Abstract
Background: Periodontitis is a chronic inflammatory disease characterized by the loss of tooth-supporting tissues (or periodontium) leading to the formation of periodontal pocket then to tooth loss. Conventional therapies that involve tooth root debridement are still disappointing because they are more centered on periodontal repair than disease pathophysiology causes. The meta-analysis we present here focused on the results of experimental studies that investigated periodontal mesenchymal stromal cells (MSCs) therapy, a promising strategy to regenerate tissue, given to their immunomodulatory and trophic properties.
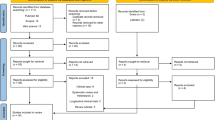
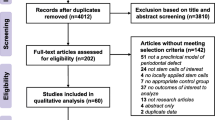
Methods: Using PubMed database and ICTRP search portal, 84 animal and 3 randomized human studies were analyzed.
Results: Overall, our results highlighted that MSCs grafting, regardless of their tissue origin, enhances periodontal regeneration. A defect morphology suitable for an initial clot stabilization increases the procedure efficacy, especially if cells are carried using a vehicle from natural origin. Nevertheless, methodological biases have been highlighted and still limit the translation to human with high prognosis and regulatory considerations. Besides, because only 2 randomized human trials demonstrated the efficacy of the procedure, further studies are needed to investigate periodontal regeneration procedures on experimental models closer to human pathophysiology.
Conclusion: Although MSCs grafting in periodontal disease demonstrated therapeutic benefits in animal, it is critical to define more accurately protocols translatable to human and focus on the treatment of the pathology as a whole rather than on the restitution of the sole destroyed tissues.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Abdal-Wahab M, Ghaffar KAA, Ezzatt OM et al (2020) Regenerative potential of cultured gingival fibroblasts in treatment of periodontal intrabony defects (randomized clinical and biochemical trial). J Periodontal Res 55:441–452. https://doi.org/10.1111/jre.12728
Aichelmann-Reidy ME, Reynolds MA (2008) Predictability of clinical outcomes following regenerative therapy in intrabony defects. J Periodontol 79:387–393. https://doi.org/10.1902/jop.2008.060521
Aimetti M, Ferrarotti F, Cricenti L et al (2014) Autologous dental pulp stem cells in periodontal regeneration: a case report. Int J Periodontics Restorative Dent 34(Suppl 3):s27–s33. https://doi.org/10.11607/prd.1635
Akbay A, Baran C, Günhan O et al (2005) Periodontal regenerative potential of autogenous periodontal ligament grafts in Class II furcation defects. J Periodontol 76:595–604. https://doi.org/10.1902/jop.2005.76.4.595
Al-Sharabi N, Xue Y, Udea M et al (2016) Influence of bone marrow stromal cell secreted molecules on pulpal and periodontal healing in replanted immature rat molars. Dent Traumatol 32:231–239. https://doi.org/10.1111/edt.12246
An K, Liu H (2014) [Survival of bone marrow mesenchymal stem cells and periodontal ligament stem cells in cell sheets]. Zhonghua Kou Qiang Yi Xue Za Zhi 49:682–687
Ankrum JA, Ong JF, Karp JM (2014) Mesenchymal stem cells: immune evasive, not immune privileged. Nat Biotechnol 32:252–260. https://doi.org/10.1038/nbt.2816
Bartold PM, Van Dyke TE (2013) Periodontitis: a host-mediated disruption of microbial homeostasis. Unlearning learned concepts Periodontol 2000 62:203–217. https://doi.org/10.1111/j.1600-0757.2012.00450.x
Berglund AK, Fortier LA, Antczak DF, Schnabel LV (2017) Immunoprivileged no more: measuring the immunogenicity of allogeneic adult mesenchymal stem cells. Stem Cell Res Ther 8. https://doi.org/10.1186/s13287-017-0742-8
