Abstract
The aim of this study was to determine the level of antibodies against hemagglutinin of influenza viruses in the sera of people in different age groups in the epidemic season 2013/2014 in Poland. The level of anti-hemagglutinin antibodies was determined by hemagglutination inhibition test (HAI). A total number of 1,050 randomly selected sera was tested in seven age groups. The level of antibodies against influenza viruses was very low, which indicates that the people have not been vaccinated against influenza in the epidemic season 2013/2014. The value of protection rate against influenza in the Polish population is very low. These results are worrying, because complications of influenza may be harmful to health and even life-threatening to persons who are not vaccinated. Furthermore, these results confirm the circulation of three antigenically different influenza virus strains, two subtypes of influenza A virus – A/California/7/2009/(H1N1)pdm09 and A/Victoria/361/2011(H3N2) - and B/Massachusetts/2/2012.
You have full access to this open access chapter, Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
Influenza is an infectious disease caused by influenza viruses from the Orthomyxoviridae family. The continuing evolution of the virus is the cause of seasonal epidemics and, from time to time, of pandemics in the human population. Furthermore, due to appearance of influenza-like illnesses, diagnosis of this disease on the basis of clinical symptoms is possible only during the outbreak. It should be noted that in case of respiratory infections various clinical symptoms can be caused by the same virus and, on the other hand, the same set of symptoms can be caused by more than 200 different viruses (e.g. parainfluenza, adenovirus, rhinovirus, and coronavirus). For this reason, the laboratory confirmation of influenza virus infection is crucial in the influenza surveillance and is essential for evaluating the effectiveness of vaccines and antiviral drugs. Laboratory diagnosis of influenza includes confirmation of the presence of influenza virus antigen in the material collected from the patient and serological evidence of infection with influenza virus by detecting the increase of specific antibodies in patient’s serum (Brydak 2008).
The major line of defense from influenza infection are antibodies directed against two glycoproteins exposed on the surface of the virion – hemagglutinin (HA) and neuraminidase (NA) (Johansson et al. 1989). Furthermore, evolution of influenza virus is most evident in the case of these surface proteins. HA and NA antigens are constantly changing due to antigenic pressure. They both are highly immunogenic, and antibodies produced in response to viral infection are specific for a particular subtype of hemagglutinin (H1-H18) and neuraminidase (N1-N11) and do not give complete protection against all influenza virus strains (Nicholson et al. 1998). The presence of hemagglutinin antibodies (anti-HA) provides not only protection against infection with specific strains of influenza virus, but also might alleviate symptoms of the disease in case of infection with another variant of the virus. This is caused by the occurrence of so-called cross-reactive antibodies. It has been shown that subtype-specific anti-HA antibodies can decrease the infectivity of the virus of other subtype by disruption of proliferation and release of viral particles during infection (Ekiert et al. 2011; Epstein and Price 2010; Thorsby et al. 2008). For this reason, regular vaccinations are essential for reducing the impact of seasonal influenza and influenza prevention. Seasonal vaccinations protect from infection with currently circulating viruses and give cross-protection, which can reduce viral replication, accelerate viral clearance, and thus reduce the severity of disease. The World Health Organization leads the global influenza surveillance and gives seasonal recommendations for influenza virus strains included in the vaccine for the upcoming epidemic season.
An anti-HA antibody titers of 1:40 has been determined as corresponding to a 50 % reduction in the risk of contracting influenza in population (Hobson et al. 1972) and it is assumed that high titers of anti-HA antibodies (≥1:40) provide protection against influenza infection. Furthermore, this value of titer, after vaccination, is required by European Agency for the Evaluation of Medicinal Products for assessment of vaccines (Committee for Proprietary Medicinal Products 1997). On the other hand, the anti-NA antibodies, even at high titers, only support the resistance because they do not prevent influenza infection themselves. However, it has been shown that the anti-NA antibodies block the replication process, alleviate the severity of infection, and reduce the incidence of disease (Brydak 2008).
Serological methods for detection of anti-influenza antibodies include, among others, hemagglutination inhibition (HAI) test and neuraminidase inhibition (NI) test. Serological tests are used not only for diagnostic purposes, but also to evaluate the resistance of the population resulting from both, natural infection and vaccination against influenza. Most laboratories use the hemagglutination inhibition test for serological diagnosis. The method is based on the ability of anti-HA antibodies to inhibit virus-induced agglutination of erythrocytes (WHO – Global Influenza Surveillance Network 2011). It is a simple, inexpensive, and rapid test, during which a small amount of reagents is used. Due to the high cost and labor-consumption, not many laboratories determines the level of antibodies with neuraminidase inhibition test (Brydak 2008).
The recorded number of cases of influenza and influenza-like illnesses depends on reporting by health care workers. In Poland, this is done by Local Sanitary Epidemiological Stations. Thereafter, these data in the form of weekly reports are sent to the National Institute of Public Health – National Institute of Hygiene by Voivodeship Sanitary Epidemiological Stations. There are two types of influenza vaccines, which are currently available in Poland: inactivated split virion and subunit. Split type vaccine contains inactivated split virus, whereas subunit type contains only viral glycoproteins, hemagglutinin and neuraminidase. It should be noted that already for many influenza seasons, numerous local governments offer free influenza vaccinations for people over 50 years of age, who often belong to high-risk groups of health. Despite this, the proportion of people vaccinated is diminishing season by season. In the epidemic season 2013/2014 only 3.75 % of the population was vaccinated against influenza (Brydak 2014).
