Abstract
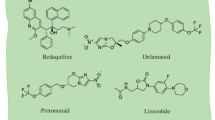
The World Health Organization (WHO) estimated that there were 1.6 million deaths worldwide in 2017 from tuberculosis (TB). Today, TB kills more humans than any other infectious agent, even surpassing HIV/AIDS or malaria (WHO TB report 2018). Prolonged treatment with poorly tolerated drugs to treat drug-resistant tuberculosis (DR-TB) has further exacerbated this global health crisis. Overall success rate of treating multidrug-resistant (MDR) and extensively drug-resistant (XDR) TB is only 54%, which means for a significant number of patients, especially those with XDR-TB, prognosis is death. Factors that make existing treatment options of MDR/XDR-TB inadequate are (1) high incidence of undesirable side effects from the only drugs that are available today to treat these infections, (2) the protracted treatment duration (more than 18 months) and (3) the high cost of the treatment. The WHO has approved several new and repurposing of existing antibiotics for treatment of DR-TB aimed at improving outcomes of MDR/XDR-TB treatment. These recommendations have focused on optimizing all aspects of TB treatment including shortening treatment duration, optimizing dosages and develo** new combination regimens. Although new anti-TB drugs, like bedaquiline, delamanid and pretomanid, have been successfully developed, their slow implementation, suboptimal availability and unanticipated cardiac toxicities mean availability of additional antibiotics would provide choices and improve our ability to treat DR-TB. Repurposing of already available antibiotics that are safe and readily accessible can be a practical solution for treating DR-TB, especially in resource-poor settings where majority of TB patients live. One class of antibiotics that matches this profile are the powerful carbapenems of the β-lactam group. There is a long history of their use in treating bacterial infections, they are safe and widely available, and emerging evidence shows that they can be immediately repurposed to treat DR-TB. This book chapter describes recent important developments in the repurposing of carbapenems for MDR and XDR-TB treatment.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
Abbreviations
- WHO:
-
World Health Organization
- TB:
-
Tuberculosis
- MDR:
-
Multidrug resistant
- XDR:
-
Extensively drug resistant
- CrfA:
-
Carbapenem-resistant factor A
- PBP:
-
Penicillin-binding protein
- DHP-1:
-
Dehydropeptidase 1
References
Andries K, Verhasselt P, Guillemont J, Gohlmann HW, Neefs JM, Winkler H, Van Gestel J, Timmerman P, Zhu M, Lee E, Williams P, de Chaffoy D, Huitric E, Hoffner S, Cambau E, Truffot-Pernot C, Lounis N, Jarlier V (2005) A diarylquinoline drug active on the ATP synthase of Mycobacterium tuberculosis. Science 307(5707):223–227. https://doi.org/10.1126/science.1106753
Arbex MA, Bonini EH, Kawakame Pirolla G, D’Ambrosio L, Centis R, Migliori GB (2016) Effectiveness and safety of imipenem/clavulanate and linezolid to treat multidrug and extensively drug-resistant tuberculosis at a referral hospital in Brazil. Rev Port Pneumol (2006) 22(6):337–341. https://doi.org/10.1016/j.rppnen.2016.06.006
Brammer Basta LA, Ghosh A, Pan Y, Jakoncic J, Lloyd EP, Townsend CA, Lamichhane G, Bianchet MA (2015) Loss of a functionally and structurally distinct ld-Transpeptidase, LdtMt5, compromises cell wall integrity in Mycobacterium tuberculosis. J Biol Chem 290(42):25670–25685. https://doi.org/10.1074/jbc.M115.660753
Chambers HF, Turner J, Schecter GF, Kawamura M, Hopewell PC (2005) Imipenem for treatment of tuberculosis in mice and humans. Antimicrob Agents Chemother 49(7):2816–2821. https://doi.org/10.1128/AAC.49.7.2816-2821.2005
