-0115(93)90335-6
Gerozissis K (2010) The brain-insulin connection, metabolic diseases and related pathologies. In: Craft S (ed) Diabetes, insulin and Alzheimer’s disease. Springer, Berlin, pp 21–42. https://doi.org/10.1007/978-3-642-04300-0_2
Gray SM, Meijer RI, Barrett EJ (2014) Insulin regulates brain function, but how does it get there? Diabetes 63(12):3992–3997. https://doi.org/10.2337/db14-0340
Kuwabara T, Kagalwala MN, Onuma Y et al (2011) Insulin biosynthesis in neuronal progenitors derived from adult hippocampus and the olfactory bulb. EMBO Mol Med 3(12):742–754. https://doi.org/10.1002/emmm.201100177
Molnár G, Faragó N, Kocsis ÁK et al (2014) GABAergic neurogliaform cells represent local sources of insulin in the cerebral cortex. J Neurosci 34(4):1133–1137. https://doi.org/10.1523/JNEUROSCI.4082-13.2014
Csajbók ÉA, Tamás G (2016) Cerebral cortex: a target and source of insulin? Diabetologia 59(8):1609–1615. https://doi.org/10.1007/s00125-016-3996-2
Craft S, Baker LD, Montine TJ et al (2012) Intranasal insulin therapy for Alzheimer disease and amnestic mild cognitive impairment: a pilot clinical trial. Arch Neurol 69(1):29–38. https://doi.org/10.1001/archneurol.2011.233
Holscher C (2016) Glucagon-like peptide 1 and glucose-dependent insulinotropic polypeptide analogues as novel treatments for Alzheimer’s and Parkinson’s disease. Cardiovasc Endocrinol 5(3):93–98. https://doi.org/10.1097/XCE.0000000000000087
Gejl M, Gjedde A, Egefjord L et al (2016) In Alzheimer’s disease, 6-month treatment with GLP-1 analog prevents decline of brain glucose metabolism: randomized, placebo-controlled, double-blind clinical trial. Front Aging Neurosci 8:108. https://doi.org/10.3389/fnagi.2016.00108
Bertilsson G, Patrone C, Zachrisson O et al (2008) Peptide hormone exendin-4 stimulates subventricular zone neurogenesis in the adult rodent brain and induces recovery in an animal model of Parkinson’s disease. J Neurosci Res 86(2):326–338. https://doi.org/10.1002/jnr.21483
Hakon J, Ruscher K, Romner B, Tomasevic G (2015) Preservation of the blood brain barrier and cortical neuronal tissue by liraglutide, a long acting glucagon-like-1 analogue, after experimental traumatic brain injury. PLoS One 10(3):e0120074. https://doi.org/10.1371/journal.pone.0120074
Greig NH, Tweedie D, Rachmany L et al (2014) Incretin mimetics as pharmacologic tools to elucidate and as a new drug strategy to treat traumatic brain injury. Alzheimers Dement 10(1):S62–S75. https://doi.org/10.1016/j.jalz.2013.12.011
Faragó N, Kocsis ÁK, Lovas S et al (2013) Digital PCR to determine the number of transcripts from single neurons after patch-clamp recording. Biotechniques 54(6):327–336. https://doi.org/10.2144/000114029
Silver IA, Erecińska M (1994) Extracellular glucose concentration in mammalian brain: continuous monitoring of changes during increased neuronal activity and upon limitation in oxygen supply in normo-, hypo-, and hyperglycemic animals. J Neurosci 14:5068–5076
Alpert S, Hanahan D, Teitelman G (1988) Hybrid insulin genes reveal a developmental lineage for pancreatic endocrine cells and imply a relationship with neurons. Cell 53(2):295–308. https://doi.org/10.1016/0092-8674(88)90391-1
Habener JF, Kemp DM, Thomas MK (2005) Minireview: transcriptional regulation in pancreatic development. Endocrinology 146(3):1025–1034. https://doi.org/10.1210/en.2004-1576
Hang Y, Stein R (2011) MafA and MafB activity in pancreatic β cells. Trends Endocrinol Metab 22(9):364–373. https://doi.org/10.1016/j.tem.2011.05.003
Baron M, Veres A, Wolock SL et al (2016) A single-cell transcriptomic map of the human and mouse pancreas reveals inter- and intra-cell population structure. Cell Syst 3(4):346–360.e4. https://doi.org/10.1016/j.cels.2016.08.011
Lawlor N, George J, Bolisetty M et al (2017) Single-cell transcriptomes identify human islet cell signatures and reveal cell-type-specific expression changes in type 2 diabetes. Genome Res 27(2):208–222. https://doi.org/10.1101/gr.212720.116
Li J, Klughammer J, Farlik M et al (2016) Single-cell transcriptomes reveal characteristic features of human pancreatic islet cell types. EMBO Rep 17(2):178–187. https://doi.org/10.15252/embr.201540946
Muraro MJ, Dharmadhikari G, Grün D et al (2016) A single-cell transcriptome atlas of the human pancreas. Cell Syst 3(4):385–394.e3. https://doi.org/10.1016/j.cels.2016.09.002
Wang YJ, Schug J, Won K-J et al (2016) Single-cell transcriptomics of the human endocrine pancreas. Diabetes 65(10):3028–3038. https://doi.org/10.2337/db16-0405
Farkas I, Vastagh C, Farkas E et al (2016) Glucagon-like peptide-1 excites firing and increases GABAergic miniature postsynaptic currents (mPSCs) in gonadotropin-releasing hormone (GnRH) neurons of the male mice via activation of nitric oxide (NO) and suppression of endocannabinoid signaling pathways. Front Cell Neurosci 10:214. https://doi.org/10.3389/fncel.2016.00214
Korol SV, ** Z, Babateen O, Birnir B (2015) GLP-1 and exendin-4 transiently enhance GABAA receptor-mediated synaptic and tonic currents in rat hippocampal CA3 pyramidal neurons. Diabetes 64(1):79–89. https://doi.org/10.2337/db14-0668
