Abstract
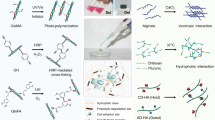
The design of bioactive scaffolding materials with favorable properties is paramount for successful application in biomedical engineering. Polymeric hydrogels attract significant attention as leading candidates for scaffold engineering due to their specific compositional and structural similarities to the natural extracellular matrix. The ability to control porosity, surface morphology, and size of hydrogel scaffolds has created new approaches to overcome various issues in tissue engineering such as vascularization, tissue architecture, and simultaneous multiple cells seeding. This review imparts an overview of hydrogel scaffolds based on synthetic and natural polymeric components (alginate, gelatin, and 2-hydroxyethyl methacrylate). We made hydrogel scaffolds with unique properties. Their in vitro and in vivo biological response, morphology, mechanical properties, porosity, hydrophilicity, and degradability were tested to find optimal patterns of tissue regeneration.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Aldana AA, Abraham GA (2017) Current advances in electrospun gelatin-based scaffolds for tissue engineering applications. Int J Pharm 523:441–453
Alves da Silva M, Martins A, Costa-Pinto AR, Monteiro N, Faria S, Reis RL, Neves NM (2017) Electrospun nanofibrous meshes cultured with Wharton’s jelly stem cell: an alternative for cartilage regeneration, without the need of growth factors. Biotechnol J. https://doi.org/10.1002/biot.201700073
Amado S, Morouço P, Pascoal-Faria P, Alves N (2017) Tailoring Bioengineered scaffolds for regenerative medicine. In: Dobrzański LA (ed) Biomaterials in regenerative medicine. IntechOpen, London. https://doi.org/10.5772/intechopen.69857. Available from: https://www.intechopen.com/chapters/56531
Annabi N, Nichol JW, Zhong X, Ji C et al (2010) Controlling the porosity and microarchitecture of hydrogels for tissue engineering. Tissue Eng Part B16:371–383
Atala A (2008) Advances in tissue and organ replacement. Curr Stem Cell Res Ther 3:21–31
Atala A (2012) Regenerative medicine strategies. J Pediatr Surg 47:17–28
Babić MM, Tomić SLj (2020) Semi-interpenetrating networks based on (Meth)acrylate, itaconic acid, and poly(vinyl Pyrrolidone) hydrogels for biomedical applications. In: Jana S, Jana S (eds) Interpenetrating polymer network: biomedical applications. Springer, Singapore, pp 263–288
Babitha S, Rachita L, Karthikeyan K, Shoba E, Janani I, Poornima B et al (2017) Electrospun protein nanofibers in healthcare: a review. Int J Pharm 523:52–90
Bailey AM, Mendicino M, Au P (2014) An FDA perspective on preclinical development of cell-based regenerative medicine products. Nat Biotechnol 32:721–723
Bajpai AK, Kankane S (2007) Preparation and characterization of macroporous poly(2-hydroxyethyl methacrylate)-based biomaterials: water sorption property and in vitro blood compatibility. J Appl Polym Sci 104:1559–1571
Baker BM, Trappmann B, Wang WY, Sakar MS, Kim IL, Shenoy VB, Burdick JA, Chen CS (2015) Cell-mediated fibre recruitment drives extracellular matrix mechanosensing in engineered fibrillar microenvironments. Nat Mater 14:1262–1268
Bakhsheshi-Rad HR, Hadisi Z, Hamzah E, Ismail AF, Aziz M, Kashefian M (2017) Drug delivery and cytocompatibility of ciprofloxacin loaded gelatin nanofibers-coated Mg alloy. Mater Lett 207:179–182
Barros TP, Alderton WK, Reynolds HM, Roach AG, Berghmans S (2008) Zebrafish: an emerging technology for in vivo pharmacological assessment to identify potential safety liabilities in early drug discovery. Br J Pharmacol 154:1400–1413
Behravesh E, Mikos AG (2003) Three-dimensional culture of differentiating marrow stromal osteoblasts in biomimetic poly(propylene fumarate-co-ethylene glycol)-based macroporous hydrogels. J Biomed Mater Res A 66:698–706