Bosshardt DD, Stadlinger B, Terheyden H (2015) Cell-to-cell communication—periodontal regeneration. Clin Oral Implants Res 26:229–239. https://doi.org/10.1111/clr.12543
Chen F-M, Gao L-N, Tian B-M et al (2016a) Treatment of periodontal intrabony defects using autologous periodontal ligament stem cells: a randomized clinical trial. Stem Cell Res Ther 7:33. https://doi.org/10.1186/s13287-016-0288-1
Chen F-M, Gao L-N, Tian B-M et al (2016b) Treatment of periodontal intrabony defects using autologous periodontal ligament stem cells: a randomized clinical trial. Stem Cell Res Ther 7:33. https://doi.org/10.1186/s13287-016-0288-1
Chen F-M, Wu L-A, Zhang M et al (2011) Homing of endogenous stem/progenitor cells for in situ tissue regeneration: promises, strategies, and translational perspectives. Biomaterials 32:3189–3209. https://doi.org/10.1016/j.biomaterials.2010.12.032
Dhote R, Charde P, Bhongade M, Rao J (2015) Stem cells cultured on beta tricalcium phosphate (β-TCP) in combination with recombinant human platelet-derived growth factor – BB (rh-PDGF-BB) for the treatment of human infrabony defects. J Stem Cells 10:243–254. jsc.2015.10.4.243
Feng F, Akiyama K, Liu Y et al (2010) Utility of PDL progenitors for in vivo tissue regeneration: a report of 3 cases. Oral Dis 16:20–28
Fu**ami K, Yamamoto S, Ota M et al (2007) Effectiveness of proliferating tissues in combination with bovine-derived xenografts to intrabony defects of alveolar bone in dogs. Biomed Res 28:107–113. https://doi.org/10.2220/biomedres.28.107
Galipeau J, Sensébé L (2018) Mesenchymal stromal cells: clinical challenges and therapeutic opportunities. Cell Stem Cell 22:824–833. https://doi.org/10.1016/j.stem.2018.05.004
Graves DT, Fine D, Teng Y-TA et al (2008) The use of rodent models to investigate host-bacteria interactions related to periodontal diseases. J Clin Periodontol 35:89–105. https://doi.org/10.1111/j.1600-051X.2007.01172.x
Graziani F, Karapetsa D, Alonso B, Herrera D (2017) Nonsurgical and surgical treatment of periodontitis: how many options for one disease? Periodontology 2000 75:152–188. https://doi.org/10.1111/prd.12201
Hajishengallis G (2014) Immunomicrobial pathogenesis of periodontitis: keystones, pathobionts, and host response. Trends Immunol 35:3–11. https://doi.org/10.1016/j.it.2013.09.001
Han N, Zhang F, Li G et al (2017) Local application of IGFBP5 protein enhanced periodontal tissue regeneration via increasing the migration, cell proliferation and osteo/dentinogenic differentiation of mesenchymal stem cells in an inflammatory niche. Stem Cell Res Ther 8:210. https://doi.org/10.1186/s13287-017-0663-6
Haney JM, Zimmerman GJ, Wikesjö UM (1995) Periodontal repair in dogs: evaluation of the natural disease model. J Clin Periodontol 22:208–213. https://doi.org/10.1111/j.1600-051x.1995.tb00136.x
Hernández-Monjaraz B, Santiago-Osorio E, Ledesma-Martínez E et al (2018) Retrieval of a periodontally compromised tooth by allogeneic grafting of mesenchymal stem cells from dental pulp: a case report. J Int Med Res 46:2983–2993. https://doi.org/10.1177/0300060518773244
Huang GT-J, Gronthos S, Shi S (2009) Mesenchymal stem cells derived from dental tissues vs. those from other sources: their biology and role in regenerative medicine. J Dent Res 88:792–806. https://doi.org/10.1177/0022034509340867
Kawaguchi H, Hayashi H, Mizuno N, et al (2005) [Cell transplantation for periodontal diseases. A novel periodontal tissue regenerative therapy using bone marrow mesenchymal stem cells]. Clin Calcium 15:99–104. CliCa11971202
Kawai T, Katagiri W, Osugi M et al (2015) Secretomes from bone marrow-derived mesenchymal stromal cells enhance periodontal tissue regeneration. Cytotherapy 17:369–381. https://doi.org/10.1016/j.jcyt.2014.11.009
