Abstract
Objective: The objective of this study was to assess the cost effectiveness of using epoetin-α (erythropoietin) to augment preoperative autologous donation (PAD) of blood prior to elective cardiac surgery.
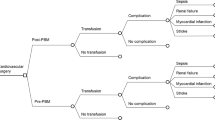
Design and setting: We designed a decision-analytic model incorporating the risk of receiving allogeneic blood, the costs of blood products, the likelihood of develo** transfusion-related diseases, the costs of transfusion-related diseases and their impact on life expectancy, and the effect of epoetin-α on the probability of transfusion.
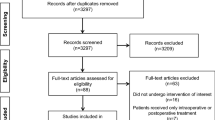
Interventions: The efficacy of epoetin-α was derived from data from a meta-analysis of published randomised trials comparing the use of epoetin-α to augment PAD with the use of PAD alone. Estimates for the other parameters were obtained by a systematic review of the literature.
Main outcome measures and results: The use of epoetin-α reduced the proportion of patients receiving allogeneic transfusions by 60% (from 31.6 to 12.7%). However, this led to only a modest benefit of 0.000035 life years gained per patient and an incremental cost per life year gained of $Can44.6 million (1998 Canadian dollars). A detailed sensitivity analysis confirmed that the cost-effectiveness ratio was larger than that which is generally considered acceptable.
Conclusions: Our study indicates that the use of epoetin-α to reduce perioperative allogeneic transfusions in cardiac surgery is not cost effective.





Similar content being viewed by others
References
Schreiber GB, Busch MP, Kleinman, et al. The risk of transfusion- transmitted viral infections. N Engl J Med 1996; 334: 1685–90
Lackritz EM, Satten GA, Aberle-Grasse J, et al. Estimated risk of transfusion of the human immunodeficiency virus by screened blood in the United States. N Engl J Med 1995; 333: 1721–5
Turner ML, Ironside JW. New-variant Creutzfeldt-Jakob disease: the risk of transmission by blood transfusion. Blood Rev 1998; 12: 255–68
Blajchman MA. Transfusion associated immunomodulation and universal white cell reduction: are we putting the cart before the horse? Transfusion 1999; 39: 665–70
Chiavetta JA, Herst R, Freedman J, et al. A survey of red cell use in 45 hospitals in central Ontario, Canada. Transfusion 1996; 35: 699–706
D’Ambra MN, Lynch KE, Boccagno MS, et al. The effect of perioperative administration of recombinant human erythropoietin (r-HuEPO) in CABG patients: a double blind, placebo- controlled study. Anesthesiology 1992; 77: 159
Sowade O, Warnke H, Sowade B, et al. Avoidance of homologous blood transfusion and increase of oxygen availability by preoperative epoetin beta therapy in patients undergoing coronary artery bypass grafting (CABG) [abstract]. Blood 1996; 86: 352a
Laupacis A, Fergusson D. Erythropoietin to minimize perioperative blood transfusion: a systematic review of randomized trials. Transfus Med 1998; 8: 309–17
Hayashi J, Kumon K, Takanashi S, et al. Subcutaneous administration of recombinant human erythropoietin before cardiac surgery: a double-blind, multicenter trial in Japan. Transfusion 1994; 34: 142–6
Kulier AH, Gombotz H, Fuchs G, et al. Subcutaneous recombinant human erythropoietin and autologous blood donation before coronary artery bypass surgery. Anesth Analg 1993; 76: 102–6
Schmoeckel M, Nollert G, Mempel M, et al. Effects of recombinant human erythropoietin on autologous blood donation before open heart surgery. Thorac Cardiovasc Surg 1993; 41: 364–8
Walpoth BH, Spirig P, Galliker B, et al. Erythropoietin and autologous blood donation in cardiac surgery. In: The role of epoetin alfa in surgery. Forging the link in blood conservation [monograph]. Macclesfield: Adelphi Communications, 1995
Watanabe Y, Fuse K, Naruse Y, et al. Subcutaneous use of erythropoietin in heart surgery. Ann Thorac Surg 1992; 54: 479–83
Fergusson D, VanWalraven C, Coyle D, et al. Economic evaluations of technologies to minimize perioperative transfusion: a systematic review of published studies. Transfus Med Rev 1999; 13: 106–17
Coyle D, Lee KM, Fergusson DA, et al. Economic analysis of erythropoietin use in orthopaedic surgery. Transfus Med 1999; 9: 21–30
Messmer K. Consensus statement: using epoetin alfa to decrease the risk of allogeneic blood transfusion in the surgical setting. Semin Hematol 1996; 33: 78–80
