Abstract
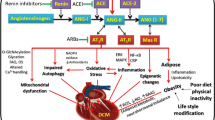
Type 2 diabetes mellitus is associated with a high risk of heart failure, in part because of its potential to induce impaired cardiac function even in the absence of coronary artery disease and hypertension. The pathogenesis of diabetic cardiomyopathy is not yet fully understood, although it is known that alterations in the cardiac substrate metabolism and energy play a significant role in the development and progression of this condition. Among these abnormalities, increased fatty acid storage and utilization, associated with reduced glucose oxidation and altered mitochondrial oxidative phosphorylation stand out. One of the key connections linking diabetes and the remarkably prevalence of cardiomyopathy is the renin angiotensin system (RAS) hyperactivation. RAS has been described for its crucial involvement in the generation and progression of diabetic cardiovascular complications, as its exacerbated activation supports mechanisms that lead to cardiomyocyte death and myocardial fibrosis. The importance of RAS blockage in the prevention of diabetic cardiomyopathy exhibits the fundamental role that RAS plays in the onset and development of this pathology. Angiotensin-converting enzyme inhibitors and blockers of angiotensin II actions denote the first-line therapy for primary and secondary prevention of cardiovascular disease in type 2 diabetic. Recent studies have revealed new features of RAS and, consequently, new therapeutic potential against diabetic cardiomyopathy. In this chapter, a description of the main mechanisms involved in the correlation between excessive activation of the RAS and type 2 diabetes is presented, with attention on mechanisms associated to pathogenesis and progression of diabetic cardiomyopathy.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Borghetti G, von Lewinski D, Eaton DM, Sourij H, Houser SR, Wallner M (2018) Diabetic cardiomyopathy: current and future therapies. Beyond Glycemic Control. Front Physiol 9:1514. https://doi.org/10.3389/fphys.2018.01514
Jia G, Hill MA, Sowers JR (2018) Diabetic cardiomyopathy: an update of mechanisms contributing to this clinical entity. Circ Res 122(4):624–638. https://doi.org/10.1161/CIRCRESAHA.117.311586
Goossens GH, Blaak EE, van Baak MA (2003) Possible involvement of the adipose tissue renin-angiotensin system in the pathophysiology of obesity and obesity-related disorders. Obes Rev 4(1):43–55. https://doi.org/10.1046/j.1467-789x.2003.00091.x
Engeli S, Negrel R, Sharma AM (2000) Physiology and pathophysiology of the adipose tissue renin-angiotensin system. Hypertension 35(6):1270–1277. https://doi.org/10.1161/01.hyp.35.6.1270
Ferrario CM, Strawn WB (2006) Role of the renin-angiotensin-aldosterone system and proinflammatory mediators in cardiovascular disease. Am J Cardiol 98(1):121–128. https://doi.org/10.1016/j.amjcard.2006.01.059
Kim S, Iwao H (2000) Molecular and cellular mechanisms of angiotensin II-mediated cardiovascular and renal diseases. Pharmacol Rev 52(1):11–34
Unger T (2002) The role of the renin-angiotensin system in the development of cardiovascular disease. Am J Cardiol 89(2):3–9. https://doi.org/10.1016/s0002-9149(01)02321-9
Henriksen EJ (2007) Improvement of insulin sensitivity by antagonism of the renin-angiotensin system. Am J Physiol Regul Integr Comp Physiol 293(3):R974-980. https://doi.org/10.1152/ajpregu.00147.2007
Leung PS (2007) Mechanisms of protective effects induced by blockade of the renin-angiotensin system: novel role of the pancreatic islet angiotensin-generating system in type 2 diabetes. Diabet Med 24(2):110–116. https://doi.org/10.1111/j.1464-5491.2007.02072.x