Kern S, Eichler H, Stoeve J et al (2006) Comparative analysis of mesenchymal stem cells from bone marrow, umbilical cord blood, or adipose tissue. Stem Cells 24:1294–1301. https://doi.org/10.1634/stemcells.2005-0342
Kinane DF, Bartold PM (2007) Clinical relevance of the host responses of periodontitis. Periodontol 2000 43:278–293. https://doi.org/10.1111/j.1600-0757.2006.00169.x
Kinane DF, Stathopoulou PG, Papapanou PN (2017) Periodontal diseases. Nat Rev Dis Primers 3:17038. https://doi.org/10.1038/nrdp.2017.38
Kl V, Ryana H, Dalvi PJ (2017) Autologous periodontal stem cell assistance in periodontal regeneration technique (SAI-PRT) in the treatment of periodontal intrabony defects: a case report with one-year follow-up. J Dent Res Dent Clin Dent Prospects 11:123–126. https://doi.org/10.15171/joddd.2017.022
Lamont RJ, Hajishengallis G (2015) Polymicrobial synergy and dysbiosis in inflammatory disease. Trends Mol Med 21:172–183. https://doi.org/10.1016/j.molmed.2014.11.004
Lemaitre M, Monsarrat P, Blasco-Baque V et al (2017) Periodontal tissue regeneration using syngeneic adipose-derived stromal cells in a mouse model. Stem Cells Transl Med. https://doi.org/10.5966/sctm.2016-0028
Li H, Yan F, Lei L et al (2009) Application of autologous cryopreserved bone marrow mesenchymal stem cells for periodontal regeneration in dogs. Cells Tissues Organs (Print) 190:94–101. https://doi.org/10.1159/000166547
Lin N-H, Gronthos S, Bartold PM (2009) Stem cells and future periodontal regeneration. Periodontol 2000 51:239–251. https://doi.org/10.1111/j.1600-0757.2009.00303.x
Liu H, Li M, Du L et al (2015) Local administration of stromal cell-derived factor-1 promotes stem cell recruitment and bone regeneration in a rat periodontal bone defect model. Mater Sci Eng C Mater Biol Appl 53:83–94. https://doi.org/10.1016/j.msec.2015.04.002
Liu J, Ruan J, Weir MD, et al (2019) Periodontal bone-ligament-cementum regeneration via scaffolds and stem cells. Cells 8:. https://doi.org/10.3390/cells8060537
Lu H, Wu Z-F, Tian Y (2004) A study on the effects of cells and scaffolds tissue engineering on the periodontal regeneration. Zhonghua Kou Qiang Yi Xue Za Zhi 39:189–192
Martin I, Galipeau J, Kessler C et al (2019) Challenges for mesenchymal stromal cell therapies. Sci Transl Med 11. https://doi.org/10.1126/scitranslmed.aat2189
Moher D, Liberati A, Tetzlaff J et al (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ 339:b2535
Monsarrat P, Blaizot A, Kémoun P et al (2016a) Clinical research activity in periodontal medicine: a systematic map** of trial registers. J Clin Periodontol 43:390–400. https://doi.org/10.1111/jcpe.12534
Monsarrat P, Kemoun P, Vergnes J-N et al (2016b) Spatial and temporal structure of the clinical research based on mesenchymal stromal cells: A network analysis. Cytotherapy. https://doi.org/10.1016/j.jcyt.2016.09.005
Monsarrat P, Vergnes J-N, Nabet C et al (2014) Concise review: mesenchymal stromal cells used for periodontal regeneration: a systematic review. Stem Cells Transl Med 3:768–774. https://doi.org/10.5966/sctm.2013-0183
Monsarrat VJ-N, Planat-Bénard V et al (2016c) An Innovative, Comprehensive Map** and Multiscale Analysis of Registered Trials for Stem Cell-Based Regenerative Medicine. Stem Cells Transl Med 5:826–835. https://doi.org/10.5966/sctm.2015-0329
Murano Y, Ota M, Katayama A et al (2006) Periodontal regeneration following transplantation of proliferating tissue derived from periodontal ligament into class III furcation defects in dogs. Biomed Res 27:139–147. https://doi.org/10.2220/biomedres.27.139
Nagata M, Iwasaki K, Akazawa K et al (2017) Conditioned medium from periodontal ligament stem cells enhances periodontal regeneration. Tissue Eng Part A 23:367–377. https://doi.org/10.1089/ten.TEA.2016.0274
Nanci A, Bosshardt DD (2006) Structure of periodontal tissues in health and disease. Periodontol 2000 40:11–28. https://doi.org/10.1111/j.1600-0757.2005.00141.x