Olah S, Fule M, Komlosi G et al (2009) Regulation of cortical microcircuits by unitary GABA-mediated volume transmission. Nature 461(7268):1278–1281. https://doi.org/10.1038/nature08503
Overstreet-Wadiche L, McBain CJ (2015) Neurogliaform cells in cortical circuits. Nat Rev Neurosci 16(8):458–468. https://doi.org/10.1038/nrn3969
** Z, ** Y, Kumar-Mendu S et al (2011) Insulin reduces neuronal excitability by turning on GABA(A) channels that generate tonic current. PLoS One 6(1):e16188. https://doi.org/10.1371/journal.pone.0016188
Anthony K, Reed LJ, Dunn JT et al (2006) Attenuation of insulin-evoked responses in brain networks controlling appetite and reward in insulin resistance: the cerebral basis for impaired control of food intake in metabolic syndrome? Diabetes 55(11):2986–2992. https://doi.org/10.2337/db06-0376
Heni M, Kullmann S, Preissl H et al (2015) Impaired insulin action in the human brain: causes and metabolic consequences. Nat Rev Endocrinol 11(12):701–711. https://doi.org/10.1038/nrendo.2015.173
Kleinridders A, Ferris HA, Cai W, Kahn CR (2014) Insulin action in brain regulates systemic metabolism and brain function. Diabetes 63(7):2232–2243. https://doi.org/10.2337/db14-0568
Olah S, Komlosi G, Szabadics J et al (2007) Output of neurogliaform cells to various neuron types in the human and rat cerebral cortex. Front Neural Circuits 1:4. https://doi.org/10.3389/neuro.04.004.2007
Morrison JH, Hof PR (1997) Life and death of neurons in the aging brain. Science 278(5337):412–419. https://doi.org/10.1126/science.278.5337.412
Thor S, Ericson J, Brännström T, Edlund T (1991) The homeodomain LIM protein Isl-1 is expressed in subsets of neurons and endocrine cells in the adult rat. Neuron 7(6):881–889. https://doi.org/10.1016/0896-6273(91)90334-V
Karlsson O, Thor S, Norberg T et al (1990) Insulin gene enhancer binding protein Isl-1 is a member of a novel class of proteins containing both a homeo-and a Cys-His domain. Nature 344(6269):879–882. https://doi.org/10.1038/344879a0
Zhang H, Wang W-P, Guo T et al (2009) The LIM-homeodomain protein ISL1 activates insulin gene promoter directly through synergy with BETA2. J Mol Biol 392(3):566–577. https://doi.org/10.1016/j.jmb.2009.07.036
Guo T, Wang W, Zhang H et al (2011) ISL1 promotes pancreatic islet cell proliferation. PLoS One 6(8):e22387. https://doi.org/10.1371/journal.pone.0022387
Pfaff SL, Mendelsohn M, Stewart CL et al (1996) Requirement for LIM homeobox gene Isl1 in motor neuron generation reveals a motor neuron-dependent step in interneuron differentiation. Cell 84(2):309–320. https://doi.org/10.1016/S0092-8674(00)80985-X
Benner C, van der Meulen T, Cacéres E et al (2014) The transcriptional landscape of mouse beta cells compared to human beta cells reveals notable species differences in long non-coding RNA and protein-coding gene expression. BMC Genomics 15(1):620. https://doi.org/10.1186/1471-2164-15-620
Cobos I, Long JE, Thwin MT, Rubenstein JL (2006) Cellular patterns of transcription factor expression in develo** cortical interneurons. Cereb Cortex 16(Suppl_1):i82–i88. https://doi.org/10.1093/cercor/bhk003
Acknowledgements
The authors thank É. Tóth, M. V. Várady and N. Tóth for technical assistance (MTA-SZTE Research Group for Cortical Microcircuits, University of Szeged, Szeged, Hungary). Some of these data were presented as an abstract at the ADA 77th Scientific Sessions in 2017.
Funding
This work was supported by the European Research Council INTERIMPACT project (GT), the Hungarian Academy of Sciences (GT), the National Research, Development and Innovation Office of Hungary (GINOP-2.3.2-15-2016-00018, VKSZ-14-1-2015-0155), the Ministry of Human Capacities, Hungary (grant 20391-3/2018/FEKUSTRAT) and by the National Brain Research Program, Hungary (GT).
Author information
Authors and Affiliations
Contributions
EAC and GT formulated the key hypothesis, designed the experiments, contributed to the data analysis, interpretation and production of figures, and wrote the paper with final approval of the version to be published. ÁKK, NF, EAC, ÁZ, IL, AP and LGP performed single-cell digital PCR and molecular data interpretation, drafted the article and gave final approval of the version to be published. SF, BK, SL and GM performed electrophysiology, harvested cytoplasms, drafted the text, performed analysis and produced figures, drafted the manuscript and gave final approval of the version to be published. GT is responsible for the integrity of the work as a whole.
Corresponding author
Ethics declarations
The authors declare that there is no duality of interest associated with this manuscript.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Csajbók, É.A., Kocsis, Á.K., Faragó, N. et al. Expression of GLP-1 receptors in insulin-containing interneurons of rat cerebral cortex. Diabetologia 62, 717–725 (2019). https://doi.org/10.1007/s00125-018-4803-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-018-4803-z