Correale S, Ruggiero A, Capparelli R, Pedone E, Berisio R (2013) Structures of free and inhibited forms of the L,D-transpeptidase LdtMt1 from Mycobacterium tuberculosis. Acta Crystallogr D Biol Crystallogr 69(Pt 9):1697–1706. https://doi.org/10.1107/S0907444913013085
Deshpande D, Srivastava S, Nuermberger E, Pasipanodya JG, Swaminathan S, Gumbo T (2016) A Faropenem, Linezolid, and Moxifloxacin Regimen for both drug-susceptible and multidrug-resistant Tuberculosis in children: FLAME path on the Milky Way. Clin Infect Dis 63(Suppl 3):S95–S101. https://doi.org/10.1093/cid/ciw474
Dhar N, Dubee V, Ballell L, Cuinet G, Hugonnet JE, Signorino-Gelo F, Barros D, Arthur M, McKinney JD (2015) Rapid cytolysis of Mycobacterium tuberculosis by faropenem, an orally bioavailable beta-lactam antibiotic. Antimicrob Agents Chemother 59(2):1308–1319. https://doi.org/10.1128/AAC.03461-14
Diacon AH, Pym A, Grobusch M, Patientia R, Rustomjee R, Page-Shipp L, Pistorius C, Krause R, Bogoshi M, Churchyard G, Venter A, Allen J, Palomino JC, De Marez T, van Heeswijk RP, Lounis N, Meyvisch P, Verbeeck J, Parys W, de Beule K, Andries K, Mc Neeley DF (2009) The diarylquinoline TMC207 for multidrug-resistant tuberculosis. N Engl J Med 360(23):2397–2405. https://doi.org/10.1056/NEJMoa0808427
Diacon AH, van der Merwe L, Barnard M, von Groote-Bidlingmaier F, Lange C, Garcia-Basteiro AL, Sevene E, Ballell L, Barros-Aguirre D (2016) Beta-Lactams against Tuberculosis–new trick for an old dog? N Engl J Med 375(4):393–394. https://doi.org/10.1056/NEJMc1513236
England K, Boshoff HI, Arora K, Weiner D, Dayao E, Schimel D, Via LE, Barry CE 3rd (2012) Meropenem-clavulanic acid shows activity against Mycobacterium tuberculosis in vivo. Antimicrob Agents Chemother 56(6):3384–3387. https://doi.org/10.1128/AAC.05690-11
Erdemli SB, Gupta R, Bishai WR, Lamichhane G, Amzel LM, Bianchet MA (2012) Targeting the cell wall of Mycobacterium tuberculosis: structure and mechanism of L,D-transpeptidase 2. Structure 20(12):2103–2115. https://doi.org/10.1016/j.str.2012.09.016
Falzon D, Gandhi N, Migliori GB, Sotgiu G, Cox HS, Holtz TH, Hollm-Delgado MG, Keshavjee S, DeRiemer K, Centis R, D’Ambrosio L, Lange CG, Bauer M, Menzies D, Collaborative Group for meta-analysis of individual patient data in M-T (2013) Resistance to fluoroquinolones and second-line injectable drugs: impact on multidrug-resistant TB outcomes. Eur Respir J 42(1):156–168. https://doi.org/10.1183/09031936.00134712
Giovanni Satta XG, Canseco JO, Wey E, Drobniewski F, McHugh TD (2018) 2447. Ertapenem and Faropenem for the Treatment of drug-resistant Tuberculosis. Open Forum Infect Dis 5:1
Gupta R, Lavollay M, Mainardi JL, Arthur M, Bishai WR, Lamichhane G (2010) The Mycobacterium tuberculosis protein LdtMt2 is a nonclassical transpeptidase required for virulence and resistance to amoxicillin. Nat Med 16(4):466–469. https://doi.org/10.1038/nm.2120
Gurumurthy M, Verma R, Naftalin CM, Hee KH, Lu Q, Tan KH, Issac S, Lin W, Tan A, Seng KY, Lee LS, Paton NI (2017) Activity of faropenem with and without rifampicin against Mycobacterium tuberculosis: evaluation in a whole-blood bactericidal activity trial. J Antimicrob Chemother 72(7):2012–2019. https://doi.org/10.1093/jac/dkx081
Hikida M, Kawashima K, Nishiki K, Furukawa Y, Nishizawa K, Saito I, Kuwao S (1992) Renal dehydropeptidase-I stability of LJC 10,627, a new carbapenem antibiotic. Antimicrob Agents Chemother 36(2):481–483
Horita Y, Maeda S, Kazumi Y, Doi N (2014) In vitro susceptibility of Mycobacterium tuberculosis isolates to an oral carbapenem alone or in combination with beta-lactamase inhibitors. Antimicrob Agents Chemother 58(11):7010–7014. https://doi.org/10.1128/AAC.03539-14
