Abstract
Background
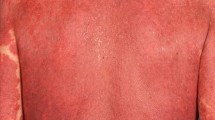
Pityriasis rubra pilaris (PRP) is an uncommon papulosquamous inflammatory disease of the skin, which may progress to erythroderma. The diagnosis is based on both clinical and histopathological findings. There are numerous treatment options in the literature, but often reported as unsuccessful.
Objectives
To summarize the therapy of type I PRP in a systematic manner.
Materials and methods
We performed a systematic search following the PRISMA Guidelines based on PubMed, Web of Science, and Medline databases using the term ‘pityriasis rubra pilaris treatment’ (in German and English) on human subjects, published between 1997 and 2017, documenting therapy for PRP type I. A total of 449 records were identified; 148 full-text articles were assessed for eligibility and 105 articles were included in the qualitative synthesis.
Results
We identified mainly individual case reports, a few retrospective studies, and small case series. No randomized controlled trials were found. Treatment options included topical and systemic agents, and physical modalities. Based on our review, we suggest a continuous topical treatment and, when appropriate, in combination with phototherapy. As first-line therapy, we recommend a retinoid, and as second-line, a combination of retinoid and methotrexate (considering the patient’s condition and side effects), azathioprine, or cyclosporine A. Biologicals can be used as third-line therapy. In case of treatment failure, biologicals can be combined with a retinoid, methotrexate, or cyclosporine A.
Conclusion
Randomized controlled clinical trials are needed in order to provide an evidence-based high-quality standardized treatment for patients with PRP type I.
Similar content being viewed by others
References
Wollina U. Pityriasis rubra pilaris. Hautarzt 2012; 63: 655–61.
Artik S, Kuhn A, Neumann NJ, Ruzicka T, Megahed M. Pityriasis rubra pilaris. Hautarzt 2004; 55: 980–3.
Karadag AS, Kavala M, Ozlu E, Ozkanli S, Zindanci I, Turkoglu Z. Erythrodermic pityriasis rubra pilaris: dramatic response to infliximab therapy. Indian J Dermatol Venereol Leprol 2016; 82: 112.
Stieler KM, Vogt A, Blume-Peytavi U. Erythematosquamous dermatoses in adolescence. Hautarzt 2016; 67: 293–7.
Albert MR, Mackool BT. Pityriasis rubra pilaris. Int J Dermatol 1999; 38: 1–11.
Griffiths WA. Pityriasis rubra pilaris. Clin Exp Dermatol 1980; 5: 105–12.
Ivanova K, Itin P, Haeusermann P. Pityriasis rubra pilaris: treatment with biologics — a new promising therapy? Dermatology 2012; 224: 120–5.
Ross NA, Chung HJ, Li Q, Andrews JP, Keller MS, Uitto J. Epidemiologic, clinicopathologic, diagnostic, and management challenges of pityriasis rubra pilaris: a case series of 100 patients. JAMA Dermatol 2016; 152: 670–5.
Mease PJ. Measures of psoriatic arthritis: Tender and Swollen Joint Assessment, Psoriasis Area and Severity Index (PASI), Nail Psoriasis Severity Index (NAPSI), Modified Nail Psoriasis Severity Index (mNAPSI), Mander/Newcastle Enthesitis Index (MEI), Leeds Enthesitis Index (LEI), Spondyloarthritis Research Consortium of Canada (SPARCC), Maastricht Ankylosing Spondylitis Enthesis Score (MASES), Leeds Dactylitis Index (LDI), Patient Global for Psoriatic Arthritis, Dermatology Life Quality Index (DLQI), Psoriatic Arthritis Quality of Life (PsAQOL), Functional Assessment of Chronic Illness Therapy-Fatigue (FACIT-F), Psoriatic Arthritis Response Criteria (PsARC), Psoriatic Arthritis Joint Activity Index (PsAJAI), Disease Activity in Psoriatic Arthritis (DAPSA), and Composite Psoriatic Disease Activity Index (CPDAI). Arthritis Care Res (Hoboken) 2011; 63: S64–85.
Wallace AD, Cidlowski JA. Proteasome-mediated glucocorticoid receptor degradation restricts transcriptional signaling by glucocorticoids. J Biol Chem 2001; 276: 42714–21.
Kimura T, Doi K. Dorsal skin reactions of hairless dogs to topical treatment with corticosteroids. Toxicol Pathol 1999; 27: 528–35.
