Abstract
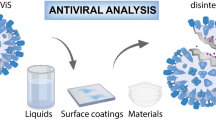
In this chapter, we surveyed the differences of viral behaviors inside and outside of our bodies. Then, we introduced an international standard to evaluate the viral activity on various materials. This evaluation technique is the combination of a film covering method developed for antibacterial evaluation of materials by SIAA (Society of International Sustaining Growth of Antimicrobial Articles) in Japan and the conventional plaque assay. However, this evaluation process provides visualization to the researchers and engineers who use it. From this viewpoint, we would say the method is intuitive, rapid, relatively inexpensive, and user-friendly. It is used in industry to evaluate materials.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Lee, G., & Bishop, P. (2015). Microbiology—and infection control for health professional (6th ed.). Pearson.
Nelson, D. L., & Cox, M. M. (2008). Lehninger principles of biochemistry (5th ed.). W. H. Freeman.
Lostroh, P. (2019). Molecular and cellular biology of viruses (Vol. 523). Garland Science.
Djellabi, R., Basilico, N., Delbue, S., D’Alessandro, S., Parapini, S., Cerrato, G., Laurenti, E., Falletta, E., & Bianchi, C. L. (2021). Oxidative Inactivation of SARS-CoV-2 on Photoactive AgNPs@TiO2 Ceramic Tiles. Int. J. Mol. Sci., 22, 8836. https://doi.org/10.3390/ijms22168836.
Butot, S., Baert, L., & Zuber, S. (2021). Assessment of antiviral coatings for high-touch surfaces by using human coronaviruses HCoV-229E and SARS-CoV-2. Applied and Environmental Microbiology, 87(19), e01098–e01021.
Thraenhart, O., Jursch, C., & Buozzi, V. B. (2021). Testing of the antiviral equipped product “Argentum 20 a-Base” against the Bovine Coronavirus (Bocv) at 25°C –Evaluation of the virucidal activity against the Bovine Coronavirus (S379 Riems) using the quantitative carrier test according to ISO 21702: 2019. (Excerpt from the Test Report Ter_Eur-09_181220_Bocv). Eurofins Co.
Fu, H., & Gray, K. A. (2021). The key to maximizing the benefits of antimicrobial and self-cleaning coatings is to fully determine their risks. Current Opinion in Chemical Engineering, 34, 100761.
Tatsuma, T., Nakakido, M., Ichinohe, T., Kuroiwa, Y., Tomioka, K., Liu, C., Wakihara, T., et al. (2021). Inactivation of novel coronavirus and alpha variant by photo-renewable CuxO/TiO2 nanocomposites. Cambridge University Press.
Hong, S. G., Lee, Y. K., Yim, J. H., Chun, J., & Lee, H. K. (2008). Sanguibacter antarcticus sp. nov., isolated from Antarctic Sea sand. International Journal of Systematic and Evolutionary Microbiology, 58(1), 50–52.
Falcó, I., Randazzo, W., Sánchez, G., Vilarroig, J., Climent, J., Chiva, S., Navarro-Laboulais, J., et al. (2021). Experimental and CFD evaluation of ozone efficacy against coronavirus and enteric virus contamination on public transport surfaces. Journal of Environmental Chemical Engineering, 9(5), 106217.
Li, Z., Qiao, D., Xu, Y., Zhou, E., Yang, C., Yuan, X., Wang, F., et al. (2021). Cu-bearing high-entropy alloys with excellent antiviral properties. Journal of Materials Science & Technology, 84, 59–64.
Kanematsu, H., Kawai, R., & Barry, D. M. (2021). Measuring virus infectivity on material surfaces: Various methods are available to evaluate the behavior of viruses on material surfaces, an important area of research for determining how long a virus can live on an inanimate object, and learning how to design and develop advanced antiviral materials. Advanced Materials & Processes, 179(5), 28–31.
Govind, V., Bharadwaj, S., Sai Ganesh, M. R., Vishnu, J., Shankar, K. V., Shankar, B., & Rajesh, R. (2021). Antiviral properties of copper and its alloys to inactivate COVID-19 virus: A review. Biometals, 34(6), 1217–1235.
Botequim, D., Maia, J., Lino, M. M. F., Lopes, L. M. F., Simões, P. N., Ilharco, L. M., & Ferreira, L. (2012). Nanoparticles and surfaces presenting antifungal, antibacterial and antiviral properties. Langmuir, 28(20), 7646–7656.
