Abstract
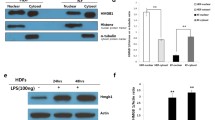
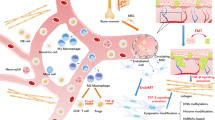
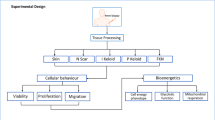
Keloid scars are common benign fibroproliferative reticular dermal lesions with unknown etiology and ill-defined management with high rate of recurrence post surgery. The progression of keloids is characterized by increased deposition of extracellular matrix proteins, invasion into the surrounding healthy skin and inflammation. Fibroblasts are considered to be the key cellular mediators of fibrogenesis in keloid scars. Fibroblast activation protein alpha (FAP-α) and dipeptidyl peptidase IV (DPPIV) are proteases located at the plasma membrane promoting cell invasiveness and tumor growth and have been previously associated with keloid scars. Therefore, in this study we analyzed in further detail the expression of FAP-α in keloid fibroblasts compared to control skin fibroblasts. Dermal fibroblasts were obtained from punch-biopsies from the active margin of four keloids and four control skin samples. Flow cytometry was used to analyze FAP-α expression and the CytoSelect® 24-Well Collagen I Cell Invasion Assay was applied to study fibroblast invasion. Secretion of extracellular matrix (ECM) proteins was investigated by multiplexed particle-based flow cytometric assay and enzyme-linked immunosorbent assay. We found an increased expression of FAP-α in keloid fibroblasts compared to control skin fibroblasts (p < 0.001). Inhibition of FAP-α/DPPIV activity using the irreversible inhibitor H2N-Gly-Pro diphenylphosphonate reduced the increased invasiveness of keloid fibroblasts (p < 0.001) indicating that keloid invasion may be partly FAP-α/DPPIV mediated. FAP-α/DPPIV inhibition had no effect, (a) on the synthesis of the ECM proteins procollagen type I C-terminal peptide and fibronectin, (b) on the production of fibroblast growth factor or vascular endothelial growth factor, (c) on the expression of the proinflammatory cytokines interleukin-6 (IL-6), interleukin 8 (IL-8) or monocyte chemotactic protein-1. These results suggest a potential role for FAP-α and DPPIV in the invasive behavior of keloids. FAP-α and DPPIV may increase the invasive capacity of keloid fibroblasts rather than by modulating inflammation or ECM production. Since FAP-α expression is restricted to reactive fibroblasts in wound healing and normal adult tissues are generally FAP-α negative, inhibiting FAP-α/DPPIV activity may be a novel treatment option to prevent keloid progression.




Similar content being viewed by others
References
Abergel RP, Pizzurro D, Meeker CA, Lask G, Matsuoka LY, Minor RR, Chu ML, Uitto J (1985) Biochemical composition of the connective tissue in keloids and analysis of collagen metabolism in keloid fibroblast cultures. J Invest Dermatol 84:384–390
Babu M, Diegelmann R, Oliver N (1989) Fibronectin is overproduced by keloid fibroblasts during abnormal wound healing. Mol Cell Biol 9:1642–1650
Bock O, Schmid-Ott G, Malewski P, Mrowietz U (2006) Quality of life of patients with keloid and hypertrophic scarring. Arch Dermatol Res 297:433–438
Durani P, Bayat A (2008) Levels of evidence for the treatment of keloid disease. J Plast Reconstr Aesthet Surg 61:4–17
Garin-Chesa P, Old LJ, Rettig WJ (1990) Cell surface glycoprotein of reactive stromal fibroblasts as a potential antibody target in human epithelial cancers. Proc Natl Acad Sci USA 87:7235–7239
Ghazizadeh M, Tosa M, Shimizu H, Hyakusoku H, Kawanami O (2007) Functional implications of the IL-6 signaling pathway in keloid pathogenesis. J Invest Dermatol 127:98–105