Hugonnet JE, Tremblay LW, Boshoff HI, Barry CE 3rd, Blanchard JS (2009) Meropenem-clavulanate is effective against extensively drug-resistant Mycobacterium tuberculosis. Science 323(5918):1215–1218. https://doi.org/10.1126/science.1167498
Isaakidis P, Das M, Kumar AM, Peskett C, Khetarpal M, Bamne A, Adsul B, Manglani M, Sachdeva KS, Parmar M, Kanchar A, Rewari BB, Deshpande A, Rodrigues C, Shetty A, Rebello L, Saranchuk P (2014) Alarming levels of drug-resistant tuberculosis in HIV-infected patients in metropolitan Mumbai, India. PLoS One 9(10):e110461. https://doi.org/10.1371/journal.pone.0110461
Jaganath D, Lamichhane G, Shah M (2016) Carbapenems against Mycobacterium tuberculosis: a review of the evidence. Int J Tuberc Lung Dis 20(11):1436–1447. https://doi.org/10.5588/ijtld.16.0498
Kaushik A, Makkar N, Pandey P, Parrish N, Singh U, Lamichhane G (2015) Carbapenems and Rifampin exhibit synergy against Mycobacterium tuberculosis and Mycobacterium abscessus. Antimicrob Agents Chemother 59(10):6561–6567. https://doi.org/10.1128/AAC.01158-15
Kaushik A, Ammerman NC, Tasneen R, Story-Roller E, Dooley KE, Dorman SE, Nuermberger EL, Lamichhane G (2017a) In vitro and in vivo activity of biapenem against drug-susceptible and rifampicin-resistant Mycobacterium tuberculosis. J Antimicrob Chemother 72(8):2320–2325. https://doi.org/10.1093/jac/dkx152
Kaushik A, Gupta C, Fisher S, Story-Roller E, Galanis C, Parrish N, Lamichhane G (2017b) Combinations of avibactam and carbapenems exhibit enhanced potencies against drug-resistant Mycobacterium abscessus. Future Microbiol 12:473–480. https://doi.org/10.2217/fmb-2016-0234
Keener AB (2014) Oldie but goodie: Repurposing penicillin for tuberculosis. Nat Med 20(9):976–978. https://doi.org/10.1038/nm0914-976
Kim HS, Kim J, Im HN, Yoon JY, An DR, Yoon HJ, Kim JY, Min HK, Kim SJ, Lee JY, Han BW, Suh SW (2013) Structural basis for the inhibition of Mycobacterium tuberculosis L,D-transpeptidase by meropenem, a drug effective against extensively drug-resistant strains. Acta Crystallogr D Biol Crystallogr 69 (Pt 3):420-431. doi:https://doi.org/10.1107/S0907444912048998
Kumar P, Kaushik A, Bell DT, Chauhan V, **a F, Stevens RL, Lamichhane G (2017a) Mutation in an unannotated protein confers Carbapenem resistance in Mycobacterium tuberculosis. Antimicrob Agents Chemother 61(3). https://doi.org/10.1128/AAC.02234-16
Kumar P, Kaushik A, Lloyd EP, Li SG, Mattoo R, Ammerman NC, Bell DT, Perryman AL, Zandi TA, Ekins S, Ginell SL, Townsend CA, Freundlich JS, Lamichhane G (2017b) Non-classical transpeptidases yield insight into new antibacterials. Nat Chem Biol 13(1):54–61. https://doi.org/10.1038/nchembio.2237
Matsumoto M, Hashizume H, Tomishige T, Kawasaki M, Tsubouchi H, Sasaki H, Shimokawa Y, Komatsu M (2006) OPC-67683, a nitro-dihydro-imidazooxazole derivative with promising action against tuberculosis in vitro and in mice. PLoS Med 3(11):e466. https://doi.org/10.1371/journal.pmed.0030466
Moraes GL, Gomes GC, Monteiro de Sousa PR, Alves CN, Govender T, Kruger HG, Maguire GE, Lamichhane G, Lameira J (2015) Structural and functional features of enzymes of Mycobacterium tuberculosis peptidoglycan biosynthesis as targets for drug development. Tuberculosis (Edinb) 95(2):95–111. https://doi.org/10.1016/j.tube.2015.01.006
Organization WH (2016) Global Tuberculosis Report 2016
Organization WH (2018) Global Tuberculosis Report 2018
Payen MC, Muylle I, Vandenberg O, Mathys V, Delforge M, Van den Wijngaert S, Clumeck N, De Wit S (2018) Meropenem-clavulanate for drug-resistant tuberculosis: a follow-up of relapse-free cases. Int J Tuberc Lung Dis 22(1):34–39. https://doi.org/10.5588/ijtld.17.0352