Tretiak R, Laupacis A, Riviere M, et al. Cost of allogeneic and autologous blood transfusion in Canada. Can Med Assoc J 1996; 154: 1501–8
Canadian Coordinating Office of Health Technology Assessment (CCOHTA). Guidelines for the economic evaluation of pharmaceuticals: Ottawa (ON): CCOHTA, 1997
Statistics Canada. Life tables, Canada and provinces 1990–1992. (Catalogue 84–537Occasional).Ottawa (ON): Statistics Canada
Gold M, Gafni A, Nelligan P, et al. Needle exchange programs: an economic evaluation of a local experience. Can Med Assoc J 1997; 157: 255–62
Huber TS, McGorray SP, Carlton LC, et al. Intraoperative autologous transfusion during elective infrarenal aortic reconstruction: a decision analysis model. J Vasc Surg 1997; 25: 984–94
Blood supply: transfusion-associated risks. Washington (DC): General Accounting Office, 1997
Krever H. Interim report of the commission of inquiry on the blood system in Canada. Ottawa (ON): Ministry of Supply and Services Canada, 1995
Etchason J, Petz L, Keeler E, et al. The cost effectiveness of preoperative autologous blood donations. N Engl J Med 1995; 332: 719–24
Healy JC, Frankforter SA, Graves BK, et al. Preoperative autologous blood donation in total-hip arthroplasty. Arch Pathol Lab Med 1994; 118: 465–70
Birkmeyer JD, Goodnough LT, AuBuchon JP et al. The cost-effectiveness of preoperative autologous blood donation for total hip and knee replacement. Transfusion 1993; 33: 544–51
Nelson KE, Donahue JG, Munoz A, et al. Transmission of retroviruses from seronegative donors by transfusion during cardiac surgery. Ann Intern Med 1992; 117: 554–9
Murphy PJ, Connery C, Hicks GL, et al. Homologous blood transfusion as a risk factor for post-operative infection after coronary artery bypass graft operations. J Thorac Cardiovasc Surg 1992; 104: 1092–9
Public service inter-agency guidelines for screening donors of blood, plasma, organs, tissues, and semen for evidence of hepatitis B and hepatitis C. MMWR Morbid Mortal Wkly Rep 1991; 40: 1–17
Donahue JD, Munoz A, Ness PM, et al. The declining risk of post-transfusion hepatitis C virus infection. N Engl J Med 1992; 327: 369–73
Linden JV, Kaplan HS. Transfusion errors: causes and effects. Transfus Med Rev 1994; 9: 169–83
Gibis B. Leukodepletion: an investigation into the techniques used, their effectiveness and costs. Ottawa (ON): Canadian Coordinating Office of Health Technology Assessment (CCOHTA), 1997
Brettle RP, Atkinson FI, Wilcock J, et al. The cost of health care for HIV-positive patients. Int J STD AIDS 1997; 8: 50–3
Gable CB, Tierce JC, Simison D, et al. Cost of HIV+/AIDS at CD4+ counts disease stages based on treatment protocols. J Acquir Immune Defic Human Retrovirol 1996; 12: 413–20
Petrou S, Dooley M, Whitaker L, et al. The economic costs of caring for people with HIV infection and AIDS in England and Wales. Pharmacoeconomics 1996; 9: 332–40
Brettle RP, Willock I, Cowan RM, et al. Inpatient health care utilization for patients with HIV and AIDS in Edinburgh city hospital. Int J STD AIDS 1994; 5: 194–201
Fortgang IS, Moore RD. Hospital admission of HIV-infected patients from 1988 to 1992 in Maryland. J Acquir Immune Defic Syndr Human Retrovirol 1995; 8: 365–72
Birkmeyer JD, AuBuchon JP, Littenberg B, et al. Cost-effectiveness of preoperative autologous donation in coronary artery bypass grafting. Ann Thorac Surg 1994; 57: 161–8
Hellinger FJ. The lifetime cost of treating a person with HIV. JAMA 1993; 270: 474–8
Andrulis DP, Weslowski VB, Hintz E, et al. Comparisons of hospital care for patients with AIDS and other HIV-related conditions. JAMA 1992; 267: 2482–6
Zowall H, Coupal L, Fraser RD, et al. Economic impact of HIV infection and coronary heart disease in immigrants to Canada. Can Med Assoc J 1992; 147: 1163–72
Andrews RM, Keyes MA, Fanning TR, et al. Lifetime medicaid service utilization and expenditures for AIDS in New York and California. J Acquir Immune Defic Syndr 1991; 4: 1046–58
Roberts WA, Kirkley SA, Newby M. A cost comparison of allogeneic and preoperatively or intraoperatively donated autologous blood. Anesth Analg 1996; 83: 129–33
Mah ET, Davis R, Seshadri P, et al. The role of autologous blood transfusion in joint replacement surgery. Anaesth Intensive Care 1995; 23: 472–7