Bettinger CJ, Borenstein JT, Langer R (2007) Micro- and nanofabricated scaffolds. In: Lanza R, Langer R, Vacanti J (eds) Principles of tissue engineering, 3rd edn. Elsevier Academic Press, San Diego, CA, pp 341–358
Bigi A, Panzavolta S, Rovery N (1998) Hydroxyapatite-gelatin films: a structural and mechanical characterization. Biomaterials 19:739–744
Borselli C, Storrie H, Benesch-Lee F, Shvartsman D, Cezar C, Lichtman JW, Vandenburgh HH, Mooney DJ (2010) Functional muscle regeneration with combined delivery of angiogenesis and myogenesis factors. Proc Natl Acad Sci U S A 107:3287–3292
Boyan BD, Lohmann CH, Romero J, Schwartz Z (1999) Bone and cartilage tissue engineering. Clin Plast Surg 26:629–645
Brauker JH, Carr-Brendel VE, Martinson LA, Crudele J, Johnston WD, Johnson RC (1995) Neovascularization of synthetic membranes directed by membrane microarchitecture. J Biomed Mater Res 29:1517–1524
Bryant SJ, Anseth KS (2001) The effects of scaffold thickness on tissue engineered cartilage in photocrosslinked poly(ethylene oxide) hydrogels. Biomaterials 22:619–626
Bryant SJ, Davis-Arehart KA, Luo N, Shoemaker RK, Arthur JA, Anseth KS (2004) Synthesis and characterization of photopolymerized multifunctional hydrogels: water-soluble poly(vinyl alcohol) and chondroitin sulfate macromers for chondrocyte encapsulation. Macromolecules 37:6726–6733
Budama-Kilinc Y, Cakir-Koc R, Aslan B, Özkan B, Mutlu H, Üstün E (2017) Hydrogels in regenerative medicine. In: Dobrzański LA (ed) Biomaterials in regenerative medicine. IntechOpen. https://doi.org/10.5772/intechopen.70409
Cabodi M, Choi NW, Gleghorn JP, Lee CSD, Bonassar LJ, Stroock AD (2005) A microfluidic biomaterial. J Am Chem Soc 127:13788–13789
Camarero-Espinosa S, Cooper-White J (2016) Tailoring biomaterial scaffolds for osteochondral repair. Int J Pharm 523:476–489
Cascone MG, Barbani N, Cristallini C, Giusti P, Ciardelli G, Lazzeri L (2001) Bioartificial polymeric materials based on polysaccharides. Aust J Biol Sci 12:267–281
Chang H-I and Wang Y (2011) Cell responses to surface and architecture of tissue engineering scaffolds. In: Eberli D (ed) Regenerative medicine and tissue engineering-cells and biomaterials, BoD – books on demand. https://doi.org/10.5772/21983
Chen LJ, Wang M (2002) Production and evaluation of biodegradable composites based on PHB-PHV copolymer. Biomaterials 23:2631–2639
Cheung DYC, Duan B, Butcher JT (2015) Bioprinting of cardiac tissues. In: Atala A, Yoo JJ (eds) Essentials of 3D biofabrication and translation. Academic Press, Elsevier Science, London, pp 351–370
Cho SJ, Jung SM, Kang M, Shin HS, Youk JH (2015) Preparation of hydrophilic PCL nanofiber scaffolds via electrospinning of PCL/PVP-b-PCL block copolymers for enhanced cell biocompatibility. Polymer 69:95–102. https://doi.org/10.1016/j.polymer.2015.05.037
Choi K, Kuhn J, Ciarelli M, Goldstein S (1990) The elastic moduli of human subchondral, trabecular, and cortical bone tissue and the size-dependency of cortical bone modulus. J Biomech 23:1103–1113
Ciardelli G, Chiono V, Vozzi G, Pracella M, Ahluwalia A, Barbani N, Cristallini C, Giusti P (2005) Blends of poly(ε-caprolactone) and polysaccharides in tissue engineering applications. Biomacromolecules 6:1961–1976
Cosson S, Otte EA, Hezaveh H, Cooper-White JJ (2015) Concise review: tailoring bioengineered scaffolds for stem cell applications in tissue engineering and regenerative medicine. Stem Cells Transl Med 4:156–164
Das S, Subuddhi U (2020) Alginate-based interpenetrating network carriers for biomedical applications. In: Jana S, Jana S (eds) Interpenetrating polymer network: biomedical applications. Springer, Singapore, pp 79–118