Jung, S., Yang, J. Y., Byeon, E. Y., Kim, D. G., Lee, D. G., Ryoo, S., Lee, S., et al. (2021). Copper-coated polypropylene filter face mask with SARS-COV-2 antiviral ability. Polymers, 13(9), 1367.
Ordon, M., Nawrotek, P., Stachurska, X., & Mizielińska, M. (2021). Polyethylene films coated with antibacterial and antiviral layers based on CO2 extracts of raspberry seeds, of pomegranate seeds and of rosemary. Coatings, 11(10), 1179.
Seidi, F., Deng, C., Zhong, Y., Liu, Y., Huang, Y., Li, C., & **ao, H. (2021). Functionalized masks: Powerful materials against COVID-19 and future pandemics. Small, 17(42), 2102453.
Idumah, C. I. (2021). Influence of nanotechnology in polymeric textiles, applications, and fight against COVID-19. The Journal of the Textile Institute, 112(12), 2056–2076.
Malmsten, M. (2011). Antimicrobial and antiviral hydrogels. Soft Matter, 7(19), 8725–8736.
Nowacek, A. S., Balkundi, S., McMillan, J., Roy, U., Martinez-Skinner, A., Mosley, R. L., Gendelman, H. E., et al. (2011). Analyses of nanoformulated antiretroviral drug charge, size, shape and content for uptake, drug release and antiviral activities in human monocyte-derived macrophages. Journal of Controlled Release, 150(2), 204–211.
Chen, L., & Liang, J. (2020). An overview of functional nanoparticles as novel emerging antiviral therapeutic agents. Materials Science and Engineering: C, 112, 110924.
Mallakpour, S., Azadi, E., & Hussain, C. M. (2021). Recent breakthroughs of antibacterial and antiviral protective polymeric materials during COVID-19 pandemic and post-pandemic: Coating, packaging, and textile applications. Current Opinion in Colloid & Interface Science, 55, 101480.
Tang, S., Puryear, W. B., Seifried, B. M., Dong, X., Runstadler, J. A., Ribbeck, K., & Olsen, B. D. (2016). Antiviral agents from multivalent presentation of sialyl oligosaccharides on brush polymers. ACS Macro Letters, 5(3), 413–418.
Erkoc, P., & Ulucan-Karnak, F. (2021). Nanotechnology-based antimicrobial and antiviral surface coating strategies. PRO, 3(1), 25–52.
Rosilo, H., McKee, J. R., Kontturi, E., Koho, T., Hytönen, V. P., Ikkala, O., & Kostiainen, M. A. (2014). Cationic polymer brush-modified cellulose nanocrystals for high-affinity virus binding. Nanoscale, 6(20), 11871–11881.
Koylu, D., & Carter, K. R. (2009). Stimuli-responsive surfaces utilizing cleavable polymer brush layers. Macromolecules, 42(22), 8655–8660.
Zan, T., Wu, F., Pei, X., Jia, S., Zhang, R., Wu, S., Zhang, Z., et al. (2016). Into the polymer brush regime through the “grafting-to” method: Densely polymer-grafted rodlike viruses with an unusual nematic liquid crystal behavior. Soft Matter, 12(3), 798–805.
Riedel, T., Rodriguez-Emmenegger, C., de los Santos Pereira, A., Bědajánková, A., **och, P., Boltovets, P. M., & Brynda, E. (2014). Diagnosis of Epstein–Barr virus infection in clinical serum samples by an SPR biosensor assay. Biosensors and Bioelectronics, 55, 278–284.
Demirci, S., Kinali-Demirci, S., & Jiang, S. (2017). A switchable polymer brush system for antifouling and controlled detection. Chemical Communications, 53(26), 3713–3716.
Vermisoglou, E., Panáček, D., Jayaramulu, K., Pykal, M., Frébort, I., Kolář, M., Otyepka, M., et al. (2020). Human virus detection with graphene-based materials. Biosensors and Bioelectronics, 166, 112436.
Afsahi, S., Lerner, M. B., Goldstein, J. M., Lee, J., Tang, X., Bagarozzi, D. A., Jr., Goldsmith, B. R., et al. (2018). Novel graphene-based biosensor for early detection of Zika virus infection. Biosensors and Bioelectronics, 100, 85–88.
