Abstract
This study tested the hypothesis that mild hypothermia after severe transient hypoxia-ischemia reduces the subsequent delayed rise in cerebral lactate peak-area ratios as determined by proton (1H) magnetic resonance spectroscopy (MRS) in the newborn piglet. Nine piglets aged <24 h underwent temporary occlusion of the common carotid arteries and hypoxemia. Resuscitation was started when cerebral [phosphocreatine]/[inorganic phosphate] had fallen close to zero and [nucleotide triphosphate(NTP)]/[exchangeable phosphate pool (EPP)] was below about a third of baseline. On resuscitation rectal and tympanic temperatures were lowered to 35°C for 12 h after which normothermia (38.5 °C) was resumed. 1H MRS data collected over 48 or 64 h after resuscitation were compared with concurrently established data from 12 piglets similarly subjected to transient cerebral hypoxia-ischemia, but maintained normothermic, and six shamoperated controls. The severity of the primary insult (judged from the time integral of depletion of [NTP]/[EPP]) was similar in the hypothermic and normothermic groups. The maximum lactate/N-acetylaspartate ratio observed between 24 and 48 h after resuscitation in the hypothermic group was 0.10 (0.05-0.97), median (interquartile range), which was significantly lower than that observed in the normothermic group, 1.28 (0.97-2.14), and not significantly different from that observed in the control group, 0.08 (0.06-0.11). Similar results were obtained for lactate/choline and lactate/total creatine. We conclude that mild hypothermia after a severe acute cerebral hypoxic-ischemic insult reduces the delayed elevation in lactate peak-area ratios, thus reflecting reduced lactate accumulation.
Similar content being viewed by others
Main
Perinatal hypoxic-ischemic brain injury remains a major cause of neonatal and infant mortality, and of permanent neurodevelopmental disability(1). Ideally this form of brain injury should be prevented by appropriate obstetric intervention. However, this is not always possible, and current clinical management of an infant with severe hypoxic-ischemic encephalopathy continues to rely on supportive and symptomatic treatments. It is therefore highly desirable that specific cerebroprotective interventions are developed with the potential to limit or prevent the irreversible brain injury that otherwise may ensue. Before these therapies are used in infants, they should be tested on suitable animal models, to investigate their efficacy and safety.
We have developed, in the piglet, a model of perinatal cerebral hypoxic-ischemic brain injury where cerebral energy metabolism is monitored continuously by interleaved phosphorus (31P) and 1H MRS during and after a severe acute reversed hypoxic-ischemic insult, designed to mimic that occurring during birth asphyxia(2). The anesthetized newborn piglet is cared for throughout the experiment with the same techniques that are used for a human infant undergoing intensive care. In this model, cerebral energy metabolism as determined by 31P MRS is severely impaired during the primary insult but returns to normal after resuscitation. Over the subsequent 48 h delayed or “secondary” energy failure develops as shown by falling [PCr]/[Pi] and [NTP]. The severity of this delayed energy failure is directly related to the severity of the primary insult(2). The evolution of delayed energy failure in the piglet duplicates the pattern and time course of that previously observed in birth-asphyxiated infants(3). In infants, the severity of delayed energy failure, as monitored by 31P MRS, is directly related to the chances of death or persistent neurodevelopmental impairment at 1 and 4 y(3–5).
In a companion study(6), we have described the results of 1H MRS during and for 48 h after acute reversed cerebral hypoxia-ischemia in the newborn piglet. During the acute insult, the Lac peak-area ratios rose sharply and then fell on resuscitation. Over the subsequent 48 h, a delayed or secondary rise in these ratios occurred. Comparable changes, with elevated cerebral Lac signals, have been seen in birth-asphyxiated infants(7–10). Recently, in quantitative studies, a rise in cerebral Lac concentration after perinatal hypoxia-ischemia has been confirmed(11), along with a fall in the concentration of Naa, a metabolite found predominantly in neurones. In our own studies of asphyxiated infants, an elevated Lac/Naa peak-area ratio, above that seen in normal term infants, was related to death or neurodevelopmental disability at 1 y of age(10). Other authors have also found that elevated Lac signals after birth asphyxia convey a poor prognosis(7, 8).