Kolbe L, Kligman AM, Schreiner V, Stoudemayer T. Corticosteroid-induced atrophy and barrier impairment measured by non-invasive methods in human skin. Skin Res Technol 2001; 7: 73–7.
Luger T, Loske KD, Elsner P, et al. Topical skin therapy with glucocorticoids-therapeutic index. J Dtsch Dermatol Ges 2004; 2: 629–34.
Roos TC, Geuer S, Roos S, Brost H. Recent advances in treatment strategies for atopic dermatitis. Drugs 2004; 64: 2639–66.
Marrouche N, Kurban M, Kibbi AG, Abbas O. Pityriasis rubra pilaris: clinicopathological study of 32 cases from Lebanon. Int J Dermatol 2014; 53: 434–9.
Atanaskova Mesinkovska N, Dawes D, Sood A, Bergfeld W. Acantholytic pityriasis rubra pilaris associated with imiquimod 3.75% application. Case Rep Dermatol Med 2011; 2011: 412684.
Haenssle HA, Bertsch HP, Emmert S, Wolf C, Zutt M. Extracorporeal photochemotherapy for the treatment of exanthematic pityriasis rubra pilaris. Clin Exp Dermatol 2004; 29: 244–6.
Chapalain V, Beylot-Barry M, Doutre MS, Beylot C. Treatment of pityriasis rubra pilaris: a retrospective study of 14 patients. J Dermatol Treat 1999; 10: 113–7.
Gregoriou S, Argyriou G, Christofidou E, Vranou A, Rigopoulos D. Treatment of pityriasis rubra pilaris with pimecrolimus cream 1%. J Drugs Dermatol 2007; 6: 340–2.
Wadhwa B, Relhan V, Goel K, Kochhar AM, Garg VK. Vitamin D and skin diseases: a review. Indian J Dermatol Venereol Leprol 2015; 81: 344–55.
Thiers BH. The use of topical calcipotriene/calcipotriol in conditions other than plaque-type psoriasis. J Am Acad Dermatol 1997; 37: S69–71.
Van de Kerkhof PC, Steijlen PM. Topical treatment of pityriasis rubra pilaris with calcipotriol. Br J Dermatol 1994; 130: 675–8.
Nakafusa J, Misago N, Narisawa Y. Pityriasis rubra pilaris in association with polyarthritis. Dermatology 2002; 205: 298–300.
Vergilis-Kalner IJ, Mann DJ, Wasserman J, Petronic-Rosic V, Tsoukas MM. Pityriasis rubra pilaris sensitive to narrow band-ultraviolet B light therapy. J Drugs Dermatol 2009; 8: 270–3.
Zhang YH, Zhou Y, Ball N, Su MW, Xu JH, Zheng ZZ. Type I pityriasis rubra pilaris: upregulation of tumor necrosis factor alpha and response to adalimumab therapy. J Cutan Med Surg 2010; 14: 185–8.
Davis KF, Wu JJ, Murase JE, Rosenberg FR, Sorenson EP, Meshkinpour A. Clinical improvement of pityriasis rubra pilaris with combination etanercept and acitretin therapy. Arch Dermatol 2007; 143: 1597–9.
McGill A, Frank A, Emmett N, Turnbull DM, Birch-Machin MA, Reynolds NJ. The anti-psoriatic drug anthralin accumulates in keratinocyte mitochondria, dissipates mitochondrial membrane potential, and induces apoptosis through a pathway dependent on respiratory competent mitochondria. FASEB J 2005; 19: 1012–4.
Schmidt KN, Podda M, Packer L, Baeuerle PA. Anti-psoriatic drug anthralin activates transcription factor NF-kappa B in murine keratinocytes. J Immunol 1996; 156: 4514–9.
Sehgal VN, Verma P, Khurana A. Anthralin/dithranol in dermatology. Int J Dermatol 2014; 53: e449–60.
Amann PM, Susic M, Gluder F, Berger H, Krapf W, Loffler H. Alitretinoin (9-cis retinoic acid) is effective against pityriasis rubra pilaris: a retrospective clinical study. Acta Derm Venereol 2015; 95: 329–31.
Sakuma S, Higashi Y, Sato N, et al. Tacrolimus suppressed the production of cytokines involved in atopic dermatitis by direct stimulation of human PBMC system. (Comparison with steroids). Int Immunopharmacol 2001; 1: 1219–26.
Cury Martins J, Martins C, Aoki V, Gois AF, Ishii HA, da Silva EM. Topical tacrolimus for atopic dermatitis. Cochrane Database Syst Rev 2015; 7: CD009864.