The epidemic season 2013/2014 was mild in intensity in comparison to the previous season. A total number of 2,036,215 cases of influenza and influenza-like illness were registered in Poland in this season and the incidence was 5,284 (per 100,000 population), causing 15 deaths as a result of complications from influenza (GIS 2014). Our paper describes determination of the level of antibodies against hemagglutinin of influenza viruses present in the sera of people in different age groups, during the epidemic season 2013/2014.
2 Methods
The serum samples of people in age groups: 0–3, 4–7, 8–14, 15–25, 26–44, 45–64, and ≥65 years of age were collected by departments of epidemiology and virological laboratories of Voivodeship Sanitary Epidemiological Stations in Poland. The collected samples were stored at −80 °C until tests were done. Among the 1,050 serum samples, 150 sera were tested in each age group. Antibody status was determined by hemagglutination inhibition reaction by using eight hemagglutinin units of the virus. Prior to the HAI test, sera were inactivated according to WHO standards (Tyrell and Horsfall 1952; WHO – Global Influenza Surveillance Network 2011).
The following parameters were used for analysis of the results:
-
Geometric mean of anti-hemagglutinin antibodies in tested sera (GMT).
-
Protection rate, i. e. the proportion of subjects showing anti-hemagglutinin antibody titres ≥40.
The antigens listed in Table 1 were used in hemagglutination inhibition (HAI) tests, in agreement with the WHO recommendations (WHO 2013). All antigens were prepared in National Influenza Center, Department of Influenza Research, National Institute of Public Health – National Institute of Hygiene. Preparation and dilution of antigens for HAI tests were performed in accordance to WHO protocols (WHO – Global Influenza Surveillance Network 2011).
3 Results and Discussion
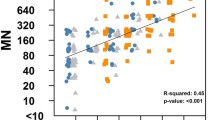
The geometric mean titers of anti-HA antibodies in sera collected from people in different age groups in the epidemic season 2013/2014 are shown in Fig. 1. The highest level of antibodies against hemagglutinin H1 was found in the age group 4–7 (GMT-27.51). The GMT of anti-H1 antibodies was slightly lower in the age group 8–14 (15.60) and low in the age groups 0–3, 15–25, 26–44 and 45–64, where there was almost the same level of antibodies (12.09-13.44). The lowest level of anti-H1 antibodies was observed in the age group ≥65 (GMT-10.05). In the case of the H3 hemagglutinin, the highest geometric mean titers were in the 4–7 (21.14) and 8–14 (20.37) years old groups. In other age groups, these values were at similar levels from 11.97 to 15.58. For type B hemagglutinin the observed level of antibodies was the highest in group of 15–25 years (GMT-24.85), lower in group of 8–14 years (GMT-12.14), and the lowest in groups of 0–3 and 4–7 years (GMT: 9.55 and 10.67, respectively). Almost identical geometric mean titers were observed in the age groups 26–44 (17.01), 45–64 (16.99), and ≥65 (16.17). In conclusion, the highest GMT titers were observed in the age groups: 4–7, 8–14, and 15–25, and a different type of anti-HA antibody had dominated in each of these groups: H1, H3 and B, respectively. The lowest geometric mean titer of antibody directed against the HA was observed in children aged 0–3 years.
The protection rate is the percentage of people with the protective titer of anti-HA antibodies of at least 40 after vaccination and, depending on age, should achieve different values: ≥70 % for people aged 18–60 years and ≥60 % for people over 60 years of age (Brydak 2008). However, the protection rate did not exceed 60 % in any age group (Fig. 2). The highest level of protection rate was observed for the hemagglutinin H1 of A/California/7/2009pdm09 strain in the age group 4–7 (53.33 %). An analysis of the protection rate with respect to the age group, including all three types of hemagglutinin, revealed that in the 0–3 years old group the level of protection exhibited similar values: 16.00 % (B), 20.67 % (H3), and 26.67 % (H1) without the domination of particular hemagglutinin type. In the age groups 4–7 and 8–14, the protection rate for H1 and H3 hemagglutinins was much higher than for hemagglutinin type B. However, in 15–25, 26–44 and 45–64 years old groups significantly higher protection rates were observed for type B hemagglutinin compared to the other two types.