We have previously shown, in the piglet, that mild hypothermia (35 °C), initiated at the time of resuscitation and maintained for 12 h, markedly reduced the subsequent changes in 31P metabolites that are characteristic of delayed energy failure(12) and also reduced the proportion of cells affected by apoptotic cell death(13). The main purpose of the present study was to test the hypothesis that mild postinsult hypothermia also reduced the delayed rise in cerebral Lac peak-area ratios. A subsidiary aim was to determine whether hypothermia reduced the delayed fall in Naa peak-area ratios previously observed in this model(6).
METHODS
These studies were carried out with Home Office approval and according to UK guidelines. Nine healthy Large White piglets, aged <24 h, were studied. They were born at term, gestation 116 (1.4) d (mean (SD)), and weighed 1.64(0.21) kg. The piglets were maintained and monitored as described previously(2). Briefly, anesthesia was induced with 5% isoflurane, followed by tracheostomy and ventilation with oxygen, nitrous oxide, and isoflurane (<1.5%). Inflatable occluders were positioned around both common carotid arteries. Rectal and tympanic(12) temperatures were kept normal for newborn piglets at 38.5-39.0 °C(14, 15). The anesthetized, ventilated piglet was placed on a temperature-regulated water-filled mattress inside the bore of the magnet and maintained there with intensive care, including full physiologic monitoring, throughout the experiment.
MRS. 1H and 31P spectra were collected alternately using a 7-tesla Bruker Biospec spectrometer and a 25-mm diameter double-tuned inductively coupled surface coil placed on the intact scalp over the parietal lobes. 1H spectra were obtained using a [horizontal bar over]11-[horizontal bar over]22 binomial water suppression spin-echo sequence(16) optimized for Naa with echo time 270 ms, spectral width 4 kHz, 2048 quadrature data points, and 32 summed echoes sampled with a 16-bit analog-to-digital convertor. The repetition time was 5 s for baseline measurements, 1 s during and for 1 h after the acute hypoxic-ischemic insult, and 5 s thereafter. Full details of the analysis of 1H spectra are given in a companion study(6). The acquisition and analysis of fully relaxed 31P spectra were as previously described(2). NTP (which is predominantly ATP) was quantified using the β-triplet, and [NTP] was expressed as a fraction of the [EPP], defined as: [Pi] + [PCr] + [(γ + α + β) NTP].
Acute cerebral hypoxia-ischemia. After stable baseline observations for at least 1 h, (mean 1.7 (SD 0.4) h), the piglets underwent a cerebral hypoxic-ischemic insult brought about by reducing the inspired oxygen fraction (Fio2) to 0.12 and inflating the carotid occluders. This was continued until severe cerebral energy depletion was seen on the 31P spectra, with PCr depleted to less than 5%, and NTP reduced to below about a third of baseline levels. Resuscitation was then commenced by releasing the carotid occlusion and increasing the Fio2 transiently to 0.60 followed by reduction to normalize arterial Po2. The duration of the insult was 31-98 (median 73) min.
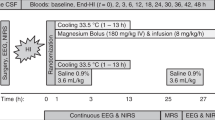
Hypothermia. Coincident with resuscitation, cooling was initiated by fanning through the bore of the magnet and reducing the temperature of the water mattress. The time taken to reach the target rectal temperature of 35 °C was 41(12) min (mean (SD)). Rectal and tympanic temperatures, which were closely similar (see Fig. 1), were maintained at 35 °C until 12 h after resuscitation. Gradual warming was then commenced at the rate of 1°C·h-1 until normothermia was resumed.
Observations were continued until 48 h after resuscitation, and in six of the nine piglets to 64 h after resuscitation (48 h after the resumption of normothermia). Six animals received 10-50 (median 17) mL·kg-1 colloid (Gelofusine, B Braun Medical Ltd, Emmenbruke, Switzerland) with the aim of maintaining blood volume. Four piglets received infusions of dopamine(5-15 μg·kg-1·min-1) for between 3 and 47(median 8) h to keep MABP above 5.3 kPa. Of these, three piglets required dopamine (in combination with colloid in one) during hypothermia, and one required both dopamine and colloid after hypothermia.