Yang FC, Jessup C, Dahiya M, Reynolds R. Pityriasis rubra pilaris exacerbation with topical use of imiquimod. Int J Dermatol 2008; 47: 1076–8.
Davies M, Marks R. Studies on the effect of salicylic acid on normal skin. Br J Dermatol 1976; 95: 187–92.
Madan RK, Levitt J. A review of toxicity from topical salicylic acid preparations. J Am Acad Dermatol 2014; 70: 788–92.
Kneczke M, Rahm C, Landersjo L. The influence of salicylic acid on the in vitro release of anthralin from an o/w cream. Acta Pharm Nord 1990; 2: 313–8.
Taylor JR, Halprin KM. Percutaneous absorption of salicylic acid. Arch Dermatol 1975; 111: 740–3.
Lebwohl M. The role of salicylic acid in the treatment of psoriasis. Int J Dermatol 1999; 38: 16–24.
Franzotti AM, Avelar JC, Cardoso TA, Pires MC, Vidigal Mdo R. Pityriasis rubra pilar and hypothyroidism. An Bras Dermatol 2014; 89: 497–500.
Artik S, Megahed M, Ruzicka T. Pityriasis rubra pilaris. Case reports and review of the literature. Hautarzt 2003; 54: 858–63.
Usuki K, Sekiyama M, Shimada T, Shimada S, Kanzaki T. Three cases of pityriasis rubra pilaris successfully treated with cyclosporin A. Dermatology 2000; 200: 324–7.
Sauder DN. Immunomodulatory and pharmacologic properties of imiquimod. J Am Acad Dermatol 2000; 43: S6–11.
Gilliet M, Conrad C, Geiges M, et al. Psoriasis triggered by toll-like receptor 7 agonist imiquimod in the presence of dermal plasmacytoid dendritic cell precursors. Arch Dermatol 2004; 140: 1490–5.
Paganelli A, Ciardo S, Odorici G, Pellacani G, Conti A. Efficacy of ustekinumab after failure of infliximab CT-P13 in a HLA-Cw6-positive patient affected by pityriasis rubra pilaris: monitoring with reflectance confocal microscopy (RCM) and optical coherence tomography (OCT). J Eur Acad Dermatol Venereol 2017; 31: e249–51.
Gupta AK, Ellis CN, Nickoloff BJ, et al. Oral cyclosporine in the treatment of inflammatory and noninflammatory dermatoses. A clinical and immunopathologic analysis. Arch Dermatol 1990; 126: 339–50.
Malvezzi P, Rostaing L. The safety of calcineurin inhibitors for kidney-transplant patients. Expert Opin Drug Saf 2015; 14: 1531–46.
Nakayama J, Koga T, Furue M. Long-term efficacy and adverse event of nifedipine sustained-release tablets for cyclosporin A-induced hypertension in patients with psoriasis. Eur J Dermatol 1998; 8: 563–8.
Vujic I, Richter L, Bartsch K, Monshi B, Rappersberger K. Pityriasis rubra pilaris types 1 and 2: different responses to treatment with TNF-alpha antagonists. Eur J Dermatol 2013; 23: 895–6.
Hofer A, Mullegger R, Kerl H, Wolf P. Extracorporeal photochemotherapy for the treatment of erythrodermic pityriasis rubra pilaris. Arch Dermatol 1999; 135: 475–6.
Ohtsuki M, Okubo Y, Komine M, et al. Apremilast, an oral phosphodiesterase 4 inhibitor, in the treatment of Japanese patients with moderate to severe plaque psoriasis: efficacy, safety and tolerability results from a phase 2b randomized controlled trial. J Dermatol 2017; 44: 873–84.
Schafer PH, Parton A, Capone L, et al. Apremilast is a selective PDE4 inhibitor with regulatory effects on innate immunity. Cell Signal 2014; 26: 2016–29.
Krase IZ, Cavanaugh K, Curiel-Lewandrowski C. Treatment of refractory pityriasis rubra pilaris with novel phosphodiesterase 4 (PDE4) inhibitor apremilast. JAMA Dermatol 2016; 152: 348–50.
Molina-Figuera E, Gonzalez-Cantero A, Martinez-Lorenzo E, et al. Successful treatment of refractory type 1 pityriasis rubra pilaris with apremilast. J Cutan Med Surg 2018; 22: 104–5.