Monk TG, Goodnough LT, Birkmeyer JD, et al. Acute normovolemic hemodilution us a cost-effective alternative to preoperative autologous blood donation by patients undergoing radical retropubic prostatectomy. Transfusion 1995; 35: 559–65
Scott WJ, Rode R, Castlemain B, et al. Efficacy, complications, and cost of comprehensive blood conservation program for cardiac operations. J Thorac Cardiovasc Surg 1992; 103: 1001–7
Solomon MD, Rutledge ML, Kane LE, et al. Cost comparison of intraoperative autologous versus homologous transfusion. Transfusion 1988; 28: 379–82
Elawad A, Benoni G, Montgomery F, et al. Cost effectiveness of blood substitution in elective orthopaedic operations. Acta Orthop Scand 1991; 62: 435–9
Laupacis A, Feeny D, Detsky AS, et al. How attractive does a new technology have to be to warrant adoption and utilization? Tentative guidelines for using clinical and economic evaluations. Can Med Assoc J 1992; 46: 473–81
The Trial to Reduce Alloimmunization to Platelets Study Group. Leukocyte reduction and ultraviolet B irradiation of platelets to prevent alloimmunization and refractoriness to platelet transfusions. N Engl J Med 1997; 337: 1861–9
Bowden RA, Sayers M, Newton B, et al. Cytomegalovirus immune globlin and seronegative blood products to prevent primary cytomegalovirus infection after marrow transplantation. N Engl J Med 1986; 314: 1006–10
Laupacis A, Fergusson D. Drugs to minimize peri-operative blood loss in cardiac surgery: meta analyses using peri-operative blood transfusion as the outcome. Anesth Analag 1997; 85: 1258–67
Bryson GL, Laupacis A, Wells G, et al. Does acute normovolemic hemodilution reduce perioperative allogeneic transfusion? A meta analysis. Anesth Analg 1998: 86: 9–15
Forgie M, Wells P, Laupacis A, et al. Pre-operative autologous donation decreases allogeneic transfusion but increases exposure to all red cell transfusion: results of a meta analysis. Arch Intern Med 1998; 158: 610–6
Rubens FD, Fergusson D, Wells PS, et al. Plateletpheresis in cardiac surgery: a meta analysis of the effect on transfusion requirements. J Cardiovasc Thorac Surg 1998; 116: 641–7
Huet C, Salmi LR, Fergusson D, et al. A meta-analysis of the effectiveness of cell salvage to minimize perioperative allogeneic blood transfusion in cardiac and orthopedic surgery. Anesth Analg 1999; 89: 861–9
Munoz JJ, Birkmeyer NJ, Birkmeyer JD, et al. Is epsilon-aminocaproic acid as effective as aprotinin in reducing bleeding with cardiac surgery? A meta-analysis. Circulation 1999; 99: 81–9
Levi M, Cromheecke ME, de Jonge E, et al. Pharmacological strategies to decrease excessive blood loss in cardiac surgery: a meta-analysis of clinically relevant endpoints. Lancet 1999; 354: 1940–7
Bennett-Guerrero E, Spillane WF, White WD, et al. Epsilon-aminocaproic acid administration and stroke following coronary artery bypass graft surgery. Ann Thorac Surg 1999; 67: 1283–7
Alderman EL, Levy JH, Rich JB, et al. Analyses of coronary graft patency after aprotinin use: results from the International Multicenter Aprotinin Graft Patency Experience (IMAGE) trial. J Thorac Cardiovasc Surg 1998; 116: 716–30
Westaby S, Katsumata T. Aprotinin and vein graft occlusion: the controversy continues. J Thorac Cardiovasc Surg 1998; 116: 731–3
McAlister FA, Clark HD, Wells PS, et al. Peri-operative allogeneic blood transfusions do not cause adverse sequelae in oncologic patients: a meta-analysis of unconfounded studies. Br J Surg 1998; 85: 171–8
Acknowledgements
Funding for this study was provided by the Canadian Coordinating Office of Health Technology Assessment (CCOHTA). We would like to acknowledge the following for providing reviews of the preliminary draft to CCOHTA: Dr D. Anderson, Dr S. Grover, Dr M. Krahn, Dr G. Paiement, Dr B. O’Brien and Dr N. Otten. We are also grateful to Dr J. Dupuis, S. Grimes and Dr B. Gibis for their assistance in providing data for this report.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Coyle, D., Lee, K.M., Fergusson, D.A. et al. Cost Effectiveness of Epoetin-α to Augment Preoperative Autologous Blood Donation in Elective Cardiac Surgery. Pharmacoeconomics 18, 161–171 (2000). https://doi.org/10.2165/00019053-200018020-00006
Published:
Issue Date:
DOI: https://doi.org/10.2165/00019053-200018020-00006