Data analysis. 1H MRS results from the nine hypothermic piglets were compared with data from the 12 piglets similarly subjected to hypoxia-ischemia but maintained normothermic, and the six sham-operated control piglets described in a companion study(6). The severity of the acute hypoxic-ischemic insult was assessed using 31P MRS to quantify the extent and duration of NTP depletion, by calculating the time integral of the depletion of [NTP]/[EPP] from the onset of hypoxia-ischemia until 1 h after resuscitation, as described previously(2); the greater this value, the greater the severity of the acute insult.
The data were examined for normality and equality of variance. The severity of the hypoxic-ischemic insult was compared between the hypothermic and normothermic groups using the Mann-Whitney test. Otherwise, statistically significant differences between the three groups were sought using one-way analysis of variance and the Student-Newman-Keuls multiple comparison test, or Kruskal-Wallis analysis of variance and Dunn's multiple comparison test.
RESULTS
Physiologic variables. Rectal and tympanic temperature measurements from the nine piglets that underwent hypothermia are displayed in Figure 1. Values for arterial Po2, Pco2, pH, base excess, glucose, electrolytes and hemoglobin are given in Table 1, together with observations of MABP and heart rate. After the insult, despite 12 h of hypothermia, these variables remained stable throughout the experiment.
Severity of acute hypoxic-ischemic insult. The median value of the time integral of the acute depletion of [NTP]/[EPP] for the hypothermic piglets was 0.14 (interquartile range 0.10-0.18) h, not significantly different from that for the normothermic piglets at 0.12 (0.11-0.15) h.
1H MRS. Figure 2 illustrates a sequence of spectra (A) from an animal subjected to 12 h of hypothermia after the acute cerebral hypoxic-ischemic insult and spectra(B) from an animal maintained normothermic after a comparable insult. A marked rise in Lac relative to the other peaks occurred during acute hypoxia-ischemia in both piglets, which fell toward baseline after resuscitation. Forty-eight hours after the acute insult, the spectra from the hypothermic piglet remain very similar to baseline in appearance. In contrast, at 24 and 48 h, the spectra from the normothermic piglet have clearly altered. A second rise in the Lac peak has occurred, and the Naa peak is reduced relative to those due to Cho and creatine plus PCr.
(A) Sequence of 1H spectra from a piglet subjected to a cerebral hypoxic-ischemic insult followed by 12 h of hypothermia and subsequent normothermia until 48 h postresuscitation.(B) Sequence of 1H spectra from a piglet subjected to a cerebral hypoxic-ischemic insult followed by 48 h of normothermia postresuscitation. The time integral of elevation of Lac/Naa from the onset of hypoxia-ischemia until 1 h after resuscitation was 1.33 h for the normothermic piglet and 2.12 h for the hypothermic piglet. Peaks are assigned to:1, glutamate/glutamine; 2, glycine/myo-inositol;3, taurine/scyllo-inositol; 4, Cho; 5, Cr; 6, glutamate/glutamine; 7, Naa; 8, Lac;9, β-hydroxybutyric acid; 10, alanine.
Figure 3A shows median values, with interquartile ranges, for changes in Lac/Naa, Lac/Cho, and Lac/Cr for all nine hypothermic piglets, together with data from piglets similarly subjected to an acute hypoxic-ischemic insult but subsequently maintained normothermic, and sham-operated controls (B)(6). The maximum Lac ratios associated with the acute insult were significantly lower in the hypothermic group than in the normothermic group (p < 0.05). However, the time integrals of the elevations in Lac peak-area ratios associated with the acute hypoxic-ischemic insult from the onset of hypoxia-ischemia until 1 h after resuscitation were similar in the two groups.(The greater these values, the greater the extent and duration of Lac peak-area elevations.) For Lac/Naa in the hypothermic piglets, the median value was 1.68 h (interquartile range 0.91-2.38 h), not significantly different from that of the normothermic piglets, median 1.55 (1.35-2.98) h. Similarly, the time integrals of the elevations of Lac/Cho and Lac/Cr did not differ significantly. On resuscitation after the acute insult, the Lac ratios for both hypothermic and normothermic piglets fell toward, although they remained significantly above, baseline and control values. Median values for Lac ratios in the hypothermic group subsequently remained low and close to control values, and did not show the secondary rise occurring in the normothermic piglets. For the six piglets whose observations were extended to 64 h after resuscitation, no further delayed rise in the Lac peak-area ratios was seen. Their median (interquartile range) Lac/Naa at 48 h after resuscitation was 0.07 (0.03-0.09) and at 64 h was 0.05 (0.05-0.06). One hypothermic piglet did, however, have a marked secondary rise in cerebral Lac, with Lac/Naa rising to 4.39 by 48 h after resuscitation. By comparison, in the normothermic group the two piglets with the most marked delayed elevation in cerebral Lac had Lac/Naa values reaching 9.11 and 2.88.