Ghersi G, Zhao Q, Salamone M, Yeh Y, Zucker S, Chen WT (2006) The protease complex consisting of dipeptidyl peptidase IV and seprase plays a role in the migration and invasion of human endothelial cells in collagenous matrices. Cancer Res 66:4652–4661
Gilmore BF, Lynas JF, Scott CJ, McGoohan C, Martin L, Walker B (2006) Dipeptide proline diphenyl phosphonates are potent, irreversible inhibitors of seprase (FAPalpha). Biochem Biophys Res Commun 346:436–446
Gorrell MD (2005) Dipeptidyl peptidase IV and related enzymes in cell biology and liver disorders. Clin Sci (Lond) 108:277–292
Gragnani A, Warde M, Furtado F, Ferreira LM (2010) Topical tamoxifen therapy in hypertrophic scars or keloids in burns. Arch Dermatol Res 302:1–4
Hsu YC, Chen MJ, Yu YM, Ko SY, Chang CC (2010) Suppression of TGF-beta1/SMAD pathway and extracellular matrix production in primary keloid fibroblasts by curcuminoids: its potential therapeutic use in the chemoprevention of keloid. Arch Dermatol Res [Epub ahead of print]
Imaizumi R, Akasaka Y, Inomata N, Okada E, Ito K, Ishikawa Y, Maruyama Y (2009) Promoted activation of matrix metalloproteinase (MMP)-2 in keloid fibroblasts and increased expression of MMP-2 in collagen bundle regions: implications for mechanisms of keloid progression. Histopathology 54:722–730
Kischer CW, Wagner HN Jr, Pindur J, Holubec H, Jones M, Ulreich JB, Scuderi P (1989) Increased fibronectin production by cell lines from hypertrophic scar and keloid. Connect Tissue Res 23:279–288
Le AD, Zhang Q, Wu Y, Messadi DV, Akhondzadeh A, Nguyen AL, Aghaloo TL, Kelly AP, Bertolami CN (2004) Elevated vascular endothelial growth factor in keloids: relevance to tissue fibrosis. Cells Tissues Organs 176:87–94
Lee J, Fassnacht M, Nair S, Boczkowski D, Gilboa E (2005) Tumor immunotherapy targeting fibroblast activation protein, a product expressed in tumor-associated fibroblasts. Cancer Res 65:11156–11163
Liao WT, Yu HS, Arbiser JL, Hong CH, Govindarajan B, Chai CY, Shan WJ, Lin YF, Chen GS, Lee CH (2010) Enhanced MCP-1 release by keloid CD14+ cells augments fibroblast proliferation: role of MCP-1 and Akt pathway in keloids. Exp Dermatol 19(8):e142–e150
Lim CP, Phan TT, Lim IJ, Cao X (2009) Cytokine profiling and Stat3 phosphorylation in epithelial-mesenchymal interactions between keloid keratinocytes and fibroblasts. J Invest Dermatol 129:851–861
Lu F, Gao J, Ogawa R, Hyakusoku H, Ou C (2007) Biological differences between fibroblasts derived from peripheral and central areas of keloid tissues. Plast Reconstr Surg 120:625–630
Marneros AG, Krieg T (2004) Keloids—clinical diagnosis, pathogenesis, and treatment options. J Dtsch Dermatol Ges 2:905–913
Marneros AG, Norris JE, Watanabe S, Reichenberger E, Olsen BR (2004) Genome scans provide evidence for keloid susceptibility loci on chromosomes 2q23 and 7p11. J Invest Dermatol 122:1126–1132
Monsky WL, Lin CY, Aoyama A, Kelly T, Akiyama SK, Mueller SC, Chen WT (1994) A potential marker protease of invasiveness, seprase, is localized on invadopodia of human malignant melanoma cells. Cancer Res 54:5702–5710
Murray JC (1994) Keloids and hypertrophic scars. Clin Dermatol 12:27–37
Nassiri M, Woolery-Lloyd H, Ramos S, Jacob SE, Gugic D, Viciana A, Romanelli P, Elgart G, Berman B, Vincek V (2009) Gene expression profiling reveals alteration of caspase 6 and 14 transcripts in normal skin of keloid-prone patients. Arch Dermatol Res 301:183–188
O’Brien P, O’Connor BF (2008) Seprase: an overview of an important matrix serine protease. Biochim Biophys Acta 1784:1130–1145
Ohtsuru A, Yoshimoto H, Ishihara H, Namba H, Yamashita S (2000) Insulin-like growth factor-I (IGF-I)/IGF-I receptor axis and increased invasion activity of fibroblasts in keloid. Endocr J 47(Suppl):S41–S44