Tigerstedt R, Bergman PQ (1898) Niere und Kreislauf1. Skandinavisches Archiv Für Physiologie 8(1):223–271. https://doi.org/10.1111/j.1748-1716.1898.tb00272.x
Grobe JL, Xu D, Sigmund CD (2008) An intracellular renin-angiotensin system in neurons: fact, hypothesis, or fantasy. Physiology (Bethesda) 23:187–193. https://doi.org/10.1152/physiol.00002.2008
Bodiga VL, Bodiga S (2013) Renin angiotensin system in cognitive function and dementia. Asian J Neurosci 2013:1–18. https://doi.org/10.1155/2013/102602
Suzuki Y, Ruiz-Ortega M, Lorenzo O, Ruperez M, Esteban V, Egido J (2003) Inflammation and angiotensin II. Int J Biochem Cell Biol 35(6):881–900. https://doi.org/10.1016/s1357-2725(02)00271-6
Paul M, Poyan Mehr A, Kreutz R (2006) Physiology of local renin-angiotensin systems. Physiol Rev 86(3):747–803. https://doi.org/10.1152/physrev.00036.2005
Fouda AY, Artham S, El-Remessy AB, Fagan SC (2016) Renin-angiotensin system as a potential therapeutic target in stroke and retinopathy: experimental and clinical evidence. Clin Sci (Lond) 130(4):221–238. https://doi.org/10.1042/CS20150350
Wright JW, Harding JW (2011) Brain renin-angiotensin–a new look at an old system. Prog Neurobiol 95(1):49–67. https://doi.org/10.1016/j.pneurobio.2011.07.001
Santos RA, Simoes e Silva AC, Maric C, et al (2003) Angiotensin-(1-7) is an endogenous ligand for the G protein-coupled receptor Mas. Proc Natl Acad Sci USA 100(14):8258−8263. https://doi.org/10.1073/pnas.1432869100
Jiang T, Gao L, Lu J, Zhang YD (2013) ACE2-Ang-(1–7)-Mas axis in brain: a potential target for prevention and treatment of ischemic stroke. Curr Neuropharmacol 11(2):209–217. https://doi.org/10.2174/1570159X11311020007
Tetzner A, Gebolys K, Meinert C et al (2016) G-Protein-coupled receptor MrgD Is a receptor for angiotensin-(1–7) involving adenylyl cyclase, cAMP, and phosphokinase A. Hypertension 68(1):185–194. https://doi.org/10.1161/HYPERTENSIONAHA.116.07572
Lautner RQ, Villela DC, Fraga-Silva RA et al (2013) Discovery and characterization of alamandine: a novel component of the renin-angiotensin system. Circ Res 112(8):1104–1111. https://doi.org/10.1161/CIRCRESAHA.113.301077
**a H, Lazartigues E (2008) Angiotensin-converting enzyme 2 in the brain: properties and future directions. J Neurochem 107(6):1482–1494. https://doi.org/10.1111/j.1471-4159.2008.05723.x
Ahmed HA, Ishrat T, Pillai B et al (2018) Role of angiotensin system modulation on progression of cognitive impairment and brain MRI changes in aged hypertensive animals—a randomized double-blind pre-clinical study. Behav Brain Res 346:29–40. https://doi.org/10.1016/j.bbr.2017.12.007
Labandeira-Garcia JL, Rodriguez-Perez AI, Garrido-Gil P, Rodriguez-Pallares J, Lanciego JL, Guerra MJ (2017) Brain renin-angiotensin system and microglial polarization: implications for aging and neurodegeneration. Front Aging Neurosci 9:129. https://doi.org/10.3389/fnagi.2017.00129
Costa-Besada MA, Valenzuela R, Garrido-Gil P et al (2018) Paracrine and intracrine angiotensin 1–7/mas receptor axis in the substantia nigra of rodents, monkeys, and humans. Mol Neurobiol 55(7):5847–5867. https://doi.org/10.1007/s12035-017-0805-y
Leonhardt J, Villela DC, Teichmann A et al (2017) Evidence for heterodimerization and functional interaction of the angiotensin type 2 receptor and the receptor MAS. Hypertension 69(6):1128–1135. https://doi.org/10.1161/HYPERTENSIONAHA.116.08814
Santos RAS, Campagnole-Santos MJ, SlP A (2000) Angiotensin-(1–7): an update. Regul Pept 91(1–3):45–62. https://doi.org/10.1016/s0167-0115(00)00138-5
