Abstract
Background
There is a group of hypopharyngeal squamous cell carcinoma (HPSCC) patients for whom larynx-preserving open partial pharyngectomy (PP) and radiotherapy/chemoradiotherapy (RT/CRT) are indicated. We aimed to retrospectively evaluate the survival difference as there is no evidence directly comparing the two therapies.
Methods
This study evaluated HPSCC patients who were initially treated by PP or RT/CRT at our institution between January 2007 and October 2019. Overall survival (OS), disease-specific survival (DSS), laryngectomy-free survival (LFS), and local relapse-free survival (LRFS) were evaluated. The main analyses were performed with inverse probability of treatment weighting (IPTW) adjustments. Sensitivity analyses compared hazard ratios (HRs) obtained with three models: unadjusted, multivariate Cox regression, and propensity score-adjusted.
Results
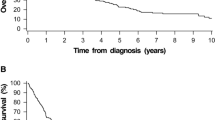
Overall, 198 patients were enrolled; 63 and 135 underwent PP and RT/CRT, respectively. IPTW-adjusted 5-year OS, DSS, LFS, and LRFS rates in the PP and RT/CRT groups were 84.3% and 61.9% (p = 0.019), 84.9% and 75.8% (p = 0.168), 94.8% and 90.0% (p = 0.010), and 75.9% and 74.1% (p = 0.789), respectively. In the IPTW-adjusted regression analysis, PP was associated with a significant benefit regarding OS (HR 0.48, 95% confidence interval [CI] 0.26–0.90) and LFS (HR 0.17, 95% CI 0.04–0.77). The results obtained with the three models in the sensitivity analyses were qualitatively similar to those of the IPTW-adjusted models.
Conclusion
Despite the risk of bias related to unadjusted factors, our results suggest that PP is associated with significantly better OS and LFS compared with RT/CRT for HPSCC.


Similar content being viewed by others
References
Japan Society for Head and Neck Cancer Registry Committee. Report of Head and Neck Cancer Registry of Japan Clinical Statistics of Registered Patients, 2019. 2019. Available at: http://www.jshnc.umin.ne.jp/pdf/HNCreport_2019.pdf. Accessed 16 Aug 2022.
Forastiere AA, Zhang Q, Weber RS, et al. Long-term results of RTOG 91–11: a comparison of three nonsurgical treatment strategies to preserve the larynx in patients with locally advanced larynx cancer. J Clin Oncol. 2013;31(7):845–52.
McDowell LJ, Rock K, Xu W, et al. Long-term late toxicity, quality of life, and emotional distress in patients with nasopharyngeal carcinoma treated with intensity modulated radiation therapy. Int J Radiat Oncol Biol Phys. 2018;102(2):340–52.
Omura G, Saito Y, Ando M, et al. Salvage surgery for local residual or recurrent pharyngeal cancer after radiotherapy or chemoradiotherapy. Laryngoscope. 2014;124(9):2075–80.
Ogura JH, Marks JE, Freeman RB. Results of conservation surgery for cancers of the supraglottis and pyriform sinus. Laryngoscope. 1980;90(4):591–600.
Chevalier D, Watelet JB, Darras JA, Piquet JJ. Supraglottic hemilaryngopharyngectomy plus radiation for the treatment of early lateral margin and pyriform sinus carcinoma. Head Neck. 1997;19(1):1–5.
Makeieff M, Mercante G, Jouzdani E, Garrel R, Crampette L, Guerrier B. Supraglottic hemipharyngolaryngectomy for the treatment of T1 and T2 carcinomas of laryngeal margin and piriform sinus. Head Neck. 2004;26(8):701–5.
Plouin-Gaudon I, Lengele B, Desuter G, et al. Conservation laryngeal surgery for selected pyriform sinus cancer. Eur J Surg Oncol. 2004;30(10):1123–30.
Laccourreye O, Merite-Drancy A, Brasnu D, et al. Supracricoid hemilaryngopharyngectomy in selected pyriform sinus carcinoma staged as T2. Laryngoscope. 1993;103(12):1373–9.
Bradley PJ, Liu L. Open-neck organ preservation surgery for hypopharyngeal cancer: indications, techniques, limits, and outcomes. Curr Opin Otolaryngol Head Neck Surg. 2019;27(2):123–9.
Takes RP, Strojan P, Silver CE, et al. Current trends in initial management of hypopharyngeal cancer: the declining use of open surgery. Head Neck. 2012;34(2):270–81.
Hirano S, Tateya I, Kitamura M, et al. Organ preservation surgery for advanced hypopharyngeal cancer. Acta Otolaryngol Suppl. 2010;563:50–5.
Chan JY, Wei WI. Current management strategy of hypopharyngeal carcinoma. Auris Nasus Larynx. 2013;40(1):2–6.
Shinozaki T, Hayashi R, Okano W, Tomioka T, Higashino T. Treatment results of 99 patients undergoing open partial hypopharyngectomy with larynx preservation. Jpn J Clin Oncol. 2019;49(10):919–23.