Park JE, Lenter MC, Zimmermann RN, Garin-Chesa P, Old LJ, Rettig WJ (1999) Fibroblast activation protein, a dual specificity serine protease expressed in reactive human tumor stromal fibroblasts. J Biol Chem 274:36505–36512
Pitche P (2006) What is true in “spontaneous” keloids? Ann Dermatol Venereol 133:501
Reinhold D, Kahne T, Steinbrecher A, Wrenger S, Neubert K, Ansorge S, Brocke S (2002) The role of dipeptidyl peptidase IV (DP IV) enzymatic activity in T cell-activation and autoimmunity. Biol Chem 383:1133–1138
Rettig WJ, Garin-Chesa P, Healey JH, Su SL, Ozer HL, Schwab M, Albino AP, Old LJ (1993) Regulation and heteromeric structure of the fibroblast activation protein in normal and transformed cells of mesenchymal and neuroectodermal origin. Cancer Res 53:3327–3335
Scanlan MJ, Raj BK, Calvo B, Garin-Chesa P, Sanz-Moncasi MP, Healey JH, Old LJ, Rettig WJ (1994) Molecular cloning of fibroblast activation protein alpha, a member of the serine protease family selectively expressed in stromal fibroblasts of epithelial cancers. Proc Natl Acad Sci USA 91:5657–5661
Seifert O, Bayat A, Geffers R, Dienus K, Buer J, Lofgren S, Matussek A (2008) Identification of unique gene expression patterns within different lesional sites of keloids. Wound Repair Regen 16:254–265
Seifert O, Mrowietz U (2009) Keloid scarring: bench and bedside. Arch Dermatol Res 301:259–272
Shih B, Bayat A (2010) Genetics of keloid scarring. Arch Dermatol Res 302:319–339
Tan EM, Hoffren J, Rouda S, Greenbaum S, Fox JW 4th, Moore JH Jr, Dodge GR (1993) Decorin, versican, and biglycan gene expression by keloid and normal dermal fibroblasts: differential regulation by basic fibroblast growth factor. Exp Cell Res 209:200–207
Tan EM, Rouda S, Greenbaum SS, Moore JH Jr, Fox JW 4th, Sollberg S (1993) Acidic and basic fibroblast growth factors down-regulate collagen gene expression in keloid fibroblasts. Am J Pathol 142:463–470
Tan KT, Shah N, Pritchard SA, McGrouther DA, Bayat A (2010) The influence of surgical excision margins on keloid prognosis. Ann Plast Surg 64:55–58
Thielitz A, Vetter RW, Schultze B, Wrenger S, Simeoni L, Ansorge S, Neubert K, Faust J, Lindenlaub P, Gollnick HP, Reinhold D (2008) Inhibitors of dipeptidyl peptidase IV-like activity mediate antifibrotic effects in normal and keloid-derived skin fibroblasts. J Invest Dermatol 128:855–866
Tuan TL, Nichter LS (1998) The molecular basis of keloid and hypertrophic scar formation. Mol Med Today 4:19–24
Uitto J, Perejda AJ, Abergel RP, Chu ML, Ramirez F (1985) Altered steady-state ratio of type I/III procollagen mRNAs correlates with selectively increased type I procollagen biosynthesis in cultured keloid fibroblasts. Proc Natl Acad Sci USA 82:5935–5939
Vignali DA (2000) Multiplexed particle-based flow cytometric assays. J Immunol Methods 243:243–255
Zhang GY, Yi CG, Li X, Zheng Y, Niu ZG, **a W, Meng Z, Meng CY, Guo SZ (2008) Inhibition of vascular endothelial growth factor expression in keloid fibroblasts by vector-mediated vascular endothelial growth factor shRNA: a therapeutic potential strategy for keloid. Arch Dermatol Res 300:177–184
Acknowledgments
This study was supported by grants from the Edvard Welander Foundation, Finsen Foundation, from the Medical Research Council of Southeast Sweden (FORSS) and from the Olle Enkvist Foundation.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Dienus, K., Bayat, A., Gilmore, B.F. et al. Increased expression of fibroblast activation protein-alpha in keloid fibroblasts: implications for development of a novel treatment option. Arch Dermatol Res 302, 725–731 (2010). https://doi.org/10.1007/s00403-010-1084-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00403-010-1084-x