Abstract
Purpose
To investigate prognosis of patients with fragility fracture of the pelvis (FFP) treated in a single trauma unit in Japan.
Methods
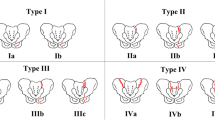
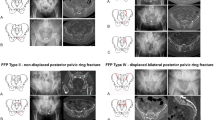
We retrospectively investigated 340 consecutive patients with FFP (40 men, 300 women; average age, 82.5 years) treated in our facility from April 2012 to April 2019. Fractures were categorized according to the Rommens classification. Patients’ mechanism of injury, existence of hip implant, standing and walking abilities (using the Majeed score), and 1-year mortality rate were evaluated.
Results
According to the Rommens classification, there were 84 type Ia, 2 type Ib, 24 type IIa, 78 type IIb, 51 type IIc, 40 type IIIa, 1 type IIIb, 4 type IIIc, 1 type IVa, 51 type IVb, and 3 type IVc fractures. Sixteen patients (4.7%) received surgical treatments. Twenty-eight patients (8.2%) had no memory of a traumatic event, and 61 (18%) had implants from a previous hip surgery. A total of 176 patients (52%) were followed up for ≥ 1 year, and 70 (39.8%) and 67 (38.1%) patients had recovery of standing and walking abilities, similar to those before the injury. The operative group (7/9 = 77.8%) had a higher proportion of patients who regained their standing and walking abilities at the 1-year follow-up than the conservative group. The 1-year mortality rate of the patients who could be followed for ≥ 1 year was 6.7%.
Conclusion
According to our data, 4.7% of patients were indicated for surgery, and only < 40% of patients were able to regain their pre-injury standing and walking abilities at 1 year after the injury. FFP may greatly affect an elderly’s activities of daily living and may lead to prognosis similar to patients with proximal hip fractures. To regain the walking ability of patients with FFP, more aggressive indication of surgical treatment may be considered depending on the patient’s background. Further examinations are necessary to determine the surgical indications and treatment protocol for FFP.




Similar content being viewed by others
References
World Fact Book. https://www.cia.gov/library/publications/theworld-factbook/rankorder/2102rank.html.
Benzinger P, Becker C, Kerse N, et al. Pelvic fracture rates in community-living people with and without disability and in residents of nursing homes. J Am Med Dir Assoc. 2013;14:673–8.
Andrich S, Haastert B, Neuhaus E, et al. Excess mortality after pelvic fractures among older people. J Bone Miner Res. 2017;32:1789–801.
Marrinan S, Pearce MS, Jiang XY, Waters S, Shanshal Y. Admission for osteoporotic pelvic fractures and predictors of length of hospital stay, mortality and loss of independence. Age Ageing. 2015;44:258–61.
Taillandier J, Langue F, Alemanni M, Taillandier-Heriche E. Mortality and functional outcomes of pelvic insufficiency fractures in older patients. Joint Bone Spine. 2003;70:287–9.
Hopf JC, Krieglstein CF, Muller LP, Koslowsky TC. Percutaneous iliosacral screw fixation after osteoporotic posterior ring fractures of the pelvis reduces pain significantly in elderly patients. Injury. 2015;46:1631–6.
Rommens PM, Hofmann A. Fragility fractures of the pelvis. Cham: Springer International Publishing; 2017.
Rommens PM, Hofmann A. Comprehensive classification of fragility fractures of the pelvic ring: recommendations for surgical treatment. Injury. 2013;44:1733–44.
Majeed SA. Grading the outcome of pelvic fractures. J Bone Joint Surg Br. 1989;71:304–6.
Rommens PM, Ossendorf C, Pairon P, Dietz SO, Wagner D, Hofmann A. Clinical pathways for fragility fractures of the pelvic ring: personal experience and review of the literature. J Orthop Sci. 2015;20:1–11.
Soles GLS, Ferguson TA. Fragility fractures of the pelvis. Curr Rev Musculoskelet Med. 2012;5:222–8.
Ueda Y, Inui T, Kurata Y, Tsuji H, Saito J, Shitan Y. Prolonged pain in patients with fragility fractures of the pelvis may be due to fracture progression. Eur J Trauma Emerg Surg. 2019. https://doi.org/10.1007/s00068-019-01150-0.
Masahiro Y. Bessatsu Seikeigeka. 2017 ISSN 0287–1645
Koval KJ, Aharonoff GB, Schwartz MC, et al. Pubic rami fractures: a benign pelvic injury? J Orthop Trauma. 1997;11:7–9.
Hill RM, Robinson CM, Keating JF. Fractures of the pubic rami. Epidemiology and five-year survival. J Bone Joint Surg Br. 2001;83:1141–4.
Noser J, Dietrich M, Tiziani S, Werner CML, Pape HS, Osterhoff G. Mid-term follow-up after surgical treatment of fragility fractures of the pelvis. Injury. 2018;49:2032–5.
Hoch A, Ozkurtul O, Pieroh P, Josten C, Bohme J. Outcome and 2-year survival rate in elderly patients with lateral compression fractures of the pelvis. Geriatr Orthop Surg Rehabil. 2017;8:3–9.
Mears SC, Berry DJ. Outcomes of displaced and nondisplaced pelvic and sacral fractures in elderly adults. J Am Geriatr Soc. 2011;59:1309–12.
Dechert TA, Duane TM, Frykberg BP, Aboutanos MB, Malhotra AK, Ivatury RR. Elderly patients with pelvic fracture: interventions and outcomes. Am Surg. 2009;75:291–5.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Yoshida, M., Tajima, K., Saito, Y. et al. Mobility and mortality of 340 patients with fragility fracture of the pelvis. Eur J Trauma Emerg Surg 47, 29–36 (2021). https://doi.org/10.1007/s00068-020-01481-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00068-020-01481-3