Passos-Silva DG, Brandan E, Santos RA (2015) Angiotensins as therapeutic targets beyond heart disease. Trends Pharmacol Sci 36(5):310–320. https://doi.org/10.1016/j.tips.2015.03.001
Passos-Silva DG, Verano-Braga T, Santos RA (2013) Angiotensin-(1–7): beyond the cardio-renal actions. Clin Sci (Lond) 124(7):443–456. https://doi.org/10.1042/CS20120461
Gironacci MM, Cerniello FM, Longo Carbajosa NA, Goldstein J, Cerrato BD (2014) Protective axis of the renin-angiotensin system in the brain. Clin Sci (Lond) 127(5):295–306. https://doi.org/10.1042/CS20130450
Timmermans PB, Wong PC, Chiu AT et al (1993) Angiotensin II receptors and angiotensin II receptor antagonists. Pharmacol Rev 45(2):205–251
Peach MJ (1977) Renin-angiotensin system: biochemistry and mechanisms of action. Physiol Rev 57(2):313–370. https://doi.org/10.1152/physrev.1977.57.2.313
Ribeiro-Oliveira AJ, Nogueira AI, Pereira RM, Boas WW, Santos RA, Simões e Silva AC (2008) The renin–angiotensin system and diabetes: an update. Vascular Health and Risk Managem 4(4):787–803
Kahn CR (2008) Medicine. Can we nip obesity in its vascular bud? Science 322(5901):542–543. https://doi.org/10.1126/science.1165667
Kahn SE (2003) The relative contributions of insulin resistance and beta-cell dysfunction to the pathophysiology of type 2 diabetes. Diabetologia 46(1):3–19. https://doi.org/10.1007/s00125-002-1009-0
Tikellis C, Cooper ME, Thomas MC (2006) Role of the renin-angiotensin system in the endocrine pancreas: implications for the development of diabetes. Int J Biochem Cell Biol 38(5–6):737–751. https://doi.org/10.1016/j.biocel.2005.08.007
Kampf C, Lau T, Olsson R, Leung PS, Carlsson PO (2005) Angiotensin II type 1 receptor inhibition markedly improves the blood perfusion, oxygen tension and first phase of glucose-stimulated insulin secretion in revascularised syngeneic mouse islet grafts. Diabetologia 48(6):1159–1167. https://doi.org/10.1007/s00125-005-1761-z
Huang Z, Jansson L, Sjoholm A (2006) Pancreatic islet blood flow is selectively enhanced by captopril, irbesartan and pravastatin, and suppressed by palmitate. Biochem Biophys Res Commun 346(1):26–32. https://doi.org/10.1016/j.bbrc.2006.05.144
Chu KY, Lau T, Carlsson PO, Leung PS (2006) Angiotensin II type 1 receptor blockade improves beta-cell function and glucose tolerance in a mouse model of type 2 diabetes. Diabetes 55(2):367–374. https://doi.org/10.2337/diabetes.55.02.06.db05-1022
Shao J, Iwashita N, Ikeda F et al (2006) Beneficial effects of candesartan, an angiotensin II type 1 receptor blocker, on beta-cell function and morphology in db/db mice. Biochem Biophys Res Commun 344(4):1224–1233. https://doi.org/10.1016/j.bbrc.2006.04.011
Yuan L, Li X, Li J, Li HL, Cheng SS (2013) Effects of renin-angiotensin system blockade on the islet morphology and function in rats with long-term high-fat diet. Acta Diabetol 50(4):479–488. https://doi.org/10.1007/s00592-010-0210-8
Ashrafian H, Neubauer S (2009) Metabolomic profiling of cardiac substrate utilization: fanning the flames of systems biology? Circulation 119(13):1700–1702. https://doi.org/10.1161/CIRCULATIONAHA.109.849919
Neubauer S (2007) The failing heart–an engine out of fuel. N Engl J Med 356(11):1140–1151. https://doi.org/10.1056/NEJMra063052
Taegtmeyer H, Golfman L, Sharma S, Razeghi P, van Arsdall M (2004) Linking gene expression to function: metabolic flexibility in the normal and diseased heart. Ann N Y Acad Sci 1015:202–213. https://doi.org/10.1196/annals.1302.017
