Abstract
Hypertrophic scar is a serious skin disorder, which reduces the patient’s quality of life. 5-aminolevulinic acid (5-ALA)-mediated photodynamic therapy has been used to treat patients with hypertrophic scar. However, the poor skin retention of 5-ALA limited the therapeutic effect. In this study, we constructed the 5-ALA-hyaluronic acid (HA) complex to potentially prolong the skin retention of 5-ALA for improving the therapeutic efficacy. HA is a polysaccharide with viscoelasticity and the carboxyl groups could conjugate with amino groups of 5-ALA via electrostatic interaction. The protoporphyrin IX (PpIX) assay revealed that 5-ALA-HA complexes markedly enhanced the skin retention, resulting in increased generation and accumulation of endogenous photosensitizer PpIX. Furthermore, 5-ALA-HA complexes allowed PpIX to be maintained at a high level for 12 h, much longer than the 3 h of 5-ALA alone. And then, the accumulative PpIX induced by 5-ALA-HA in human hypertrophic scar fibroblasts (HSF) was triggered by laser irradiation to produce sufficient reactive oxygen species, leading to efficient necrosis and apoptosis of HSF. In vivo therapeutic efficacy study indicated that 5-ALA-HA effectively reduced the appearance and scar thickness, and the scar elevation index with 5-ALA-HA treatment was significantly lower than other groups, suggesting that the 5-ALA-HA-treated scar became flattened and was closely matched to the unwounded tissues. Moreover, 5-ALA-HA treatment markedly downregulated the gene expression levels of α-SMA and TGF-β1, demonstrating attenuated the scar formation and growth. Therefore, the 5-ALA-HA complex enhancing skin retention and PpIX accumulation at the lesion site provide a promising therapeutic strategy for hypertrophic scar.
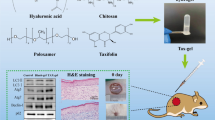
Graphical abstract








Similar content being viewed by others
References
Juckett G, Hartman-Adams H. Management of keloids and hypertrophic scars. Am Fam Physician. 2009;80(3):253–60.
English RS, Shenefelt PD. Keloids and hypertrophic scars. Dermatol Surg. 1999;25(8):631–8.
Tredget EE. Pathophysiology and treatment of fibroproliferative disorders following thermal injury. Am Fam Physician. 1999. p. 165–82.
Atiyeh BS. Nonsurgical management of hypertrophic scars: evidence-based therapies, standard practices, and emerging methods. Aesthet Plast Surg. 2007;31(5):468–92.
Finnerty CC, Jeschke MG, Branski LK, Barret JP, Dziewulski P, Herndon DN. Hypertrophic scarring: the greatest unmet challenge after burn injury. Lancet. 2016;388(10052):1427–36.
Wang Y, Beekman J, Hew J, Jackson S, Issler-Fisher AC, Parungao R, et al. Burn injury: challenges and advances in burn wound healing, infection, pain and scarring. Adv Drug Deliv Rev. 2018;123:3–17.
Rusciani L, Paradisi A, Alfano C, Chiummariello S, Rusciani A. Cryotherapy in the treatment of keloids. J Drugs Dermatol. 2006;5(7):591–5.
Shen J, Lian X, Sun Y, Wang X, Hu K, Hou X, et al. Hypofractionated electron-beam radiation therapy for keloids: retrospective study of 568 cases with 834 lesions. J Radiat Res. 2015;56(5):811–7.
Chan HH, Wong DSY, Ho WS, Lam LK, Wei W. The use of pulsed dye laser for the prevention and treatment of hypertrophic scars in Chinese persons. Dermatol Surg. 2004;30(7):987–94.
Sadeghinia A, Sadeghinia S. Comparison of the efficacy of intralesional triamcinolone acetonide and 5-Fluorouracil tattooing for the treatment of keloids. Dermatol Surg. 2012;38(1):104–9.
Yan H, Wu M, Yuan Y, Wang ZZ, Jiang H, Chen T. Priming of Toll-like receptor 4 pathway in mesenchymal stem cells increases expression of B cell activating factor. Biochem Biophys Res Commun. 2014;448(2):212–7.
Wen X, Li Y, Hamblin MR. Photodynamic therapy in dermatology beyond non-melanoma cancer: An update. Photodiagnosis Photodyn Ther. 2017;19:140–52.
Morton C, Szeimies R-M, Sidoroff A, Wennberg A-M, Basset-Seguin N, Calzavara-Pinton P, et al. European dermatology forum guidelines on topical photodynamic therapy. Eur J Dermatol. 2015;25(4):296–311.
Yu Z, Meng X, Zhang S, Wang X, Chen Y, Min P, et al. IR-808 loaded nanoethosomes for aggregation-enhanced synergistic transdermal photodynamic/photothermal treatment of hypertrophic scars. Biomater Sci. 2022;10(1):158–66.
Morton CA. Topical photodynamic therapy in dermatology. S Afr Med J. 2001;91(8):634–637.
Li X, Zhou ZP, Hu L, Zhang WJ, Li W. Apoptotic cell death induced by 5-aminolaevulinic acid-mediated photodynamic therapy of hypertrophic scar-derived fibroblasts. J Dermatol Treat. 2014;25(5):428–33.
Campbell SM, Tyrrell J, Marshall R, Curnow A. Effect of MAL-photodynamic therapy on hypertrophic scarring. Photodiagnosis Photodyn Ther. 2010;7(3):183–8.