Diamond DA, Caldamone AA (1999) Endoscopic treatment of vesicoureteric reflux in children using autologous chondrocytes-preliminary results. J Urol 162:1185–1188
Diedwardo CA, Petrosko P, Acarturk TO, Dimilia PA, Laframboise WA, Johnson PC (1999) Muscle tissue engineering. Clin Plast Surg 26:647–656
Dzobo K, Turnley T, Wishart A et al (2016) Fibroblast-derived extracellular matrix induces chondrogenic differentiation in human adipose-derived mesenchymal stromal/stem cells in vitro. Int J Mol Sci. https://doi.org/10.3390/ijms17081259
Eaglstein WH, Falanga V (1998) Tissue engineering and the development of Apligraf a human skin equivalent. AdvWound Care 11:1–8
Engler AJ, Sen S, Sweeney HL, Discher DE (2006) Matrix elasticity directs stem cell lineage specification. Cell 126:677–689
Evans ND, Gentleman E, Chen X, Roberts CJ, Polak JM, Stevens MM (2010) Extracellular matrix-mediated osteogenic differentiation of murine embryonic stem cells. Biomaterials 31:3244–3252
Eyrich D, Brandl F, Appel B et al (2007) Long-term stable fibrin gels for cartilage engineering. Biomaterials 28:55–65
Fang Z, Starly B, Sun W (2005) Computer-aided characterization for effective mechanical properties of porous tissue scaffolds. CAD Comput Aided Design 37:65–72
Fiedler T, Videira AC, Bártolo P, Strauch M, Murch GE, Ferreira JMF (2015) On the mechanical properties of PLC-bioactive glass scaffolds fabricated via BioExtrusion. Mater Sci Eng C 57:288–293
Gao G, Cui X (2016) Three-dimensional bioprinting in tissue engineering and regenerative medicine. Biotechnol Lett 38:203–211
Gao C, Tang F, Gong G, Zhang J, Hoi MPM, Lee SMY, Wang R (2017) pH-responsive prodrug nanoparticles based on a sodium alginate derivative for selective co-release of doxorubicin and curcumin into tumor cells. Nanoscale 9:12533–12542
Germain L, Auger FA, Grandbois E et al (1999) Reconstructed human cornea produced in vitro by tissue engineering. Pathobiology 67:140–147
Goncalves AI, Rodrigues MT, Gomes ME (2017) Tissue engineered magnetic cell sheet patches for advanced strategies in tendon regeneration. Acta Biomater 63:110–122
Guan X, Avci-Adali M, Alarcin E et al (2017) Development of hydrogels for regenerative engineering. Biotechnol J 12(5):1600394. https://doi.org/10.1002/biot.201600394
Gunatillake P, Mayadunne R, Adhikari R (2006) Recent developments in biodegradable synthetic polymers. Biotechnol Annu Rev 12:301–347
Guvendiren M, Burdick JA (2012) Stiffening hydrogels to probe short- and long-term cellular responses to dynamic mechanics. Nat Commun 3:792
Hashimoto T, Suzuki Y, Suzuki K, Nakashima T, Tanihara M, Ide C (2005) Peripheral nerve regeneration using non-tubular alginate gel crosslinked with covalent bonds. J Mater Sci Mater Med 16:503–509
Haycock JW (2011) 3D cell culture: a review of current approaches and techniques. Methods Mol Biol 695:1–15
Hejcl A, Urdzikova L, Sedy J, Lesny P, Pradny M, Michalek J, Burian M, Hajek M, Zamecnik J, Jendelova P, Sykova E (2008) Acute and delayed implantation of positively charged 2-hydroxyethyl methacrylate scaffolds in spinal cord injury in the rat. J Neurosurg Spine 8:67–73
Hench LL (1998) Bioceramics. J Am Ceram Soc 81:1705–1727
Hersel U, Dahmen C, Kessler H (2003) RGD modified polymers: biomaterials for stimulated cell adhesion and beyond. Biomaterials 24:4385–4415
Hill E, Boontheekul T, Mooney DJ (2006a) Designing scaffolds to enhance transplanted myoblast survival and migration. Tissue Eng 12:1295–1304
Hill E, Boontheekul T, Mooney DJ (2006b) Regulating activation of transplanted cells controls tissue regeneration. Proc Natl Acad Sci U S A 103:2494–2499
Hoffman AS (2001) Hydrogels for biomedical applications. Ann N Y Acad Sci 944:62–73
Huang Y, Onyeri S, Siewe M, Moshfeghian A, Madihally SV (2005) In vitro characterization of chitosan–gelatin scaffolds for tissue engineering. Biomaterials 26:7616–7627
