Abstract
Background
The optimal management of patients with stage IV soft tissue sarcoma of the extremity (STSE) with distant metastases at diagnosis is unclear due to limited evidence and heterogeneity of current practice patterns. National guidelines have recommended surgical management of the primary site (SP) with or without radiotherapy (R), chemotherapy (C), and metastasectomy (M).
Methods
In the National Cancer Database (NCDB), patients with initially metastatic STSE who received definitive SP from 2004 to 2014 were identified. Survival distributions were estimated and compared using the Kaplan–Meier method and log-rank tests, and covariates were compared using Chi-square tests or analysis of variance (ANOVA). Propensity score analysis using inverse probability of treatment weighting was used.
Results
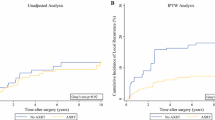
Overall, 1124 patients were included, with a median age of 55 years (range 18–90). Utilization of SP+M increased over time from 18.8% in 2004–2006, to 33.3% in 2007–2009, to 47.9% in 2010–2014 (p = 0.024). The addition of M to SP was associated with superior 5-year overall survival (OS) at 30.8% (SP+M+/−C+/−R) compared with 18.2% for those treated with non-surgical adjuvant therapies (SP+/−C+/−R) and 12.6% for SP alone (p < 0.0001). Positive surgical margins were noted in 24.1% of patients and was associated with worse OS (hazard ratio 1.44, p < 0.001) on multivariable analysis.
Conclusions
This is the first known study utilizing a large database to explore practice patterns and outcomes for patients with metastatic STSE receiving definitive SP. Utilization of metastasectomy increased in the study period and was associated with longer survival compared with SP alone. These hypothesis-generating data warrant additional study.



Similar content being viewed by others
References
Siegel RL, Miller KD, Jemal A. Cancer statistics, 2018. CA Cancer J Clin. 2018;68(1):7–30. https://doi.org/10.3322/caac.21442.
von Mehren M, Kane JM, Bui MM, et al. Soft tissue sarcoma, Version 1.2021: featured updates to the NCCN guidelines. J Natl Compr Cancer Netw. 2020;18(12):1605–12. https://doi.org/10.6004/JNCCN.2020.0058.
Yang JC, Chang AE, Baker AR, et al. Randomized prospective study of the benefit of adjuvant radiation therapy in the treatment of soft tissue sarcomas of the extremity. J Clin Oncol. 1998;16(1):197–203. https://doi.org/10.1200/JCO.1998.16.1.197.
O’Sullivan B, Davis AM, Turcotte R, et al. Preoperative versus postoperative radiotherapy in soft-tissue sarcoma of the limbs: a randomised trial. Lancet. 2002;359(9325):2235–41. https://doi.org/10.1016/S0140-6736(02)09292-9.
Koshy M, Rich SE, Mohiuddin MM. Improved survival with radiation therapy in high-grade soft tissue sarcomas of the extremities: a SEER analysis. Int J Radiat Oncol Biol Phys. 2010;77(1):203–9. https://doi.org/10.1016/j.ijrobp.2009.04.051.
Kachare SD, Brinkley J, Vohra NA, Zervos EE, Wong JH, Fitzgerald TL. Radiotherapy associated with improved survival for high-grade sarcoma of the extremity. J Surg Oncol. 2015;4:338–43.
Ramey SJ, Yechieli R, Zhao W, et al. Limb-sparing surgery plus radiotherapy results in superior survival: an analysis of patients with high-grade, extremity soft-tissue sarcoma from the NCDB and SEER. Cancer Med. 2018;7(9):4228–39. https://doi.org/10.1002/cam4.1625.
Casali PG, Abecassis N, Bauer S, et al. Soft tissue and visceral sarcomas: ESMO-EURACAN Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann Oncol. 2018;29(Suppl 4):iv51–67. https://doi.org/10.1093/annonc/mdy096.
Kraybill WG, Harris J, Spiro IJ, et al. Phase II study of neoadjuvant chemotherapy and radiation therapy in the management of high-risk, high-grade, soft tissue sarcomas of the extremities and body wall: Radiation therapy oncology group trial 9514. J Clin Oncol. 2006;24(4):619–25. https://doi.org/10.1200/JCO.2005.02.5577.
Gortzak E, Azzarelli A, Buesa J, et al. A randomised phase II study on neo-adjuvant chemotherapy for “high-risk” adult soft-tissue sarcoma. Eur J Cancer. 2001;37(9):1096–103. https://doi.org/10.1016/S0959-8049(01)00083-1.