In the last three epidemic seasons: 2011/2012, 2012/2013 and 2013/2014, the values of protection rate were different in particular age groups (Table 2). The comparison of protection rates for hemagglutinin H1 of A/California/7/2009pdm09 strain is especially interesting. This type of A influenza virus has been circulating in the population since 2009. In the age groups of 4–7, 26–44, 45–64, and ≥65 years there has been a significant increase in the protection rate compared to the previous two seasons. In the youngest age group this value is higher in comparison to the last season, but lower than in the 2011/2012 season. However, in groups of 8–14 and 15–25 years old the protection rates remain at a similar level in all analyzed seasons. In the case of H3 hemagglutinin of A/Victoria/361/2011 strain the protection rate increased in the age group 4–7, decreased in the age group 26–44, and did not change significantly in the group of 8–14 years, compared to the previous two epidemiological seasons. There has been a significant increase in the values of this factor in groups 15–25, 45–64, and ≥65 years old as compared to the epidemic season 2012/2013. With regard to the last season, value of protection rate substantially increased in the youngest group. A significant increase in protection rates was observed in four age groups: 0–3, 4–7, 15–25, and 26–44 for influenza B virus strain B/Massachusetts/2/2012 in epidemic season 2013/2014. In other age groups these values were similar to 2011/2012 season and lower than in previous season.
Despite the apparent increase of protection rate in some age groups, this value did not achieve 60 %. These results are truly alarming as it shows that the value of protection rate against influenza in the Polish population is very low. The complications of influenza may be hazardous to health and life-threatening to persons who are not vaccinated, especially in the very young, the elderly, and those with other serious medical conditions. Influenza vaccination is the most effective way to prevent infection, but this fact is ignored by many people. It can be concluded, on the basis of serological screening of sera from people at different age groups in the epidemic season 2013/2014, that:
-
1.
our results confirm the circulation of three antigenically different influenza strains: two subtypes of influenza A virus – A/California/7/2009(H1N1)pdm09 and A/Victoria/361/2011(H3N2) – and type B, B/Massachusetts/2/2012;
-
2.
protection rate did not exceed 60 % in any age group, which demonstrates that the proportion of people vaccinated against influenza in Poland is very low. This situation can be changed when more people will vaccinate against influenza.
References
Bednarska K, Hallmann-Szelińska E, Tomczuk K, Brydak LB (2014) Incidence of circulation antibodies against influenza viruses (hemagglutinins) in epidemic season 2012/2013 in Poland. Problemy Higieny i Epidemiologii 95(2):268–272
Brydak LB (2008) Grypa. Pandemia grypy – mit czy realne zagrożenie. Rytm, Warszawa, pp 1–492 (in Polish)
Brydak LB (2014) Grypa – problem zdrowia publicznego. Top Medical Trends Przewodnik Lekarza 1:13–15 (in Polish)
CPMP. Committee for Proprietary Medicinal Products (1997) Note for guidance on harmonisation of requirements for influenza vaccines. CPMP/BWP/214/96
Ekiert DC, Friesen RH, Bhabha G, Kwaks T, Jongeneelen M, Yu W et al (2011) A highly conserved neutralizing epitope on group 2 influenza A viruses. Science 333(6044):843–850
Epstein SL, Price GE (2010) Cross-protective immunity to influenza A viruses. Expert Rev Vaccines 9(11):1325–1341
GIS (2014) Meldunek Głównego Inspektora Sanitarnego dot. sytuacji epidemiologicznej grypy za okres 1 – 7 kwietnia 2014 r. Available from http://www.gis.gov.pl
Hobson D, Curry RL, Beare AS, Ward-Gardner A (1972) The role of serum haemagglutination-inhibiting antibody in protection against challenge infection with influenza A2 and B viruses. J Hyg (Lond) 70(4):767–777
Johansson BE, Bucher DJ, Kilbourne ED (1989) Purified influenza virus hemagglutinin and neuraminidase are equivalent in stimulation of antibody response but induce contrasting types of immunity to infection. J Virol 63:1239–1246
Nicholson KG, Webster RG, Hay AJ (1998) Textbook of Influenza. Wiley-Blackwell, Oxford, pp 1–592
Throsby M, van den Brink E, Jongeneelen M, Poon LL, Alard P, Cornelissen L et al (2008) Heterosubtypic neutralizing monoclonal antibodies cross-protective against H5N1 and H1N1 recovered from human IgM+ memory B cells. PLoS ONE 3(12):e3942
Tyrell DAJ, Horsfall FL (1952) A procedure which eliminates nonspecific inhibitor from human serum but does not affect specific antibodies against influenza viruses. J Immunol 69:563–574
WHO – Global Influenza Surveillance Network (2011) Manual for the laboratory diagnosis and virological surveillance of influenza. WHO Press, Geneva, pp 1–153
WHO (2013) Recommended composition of influenza virus vaccines for use in the 2013–14 northern hemisphere influenza season. Available from http://www.who.int/en/
Conflicts of Interest
The authors declare no conflicts of interest in relation to this article.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2015 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Bednarska, K., Nowak, M.A., Kondratiuk, K., Hallmann-Szelińska, E., Brydak, L.B. (2015). Incidence of Circulating Antibodies Against Hemagglutinin of Influenza Viruses in the Epidemic Season 2013/2014 in Poland. In: Pokorski, M. (eds) Pulmonary Infection. Advances in Experimental Medicine and Biology(), vol 857. Springer, Cham. https://doi.org/10.1007/5584_2015_118
Download citation
DOI: https://doi.org/10.1007/5584_2015_118
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-17457-0
Online ISBN: 978-3-319-17458-7
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)