Rick K, Sroka R, Stepp H, Kriegmair M, Huber RM, Jacob K, et al. Pharmacokinetics of 5-aminolevulinic acid-induced protoporphyrin IX in skin and blood. J Photochem Photobiol B-Biol. 1997;40(3):313–9.
Herman MA, Webber J, Fromm D, Kessel D. Hemodynamic effects of 5-aminolevulinic acid in humans. J Photochem Photobiol B-Biol. 1998;43(1):61–5.
De Rosa FS, Bentley M. Photodynamic therapy of skin cancers: sensitizers, clinical studies and future directives. Pharm Res. 2000;17(12):1447–55.
de Blois AW, Thissen M, de Bruijn HS, Grouls RJE, Dutrieux RP, Robinson DJ, et al. In vivo pharmacokinetics of protoporphyrin IX accumulation following intracutaneous injection of 5-aminolevulinic acid. J Photochem Photobiol B-Biol. 2001;61(1–2):21–9.
Lapcik L Jr and L, Lapcik L, De Smedt S, Demeester J, Chabrecek P. Hyaluronan: Preparation, Structure, Properties, and Applications. Chem Rev. 1998;98(8):2663–84.
Adams ME, Lussier AJ, Peyron JG. A risk-benefit assessment of injections of hyaluronan and its derivatives in the treatment of osteoarthritis of the knee. Drug Saf. 2000;23(2):115–30.
Almeida PV, Shahbazi M-A, Mäkilä E, Kaasalainen M, Salonen J, Hirvonen J, et al. Amine-modified hyaluronic acid-functionalized porous silicon nanoparticles for targeting breast cancer tumors. Nanoscale. 2014;6(17):10377–87.
Brown MB, Marriott C, Martin GP. The effect of hyaluronan on the in vitro deposition of diclofenac within the skin. Int J Tissue React. 1995;17(4):133–40.
Brown M, Martin G. Comparison of the effect of hyaluronan and other polysaccharides on drug skin partitioning. Int J Pharm. 2001;225:113–21.
Brown MB, Forbes B, Hanpanitcharoen M, Martin GP. The use of hyaluronan in topical drug delivery. Hyaluronan: Elsevier; 2002. p. 249–56.
Gribbon P, Heng BC, Hardingham TE. The analysis of intermolecular interactions in concentrated hyaluronan solutions suggest no evidence for chain-chain association. Biochem J. 2000;350:329–35.
Brown M, Marriott C, Martin GP, editors. A study of the transdermal drug delivery properties of hyaluronan. Third Int Workshop on Hyaluronanin Drug 433 Delivery. 1995 : Royal Society of Medicine Press.
Zhang Y, **a Q, Li Y, He Z, Li Z, Guo T, et al. CD44 Assists the topical anti-psoriatic efficacy of curcumin-loaded hyaluronan-modified ethosomes: a new strategy for clustering drug in inflammatory skin. Theranostics. 2019;9(1):48–64.
Burdick JA, Prestwich GD. Hyaluronic acid hydrogels for biomedical applications. Adv Mater. 2011;23(12):H41–56.
Sharma M, Sahu K, Singh SP, Jain B. Wound healing activity of curcumin conjugated to hyaluronic acid: in vitro and in vivo evaluation. Artif Cell Nanomed Biotechnol. 2018;46(5):1009–17.
Zhu J, Tang X, Jia Y, Ho C-T, Huang Q. Applications and delivery mechanisms of hyaluronic acid used for topical/transdermal delivery – a review. Int J Pharm. 2020;578: 119127.
Brown MB, Jones SA. Hyaluronic acid: a unique topical vehicle for the localized delivery of drugs to the skin. J Eur Acad Dermatol Venereol. 2005;19(3):308–18.
Botros SR, Hussein AK, Mansour HF. A novel nanoemulsion intermediate gel as a promising approach for delivery of itraconazole: design, in vitro and ex vivo appraisal. AAPS PharmSciTech. 2020;21(7):272.
Granstein RD, Rook A, Flotte TJ, Haas A, Gallo RL, Jaffe HS, et al. A controlled trial of intralesional recombinant interferon-? in the treatment of keloidal scarring: clinical and histologic findings. Arch Dermatol. 1990;126(10):1295–302.
Martin P, Dickson MC, Millan FA, Akhurst RJ. Rapid induction and clearance of TGF beta 1 is an early response to wounding in the mouse embryo. Dev Genet. 1993;14(3):225–38.
Wang J, Liu DQ, Li XY, Li XJ. BTXA Could induce fibroblast apoptosis and inhibit the expression of alpha-SMA and myosin II in scar tissue of rabbit ears. Biotechnol Bioprocess Eng. 2020;25(5):699–706.
Funding
This work was supported by the Fundamental Research Funds for the Central Universities, Sun Yat-sen University (Project No. 22qntd4504) and Guangdong Basic and Applied Basic Research Foundation (Project No. 2020A1515110147, 2021A1515011418, 2021A1515012025).
Author information
Authors and Affiliations
Contributions
Min Feng and Lin Guo planned and supervized the project. Huihui Deng, Liya Yang, and Yuling Chen formulated the systems and performed experimental work. Liya Yang and Yiman Chen contributed to writing the manuscript. All the authors contributed to editing the manuscript.
Corresponding authors
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yang, L., Deng, H., Chen, Y. et al. 5-Aminolevulinic Acid-Hyaluronic Acid Complexes Enhance Skin Retention of 5-Aminolevulinic Acid and Therapeutic Efficacy in the Treatment of Hypertrophic Scar. AAPS PharmSciTech 23, 216 (2022). https://doi.org/10.1208/s12249-022-02370-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1208/s12249-022-02370-1