Predina JD, Puc MM, Bergey MR, et al. Improved survival after pulmonary metastasectomy for soft tissue sarcoma. J Thorac Oncol. 2011;6(5):913–9. https://doi.org/10.1097/JTO.0b013e3182106f5c.
Kane JM, Finley JW, Driscoll D, Kraybill WG, Gibbs JF. The treatment and outcome of patients with soft tissue sarcomas and synchronous metastases. Sarcoma. 2002;6(2):69–73. https://doi.org/10.1080/1357714021000022168.
Billingsley KG, Burt ME, Jara E, et al. Pulmonary metastases from soft tissue sarcoma: Analysis of patterns of disease and postmetastasis survival. Annals of Surgery. 1999;229:602–12. https://doi.org/10.1097/00000658-199905000-00002.
Li Y, Zhang W, Li S, Tu C. Clinical efficiency of repeated pulmonary metastasectomy in sarcoma patients with recurrent pulmonary metastasis: a meta-analysis. J Cancer Res Ther. 2018;14(9):457. https://doi.org/10.4103/0973-1482.183207.
Blackmon SH, Shah N, Roth JA, et al. Resection of pulmonary and extrapulmonary sarcomatous metastases is associated with long-term survival. Ann Thorac Surg. 2009;88(3):877–85. https://doi.org/10.1016/j.athoracsur.2009.04.144.
Pastorino U, Buyse M, Friedel G, et al. Long-term results of lung metastasectomy: prognostic analyses based on 5206 cases. J Thorac Cardiovasc Surg. 1997;113(1):37–49. https://doi.org/10.1016/S0022-5223(97)70397-0.
Chudgar NP, Brennan MF, Tan KS, et al. Is repeat pulmonary metastasectomy indicated for soft tissue sarcoma? Ann Thorac Surg. 2017;104:1837–45. https://doi.org/10.1016/j.athoracsur.2017.07.024.
Wang Y, Farmer M, Izaguirre EW, et al. Association of definitive pelvic radiation therapy with survival among patients with newly diagnosed metastatic cervical cancer. JAMA Oncol. 2018;4(9):1288–91. https://doi.org/10.1001/jamaoncol.2018.2677.
Gomez DR, Blumenschein GR, Lee JJ, et al. Local consolidative therapy versus maintenance therapy or observation for patients with oligometastatic non-small-cell lung cancer without progression after first-line systemic therapy: a multicentre, randomised, controlled, phase 2 study. Lancet Oncol. 2016;17(12):1672–82. https://doi.org/10.1016/S1470-2045(16)30532-0.
Rusthoven CG, Jones BL, Flaig TW, et al. Improved survival with prostate radiation in addition to androgen deprivation therapy for men with newly diagnosed metastatic prostate cancer. J Clin Oncol. 2016;34(24):2835–42. https://doi.org/10.1200/JCO.2016.67.4788.
Austin PC, Grootendorst P, Anderson GM. A comparison of the ability of different propensity score models to balance measured variables between treated and untreated subjects: a Monte Carlo study. Stat Med. 2007;26(4):734–53. https://doi.org/10.1002/sim.2580.
Liu Y, Nickleach D, Lipscomb J. Propensity score matching for multiple treatment comparisons in observational studies. 2013. https://www.isi-web.org/. Accessed 13 May 2021.
Liu Y, Kowalski J, Gillepsie T. Propensity score approach for multiple treatment options and its application in cancer outcome research. Joint Statistical Meeting. 2016. https://ww2.amstat.org/meetings/jsm/2016/onlineprogram/AbstractDetails.cfm?abstractid=319875. Accessed 13 May 2021.
Mccaffrey DF, Griffin BA, Almirall D, Slaughter ME, Ramchand R, Burgette LF. A tutorial on propensity score estimation for multiple treatments using generalized boosted models. Stat Med. 2013;32(19):3388–414. https://doi.org/10.1002/sim.5753.
Ferguson PC, Deheshi BM, Chung P, et al. Soft tissue sarcoma presenting with metastatic disease. Cancer. 2011;117(2):372–9. https://doi.org/10.1002/cncr.25418.
Marulli G, Mammana M, Comacchio G, Rea F. Survival and prognostic factors following pulmonary metastasectomy for sarcoma. J Thorac Dis. 2017;9(Suppl 12):S1305–15. https://doi.org/10.21037/jtd.2017.03.177.