Maloney NJ, Hisaw LD, Worswick S. Refractory pityriasis rubra pilaris treated with etanercept, adalimumab, or ustekinumab: a retrospective investigation. Dermatol Ther 2017; 30: 6.
Litjens NH, Nibbering PH, Barrois AJ, et al. Beneficial effects of fumarate therapy in psoriasis vulgaris patients coincide with downregulation of type 1 cytokines. Br J Dermatol 2003; 148: 444–51.
Klein A, Coras B, Landthaler M, Babilas P. Off-label use of fumarate therapy for granulomatous and inflammatory skin diseases other than psoriasis vulgaris: a retrospective study. J Eur Acad Dermatol Venereol 2012; 26: 1400–6.
Xu J, Drew PD. 9-Cis-retinoic acid suppresses inflammatory responses of microglia and astrocytes. J Neuroimmunol 2006; 171: 135–44.
Stephensen CB, Rasooly R, Jiang X, et al. Vitamin A enhances in vitro Th2 development via retinoid X receptor pathway. J Immunol 2002; 168: 4495–503.
Ruzicka T, Lynde CW, Jemec GB, et al. Efficacy and safety of oral alitretinoin (9-cis retinoic acid) in patients with severe chronic hand eczema refractory to topical corticosteroids: results of a randomized, double-blind, placebo-controlled, multicentre trial. Br J Dermatol 2008; 158: 808–17.
Ellis CN, Pennes DR, Hermann RC, Blauvelt A, Martel W, Voorhees JJ. Long-term radiographic follow-up after isotretinoin therapy. J Am Acad Dermatol 1988; 18: 1252–61.
Ahn SY, Kim JH, Ahn SK, Oh YS. Clinical improvement of pityriasis rubra pilaris with antibiotic therapy. Eur J Dermatol 2011; 21: 106–7.
Popova L, Darlenski R, Tsankov N. Penicillin and vitamin A as possible therapeutic agents in pityriasis rubra pilaris. J Dtsch Dermatol Ges 2010; 8: 354–6.
Schmitt L, Inhoff O, Dippel E. Oral alitretinoin for the treatment of recalcitrant pityriasis rubra pilaris. Case Rep Dermatol 2011; 3: 85–8.
Clayton BD, Jorizzo JL, Hitchcock MG, et al. Adult pityriasis rubra pilaris: a 10-year case series. J Am Acad Dermatol 1997; 36: 959–64.
Huynh NT, Hunt MJ, Cachia AR, Veness MJ. Merkel cell carcinoma and multiple cutaneous squamous cell carcinomas in a patient with pityriasis rubra pilaris. Australas J Dermatol 2002; 43: 48–51.
Demonchy E, Lacour JP, Ortonne JP, Passeron T. Erythema gyratum repens, not always a bad omen for patients. J Eur Acad Dermatol Venereol 2010; 24: 738–9.
Abbott RA, Griffiths WA. Pityriasis rubra pilaris type 1 spontaneously resolving after 20 years. Clin Exp Dermatol 2009; 34: 378–9.
Byekova Y, Sami N. Successful response of refractory type I adult-onset pityriasis rubra pilaris with ustekinumab and acitretin combination therapy. J Dermatol 2015; 42: 830–1.
Eastham AB, Femia AN, Qureshi A, Vleugels RA. Treatment options for pityriasis rubra pilaris including biologic agents: a retrospective analysis from an academic medical center. JAMA Dermatol 2014; 150: 92–4.
Liu PY, Prete PE. Arthritis associated with pityriasis rubra pilaris. BMJ Case Rep 2010; 2010.
Selvaag E, Haedersdal M, Thomsen K. Pityriasis rubra pilaris: a retrospective study of 12 patients. J Eur Acad Dermatol Venereol 2000; 14: 514–5.
Ga**ov ZT, Matic MB, Duran VD, Vuckovic N, Prcic ST, Vujanovic LM. Drug-related pityriasis rubra pilaris with acantholysis. Vojnosanit Pregl 2013; 70: 871–3.
Battistella M, Pages C, Demongeot C, Cavelier-Balloy B, Bagot M, Viguier M. Pityriasis rubra pilaris with prominent acantholytic dyskeratosis. Eur J Dermatol 2011; 21: 796–7.
Gemmeke A, Schonlebe J, Koch A, Wollina U. Pityriasis rubra pilaris-a retrospective single center analysis over eight years. J Dtsch Dermatol Ges 2010; 8: 43944.