Hubbell JA (1999) Bioactive biomaterials. Curr Opin Biotechnol 10:123–129
Huebsch N, Arany PR, Mao AS, Shvartsman D, Ali OA, Bencherif SA, Rivera-Feliciano J, Mooney DJ (2010) Harnessing traction-mediated manipulation of the cell/matrix interface to control stem-cell fate. Nat Mater 9:518–526
Hutmacher DW (2001) Scaffold design and fabrication technologies for engineering tissues-state of the art and future perspectives. J Biomat Sci Polym E 12:107–124
Jhon MS, Andrade JD (1973) Water and hydrogels. J Biomed Mater Res 7:509–522
Ji Y, Ghosh K, Shu XZ, Li B, Sokolov JC, Prestwich GD, Clark RAF, Rafailovich MH (2006) Electrospun three-dimensional hyaluronic acid nanofibrous scaffolds. Biomaterials 27:3782–3792
Joodaki H, Panzer MB (2018) Skin mechanical properties and modeling: a review. Proc Inst Mech Eng H. https://doi.org/10.1177/0954411918759801
Kariduraganavar MY (2016) Advances in polymers and tissue engineering scaffolds. In: Inamuddin (ed) Green polymer composites technology properties and applications. CRC Press, Boca Raton, FL, pp 343–354
Kataoka K, Suzuki Y, Kitada M, Hashimoto T, Chou H, Bai HL, Ohta M, Wu S, Suzuki K, Ide C (2004) Alginate enhances elongation of early regenerating axons in spinal cord of young rats. Tissue Eng 10:493–504
Ker EDF, Nain AS, Weiss LE, Wang J, Suhan J, Amon CH et al (2011) Bioprinting of growth factors onto aligned sub-micron fibrous scaffolds for simultaneous control of cell differentiation and alignment. Biomaterials 32:8097–8107
Kershen RT, Fefer SD, Atala A (2000) Tissue-engineered therapies for the treatment of urinary incontinence and vesicoureteral reflux. World J Urol 18:51–55
Khang G (2017) Biomaterials and manufacturing methods for scaffolds in regenerative medicine: update 2015. In: Khang G (ed) Handbook of intelligent scaffolds for tissue engineering and regenerative medicine. Taylor & Francis Group, Singapore, pp 1–53
Kim UJ, Park J, Li C, ** HJ, Valluzzi R, Kaplan DL (2004) Structure and properties of silk hydrogels. Biomacromolecules 5:786–792
Kim H-W, Kim H-E, Salih V (2005) Stimulation of osteoblast responses to biomimetic nanocomposites of gelatin-hydroxyapatite for tissue engineering scaffolds. Biomaterials 26:5221–5230
Kim T-R, Kim M-S, Goh TS, Lee JS, Kim YH, Yoon S-Y, Lee C-S (2019) Evaluation of structural and mechanical properties of porous artificial bone scaffolds fabricated via advanced TBA-based freeze-gel casting technique. Appl Sci 9(9):1965. https://doi.org/10.3390/app9091965
Klawitter J, Hulbert S (1971) Application of porous ceramics for the attachment of load bearing internal orthopedic applications. J Biomed Mater Res 5:161–229
Knoepfler PS (2015) From bench to FDA to bedside: us regulatory trends for new stem cell therapies. Adv Drug Del Rev 82-83:192–196
Kong HJ, Smith MK, Mooney DJ (2003) Designing alginate hydrogels to maintain viability of immobilized cells. Biomaterials 24:4023–4029
Kotton DN, Morrisey EE (2014) Lung regeneration: mechanisms, applications and emerging stem cell populations. Nat Med 20:822–832
Kozlov PV, Burdygina GI (1983) The structure and properties of solid gelatin and the principles of their modification. Polymer 24:651–666
Kubinova S, Horak D, Hejcl A, Plichta Z, Kotek J, Proks V, Forostyak S, Sykova E (2015) SIKVAV-modified highly superporous PHEMA scaffolds with oriented pores for spinal cord injury repair. J Tissue Eng Regen Med 9:1298–1309
Kuo W-T, Huang H-Y, Chou M-J, Wu M-C, Huang Y-Y (2011) Surface modification of gelatin nanoparticles with polyethyleneimine as gene vector. J Nanomater 2011:1–5
Langer R, Vacanti J (1993) Tissue engineering. Science 260:920–926
Laurencin CT, Khan Y (2012) Regenerative engineering. Sci Transl Med 4:160ed9