Neely JR, Rovetto MJ, Oram JF (1972) Myocardial utilization of carbohydrate and lipids. Prog Cardiovasc Dis 15(3):289–329. https://doi.org/10.1016/0033-0620(72)90029-1
Labbe SM, Grenier-Larouche T, Noll C et al (2012) Increased myocardial uptake of dietary fatty acids linked to cardiac dysfunction in glucose-intolerant humans. Diabetes 61(11):2701–2710. https://doi.org/10.2337/db11-1805
Ferre P (2004) The biology of peroxisome proliferator-activated receptors: relationship with lipid metabolism and insulin sensitivity. Diabetes 53(Suppl 1):S43-50. https://doi.org/10.2337/diabetes.53.2007.s43
Cha DR, Han JY, Su DM et al (2007) Peroxisome proliferator-activated receptor-alpha deficiency protects aged mice from insulin resistance induced by high-fat diet. Am J Nephrol 27(5):479–482. https://doi.org/10.1159/000106485
Rijzewijk LJ, van der Meer RW, Lamb HJ et al (2009) Altered myocardial substrate metabolism and decreased diastolic function in nonischemic human diabetic cardiomyopathy: studies with cardiac positron emission tomography and magnetic resonance imaging. J Am Coll Cardiol 54(16):1524–1532. https://doi.org/10.1016/j.jacc.2009.04.074
Ng AC, Delgado V, Bertini M et al (2010) Myocardial steatosis and biventricular strain and strain rate imaging in patients with type 2 diabetes mellitus. Circulation 122(24):2538–2544. https://doi.org/10.1161/CIRCULATIONAHA.110.955542
Du X, Edelstein D, Obici S, Higham N, Zou MH, Brownlee M (2006) Insulin resistance reduces arterial prostacyclin synthase and eNOS activities by increasing endothelial fatty acid oxidation. J Clin Invest 116(4):1071–1080. https://doi.org/10.1172/JCI23354
Fillmore N, Mori J, Lopaschuk GD (2014) Mitochondrial fatty acid oxidation alterations in heart failure, ischaemic heart disease and diabetic cardiomyopathy. Br J Pharmacol 171(8):2080–2090. https://doi.org/10.1111/bph.12475
Hafstad AD, Nabeebaccus AA, Shah AM (2013) Novel aspects of ROS signalling in heart failure. Basic Res Cardiol 108(4):359. https://doi.org/10.1007/s00395-013-0359-8
How OJ, Aasum E, Severson DL, Chan WY, Essop MF, Larsen TS (2006) Increased myocardial oxygen consumption reduces cardiac efficiency in diabetic mice. Diabetes 55(2):466–473. https://doi.org/10.2337/diabetes.55.02.06.db05-1164
Hafstad AD, Solevag GH, Severson DL, Larsen TS, Aasum E (2006) Perfused hearts from type 2 diabetic (db/db) mice show metabolic responsiveness to insulin. Am J Physiol Heart Circ Physiol 290(5):H1763-1769. https://doi.org/10.1152/ajpheart.01063.2005
Chung SS, Ho EC, Lam KS, Chung SK (2003) Contribution of polyol pathway to diabetes-induced oxidative stress. J Am Soc Nephrol 14(8 Suppl 3):S233-236. https://doi.org/10.1097/01.asn.0000077408.15865.06
Sochor M, Gonzalez A-M, McLean P (1984) Regulation of alternative pathways of glucose metabolism in rat heart in alloxan diabetes: changes in the pentose phosphate pathway. Biochem Biophys Res Commun 118(1):110–116. https://doi.org/10.1016/0006-291x(84)91074-x
Petrova R, Yamamoto Y, Muraki K et al (2002) Advanced glycation endproduct-induced calcium handling impairment in mouse cardiac myocytes. J Mol Cell Cardiol 34(10):1425–1431. https://doi.org/10.1006/jmcc.2002.2084
Brownlee M (1995) Advanced protein glycosylation in diabetes and aging. Annu Rev Med 46:223–234. https://doi.org/10.1146/annurev.med.46.1.223
McNulty PH (2007) Hexosamine biosynthetic pathway flux and cardiomyopathy in type 2 diabetes mellitus. Focus on “Impact of type 2 diabetes and aging on cardiomyocyte function and O-linked N-acetylglucosamine levels in the heart”. Am J Physiol Cell Physiol 292(4):C1243–1244. https://doi.org/10.1152/ajpcell.00521.2006