Genereux AD, Wetter DA. Widespread erythematous skin eruption. J Fam Pract 2017; 66: 181–3.
Schuster D, Pfister-Wartha A, Bruckner-Tuderman L, Schempp CM. Successful treatment of refractory pityriasis rubra pilaris with secukinumab. JAMA Dermatol 2016; 152: 1278–80.
Kim BR, Chae JB, Park JT, Byun SY, Youn SW. Clinical remission of pityriasis rubra pilaris with adalimumab in an adolescent patient. J Dermatol 2015; 42: 1122–3.
Chowdhary M, Davila U, Cohen DJ. Ustekinumab as an alternative treatment option for chronic pityriasis rubra pilaris. Case Rep Dermatol 2015; 7: 46–50.
Vogel AS, Marsch WC, Taube KM, Kreft B. Successful treatment of a therapy resistant pityriasis rubra pilaris with etanercept. J Der Deutschen Dermatologischen Gesellschaft 2015; 13: 150.
Mattox AR, Chappell JA, Hurley MY. New-onset vitiligo during long-term, stable infliximab treatment of pityriasis rubra pilaris. J Drugs Dermatol 2013; 12: 217–9.
Zirbs M, Kigitsidou E, Seifert F, Ring J, Brockow K. Successful treatment with infliximab despite positive tuberculosis ELISpot results in a patient with pityriasis rubra pilaris taking prophylactic isoniazid. Clin Exp Dermatol 2011; 36: 808–9.
Di Stefani A, Galluzzo M, Talamonti M, Chiricozzi A, Costanzo A, Chimenti S. Long-term ustekinumab treatment for refractory type I pityriasis rubra pilaris. J Dermatol Case Rep 2013; 7: 5–9.
Conde-Taboada A, Fueyo A, Lopez-Bran E, Pedraz J, Campos L. Treatment of refractory pityriasis rubra pilaris with etanercept. J Am Acad Dermatol 2013; 68: AB216.
Sehgal VN, Srivastava G, Aggarwal AK, Sardana K, Jain M. Efficacy of isotretinoin in pityriasis rubra pilaris: unapproved use. Int J Dermatol 2006; 45: 123840.
White KL. Pityriasis rubra pilaris. Dermatol Online J 2003; 9: 6.
Guedes R, Leite L. Therapeutic hotline. Treatment of pityriasis rubra pilaris with etanercept. Dermatol Ther 2011; 24: 285–6.
Conaghan PG, Sommer S, McGonagle D, et al. The relationship between pityriasis rubra pilaris and inflammatory arthritis: case report and response of the arthritis to anti-tumor necrosis factor immunotherapy. Arthritis Rheum 1999; 42: 1998–2001.
Feldmeyer L, Mylonas A, Demaria O, et al. Interleukin 23-helper T cell 17 axis as a treatment target for pityriasis rubra pilaris. JAMA Dermatol 2017; 153: 304–8.
Wohlrab J, Kreft B. Treatment of pityriasis rubra pilaris with ustekinumab. Br J Dermatol 2010; 163: 655–6.
Marotte H, Cimaz R. Etanercept-TNF receptor and IgG1 Fc fusion protein: is it different from other TNF blockers? Expert Opin Biol Ther 2014; 14: 569–72.
Adnot-Desanlis L, Antonicelli F, Tabary T, Bernard P, Reguiai Z. Effectiveness of infliximab in pityriasis rubra pilaris is associated with pro-inflammatory cytokine inhibition. Dermatology 2013; 226: 41–6.
Garcovich S, Di Giampetruzzi AR, Antonelli G, Garcovich A, Didona B. Treatment of refractory adult-onset pityriasis rubra pilaris with TNF-alpha antagonists: a case series. J Eur Acad Dermatol Venereol 2010; 24: 881–4.
Liao WC, Mutasim DF. Infliximab for the treatment of adult-onset pityriasis rubra pilaris. Arch Dermatol 2005; 141: 423–5.
Humme D, Beyer M, Rowert-Huber HJ, Sterry W, Philipp S. CD30-positive anaplastic large cell T-cell lymphoma develo** during immunosuppressive therapy of pityriasis rubra pilaris with ustekinumab. Hautarzt 2013; 64: 1904.
Maloney NJ, Hisaw LD, Worswick S. Type I pityriasis rubra pilaris treated with tumor necrosis factor inhibitors, ustekinumab, or secukinumab: a review. J Am Acad Dermatol 2018; 79: 585–7.