Lee KY, Mooney DJ (2001) Hydrogels for tissue engineering. Chem Rev 101:1869–1879
Lee KY, Mooney DJ (2012) Alginate: properties and biomedical applications. Prog Polym Sci 37:106–126
Lee KY, Peters MC, Anderson KW, Mooney DJ (2000) Controlled growth factor release from synthetic extracellular matrices. Nature 408:998–1000
Levenberg S, Rouwkema J, Macdonald M, Garfein ES, Kohane DS, Darland DC, Marini R, van Blitterswijk CA, Mulligan RC, D’Amore PA, Langer R (2005) Engineering vascularized skeletal muscle tissue. Nat Biotechnol 23:879–884
Lien SM, Ko LY, Huang TJ (2009) Effect of pore size on ECM secretion and cell growth in gelatin scaffold for articular cartilage tissue engineering. Acta Biomater 5:670–679
Lieschke GJ, Currie PD (2007) Animal models of human disease: zebrafish swim into view. Nat Rev Genet 8:353–367
Lim K, Morouço P, Levato R, Melchels F, Malda J (2017) Organ biofabrication. Comprehen Biomater II 5:236–266
Lim Y-S, Ok Y-J, Hwang S-Y, Kwak J-Y, Yoon S (2019) Marine collagen as a promising biomaterial for biomedical applications. Mar Drugs 17:467
Lin LJ, Chiang CJ, Chao YP, Wang SD, Chiou YT, Wang HY et al (2016) Development of alginate microspheres containing chuanxiong for oral administration to adult zebrafish. BioMed Res Int. https://doi.org/10.1155/2016/4013071
López-Ruiz E, Jiménez G, García MÁ, Antich C, Boulaiz H, Marchal JA, Peran M (2016) Polymers, scaffolds and bioactive molecules with therapeutic properties in osteochondral pathologies: what’s new? Expert Opin Ther Pat 26:877–890
Ma PX (2004) Scaffolds for tissue fabrication. Mater Today 7:30–40
MacRae CA, Peterson RT (2015) Zebrafish as tools for drug discovery. Nat Rev Drug Discov 14:721–731
Mason C, Dunnill P (2008) A brief definition of regenerative medicine. Regen Med 3:1–5
Mayer JE, Shin’oka T, Shum-Tim D (1997) Tissue engineering of cardiovascular structures. Curr Opin Cardiol 12:528–532
Mayer J, Karamuk E, Akaike T, Wintermantel E (2000) Matrices for tissue engineering-scaffold structure for a bioartificial liver support system. J Control Release 64:81–90
Mendelson A, Frenette PS (2014) Hematopoietic stem cell niche maintenance during homeostasis and regeneration. Nat Med 20:833–846
Mohammad J, Shenaq J, Rabinovsky E, Shenaq S (2000) Modulation of peripheral nerve regeneration: a tissue engineering approach. The role of amnion tube nerve conduit across a 1-centimeter nerve gap. Plast Reconstr Surg 105:660–666
Mohammadzadehmoghadam S, Dong Y (2019) Fabrication and characterization of electrospun silk fibroin/gelatin scaffolds crosslinked with glutaraldehyde vapor. Front Mater 6:91. https://doi.org/10.3389/fmats.2019.00091
Nagarajan S, Pochat-Bohatier C, Teyssier C, Balme S, Miele P, Kalkura N, Cavaillès V, Bechelany M (2016a) Design of graphene oxide/gelatin electrospun nanocomposite fibers for tissue engineering applications. RSC Adv 6:109150–109156
Nagarajan S, Soussan L, Bechelany M, Teyssier C, Cavaillès V, Pochat-Bohatier C, Miele P, Kalkura N, Janot JM, Balme S (2016b) Novel biocompatible electrospun gelatin fiber mats with antibiotic drug delivery properties. J Mater Chem B 4:1134–1141
Nagarajan S, Belaid H, Pochat-Bohatier C, Teyssier C, Iatsunskyi I, Coy E, Balme S, Cornu D, Miele P, Kalkura NS, Cavailles V, Bechelany M (2017) Design of boron nitride/gelatin electrospun nanofibers for bone tissue engineering. ACS Appl Mater Interfaces 9:33695–33706
Nair LS, Laurencin CT (2007) Biodegradable polymers as biomaterials. Prog Polym Sci 32:762–798
Nair P, Thottappillil N (2015) Scaffolds in vascular regeneration: current status. Vasc Health Risk Manag 11:79–91
Oberpenning F, Meng J, Yoo JJ, Atala A (1999) De novo reconstitution of a functional mammalian urinary bladder by tissue engineering. Nat Biotechnol 17:149–155