Tateya I, Shiotani A, Satou Y, et al. Transoral surgery for laryngo-pharyngeal cancer—the paradigm shift of the head and cancer treatment. Auris Nasus Larynx. 2016;43(1):21–32.
Holsinger FC, Ferris RL. Transoral endoscopic head and neck surgery and its role within the multidisciplinary treatment paradigm of oropharynx cancer: robotics, lasers, and clinical trials. J Clin Oncol. 2015;33(29):3285–92.
Eguchi K, Matsui T, Mukai M, Sugimoto T. Prediction of the depth of invasion in superficial pharyngeal cancer: microvessel morphological evaluation with narrowband imaging. Head Neck. 2019;41(11):3970–5.
Kikuchi D, Iizuka T, Yamada A, et al. Utility of magnifying endoscopy with narrow band imaging in determining the invasion depth of superficial pharyngeal cancer. Head Neck. 2015;37(6):846–50.
Tateya I, Morita S, Muto M, et al. Magnifying endoscope with NBI to predict the depth of invasion in laryngo-pharyngeal cancer. Laryngoscope. 2015;125(5):1124–9.
National Comprehensive Cancer Network. The NCCN Clinical Practice Guidelines in Oncology Head and Neck Cancers (Version 2). Published 20 December 2022. Available at: https://www.nccn.org/professionals/physician_gls/pdf/head-and-neck.pdf. Accessed 11 Dec 2022.
Murakami N, Matsumoto F, Yoshimoto S, et al. Patterns of recurrence after selective postoperative radiation therapy for patients with head and neck squamous cell carcinoma. BMC Cancer. 2016;16:192.
Murakami N, Yoshimoto S, Matsumoto F, et al. Severe gastrointestinal bleeding in patients with locally advanced head and neck squamous cell carcinoma treated by concurrent radiotherapy and Cetuximab. J Cancer Res Clin Oncol. 2015;141(1):177–84.
Rosenbaum PR, Rubin DB. The central role of the propensity score in observational studies for causal effects. Biometrika. 1983;70(1):41–55.
Austin PC. The use of propensity score methods with survival or time-to-event outcomes: reporting measures of effect similar to those used in randomized experiments. Stat Med. 2014;33(7):1242–58.
Cole SR, Hernan MA. Adjusted survival curves with inverse probability weights. Comput Methods Programs Biomed. 2004;7(1):45–9.
Robins JM, Hernán MA, Brumback B. Marginal structural models and causal inference in epidemiology. Epidemiology. 2000;11(5):550–60.
Kanda Y. Investigation of the freely available easy-to-use software ‘EZR’ for medical statistics. Bone Marrow Transplant. 2013;48(3):452–8.
Din HA, Zhan KY, Boling C, Nguyen S, Lentsch EJ. Predictors of survival in posterior cricoid squamous cell carcinoma: a study of 248 cases. Laryngoscope. 2017;127(5):1093–6.
Kadapa N, Mangale K, Watve P, Rao SLM, Raju AK, Subramanyeshwar Rao T. Postcricoid carcinoma: Is organ preservation justified in T3? Laryngoscope. 2015;125(2):356–9.
Grant DG, Salassa JR, Hinni ML, Pearson BW, Hayden RE, Perry WC. Transoral laser microsurgery for recurrent laryngeal and pharyngeal cancer. Otolaryngol Head Neck Surg. 2008;138(5):606–13.
Timmermans AJ, van Harten MC, Remmelts AJ, et al. Complications after transoral excision in previously irradiated head and neck cancer patients: our experience in a retrospective cohort study of fifty-two patients. Clin Otolaryngol. 2014;39(4):245–51.
Tomifuji M, Araki K, Yamashita T, Shiotani A. Salvage transoral videolaryngoscopic surgery for radiorecurrent hypopharyngeal and supraglottic cancer. Auris Nasus Larynx. 2017;44(4):464–71.
Asakage T, Yokoyama A, Haneda T, et al. Genetic polymorphisms of alcohol and aldehyde dehydrogenases, and drinking, smoking and diet in Japanese men with oral and pharyngeal squamous cell carcinoma. Carcinogenesis. 2007;28(4):865–74.
Pignon JP, Bourhis J, Domenge C, Designé L. Chemotherapy added to locoregional treatment for head and neck squamous-cell carcinoma: three meta-analyses of updated individual data. MACH-NC Collaborative Group. Meta-analysis of chemotherapy on head and neck cancer. Lancet. 2000;355(9208):949–55.
Acknowledgment
This work was supported by the Japan Society for the Promotion of Science (JSPS) KAKENHI Grant Number 21K16849. The authors thank Jane Charbonneau, DVM, from Edanz (https://jp.edanz.com/ac), for editing a draft of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Eguchi, K., Omura, G., Murakami, N. et al. Comparison of Survival Outcomes Between Larynx-Preserving Open Partial Pharyngectomy and Radiotherapy or Chemoradiotherapy in Patients with Hypopharyngeal Squamous Cell Carcinoma: A Single-Center Retrospective Analysis with Inverse Probability of Treatment Weighting Adjustments. Ann Surg Oncol 30, 6867–6874 (2023). https://doi.org/10.1245/s10434-023-13934-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-023-13934-1