Sinha A, Natarajan S. Efalizumab for the treatment of pityriasis rubra pilaris: experience in three patients. Br J Dermatol 2009; 161: 15.
Heibel MD, Heibel HD. Successful treatment of type I pityriasis rubra pilaris with ixekizumab. JAAD Case Rep 2018; 4: 774–6.
Fitz S, Longley BJ, Puchalsky D. Treatment of pityriasis rubra pilaris with ustekinumab. J Am Acad Dermatol 2013; 68: AB216.
Chiu HY, Tsai TF. Pityriasis rubra pilaris with polyarthritis treated with adalimumab. J Am Acad Dermatol 2013; 68: 187–8.
Hueber W, Patel DD, Dryja T, et al. Effects of AIN457, a fully human antibody to interleukin-17A, on psoriasis, rheumatoid arthritis, and uveitis. Sci Transl Med 2010; 2: 52ra72.
Liu L, Lu J, Allan BW, et al. Generation and characterization of ixekizumab, a humanized monoclonal antibody that neutralizes interleukin-17A. J Inflamm Res 2016; 9: 39–50.
Bonomo L, Levitt JO. Secukinumab emerges as a rapidly effective therapy for pityriasis rubra pilaris. Cutis 2018; 101: 367–9.
Kim J, Krueger JG. The immunopathogenesis of psoriasis. Dermatol Clin 2015; 33: 13–23.
Hanfstingl K, Pekar-Lukacs A, Motz R, Guenova E, Hoetzenecker W. Successful treatment of pityriasis rubra pilaris with ixekizumab. Case Rep Dermatol 2018; 10: 97–100.
Tzu J, Kerdel F. From conventional to cutting edge: the new era of biologics in treatment of psoriasis. Dermatol Ther 2008; 21: 131–41.
Jullien D, Prinz JC, Langley RG, et al. T-cell modulation for the treatment of chronic plaque psoriasis with efalizumab (Raptiva): mechanisms of action. Dermatology 2004; 208: 297–306.
Lin EJ, Reddy S, Shah VV, Wu JJ. A review of neurologic complications of biologic therapy in plaque psoriasis. Cutis 2018; 101: 57–60.
Lotsikas-Baggili AJ, Kupiec-Banasikowska A, Kauffman CL. Efalizumab treatment of a case of pityriasis rubra pilaris (PRP). J Am Acad Dermatol 2007; 56: Ab189–Ab.
Nunemacher KJ. Advocacy and hope for the patient with pityriasis rubra pilaris. Dermatol Nurs 2008; 20: 375–7.
Klein A, Szeimies RM, Landthaler M, Karrer S. Exacerbation of pityriasis rubra pilaris under efalizumab therapy. Dermatology 2007; 215: 72–5.
Nanau RM, Cohen LE, Neuman MG. Risk of infections of biological therapies with accent on inflammatory bowel disease. J Pharm Pharm Sci 2014; 17: 485–531.
Lebwohl M, Bagel J, Gelfand JM, et al. From the Medical Board of the National Psoriasis Foundation: monitoring and vaccinations in patients treated with biologics for psoriasis. J Am Acad Dermatol 2008; 58: 94–105.
Goodman TA, Polisson RP. Methotrexate: adverse reactions and major toxicities. Rheum Dis Clin North Am 1994; 20: 513–28.
Raaby L, Zachariae C, Ostensen M, et al. Methotrexate use and monitoring in patients with psoriasis: a consensus report based on a Danish expert meeting. Acta Derm Venereol 2017; 97: 426–32.
Duncan KO, Imaeda S, Milstone LM. Pneumocystis carinii pneumonia complicating methotrexate treatment of pityriasis rubra pilaris. J Am Acad Dermatol 1998; 39: 276–8.
Gul U, Gonul M, Kilic A, et al. A case of pityriasis rubra pilaris associated with sacroileitis and autoimmune thyroiditis. J Eur Acad Dermatol Venereol 2008; 22: 889–90.
Iredale HE, Meggitt SJ. Photosensitive pityriasis rubra pilaris. Clin Exp Dermatol 2006; 31: 36–8.
Lister RK, Perry JD, Cerio R. Pityriasis rubra pilaris and a seronegative polyarthritis. Br J Dermatol 1997; 137: 318–9.
Durairaj VD, Horsley MB. Resolution of pityriasis rubra pilaris-induced cicatricial ectropion with systemic low-dose methotrexate. Am J Ophthalmol 2007; 143: 709–10.