Kim S, Ott HC, Wright CD, et al. Pulmonary resection of metastatic sarcoma: prognostic factors associated with improved outcomes. Ann Thorac Surg. 2011;92(5):1780–7. https://doi.org/10.1016/j.athoracsur.2011.05.081.
Okiror L, Peleki A, Moffat D, et al. Survival following pulmonary metastasectomy for sarcoma. Thorac Cardiovasc Surg. 2015;64(2):146–9. https://doi.org/10.1055/s-0035-1546430.
Chudgar NP, Brennan MF, Munhoz RR, et al. Pulmonary metastasectomy with therapeutic intent for soft-tissue sarcoma. J Thorac Cardiovasc Surg. 2017;154(1):319-330.e1. https://doi.org/10.1016/j.jtcvs.2017.02.061.
Billingsley K, Lewis J, Leung D, Casper E, Woodruff J, Brennan M. Multifactorial analysis of the survival of patients with distant metastasis arising from primary extremity sarcoma. Cancer. 1999;15(85):389–95.
Dhakal S, Corbin KS, Milano MT, et al. Stereotactic body radiotherapy for pulmonary metastases from soft-tissue sarcomas: excellent local lesion control and improved patient survival. Int J Radiat Oncol Biol Phys. 2012;82(2):940–5. https://doi.org/10.1016/j.ijrobp.2010.11.052.
Navarria P, Ascolese AM, Cozzi L, et al. Stereotactic body radiation therapy for lung metastases from soft tissue sarcoma. Eur J Cancer. 2015;51(5):668–74. https://doi.org/10.1016/j.ejca.2015.01.061.
Bramwell V, Anderson D, Charette M. Doxorubicin-based chemotherapy for the palliative treatment of adult patients with locally advanced or metastatic soft tissue sarcoma. Cochrane Database Syst Rev. 2003;2003(3):CD003293. https://doi.org/10.1002/14651858.CD003293.
Verma S, Younus J, Stys-Norman D, Haynes AE, Blackstein M. Meta-analysis of ifosfamide-based combination chemotherapy in advanced soft tissue sarcoma. Cancer Treat Rev. 2008;34(4):339–47. https://doi.org/10.1016/j.ctrv.2008.01.005.
Canter RJ, Qin LX, Downey RJ, Brennan MF, Singer S, Maki RG. Perioperative chemotherapy in patients undergoing pulmonary resection for metastatic soft-tissue sarcoma of the extremity: a retrospective analysis. Cancer. 2007;110(9):2050–60. https://doi.org/10.1002/cncr.23023.
Gronchi A, Ferrari S, Quagliuolo V, et al. Histotype-tailored neoadjuvant chemotherapy versus standard chemotherapy in patients with high-risk soft-tissue sarcomas (ISG-STS 1001): an international, open-label, randomised, controlled, phase 3, multicentre trial. Lancet Oncol. 2017;18(6):812–22. https://doi.org/10.1016/S1470-2045(17)30334-0.
Acknowledgment
Research reported in this publication was supported in part by the Biostatistics and Bioinformatics Shared Resource of Winship Cancer Institute of Emory University and the NIH/NCI under award number P30CA138292. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Funding
No specific funding was received for this work.
Author information
Authors and Affiliations
Contributions
Concept and design: All authors. Acquisition of data: JS. Analysis and interpretation of data: MA, JJN, JS, ST, PP. Drafting of the article: MA, JJN. Critical revision: All authors. Final approval: All authors.
Corresponding author
Ethics declarations
Disclosures
Mustafa Abugideiri, James Janopaul-Naylor, Jeffrey Switchenko, Sibo Tian, William Read, Robert Press, Shervin Oskouei, Nickolas Reimer, Matthew Ferris, Richard J. Cassidy, Madhusmita Behera, David Monson, Jerome Landry, Karen D. Godette, and Pretesh R. Patel have no conflicts of interest to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Mustafa Abugideiri and James Janopaul-Naylor are co-first authors on this work.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Abugideiri, M., Janopaul-Naylor, J., Switchenko, J. et al. Impact of Metastasectomy and Aggressive Local Therapy in Newly Diagnosed Metastatic Soft Tissue Sarcoma: An Analysis of the NCDB. Ann Surg Oncol 29, 649–659 (2022). https://doi.org/10.1245/s10434-021-10466-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-021-10466-4