Roche E, Farfari S, Witters LA et al (1998) Long-term exposure of beta-INS cells to high glucose concentrations increases anaplerosis, lipogenesis, and lipogenic gene expression. Diabetes 47(7):1086–1094. https://doi.org/10.2337/diabetes.47.7.1086
Anderson EJ, Kypson AP, Rodriguez E, Anderson CA, Lehr EJ, Neufer PD (2009) Substrate-specific derangements in mitochondrial metabolism and redox balance in the atrium of the type 2 diabetic human heart. J Am Coll Cardiol 54(20):1891–1898. https://doi.org/10.1016/j.jacc.2009.07.031
Croston TL, Thapa D, Holden AA et al (2014) Functional deficiencies of subsarcolemmal mitochondria in the type 2 diabetic human heart. Am J Physiol Heart Circ Physiol 307(1):H54-65. https://doi.org/10.1152/ajpheart.00845.2013
Boudina S, Sena S, Theobald H et al (2007) Mitochondrial energetics in the heart in obesity-related diabetes: direct evidence for increased uncoupled respiration and activation of uncoupling proteins. Diabetes 56(10):2457–2466. https://doi.org/10.2337/db07-0481
Giardino I, Edelstein D, Brownlee M (1996) BCL-2 expression or antioxidants prevent hyperglycemia-induced formation of intracellular advanced glycation endproducts in bovine endothelial cells. J Clin Invest 97(6):1422–1428. https://doi.org/10.1172/JCI118563
Zorzano A, Liesa M, Palacin M (2009) Role of mitochondrial dynamics proteins in the pathophysiology of obesity and type 2 diabetes. Int J Biochem Cell Biol 41(10):1846–1854. https://doi.org/10.1016/j.biocel.2009.02.004
Scheuermann-Freestone M, Madsen PL, Manners D et al (2003) Abnormal cardiac and skeletal muscle energy metabolism in patients with type 2 diabetes. Circulation 107(24):3040–3046. https://doi.org/10.1161/01.CIR.0000072789.89096.10
Savabi F (1991) Alteration of the phosphocreatine energy shuttle components in diabetic rat heart. J Mol Cell Cardiol 23(11):1323–1333. https://doi.org/10.1016/0022-2828(91)90089-5
Montaigne D, Marechal X, Coisne A et al (2014) Myocardial contractile dysfunction is associated with impaired mitochondrial function and dynamics in type 2 diabetic but not in obese patients. Circulation 130(7):554–564. https://doi.org/10.1161/CIRCULATIONAHA.113.008476
Andreyev AY, Kushnareva YE, Starkov AA (2005) Mitochondrial metabolism of reactive oxygen species. Biochemistry (Mosc) 70(2):200–214. https://doi.org/10.1007/s10541-005-0102-7
Nishikawa T, Edelstein D, Du XL et al (2000) Normalizing mitochondrial superoxide production blocks three pathways of hyperglycaemic damage. Nature 404(6779):787–790. https://doi.org/10.1038/35008121
Schannwell CM, Schneppenheim M, Perings S, Plehn G, Strauer BE (2002) Left ventricular diastolic dysfunction as an early manifestation of diabetic cardiomyopathy. Cardiology 98(1–2):33–39. https://doi.org/10.1159/000064682
Pereira L, Ruiz-Hurtado G, Rueda A, Mercadier JJ, Benitah JP, Gomez AM (2014) Calcium signaling in diabetic cardiomyocytes. Cell Calcium 56(5):372–380. https://doi.org/10.1016/j.ceca.2014.08.004
Murarka S, Movahed MR (2010) Diabetic cardiomyopathy. J Card Fail 16(12):971–979. https://doi.org/10.1016/j.cardfail.2010.07.249
Levy D, Garrison RJ, Savage DD, Kannel WB, Castelli WP (1990) Prognostic implications of echocardiographically determined left ventricular mass in the framingham heart study. N Engl J Med 322(22):1561–1566. https://doi.org/10.1056/NEJM199005313222203
Selmeryd J, Sundstedt M, Nilsson G, Henriksen E, Hedberg P (2014) Impact of left ventricular geometry on long-term survival in elderly men and women. Clin Physiol Funct Imaging 34(6):442–448. https://doi.org/10.1111/cpf.12114