Liu, F., Choi, K. S., Park, T. J., Lee, S. Y., & Seo, T. S. (2011). Graphene-based electrochemical biosensor for pathogenic virus detection. BioChip Journal, 5(2), 123–128.
Joshi, S. R., Sharma, A., Kim, G. H., & Jang, J. (2020). Low cost synthesis of reduced graphene oxide using biopolymer for influenza virus sensor. Materials Science and Engineering: C, 108, 110465.
Deokar, A. R., Nagvenkar, A. P., Kalt, I., Shani, L., Yeshurun, Y., Gedanken, A., & Sarid, R. (2017). Graphene-based “hot plate” for the capture and destruction of the herpes simplex virus type 1. Bioconjugate Chemistry, 28(4), 1115–1122.
**, X., Zhang, H., Li, Y. T., **ao, M. M., Zhang, Z. L., Pang, D. W., Zhang, G. J., et al. (2019). A field effect transistor modified with reduced graphene oxide for immunodetection of Ebola virus. Microchimica Acta, 186(4), 1–9.
Innocenzi, P., & Stagi, L. (2020). Carbon-based antiviral nanomaterials: Graphene, C-dots, and fullerenes. A perspective. Chemical Science, 11(26), 6606–6622.
Palmieri, V., & Papi, M. J. N. T. (2020). Can graphene take part in the fight against COVID-19? Nano Today, 33, 100883.
Ye, S., Shao, K., Li, Z., Guo, N., Zuo, Y., Li, Q., Han, H., et al. (2015). Antiviral activity of graphene oxide: How sharp edged structure and charge matter. ACS Applied Materials & Interfaces, 7(38), 21571–21579.
Du, T., Lu, J., Liu, L., Dong, N., Fang, L., **ao, S., & Han, H. (2018). Antiviral activity of graphene oxide–silver nanocomposites by preventing viral entry and activation of the antiviral innate immune response. ACS Applied Bio Materials, 1(5), 1286–1293.
Darling, A. J., Boose, J. A., & Spaltro, J. (1998). Virus assay methods: Accuracy and validation. Biologicals, 26(2), 105–110.
Manceur, A. P., & Kamen, A. A. (2015). Critical review of current and emerging quantification methods for the development of influenza vaccine candidates. Vaccine, 33(44), 5913–5919.
Baer, A., & Kehn-Hall, K. (2014). Viral concentration determination through plaque assays: Using traditional and novel overlay systems. Journal of Visualized Experiments, (93), e52065.
Smither, S. J., Lear-Rooney, C., Biggins, J., Pettitt, J., Lever, M. S., & Olinger, G. G., Jr. (2013). Comparison of the plaque assay and 50% tissue culture infectious dose assay as methods for measuring filovirus infectivity. Journal of Virological Methods, 193(2), 565–571.
Tobita, K., Sugiura, A., Enomoto, C., & Furuyama, M. (1975). Plaque assay and primary isolation of influenza A viruses in an established line of canine kidney cells (MDCK) in the presence of trypsin. Medical Microbiology and Immunology, 162(1), 9–14.
Wiegand, C., Völpel, A., Ewald, A., Remesch, M., Kuever, J., Bauer, J., Bossert, J., et al. (2018). Critical physiological factors influencing the outcome of antimicrobial testing according to ISO 22196/JIS Z 2801. PLoS One, 13(3), e0194339.
Cunliffe, A. J., Askew, P. D., Stephan, I., Iredale, G., Cosemans, P., Simmons, L. M., Redfern, J., et al. (2021). How do we determine the efficacy of an antibacterial surface? A review of standardised antibacterial material testing methods. Antibiotics, 10(9), 1069.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2022 The Author(s), under exclusive license to Springer Nature Singapore Pte Ltd.
About this chapter
Cite this chapter
Kanematsu, H., Barry, D. (2022). Viral Behaviors on Materials and the International Standard Between Materials and Microbial/Viral Environments. In: Barry, D., Kanematsu, H. (eds) Studies to Combat COVID-19 using Science and Engineering. Springer, Singapore. https://doi.org/10.1007/978-981-19-1356-3_4
Download citation
DOI: https://doi.org/10.1007/978-981-19-1356-3_4
Published:
Publisher Name: Springer, Singapore
Print ISBN: 978-981-19-1355-6
Online ISBN: 978-981-19-1356-3
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)