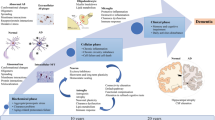
Abstract
Alzheimer’s disease (AD) is the most common type of neurodegenerative disease and is primarily characterized by progressive cognitive dysfunction and behavioral impairment. It accounts for approximately 50–75% of senile dementia cases. Mild cognitive impairment (MCI) is an intermediate state of cognition, somewhere between normal aging and dementia, and has a high risk of conversion to AD or other types of dementia, with approximately 10–15% of MCI cases converting to AD each year. With the steady increase in life expectancy, the incidence of AD has grown each year, and the number of patients with AD worldwide is projected to reach 130 million by 2050, which will place an immense burden on social development and home care. However, the pathogenesis of AD remains poorly understood, and currently, there is no effective pharmaceutical treatment. Therefore, AD continues to be a key focus of and challenge to research in the field of global medicine. The characteristic pathological changes observed in AD involve senile plaques that are formed by the extracellular deposition of β-amyloid (Aβ), intracellular neurofibrillary tangles (NFTs) that are formed of hyperphosphorylated tau protein, and extensive neuronal loss. The primary imaging techniques currently utilized in AD research include MRI and PET. Structural MRI can show the atrophy of the medial temporal lobe (MTL), which is now considered to be a diagnostic marker of AD, while functional MRI (fMRI) is a valuable tool for exploring the functional changes of the brain and the neurobiological mechanisms of AD. PET, however, is an important imaging technique for the detection of AD-specific brain metabolism and the in vivo assessment of pathological proteins. In this chapter, we will summarize the advances in research regarding the application of fMRI, PET, and PET/MR in the study of AD.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
Suggested Readings
Agosta F, Pievani M, Geroldi C, et al. Resting state fMRI in Alzheimer’s disease: beyond the default mode network. Neurobiol Aging. 2012;33:1564–78.
Aiello M, Salvatore E, Cachia A, et al. Relationship between simultaneously acquired resting-state regional cerebral glucose metabolism and functional MRI: a PET/MR hybrid scanner study. Neuroimage. 2015;113:111–21.
Alsop DC, Detre JA, Grossman M. Assessment of cerebral blood flow in Alzheimer’s disease by spin-labeled magnetic resonance imaging. Ann Neurol. 2000;47:93–100.
Binnewijzend MA, Benedictus MR, Kuijer JP, et al. Cerebral perfusion in the predementia stages of Alzheimer’s disease. Eur Radiol. 2016;26:506–14.
Binnewijzend MA, Kuijer JP, Benedictus MR, et al. Cerebral blood flow measured with 3D pseudocontinuous arterial spin-labeling MR imaging in Alzheimer disease and mild cognitive impairment: a marker for disease severity. Radiology. 2013;267:221–30.
Cho H, Choi JY, Hwang MS, et al. In vivo cortical spreading pattern of tau and amyloid in the Alzheimer disease spectrum. Ann Neurol. 2016;80(2):247–58.
Clark CM, Pontecorvo MJ, Beach TG, et al. Cerebral PET with florbetapir compared with neuropathology at autopsy for detection of neuritic amyloid-beta plaques: a prospective cohort study. Lancet Neurol. 2012;11(8):669–78.
Dai W, Lopez OL, Carmichael OT, et al. Mild cognitive impairment and Alzheimer disease: patterns of altered cerebral blood flow at MR imaging. Radiology. 2009;250:856–66.
Franzmeier N, Rubinski A, Neitzel J, et al. Functional connectivity associated with tau levels in ageing, Alzheimer’s, and small vessel disease. Brain. 2019;142:1093–107.
Gardini S, Venneri A, Sambataro F, et al. Increased functional connectivity in the default mode network in mild cognitive impairment: a maladaptive compensatory mechanism associated with poor semantic memory performance. J Alzheimers Dis. 2015;45:457–70.
Gottler J, Preibisch C, Riederer I, et al. Reduced blood oxygenation level dependent connectivity is related to hypoperfusion in Alzheimer’s disease. J Cereb Blood Flow Metab. 2019;39:1314–25.
Han SD, Houston WS, Jak AJ, et al. Verbal paired-associate learning by APOE genotype in non-demented older adults: fMRI evidence of a right hemispheric compensatory response. Neurobiol Aging. 2007;28:238–47.
Hoenig MC, Bischof GN, Seemiller J, et al. Networks of tau distribution in Alzheimer’s disease. Brain. 2018;141:568–81.
Im HK, Nebes R, Snitz B, et al. Regional amyloid burden and intrinsic connectivity networks in cognitively normal elderly subjects. Brain. 2014;137:3327–38.
Jack CR, Bennett DA, Blennow K, et al. NIA-AA research framework: toward a biological definition of Alzheimer's disease. Alzheimers Dement. 2018;14(4):535–62.
Kantarci K, Lowe V, Przybelski SA, et al. Magnetic resonance spectroscopy, beta-amyloid load, and cognition in a population-based sample of cognitively normal older adults. Neurology. 2011;77:951–8.
Kuhl DE, Koeppe RA, Minoshima S, et al. In vivo map** of cerebral acetylcholinesterase activity in aging and Alzheimer’s disease. Neurology. 1999;52(4):691–9.
Lacalle-Aurioles M, Mateos-Perez JM, Guzman-De-Villoria JA, et al. Cerebral blood flow is an earlier indicator of perfusion abnormalities than cerebral blood volume in Alzheimer’s disease. J Cereb Blood Flow Metab. 2014;34:654–9.