Lieb W, Gona P, Larson MG et al (2014) The natural history of left ventricular geometry in the community: clinical correlates and prognostic significance of change in LV geometric pattern. JACC Cardiovasc Imaging 7(9):870–878. https://doi.org/10.1016/j.jcmg.2014.05.008
Forbes JM, Cooper ME (2013) Mechanisms of diabetic complications. Physiol Rev 93(1):137–188. https://doi.org/10.1152/physrev.00045.2011
Paradis P, Dali-Youcef N, Paradis FW, Thibault G, Nemer M (2000) Overexpression of angiotensin II type I receptor in cardiomyocytes induces cardiac hypertrophy and remodeling. Proc Natl Acad Sci U S A 97(2):931–936. https://doi.org/10.1073/pnas.97.2.931
Munzel T, Gori T, Keaney JF Jr, Maack C, Daiber A (2015) Pathophysiological role of oxidative stress in systolic and diastolic heart failure and its therapeutic implications. Eur Heart J 36(38):2555–2564. https://doi.org/10.1093/eurheartj/ehv305
Kumar R, Thomas CM, Yong QC, Chen W, Baker KM (2012) The intracrine renin-angiotensin system. Clin Sci (Lond) 123(5):273−284. https://doi.org/10.1042/CS20120089
Yamamoto E, Dong YF, Kataoka K et al (2008) Olmesartan prevents cardiovascular injury and hepatic steatosis in obesity and diabetes, accompanied by apoptosis signal regulating kinase-1 inhibition. Hypertension 52(3):573–580. https://doi.org/10.1161/HYPERTENSIONAHA.108.112292
Fukuda M, Nakamura T, Kataoka K et al (2010) Potentiation by candesartan of protective effects of pioglitazone against type 2 diabetic cardiovascular and renal complications in obese mice. J Hypertens 28(2):340–352. https://doi.org/10.1097/HJH.0b013e32833366cd
Liu X, Xu Q, Wang X et al (2015) Irbesartan ameliorates diabetic cardiomyopathy by regulating protein kinase D and ER stress activation in a type 2 diabetes rat model. Pharmacol Res 93:43–51. https://doi.org/10.1016/j.phrs.2015.01.001
Oliveira-Junior SA, Martinez PF, Guizoni DM, et al. (2014) AT1 receptor blockade attenuates insulin resistance and myocardial remodeling in rats with diet-induced obesity. PLoS One 9(1):e86447. https://doi.org/10.1371/journal.pone.0086447
Huynh K, Bernardo BC, McMullen JR, Ritchie RH (2014) Diabetic cardiomyopathy: mechanisms and new treatment strategies targeting antioxidant signaling pathways. Pharmacol Ther 142(3):375–415. https://doi.org/10.1016/j.pharmthera.2014.01.003
Zaman AK, Fujii S, Sawa H et al (2001) Angiotensin-converting enzyme inhibition attenuates hypofibrinolysis and reduces cardiac perivascular fibrosis in genetically obese diabetic mice. Circulation 103(25):3123–3128. https://doi.org/10.1161/01.cir.103.25.3123
Toblli JE, Cao G, DeRosa G, Forcada P (2005) Reduced cardiac expression of plasminogen activator inhibitor 1 and transforming growth factor beta1 in obese Zucker rats by perindopril. Heart 91(1):80–86. https://doi.org/10.1136/hrt.2003.022707
Nevelsteen I, Bito V, Van der Mieren G et al (2013) ACE-inhibition, but not weight reduction restores cardiomyocyte response to beta-adrenergic stimulation in the metabolic syndrome. BMC Cardiovasc Disord 13:51. https://doi.org/10.1186/1471-2261-13-51
Tabbi-Anneni I, Buchanan J, Cooksey RC, Abel ED (2008) Captopril normalizes insulin signaling and insulin-regulated substrate metabolism in obese (ob/ob) mouse hearts. Endocrinology 149(8):4043–4050. https://doi.org/10.1210/en.2007-1646
Kang YS, Lee MH, Song HK et al (2011) Aliskiren improves insulin resistance and ameliorates diabetic vascular complications in db/db mice. Nephrol Dial Transplant 26(4):1194–1204. https://doi.org/10.1093/ndt/gfq579