Marchetti MA, Greer KE. Pityriasis rubra pilaris treated with methotrexate resolving with an erythema gyratum repens-like appearance. J Am Acad Dermatol 2013; 69: e32–3.
Lin CY, Maurice PD, Cross NB. A case of pityriasis rubra pilaris associated with membranous nephropathy. Australas J Dermatol 2013; 54: e1–3.
Wassef C, Lombardi A, Rao BK. Adalimumab for the treatment of pityriasis rubra pilaris: a case report. Cutis 2012; 90: 244–7.
Varma S, Logan RA. Exanthematic pityriasis rubra pilaris. Br J Dermatol 1999; 141: 769–71.
Schreml S, Zeller V, Babilas P, Karrer S, Landthaler M, Szeimies RM. Pityriasis rubra pilaris successfully treated with adalimumab. Clin Exp Dermatol 2010; 35: 792–3.
Abikhair M, Roberts H. Successful treatment of erythrodermic pityriasis rubra pilaris with adalimumab: a case study. Austr J Dermatol 2013; 54: 9.
O’Kane D, Devereux CE, Walsh MY, Hoey SE. Rapid and sustained remission of pityriasis rubra pilaris with adalimumab treatment. Clin Exp Dermatol 2010; 35: e155–6.
Barth D, Harth W, Treudler R, Simon JC. Successful treatment of pityriasis rubra pilaris (type 1) under combination of infliximab and methotrexate. J Dtsch Dermatol Ges 2009; 7: 1071–4.
Blanes M, Amador C, Selles I, Massa B. Treatment with infliximab of pityriasis rubra pilaris refractary to conventional therapy in a patient with concurrent chronic hepatitis B viral infection. J Am Acad Dermatol 2007; 56: AB178.
Manoharan S, White S, Gumparthy K. Successful treatment of type I adult-onset pityriasis rubra pilaris with infliximab. Australas J Dermatol 2006; 47: 124–9.
Roberts RL, Barclay ML. Current relevance of pharmacogenetics in immunomodulation treatment for Crohn’s disease. J Gastroenterol Hepatol 2012; 27: 1546–54.
Schutz E, Gummert J, Mohr F, Oellerich M. Azathioprine-induced myelosuppression in thiopurine methyltransferase deficient heart transplant recipient. Lancet 1993; 341: 436.
McCoy LS, **e Y, Tor Y. Antibiotics that target protein synthesis. Wiley Interdiscip Rev RNA 2011; 2: 209–32.
Keeney KM, Yurist-Doutsch S, Arrieta MC, Finlay BB. Effects of antibiotics on human microbiota and subsequent disease. Annu Rev Microbiol 2014; 68: 217–35.
Sebastian A, Koff AB, Goldberg LJ. PRP with subcorneal acantholysis: case report and review. J Cutan Pathol 2010; 37: 99–101.
Buttgereit F, Saag KG, Cutolo M, da Silva JA, Bijlsma JW. The molecular basis for the effectiveness, toxicity, and resistance to glucocorticoids: focus on the treatment of rheumatoid arthritis. Scand J Rheumatol 2005; 34: 14–21.
Ruiz-Irastorza G, Danza A, Khamashta M. Glucocorticoid use and abuse in SLE. Rheumatology (Oxford) 2012; 51: 1145–53.
Da Silva JA, Jacobs JW, Kirwan JR, et al. Safety of low dose glucocorticoid treatment in rheumatoid arthritis: published evidence and prospective trial data. Ann Rheum Dis 2006; 6: 285–93.
Doran MF, Crowson CS, Pond GR, O’Fallon WM, Gabriel SE. Predictors of infection in rheumatoid arthritis. Arthritis Rheum 2002; 46: 2294–300.
Gurwitz JH, Field TS, Glynn RJ, et al. Risk factors for non-insulin-dependent diabetes mellitus requiring treatment in the elderly. J Am Geriatr Soc 1994; 42: 1235–40.
Berlin JM, Goldberg SM. A rash on the legs and palms. Cleve Clin J Med 2010; 77: 294–5.
Lu R, George SJ, Hsu S. Pityriasis rubra pilaris: failure of combination treatment with acitretin and infliximab. Dermatol Online J 2006; 12: 18.
Kaskel P, Grundmann-Kollmann M, Schiller PI, et al. Bath-PUVA as a treatment for Pityriasis rubra pilaris provoked by ultraviolet B. Br J Dermatol 1999; 140: 769–70.