OECD, OECD Guidelines for the Testing of Chemicals (2013) Test No 236
Onal U, Langdon C (2000) Characterization of two microparticle types for delivery of food to altricial fish larvae. Aquac Nutr 6:159–170
Panzavolta S, Gioffrè M, Focarete ML, Gualandi C, Foroni L, Bigi A (2011) Electrospun gelatin nanofibers: optimization of genipin cross-linking to preserve fiber morphology after exposure to water. Acta Biomater 7:1702–1709
Parker GJM, Wheeler-Kingshott CAM, Barker GJ (2002) Diffusion tensor imaging. IEEE T Med Imaging 21:505–512
Paszek MJ, Zahir N, Johnson KR, Lakins JN, Rozenberg GI, Gefen A, Reinhart-King CA, Margulies SS, Dembo M, Boettiger D, Hammer DA, WeaverVM (2005) Tensional homeostasis and the malignant phenotype. Cancer Cell 8:241–254
Peppas NA, Khare AR (1993) Preparation, structure and diffusional behavior of hydrogels in controlled release. Adv Drug Deliv Rev 11:1–35
Phelps EA, Enemchukwu NO, Fiore VF, Sy JC, Murty N, Sulchek TA, Barker TH, Garcia AJ (2012) Maleimide cross-linked bioactive peg hydrogel exhibits improved reaction kinetics and cross-linking for cell encapsulation and in situ delivery. Adv Mater 24:64–70
Pina S, Canadas RF, Jimenez G, Peran M, Marchal JA, Reis RL, Oliveira JM (2017) Biofunctional ionic-doped calcium phosphates: silk fibroin composites for bone tissue engineering scaffolding. Cells Tissues Organs 204:150–163
Piskin E (1994) Biodegradable polymers as biomaterials. J Biomat Sci Polym E 6:775–795
Poursamar SA, Lehner AN, Azami M, Ebrahimi-Barough S, Samadikuchaksaraei A, Antunes APM (2016) The effects of crosslinkers on physical, mechanical, and cytotoxic properties of gelatin sponge prepared via in-situ gas foaming method as a tissue engineering scaffold. Mater Sci Eng C 63:1–9
Prang P, Muller R, Eljaouhari A, Heckmann K, Kunz W, Weber T, Faber C, Vroemen M, Bogdahn U, Weidner N (2006) The promotion of oriented axonal regrowth in the injured spinal cord by alginate-based anisotropic capillary hydrogels. Biomaterials 27:3560–3569
Prasitsilp M, Siriwittayakorn T, Molloy R, Suebsanit N, Siriwittayakorn P, Veeranondha S (2003) Cytotoxicity study of homopolymers and copolymers of 2-hydroxyethyl methacrylate and some alkyl acrylates for potential use as temporary skin substitutes. J Mater Sci Mater Med 14:595–600
Ramakrishna S, Mayer J, Wintermantel E, Leong KW (2001) Biomedical applications of polymer-composite materials: a review. Compos Sci Technol 61:1189–1224
Rezwan K, Chen QZ, Blaker JJ, Boccaccini AR (2006) Biodegradable and bioactive porous polymer/inorganic composite scaffolds for bone tissue engineering. Biomaterials 27:3413–3431
Roether JA, Boccaccini AR, Hench LL, Maquet V, Gautier S, Jerome R (2002) Development and in vitro characterization of novel bioresorbable and bioactive composite materials based on polylactide foams and bioglass® for tissue engineering applications. Biomaterials 23:3871–3878
Roseti L, Parisi V, Petretta M, Cavallo C, Desando G, Bartolotti I, Grigolo B (2017) Scaffolds for bone tissue engineering: state of the art and new perspectives. Mat Sci Eng C Bio S 78:1246–1262
Sadeghi M, Heidari B (2011) Crosslinked graft copolymer of methacrylic acid and gelatin as a novel hydrogel with pHresponsiveness properties. Materials 4:543–552
Sadtler K, Singh A, Wolf MT, Wang T, Pardoll DM, Elisseeff JH (2016) Design, clinical translation and immunological response of biomaterials in regenerative medicine. Nat Rev Mater 1:16040
Sajkiewicz P, Kołbuk D (2014) Electrospinning of gelatin for tissue engineering-molecular conformation as one of the overlooked problems. J Biomater Sci Polym Ed 25:2009–2022
Saxena AK, Marler J, Benvenuto M, Willital GH, Vacanti JP (1999) Skeletal muscle tissue engineering using isolated myoblasts on synthetic biodegradable polymers: preliminary studies. Tissue Eng 5:525–532