Ou L, Liu H, Pang J (2000) Effects of autogenous periodontal ligament cell transplantation on periodontal tissue regeneration in dogs. Zhonghua Kou Qiang Yi Xue Za Zhi 35:44–46
Ou L, Liu H, Wang D et al (2002) The study of calcification of autogenous bone marrow stem cell transplantation on alveolar bone defect in dogs. Zhonghua Kou Qiang Yi Xue Za Zhi 37:132–134
Papapanou PN, Sanz M, Buduneli N et al (2018) Periodontitis: consensus report of workgroup 2 of the 2017 world workshop on the classification of periodontal and peri-implant diseases and conditions. J Periodontol 89(Suppl 1):S173–S182. https://doi.org/10.1002/JPER.17-0721
Pittenger MF, Discher DE, Péault BM et al (2019) Mesenchymal stem cell perspective: cell biology to clinical progress. npj. Regen Med 4:1–15. https://doi.org/10.1038/s41536-019-0083-6
Poggi A, Zocchi MR (2019) Immunomodulatory properties of mesenchymal stromal cells: still unresolved “Yin and Yang”. Curr Stem Cell Res Ther 14:344–350. https://doi.org/10.2174/1574888X14666181205115452
Polimeni G, **ropaidis AV, Wikesjö UME (2006) Biology and principles of periodontal wound healing/regeneration. Periodontol 2000 41:30–47. https://doi.org/10.1111/j.1600-0757.2006.00157.x
Qiu J, Wang X, Zhou H et al (2020) Enhancement of periodontal tissue regeneration by conditioned media from gingiva-derived or periodontal ligament-derived mesenchymal stem cells: a comparative study in rats. Stem Cell Res Ther 11:42. https://doi.org/10.1186/s13287-019-1546-9
Sakaguchi K, Katagiri W, Osugi M et al (2017) Periodontal tissue regeneration using the cytokine cocktail mimicking secretomes in the conditioned media from human mesenchymal stem cells. Biochem Biophys Res Commun 484:100–106. https://doi.org/10.1016/j.bbrc.2017.01.065
Schwarzer G, Carpenter JR, Rücker G (2015) Meta-analysis with R. Springer
Sculean A, Nikolidakis D, Nikou G et al (2015) Biomaterials for promoting periodontal regeneration in human intrabony defects: a systematic review. Periodontol 2000 68:182–216. https://doi.org/10.1111/prd.12086
Sculean A, Windisch P, Szendröi-Kiss D et al (2008) Clinical and histologic evaluation of an enamel matrix derivative combined with a biphasic calcium phosphate for the treatment of human intrabony periodontal defects. J Periodontol 79:1991–1999. https://doi.org/10.1902/jop.2008.080009
Shalini HS, Vandana KL (2018) Direct application of autologous periodontal ligament stem cell niche in treatment of periodontal osseous defects: A randomized controlled trial. J Indian Soc Periodontol 22:503–512. https://doi.org/10.4103/jisp.jisp_92_18
Si Z, Wang X, Sun C et al (2019) Adipose-derived stem cells: Sources, potency, and implications for regenerative therapies. Biomed Pharmacother 114:108765. https://doi.org/10.1016/j.biopha.2019.108765
Struillou X, Boutigny H, Soueidan A, Layrolle P (2010) Experimental animal models in periodontology: a review. Open Dent J 4:37–47. https://doi.org/10.2174/1874210601004010037
Suaid FF, Ribeiro FV, Gomes TRLES et al (2012) Autologous periodontal ligament cells in the treatment of Class III furcation defects: a study in dogs. J Clin Periodontol 39:377–384. https://doi.org/10.1111/j.1600-051X.2012.01858.x
Sun C, Liu H (2014) Periodontal tissue in a bio-implant by periodontal ligament cells sheet and bone marrow stromal cells sheet. Zhonghua Kou Qiang Yi Xue Za Zhi 49:84–88
Sun W, Wang Z, Xu Q et al (2019) The treatment of systematically transplanted gingival mesenchymal stem cells in periodontitis in mice. Exp Ther Med 17:2199–2205. https://doi.org/10.3892/etm.2019.7165
Takedachi M, Sawada K, Yamamoto S et al (2013) Periodontal tissue regeneration by transplantation of adipose tissue-derived stem cells. J Oral Biosci 55:137–142. https://doi.org/10.1016/j.job.2013.04.004