Liu M, Paranjpe MD, Zhou X, Duy PQ, Goyal MS, Benzinger TLS, Lu J, Wang R, Zhou Y. Sex modulates the ApoE epsilon4 effect on brain tau deposition measured by (18)F-AV-1451 PET in individuals with mild cognitive impairment. Theranostics. 2019;9(17):4959–70.
Marchitelli R, Aiello M, Cachia A, et al. Simultaneous resting-state FDG-PET/fMRI in Alzheimer disease: relationship between glucose metabolism and intrinsic activity. Neuroimage. 2018;176:246.
Mitolo M, Stanzani-Maserati M, Capellari S, et al. Predicting conversion from mild cognitive impairment to Alzheimer’s disease using brain (1)H-MRS and volumetric changes: a two-year retrospective follow-up study. Neuroimage Clin. 2019;23:101843.
Nowrangi MA, Lyketsos CG, Leoutsakos JM, et al. Longitudinal, region-specific course of diffusion tensor imaging measures in mild cognitive impairment and Alzheimer’s disease. Alzheimers Dement. 2013;9:519–28.
Paranjpe MD, Chen X, Liu M, et al. The effect of ApoE epsilon4 on longitudinal brain region-specific glucose metabolism in patients with mild cognitive impairment: a FDG-PET study. Neuroimage Clin. 2019;22:101795.
Riederer I, Bohn KP, Preibisch C, et al. Alzheimer disease and mild cognitive impairment: integrated pulsed arterial spin-labeling MRI and (18)F-FDG PET. Radiology. 2018;288:198–206.
Riedl V, Bienkowska K, Strobel C, et al. Local activity determines functional connectivity in the resting human brain: a simultaneous FDG-PET/fMRI study. J Neurosci. 2014;34:6260–6.
Rzezga A, Becker JA, Van Dijk KR, et al. Neuronal dysfunction and disconnection of cortical hubs in non-demented subjects with elevated amyloid burden. Brain. 2011;134:1635–46.
Scherr M, Utz L, Tahmasian M, et al. Effective connectivity in the default mode network is distinctively disrupted in Alzheimer’s disease-a simultaneous resting-state FDG-PET/fMRI study. Hum Brain Mapp. 2021;42:4134–43.
Sorg C, Riedl V, Muhlau M, et al. Selective changes of resting-state networks in individuals at risk for Alzheimer's disease. Proc Natl Acad Sci U S A. 2007;104:18760–5.
Su L, Blamire AM, Watson R, et al. Whole-brain patterns of (1)H-magnetic resonance spectroscopy imaging in Alzheimer’s disease and dementia with Lewy bodies. Transl Psychiatry. 2016;6:e877.
Tahmasian M, Pasquini L, Scherr M, et al. The lower hippocampus global connectivity, the higher its local metabolism in Alzheimer disease. Neurology. 2015;84:1956–63.
Thomas B, Sheelakumari R, Kannath S, et al. Regional cerebral blood flow in the posterior cingulate and precuneus and the entorhinal cortical atrophy score differentiate mild cognitive impairment and dementia due to Alzheimer Disease. AJNR Am J Neuroradiol. 2019;40:1658–64.
Villemagne VL, Fodero-Tavoletti MT, Masters CL, et al. Tau imaging: early progress and future directions. Lancet Neurol. 2015;14(1):114–24.
Voevodskaya O, Poulakis K, Sundgren P, et al. Brain myoinositol as a potential marker of amyloid-related pathology: a longitudinal study. Neurology. 2019;92:e395–405.
Wang H, Tan L, Wang HF, et al. Magnetic resonance spectroscopy in Alzheimer’s disease: systematic review and meta-analysis. J Alzheimers Dis. 2015;46:1049–70.
Yan S, Qi Z, An Y, et al. Detecting perfusion deficit in Alzheimer’s disease and mild cognitive impairment patiets by resting-state fMRI. J Magn Reson Imaging. 2019;49(4):1099–104.
Yan S, Zheng C, Cui B, et al. Multiparametric imaging hippocampal neurodegeneration and functional connectivity with simultaneous PET-MRI in Alzheimer’s disease. Eur J Nucl Med Mol Imaging. 2020;47(10):2440–52.
Yan S, Zheng C, Manish DP, Li J, et al. Association of sex and APOE ε4 with brain tau deposition and atrophy in older adults with Alzheimer’s disease. Theranostics. 2020;10(23):10563–72.
Zhang HY, Wang SJ, Liu B, et al. Resting brain connectivity: changes during the progress of Alzheimer disease. Radiology. 2010;256:598–606.
Zhou J, Greicius MD, Gennatas ED, et al. Divergent network connectivity changes in behavioural variant frontotemporal dementia and Alzheimer’s disease. Brain. 2010;133:1352–67.
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2023 The Author(s), under exclusive license to Springer Nature Singapore Pte Ltd.
About this chapter
Cite this chapter
Yan, S., Liu, M., Qi, Z., Lu, J. (2023). Research Applications of Positron Emission Tomography/Magnetic Resonance (PET/MR) Imaging in Alzheimer’s Disease (AD). In: Lu, J., Zhao, G. (eds) PET/MR: Functional and Molecular Imaging of Neurological Diseases and Neurosciences. Springer, Singapore. https://doi.org/10.1007/978-981-19-9902-4_8
Download citation
DOI: https://doi.org/10.1007/978-981-19-9902-4_8
Published:
Publisher Name: Springer, Singapore
Print ISBN: 978-981-19-9901-7
Online ISBN: 978-981-19-9902-4
eBook Packages: MedicineMedicine (R0)