Schmedlen RH, Masters KS, West JL (2002) Photocrosslinkable polyvinyl alcohol hydrogels that can be modified with cell adhesion peptides for use in tissue engineering. Biomaterials 23:4325–4332
Sculean A, Auschill TM, Donos N, Brecx M, Arweiler NB (2001) Effect of an enamel matrix protein (Emdogain®) on ex vivo dental plaque vitality. J Clin Periodontol 28:1074–1078
Seol YJ, Park DY, Park JY, Kim SW, Park SJ, Cho DW (2013) A new method of fabricating robust freeform 3D ceramic scaffolds for bone tissue regeneration. Biotechnol Bioeng 110:1444–1455
Sharma C, Dinda AK, Potdar PD, Chou CF, Mishra NC (2016) Fabrication and characterization of novel nano-biocomposite scaffold of chitosan-gelatin-alginate-hydroxyapatite for bone tissue engineering. Mater Sci Eng 64:416–427
Slaughter BV, Khurshid SS, Fisher OZ, Khademhosseini A, Peppas NA (2009) Hydrogels in regenerative medicine. Adv Mater 21:3307–3329
Smeds KA, Grinstaff MW (2001) Photocrosslinkable polysaccharides for in situ hydrogel formation. J Biomed Mater Res 54:115–121
Solchaga LA, Gao J, Dennis JE et al (2002) Treatment of osteochondral defects with autologous bone marrow in a hyaluronan-based delivery vehicle. Tissue Eng 8:333–347
Soon-Shiong P, Heintz RE (1994) Insulin independence in a type 1 diabetic patient after encapsulated islet transplantation. Lancet 343:950–951
Suh JKF, Matthew HWT (2000) Application of chitosan-based polysaccharide biomaterials in cartilage tissue engineering: a review. Biomaterials 21:2589–2598
Sun W, Darling A, Starly B, Nam J (2004) Computer-aided tissue engineering: overview, scope and challenges. Appl Biochem Biotechnol 39:29–47
Sung H-J, Meredith C, Johnso C, Galis ZS (2004) The effect of scaffold degradation rate on three-dimensional cell growth and angiogenesis. Biomaterials 25:5735–5742
Suzuki K, Suzuki Y, Tanihara M, Ohnishi K, Hashimoto T, Endo K, Nishimura Y (2000) Reconstruction of rat peripheral nerve gap without sutures using freeze-dried alginate gel. J Biomed Mater Res 49:528–533
Tabata Y (2003) Tissue regeneration based on growth factor release. Tissue Eng 9:5–15
Taddei P, Chiono V, Anghileri A, Vozzi G, Freddi G, Ciardelli G (2013) Silk fibroin/gelatin blend films crosslinked with enzymes for biomedical applications. Macromol Biosci 13:1492–1510
Tang XL, Li Q, Rokosh G, Sanganalmath SH, Chen N, Ou Q, Stowers H, Hunt G, Bolli R (2016) Long-term outcome of administration of c-kitPOS cardiac progenitor cells after acute myocardial infarction: transplanted cells do not become cardiomyocytes, but structural and functional improvement and proliferation of endogenous cells persist for at least one year. Circ Res 118:1091–1105
Thomas LV, Nair PD (2012) Influence of mechanical stimulation in the development of a medial equivalent tissue-engineered vascular construct using a gelatin-g-vinyl acetate co-polymer scaffold. J Biomater Sci Polym Ed 23:2069–2087
Tomić SLj, Vuković JS (2020) Antimicrobial properties of (meth)acrylate-based hydrogels. In: Paquette N (ed) An introduction to antibacterial properties. Nova Science Publishers, New York. https://novapublishers.com/shop/an-introduction-to-antibacterialproperties/
Tomić SLj, Babić MM, Djokić L, Pavić A, Nikodinović-Runić J (2020) Effect of composition and method of preparation of 2-hydroxyethyl methacrylate/gelatin hydrogels on biological in vitro (cell line) and in vivo (zebrafish) properties. J Polym Res 27(10):1–8. https://doi.org/10.1007/s10965-020-02219-w
Tran TT, Hamid ZA, Cheong KY (2018) A review of mechanical properties of scaffold in tissue engineering: Aloe vera composites. J Phys Conf Ser 1082:012080