Dong YF, Liu L, Lai ZF et al (2010) Aliskiren enhances protective effects of valsartan against type 2 diabetic nephropathy in mice. J Hypertens 28(7):1554–1565. https://doi.org/10.1097/HJH.0b013e328338bb11
Jiang F, Yang J, Zhang Y et al (2014) Angiotensin-converting enzyme 2 and angiotensin 1–7: novel therapeutic targets. Nat Rev Cardiol 11(7):413–426. https://doi.org/10.1038/nrcardio.2014.59
Santos SH, Fernandes LR, Mario EG et al (2008) Mas deficiency in FVB/N mice produces marked changes in lipid and glycemic metabolism. Diabetes 57(2):340–347. https://doi.org/10.2337/db07-0953
Patel VB, Bodiga S, Basu R et al (2012) Loss of angiotensin-converting enzyme-2 exacerbates diabetic cardiovascular complications and leads to systolic and vascular dysfunction: a critical role of the angiotensin II/AT1 receptor axis. Circ Res 110(10):1322–1335. https://doi.org/10.1161/circresaha.112.268029
Zhong J, Basu R, Guo D, et al (2010) Angiotensin-converting enzyme 2 suppresses pathological hypertrophy, myocardial fibrosis, and cardiac dysfunction. Circulation 122(7):717–728. 718 p following 728. https://doi.org/10.1161/circulationaha.110.955369
Dong B, Yu QT, Dai HY et al (2012) Angiotensin-converting enzyme-2 overexpression improves left ventricular remodeling and function in a rat model of diabetic cardiomyopathy. J Am Coll Cardiol 59(8):739–747. https://doi.org/10.1016/j.jacc.2011.09.071
Patel VB, Takawale A, Ramprasath T et al (2015) Antagonism of angiotensin 1–7 prevents the therapeutic effects of recombinant human ACE2. J Mol Med (Berl) 93(9):1003–1013. https://doi.org/10.1007/s00109-015-1285-z
Patel VB, Zhong JC, Grant MB, Oudit GY (2016) Role of the ACE2/Angiotensin 1–7 axis of the renin-angiotensin system in heart failure. Circ Res 118(8):1313–1326. https://doi.org/10.1161/CIRCRESAHA.116.307708
Mori J, Patel VB, Abo Alrob O et al (2014) Angiotensin 1–7 ameliorates diabetic cardiomyopathy and diastolic dysfunction in db/db mice by reducing lipotoxicity and inflammation. Circ Heart Fail 7(2):327–339. https://doi.org/10.1161/CIRCHEARTFAILURE.113.000672
Hao PP, Yang JM, Zhang MX et al (2015) Angiotensin-(1–7) treatment mitigates right ventricular fibrosis as a distinctive feature of diabetic cardiomyopathy. Am J Physiol Heart Circ Physiol 308(9):H1007-1019. https://doi.org/10.1152/ajpheart.00563.2014
Singh K, Singh T, Sharma PL (2011) Beneficial effects of angiotensin (1–7) in diabetic rats with cardiomyopathy. Ther Adv Cardiovasc Dis 5(3):159–167. https://doi.org/10.1177/1753944711409281
Sukumaran V, Tsuchimochi H, Tatsumi E, Shirai M, Pearson JT (2017) Azilsartan ameliorates diabetic cardiomyopathy in young db/db mice through the modulation of ACE-2/ANG 1–7/Mas receptor cascade. Biochem Pharmacol 144:90–99. https://doi.org/10.1016/j.bcp.2017.07.022
Hao P, Yang J, Liu Y et al (2015) Combination of angiotensin-(1–7) with perindopril is better than single therapy in ameliorating diabetic cardiomyopathy. Sci Rep 5:8794. https://doi.org/10.1038/srep08794
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2023 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Gomes, K.P., Jadli, A.S., Patel, V.B. (2023). Renin Angiotensin System in the Pathophysiology of Diabetic Cardiomyopathy in Type 2 Diabetes. In: Dhalla, N.S., Bhullar, S.K., Shah, A.K. (eds) The Renin Angiotensin System in Cardiovascular Disease. Advances in Biochemistry in Health and Disease, vol 24. Springer, Cham. https://doi.org/10.1007/978-3-031-14952-8_15
Download citation
DOI: https://doi.org/10.1007/978-3-031-14952-8_15
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-14951-1
Online ISBN: 978-3-031-14952-8
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)