Abstract
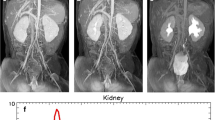
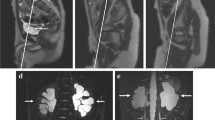
Gadolinium-based functional MR urography (fMRU) offers high spatial, contrast, and temporal resolution, using renal parenchymal signal changes in dynamic T1-weighted images related to uptake and excretion of intravenous administration of a gadolinium-based contrast agent to estimate renal function and contrast clearance times. This technique has been proved to give equivalent information to nuclear medicine renal scans and intravenous urograms without the use of ionizing radiation and with increased anatomic detail. fMRU is increasingly being used to evaluate the urinary tract with both anatomic and functional information. Common applications are related to suspected urinary tract obstruction and estimation of underlying renal function in children but can also help estimating residual renal function during surgical planning.
Familiarity with underlying assumptions and postprocessing steps is needed to generate and interpret functional MRU parameters. In this chapter, we describe fMRU patient preparation, imaging acquisition, and postprocessing including how common quantitative parameters are produced to assist further dissemination and adoption of this technology.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
Abbreviations
- CTT:
-
Calyceal transit time
- DRF:
-
Differential renal function
- eGFR:
-
Estimated glomerular filtration rate
- fMRU:
-
Functional magnetic resonance urography
- MTT:
-
Mean transit time
- RTT:
-
Renal transit time
References
Grattan-Smith JD, Chow J, Kurugol S, Jones RA. Quantitative renal magnetic resonance imaging: magnetic resonance urography. Pediatr Radiol. 2022;52(2):228–48.
Claudon M, Durand E, Grenier N, Prigent A, Balvay D, Chaumet-Riffaud P, et al. Chronic urinary obstruction: evaluation of dynamic contrastenhanced MR urography for measurement of split renal function. Radiology. 2014;273(3):801–12.
Damasio MB, Bodria M, Dolores M, Durand E, Sertorio F, Wong MCY, et al. Comparative study between functional MR urography and renal scintigraphy to evaluate drainage curves and Split renal function in children with congenital anomalies of kidney and urinary tract (CAKUT). Front Pediatr. 2020;7:7(January).
Karaveli M, Katsanidis D, Psarrakos K, Sioundas A, Dimitriadis A, Haritanti A, et al. MR urography: anatomical and quantitative information on congenital malformations in children. Niger Med J. 2013;54(2):136.
Khrichenko D, Darge K. Functional analysis in MR urography - made simple. Pediatr Radiol. 2010;40(2):182–99.
Bo S, Sedaghat F, Devi Pavuluri K, Rowe SP, Cohen A, Kates M, et al. Dynamic contrast enhanced-mr cest urography: an emerging tool in the diagnosis and management of upper urinary tract obstruction. Tomography. 2021;7(1):80–94.
Abreu-Gomez J, Udare A, Shanbhogue KP, Schieda N. Update on MR urography (MRU): technique and clinical applications. Abdom Radiol. 2019;44(12):3800–10.
Dickerson EC, Dillman JR, Smith EA, Dipietro MA, Lebowitz RL, Darge K. Pediatric MR urography: indications, techniques, and approach to review. Radiographics. 2015;35(4):1208–30.
Riccabona M. Pediatric urogenital radiology. Third edit. Springer International Publishing; 2018. p. 34.
Jones RA, Easley K, Little SB, Scherz H, Kirsch AJ, Grattan-Smith JD. Dynamic contrast-enhanced MR urography in the evaluation of pediatric hydronephrosis: part I, functional assessment. Am J Roentgenol. 2005;185(6):1598–607.
Lee MJ, Kim MJ, Yoon CS, Song SY, Park K, Kim WS. The T2-shortening effect of gadolinium and the optimal conditions for maximizing the CNR for evaluating the biliary system: a phantom study. Korean J Radiol. 2011;12(3):358;/pmc/articles/PMC3088853/.
Elster AD, Sobol WT, Hinson WH. Pseudolayering of Gd-DTPA in the urinary bladder. Radiology. 1990;174(2):379–81; https://pubmed.ncbi.nlm.nih.gov/2296649/.
May DA, Pennington DJ. Effect of gadolinium concentration on renal signal intensity: an in vitro study with a saline bag model. Radiology. 2000;216(1):232–6;https://pubmed.ncbi.nlm.nih.gov/10887253/.