Prasad R, Singh A, Balasubramanian V, Gupta N (2017) Extensively drug-resistant tuberculosis in India: current evidence on diagnosis & management. Indian J Med Res 145(3):271–293. https://doi.org/10.4103/ijmr.IJMR_177_16
Ramon-Garcia S, Gonzalez Del Rio R, Villarejo AS, Sweet GD, Cunningham F, Barros D, Ballell L, Mendoza-Losana A, Ferrer-Bazaga S, Thompson CJ (2016) Repurposing clinically approved cephalosporins for tuberculosis therapy. Sci Rep 6:34293. https://doi.org/10.1038/srep34293
Schoonmaker MK, Bishai WR, Lamichhane G (2014) Nonclassical transpeptidases of Mycobacterium tuberculosis alter cell size, morphology, the cytosolic matrix, protein localization, virulence, and resistance to beta-lactams. J Bacteriol 196(7):1394–1402. https://doi.org/10.1128/JB.01396-13
Sharma D, Dhuriya YK, Deo N, Bisht D (2017) Repurposing and revival of the drugs: a new approach to combat the drug resistant Tuberculosis. Front Microbiol 8:2452. https://doi.org/10.3389/fmicb.2017.02452
Silva DR, Dalcolmo M, Tiberi S, Arbex MA, Munoz-Torrico M, Duarte R, D’Ambrosio L, Visca D, Rendon A, Gaga M, Zumla A, Migliori GB (2018) New and repurposed drugs to treat multidrug- and extensively drug-resistant tuberculosis. J Bras Pneumol 44(2):153–160. https://doi.org/10.1590/s1806-37562017000000436
Singh R, Manjunatha U, Boshoff HI, Ha YH, Niyomrattanakit P, Ledwidge R, Dowd CS, Lee IY, Kim P, Zhang L, Kang S, Keller TH, Jiricek J, Barry CE 3rd (2008) PA-824 kills nonreplicating Mycobacterium tuberculosis by intracellular NO release. Science 322(5906):1392–1395. https://doi.org/10.1126/science.1164571
Solapure S, Dinesh N, Shandil R, Ramachandran V, Sharma S, Bhattacharjee D, Ganguly S, Reddy J, Ahuja V, Panduga V, Parab M, Vishwas KG, Kumar N, Balganesh M, Balasubramanian V (2013) In vitro and in vivo efficacy of beta-lactams against replicating and slowly growing/nonreplicating Mycobacterium tuberculosis. Antimicrob Agents Chemother 57(6):2506–2510. https://doi.org/10.1128/AAC.00023-13
Sotgiu G, Alffenaar JW, Centis R, D’Ambrosio L, Spanevello A, Piana A, Migliori GB (2015a) Therapeutic drug monitoring: how to improve drug dosage and patient safety in tuberculosis treatment. Int J Infect Dis 32:101–104. https://doi.org/10.1016/j.ijid.2014.12.001
Sotgiu G, Centis R, D’Ambrosio L, Migliori GB (2015b) Tuberculosis treatment and drug regimens. Cold Spring Harb Perspect Med 5(5):a017822. https://doi.org/10.1101/cshperspect.a017822
Sotgiu G, D’Ambrosio L, Centis R, Tiberi S, Esposito S, Dore S, Spanevello A, Migliori GB (2016) Carbapenems to treat multidrug and extensively drug-resistant Tuberculosis: a systematic review. Int J Mol Sci 17(3):373. https://doi.org/10.3390/ijms17030373
Story-Roller E, Lamichhane G (2018) Have we realized the full potential of beta-lactams for treating drug-resistant TB? IUBMB Life 70(9):881–888. https://doi.org/10.1002/iub.1875
Tiberi S, D’Ambrosio L, De Lorenzo S, Viggiani P, Centis R, Sotgiu G, Alffenaar JW, Migliori GB (2016a) Ertapenem in the treatment of multidrug-resistant tuberculosis: first clinical experience. Eur Respir J 47(1):333–336. https://doi.org/10.1183/13993003.01278-2015
Tiberi S, Payen MC, Sotgiu G, D’Ambrosio L, Alarcon Guizado V, Alffenaar JW, Abdo Arbex M, Caminero JA, Centis R, De Lorenzo S, Gaga M, Gualano G, Roby Arias AJ, Scardigli A, Skrahina A, Solovic I, Sulis G, Tadolini M, Akkerman OW, Alarcon Arrascue E, Aleska A, Avchinko V, Bonini EH, Chong Marin FA, Collahuazo Lopez L, de Vries G, Dore S, Kunst H, Matteelli A, Moschos C, Palmieri F, Papavasileiou A, Spanevello A, Vargas Vasquez D, Viggiani P, White V, Zumla A, Migliori GB (2016b) Effectiveness and safety of meropenem/clavulanate-containing regimens in the treatment of MDR- and XDR-TB. Eur Respir J 47(4):1235–1243. https://doi.org/10.1183/13993003.02146-2015