Frikha F, Frigui M, Masmoudi H, Turki H, Bahloul Z. Systemic sclerosis in a patient with pityriasis rubra pilaris. Pan Afr Med J 2010; 6: 6.
Lopez-Ferrer A, Dalmau J, Fernandez-Figueras MT, Puig L. Pityriasis rubra pilaris triggered by photodynamic therapy with response to tumor necrosis factor alpha-blocking agents and acitretin. Cutis 2014; 93: E6–7.
Ling TC, Clayton TH, Crawley J, et al. British Association of Dermatologists and British Photodermatology Group guidelines for the safe and effective use of psoralen-ultraviolet A therapy 2015. Br J Dermatol 2016; 174: 24–55.
Foerster J, Boswell K, West J, et al. Narrowband UVB treatment is highly effective and causes a strong reduction in the use of steroid and other creams in psoriasis patients in clinical practice. PLoS One 2017; 12: e0181813.
Ullrich SE. Does exposure to UV radiation induce a shift to a Th-2-like immune reaction? Photochem Photobiol 1996; 64: 254–8.
Ibbotson SH. A perspective on the use of NB-UVB phototherapy vs. PUVA photochemotherapy. Front Med (Lausanne) 2018; 5: 184.
Stern RS, Laird N. The carcinogenic risk of treatments for severe psoriasis. Photochemotherapy follow-up study. Cancer 1994; 73: 2759–64.
Kawara S, Miyake M, Oiso N, Kawada A. Pityriasis rubra pilaris with preceding cytomegalovirus infection. Dermatology 2009; 219: 350–2.
Buss Y, Folster-Holst R. Erythematous, acrally prominent plaques in a 66-year-old woman. JDtsch Dermatol Ges 2004; 2: 871–3.
Neess CM, Hinrichs R, Dissemond J, et al. Treatment of pruritus by capsaicin in a patient with pityriasis rubra pilaris receiving RE-PUVA therapy. Clin Exp Dermatol 2000; 25: 209–11.
Dippel E, Schrag H, Goerdt S, Orfanos CE. Extracorporeal photopheresis and interferon-alpha in advanced cutaneous T-cell lymphoma. Lancet 1997; 350: 32–3.
Zic J, Arzubiaga C, Salhany KE, et al. Extracorporeal photopheresis for the treatment of cutaneous T-cell lymphoma. J Am Acad Dermatol 1992; 27: 729–36.
Greinix HT, Volc-Platzer B, Rabitsch W, et al. Successful use of extracorporeal photochemotherapy in the treatment of severe acute and chronic graft-versus-host disease. Blood 1998; 92: 3098–104.
Klein A, Landthaler M, Karrer S. Pityriasis rubra pilaris: a review of diagnosis and treatment. Am J Clin Dermatol 2010; 11: 157–70.
Bravo EA, Carrion L, Paucar SM, Mendoza R, Rivera C. Successful treatment of pityriasis rubra pilaris with adalimumab — case report. Dermatol Online J 2014; 20: 22374.
Herbst RA, Vogelbruch M, Ehnis A, Kiehl P, Kapp A, Weiss J. Combined ultraviolet A1 radiation and acitretin therapy as a treatment option for pityriasis rubra pilaris. Br J Dermatol 2000; 142: 574–5.
Napolitano M, Lembo L, Fania L, Abeni D, Didona D, Didona B. Ustekinumab treatment of pityriasis rubra pilaris: a report of five cases. J Dermatol 2018; 45: 202–6.
Aragon-Miguel R, Prieto-Barrios M, Calleja-Algarra A, et al. Refractory pityriasis rubra pilaris with good response after treatment with ustekinumab. J Dtsch Dermatol Ges 2018; 16: 1022–5.
Koch L, Schoffl C, Aberer W, Massone C. Methotrexate treatment for pityriasis rubra pilaris: a case series and literature review. Acta Derm Venereol 2018; 98: 501–5.
Molin S, Ruzicka T. Treatment of refractory pityriasis rubra pilaris with oral alitretinoin: case report. Br J Dermatol 2010; 163: 221–3.
Author information
Authors and Affiliations
Corresponding author
Additional information
Disclosure. Financial support: none. Conflicts of interest: none.
Supplementary data
About this article
Cite this article
Engelmann, C., Elsner, P. & Miguel, D. Treatment of pityriasis rubra pilaris type I: a systematic review. Eur J Dermatol 29, 524–537 (2019). https://doi.org/10.1684/ejd.2019.3641
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1684/ejd.2019.3641