Tobita M, Mizuno H (2013) Adipose-derived stem cells and platelet-rich plasma: the keys to functional periodontal tissue engineering. Curr Stem Cell Res Ther 8:400–406
Tobita M, Uysal CA, Guo X et al (2013) Periodontal tissue regeneration by combined implantation of adipose tissue-derived stem cells and platelet-rich plasma in a canine model. Cytotherapy 15:1517–1526. https://doi.org/10.1016/j.jcyt.2013.05.007
Van Dyke TE, Bartold PM, Reynolds EC (2020) The nexus between periodontal inflammation and dysbiosis. Front Immunol 11. https://doi.org/10.3389/fimmu.2020.00511
Wang F, Du L, Ge S (2016) PTH/SDF-1α cotherapy induces CD90+CD34- stromal cells migration and promotes tissue regeneration in a rat periodontal defect model. Sci Rep 6:30403. https://doi.org/10.1038/srep30403
Wikesjö UM, Selvig KA (1999) Periodontal wound healing and regeneration. Periodontol 2000 (19):21–39
Wu V, Helder MN, Bravenboer N et al (2019) Bone Tissue Regeneration in the Oral and Maxillofacial Region: A Review on the Application of Stem Cells and New Strategies to Improve Vascularization. Stem Cells Int 2019:6279721. https://doi.org/10.1155/2019/6279721
Xu C, Guo F, Gao Q et al (2006) Effects of astragalus polysaccharides-chitosan/polylactic acid scaffolds and bone marrow stem cells on repairing supra-alveolar periodontal defects in dogs. Zhong Nan Da Xue Xue Bao Yi Xue Ban 31:512–517
Yamada Y, Ueda M, Hibi H, Baba S (2006) A novel approach to periodontal tissue regeneration with mesenchymal stem cells and platelet-rich plasma using tissue engineering technology: A clinical case report. Int J Periodontics Restorative Dent 26:363–369
Yan X-Z, Yang F, Jansen JA et al (2015) Cell-based approaches in periodontal regeneration: a systematic review and meta-analysis of periodontal defect models in animal experimental work. Tissue Eng Part B Rev 21:411–426. https://doi.org/10.1089/ten.TEB.2015.0049
Yang H, Aprecio RM, Zhou X et al (2014) Therapeutic effect of TSG-6 engineered iPSC-derived MSCs on experimental periodontitis in rats: a pilot study. PLoS One 9:e100285. https://doi.org/10.1371/journal.pone.0100285
Acknowledgment
We gratefully acknowledge the Programme d’Investissements d’Avenir and the Agence Nationale pour la Recherche for the grant grant ANR–16–CE18–0019–01 and the national infrastructure “ECELLFrance: Development of mesenchymal stem cell based therapies” (PIA-ANR-11-INBS-005).
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Appendix
Appendix
Forest plot of the meta-analysis of the effect of mesenchymal stromal cells therapy on bone regeneration
Forest plot of the standardized mean difference (SMD) for alveolar bone regeneration and its 95% confidence interval for each study comparison. A value above 0 means that therapeutic effect is in favor of cell therapy.
Forest plot of the meta-analysis of the effect of mesenchymal stromal cells therapy on cementum regeneration
Forest plot of the standardized mean difference (SMD) for cementum regeneration and its 95% confidence interval for each study comparison. A value above 0 means that therapeutic effect is in favor of cell therapy
Rights and permissions
Copyright information
© 2022 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Dubuc, A., Planat-Bénard, V., Marty, M., Monsarrat, P., Kémoun, P. (2022). Periodontal Cell Therapy: A Systematic Review and Meta-analysis. In: Santi-Rocca, J. (eds) Periodontitis. Advances in Experimental Medicine and Biology, vol 1373. Springer, Cham. https://doi.org/10.1007/978-3-030-96881-6_20
Download citation
DOI: https://doi.org/10.1007/978-3-030-96881-6_20
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-96880-9
Online ISBN: 978-3-030-96881-6
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)