Delgado J, Bedoya MA, Adeb M, Carson RH, Johnson AM, Khrichenko D, et al. Optimizing functional MR urography: prime time for a 30-minutes-or-less fMRU. Pediatr Radiol. 2015;45(9):1333–43.
Altun E, Martin DR, Wertman R, Lugo-Somolinos A, Fuller ER, Semelka RC. Nephrogenic systemic fibrosis: change in incidence following a switch in gadolinium agents and adoption of a gadolinium policy - report from two U.S. universities. Radiology. 2009;253(3):689–96.
ACR manual on contrast media 2022: ACR Committee on drugs and contrast media. 2022.
Runge VM, Richter JK, Heverhagen JT. Motion in magnetic resonance: new paradigms for improved clinical diagnosis. Invest Radiol. 2019;54(7):383–95;https://pubmed.ncbi.nlm.nih.gov/30946182/.
Feng L. Golden-angle Radial MRI: basics, advances, and applications. J Magn Reson Imaging. 2022;56(1):45–62;https://pubmed.ncbi.nlm.nih.gov/35396897/.
Jones RA, Grattan-Smith JD, Little S. MR urography in children. Milan: Springer; 2014. p. 295–310.
Jones RA, Schmotzer B, Little SB, Grattan-Smith JD. MRU post-processing. Pediatr Radiol. 2008;38(1 SUPPL):18–27.
Little SB, Jones RA, Grattan-Smith JD. Evaluation of UPJ obstruction before and after pyeloplasty using MR urography. Pediatr Radiol. 2008;38(1 SUPPL):106–24.
Jones RA, Perez-Brayfield MR, Kirsch AJ, Grattan-Smith JD. Renal transit time with MR urography in children. Radiology. 2004;233(1):41–50.
Viteri B, Calle-Toro JS, Ballester L, Darge K, Furth S, Khrichenko D, et al. Potential benefits of functional magnetic resonance urography (fMRU) over MAG3 renal scan in children with obstructive uropathy. J Pediatr Urol. 2021;17(5):659.e1–7.
Patlak CS, Blasberg RG. Graphical evaluation of blood-to-brain transfer constants from multiple-time uptake data. J Cereb Blood Flow Metab. 1985;5(4):584–90.
Hackstein N, Heckrodt J, Rau WS. Measurement of single-kidney glomerular filtration rate using a contrast-enhanced dynamic gradient-Echo sequence and the Rutland-Patlak plot technique. J Magn Reson Imaging. 2003;18(6):714–25.
Hackstein N, Kooijman H, Tomaselli S, Rau WS. Glomerular filtration rate measured using the Patlak plot technique and contrast-enhanced dynamic MRI with different amounts of gadolinium-DTPA. J Magn Reson Imaging. 2005;22(3):406–14; https://pubmed.ncbi.nlm.nih.gov/16106358/.
Mendichovszky I, Pedersen M, Frøkiær J, Dissing T, Grenier N, Anderson P, et al. How accurate is dynamic contrast-enhanced MRI in the assessment of renal glomerular filtration rate? A critical appraisal. J Magn Reson Imaging. 2008;27(4):925–31.
McMann LP, Kirsch AJ, Scherz HC, Smith EA, Jones RA, Shehata BM, et al. Magnetic resonance urography in the evaluation of prenatally diagnosed Hydronephrosis and renal dysgenesis. J Urol. 2006;176(4 SUPPL):1786–92.
Grattan-Smith JD, Jones RA. Magnetic resonance urography in children. Magn Reson Imaging Clin N Am. 2008;16(3):515–31.
Park JM, Bloom DA. The pathophysiology of UPJ obstruction: current concepts. Urol Clin North Am. 1998;25(2):161–9.
Farrugia MK, Whitaker RH. The search for the definition, etiology, and effective diagnosis of upper urinary tract obstruction: the Whitaker test then and now. J Pediatr Urol. 2019;15(1):18–26.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2023 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Rincon-Escobar, E.A., Khrichenko, D., Otero, H.J. (2023). Gadolinium-Based Functional MR Urography: From Image Acquisition to Interpretation. In: Serai, S.D., Darge, K. (eds) Advanced Clinical MRI of the Kidney. Springer, Cham. https://doi.org/10.1007/978-3-031-40169-5_20
Download citation
DOI: https://doi.org/10.1007/978-3-031-40169-5_20
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-40168-8
Online ISBN: 978-3-031-40169-5
eBook Packages: MedicineMedicine (R0)