Tzankova V, Aluani D, Kondeva-Burdina M, Yordanov Y, Odzhakov F, Apostolov A, Yoncheva K (2017) Hepatoprotective and antioxidant activity of quercetin- loaded chitosan/alginate particles in vitro and in vivo in a model of paracetamol-induced toxicity. Biomed Pharmacother 92:569–579
Tziampazis E, Sambanis A (1995) Tissue engineering of a bioartificial pancreas: modeling the cell environment and device function. Biotechnol Prog 11:115–126
Vacanti JP, Langer R (1999) Tissue engineering: the design and fabrication of living replacement devices for surgical reconstruction and transplantation. Lancet 354:S32–S34
Wade RJ, Bassin EJ, Gramlich WM, Burdick JA (2015) Nanofibrous hydrogels with spatially patterned biochemical signals to control cell behavior. Adv Mater 27:1356–1362
Wallace DG, Rosenblatt J (2003) Collagen gel systems for sustained delivery and tissue engineering. Adv Drug Deliv Rev 55:1631–1649
Wang K, Nune KC, Misra RDK (2016) The functional response of alginate-gelatin- nanocrystalline cellulose injectable hydrogels toward delivery of cells and bioactive molecules. Acta Biomater 36:143–151
Wongputtaraksa T, Ratanavaraporn J, Pichyangkura R, Damrongsakkul S (2012) Surface modification of Thai silk fibroin scaffolds with gelatin and chitooligosaccharide for enhanced osteogenic differentiation of bone marrow-derived mesenchymal stem cells. J Biomed Mater Res Part B Appl Biomater 100:2307–2315
Yang C, DelRio FW, Ma H, Killaars AR, Basta LP, Kyburz KA, Anseth KS (2016) Spatially patterned matrix elasticity directs stem cell fate. Proc Natl Acad Sci U S A 113:E4439–E4445
Yannas IV (2004) Classes of materials used in medicine: natural materials. In: Ratner BD, Hoffman AS, Schoen FJ, Lemons J (eds) Biomaterials science-an introduction to materialsin medicine. Elsevier Academic Press, San Diego, CA, pp 127–136
Yannas I, Lee E, Orgill D, Skrabut E, Murphy G (1989) Synthesis and characterization of a model extracellular matrix that induces partial regeneration of adult mammalian skin. Proc Natl Acad Sci U S A 86:933–937
Zadpoor AA (2015) Bone tissue regeneration: the role of scaffold geometry. Biomater Sci UK 3:231–245
Żak M, Kuropka P, Kobielarz M, Dudek A, Kaleta-Kuratewicz K, Szotek S (2011) Determination of the mechanical properties of the skin of pig foetuses with respect to its structure. Acta Bioeng Biomech 13:37–43
Zhang YZ, Venugopal J, Huang ZM, Lim CT, Ramakrishna S (2006) Crosslinking of the electrospun gelatin nanofibers. Polymer 47:2911–2917
Zhang H, Zhou L, Zhang W (2014) Control of scaffold degradation in tissue engineering: a review. Tissue Eng Part B Rev 20(5):492–502. https://doi.org/10.1089/ten.TEB.2013.0452
Zhao XH, Kim J, Cezar CA, Huebsch N, Lee K, Bouhadir K, Mooney DJ (2011) Active scaffolds for on-demand drug and cell delivery. Proc Natl Acad Sci U S A 108:67–72
Acknowledgments
This research is supported by the SCOPES program of the Swiss National Science Foundation and the Swiss Agency for Development and Cooperation [Grant No IZ73ZO_152327]. This work is supported by the Ministry for Education, Science, and Technological Development of the Republic of Serbia (Contracts Nos. 451-03-9/2021-14/172062 and 451-03-9/2021-14/172026).
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2022 The Author(s), under exclusive license to Springer Nature Singapore Pte Ltd.
About this chapter
Cite this chapter
Tomić, S.L., Vukomanović, M., Nikodinović-Runić, J., Babić, M.M., Vuković, J.S. (2022). Hydrogel Scaffolds Based on Alginate, Gelatin, and 2-Hydroxyethyl Methacrylate for Tissue Regeneration. In: Jana, S., Jana, S. (eds) Marine Biomaterials. Springer, Singapore. https://doi.org/10.1007/978-981-16-5374-2_6
Download citation
DOI: https://doi.org/10.1007/978-981-16-5374-2_6
Published:
Publisher Name: Springer, Singapore
Print ISBN: 978-981-16-5373-5
Online ISBN: 978-981-16-5374-2
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)