Tiberi S, Sotgiu G, D’Ambrosio L, Centis R, Abdo Arbex M, Alarcon Arrascue E, Alffenaar JW, Caminero JA, Gaga M, Gualano G, Skrahina A, Solovic I, Sulis G, Tadolini M, Alarcon Guizado V, De Lorenzo S, Roby Arias AJ, Scardigli A, Akkerman OW, Aleksa A, Artsukevich J, Auchynka V, Bonini EH, Chong Marin FA, Collahuazo Lopez L, de Vries G, Dore S, Kunst H, Matteelli A, Moschos C, Palmieri F, Papavasileiou A, Payen MC, Piana A, Spanevello A, Vargas Vasquez D, Viggiani P, White V, Zumla A, Migliori GB (2016c) Comparison of effectiveness and safety of imipenem/clavulanate- versus meropenem/clavulanate-containing regimens in the treatment of MDR- and XDR-TB. Eur Respir J 47(6):1758–1766. https://doi.org/10.1183/13993003.00214-2016
Tremblay LW, Fan F, Blanchard JS (2010) Biochemical and structural characterization of Mycobacterium tuberculosis beta-lactamase with the carbapenems ertapenem and doripenem. Biochemistry 49(17):3766–3773. https://doi.org/10.1021/bi100232q
van Rijn SP, van Altena R, Akkerman OW, van Soolingen D, van der Laan T, de Lange WC, Kosterink JG, van der Werf TS, Alffenaar JW (2016) Pharmacokinetics of ertapenem in patients with multidrug-resistant tuberculosis. Eur Respir J 47(4):1229–1234. https://doi.org/10.1183/13993003.01654-2015
Walsh C (2003) Where will new antibiotics come from? Nat Rev Microbiol 1(1):65–70. https://doi.org/10.1038/nrmicro727
Watt B, Edwards JR, Rayner A, Grindey AJ, Harris G (1992) In vitro activity of meropenem and imipenem against mycobacteria: development of a daily antibiotic dosing schedule. Tuber Lung Dis 73(3):134–136. https://doi.org/10.1016/0962-8479(92)90145-A
Wong EB, Cohen KA, Bishai WR (2013) Rising to the challenge: new therapies for tuberculosis. Trends Microbiol 21(9):493–501. https://doi.org/10.1016/j.tim.2013.05.002
Yew WW, Chau CH (1996) New antimycobacterial agents. Monaldi Arch Chest Dis 51(5):394–404
Zhang D, Wang Y, Lu J, Pang Y (2016) In Vitro activity of beta-Lactams in combination with beta-Lactamase inhibitors against multidrug-resistant Mycobacterium tuberculosis Isolates. Antimicrob Agents Chemother 60(1):393–399. https://doi.org/10.1128/AAC.01035-15
Zumla A, Chakaya J, Centis R, D’Ambrosio L, Mwaba P, Bates M, Kapata N, Nyirenda T, Chanda D, Mfinanga S, Hoelscher M, Maeurer M, Migliori GB (2015) Tuberculosis treatment and management–an update on treatment regimens, trials, new drugs, and adjunct therapies. Lancet Respir Med 3(3):220–234. https://doi.org/10.1016/S2213-2600(15)00063-6
Zuur MA, Ghimire S, Bolhuis MS, Wessels AMA, van Altena R, de Lange WCM, Kosterink JGW, Touw DJ, van der Werf TS, Akkerman OW, Alffenaar JWC (2018) Pharmacokinetics of 2,000 milligram ertapenem in Tuberculosis patients. Antimicrob Agents Chemother 62(5). https://doi.org/10.1128/AAC.02250-17
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2019 Springer Nature Singapore Pte Ltd.
About this chapter
Cite this chapter
Kumar, P., Singh, U.B., Lamichhane, G., Story-Roller, E. (2019). Repurposing of Carbapenems for the Treatment of Drug-Resistant Tuberculosis. In: Hasnain, S., Ehtesham, N., Grover, S. (eds) Mycobacterium Tuberculosis: Molecular Infection Biology, Pathogenesis, Diagnostics and New Interventions. Springer, Singapore. https://doi.org/10.1007/978-981-32-9413-4_26
Download citation
DOI: https://doi.org/10.1007/978-981-32-9413-4_26
Published:
Publisher Name: Springer, Singapore
Print ISBN: 978-981-32-9412-7
Online ISBN: 978-981-32-9413-4
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)