(A) Lac/Naa, Lac/Cho, and Lac/Cr (median and interquartile ranges) for hypothermic piglets (▴, n = 9).(B) Lac/Naa, Lac/Cho, and Lac/Cr (median and interquartile ranges) for control (○, n = 6) and normothermic piglets (•,n = 12). Values on the x axis are mean and SEM of the time that observations were made.
Values (median and interquartile range) for the maximum Lac peak-area ratios between 24 and 48 h for the three groups are given in Table 2a. Significant differences were found between them using ANOVA and multiple comparison testing. For Lac/Naa and Lac/Cr, the hypothermic group had significantly lower values than the normothermic group, whereas no significant differences were detected between the hypothermic group and the controls. Results for minimum Naa/Cho and minimum Naa/Cr between 24 and 48 h are presented in Table 2b. The only significant difference on multiple comparison testing between the three groups was for Naa/Cr between the normothermic and control groups. A trend, however, can be seen with the median values for the hypothermic piglets greater than those for the normothermic piglets, and similar to those of the controls.
DISCUSSION
The main purpose of this study was to investigate whether mild hypothermia, initiated at the same time as resuscitation and sustained for 12 h, reduced the subsequent delayed or “secondary” rise in Lac peak-area ratios reported in a piglet model of severe transient cerebral hypoxia-ischemia(6). A previous study using this same model has shown that the delayed fall in [PCr]/[Pi] and [NTP] was largely prevented by this degree of hypothermia, and it was argued that failure of energy generation had been avoided to the extent that the creatine kinase reaction was able to maintain [ATP] almost constant(12). Under these circumstances, it was to be expected that Lac production and accumulation resulting from increased glycolytic flux would also be reduced after hypothermia. This proposition was tested by comparing data for Lac peak-area ratios with those acquired from two comparison groups. One group comprised sham-operated control piglets and the other a group subjected to severe transient cerebral hypoxia-ischemia and treated in exactly the same way as those reported here, except that they were maintained normothermic throughout(6). The normothermic and hypothermic piglets were studied concurrently, although they were not randomized.
For valid comparisons of cerebral metabolism, it was important that the severity of the acute cerebral insult in these two groups should be similar. As in previous reports, we used the time integral of the acute depletion of[NTP]/[EPP] as an index of this, because it reflects the quantity of acute impairment of cerebral energy generation(2). The median value was greater for the hypothermic piglets, but there was no significant difference between the two groups. The time integrals of the elevations of Lac peak-area ratios, reflecting both the extent and duration of the rise in Lac associated with the acute insult, were also similar.
The data given in Figures 2 and 3 and Table 2a show that, by comparison with the normothermic group, hypothermia substantially reduced the delayed rise in Lac peak-area ratios during the 48 h after resuscitation. In the six piglets in which observations were continued to 64 h, no further rise in these ratios took place, indicating that hypothermia had not merely caused a temporary postponement in Lac accumulation. There was, however, variation between animals. One piglet, after a moderately severe insult (time integral of depletion of [NTP]/[EPP] 0.15 h) developed a marked secondary rise in Lac peak-area ratios, which was associated with severe energy failure (minimum[PCr]/[Pi] zero). Inspection of all the available data from this piglet revealed no explanation for this adverse outcome.
Reduction in Lac accumulation, together with the previously reported preservation of [PCr]/[Pi] and [NTP]/[EPP] after hypothermia in this model of perinatal hypoxic-ischemic brain injury(12), strongly suggests that the hypothermia had protected mitochondrial respiration from subsequent deterioration. There are several possible explanations. For example, glutamate release at the synapses may have been reduced during hypothermia. Glutamate causes a massive toxic entry of calcium into neurones damaging mitochondria(17, 18) and stimulates the production of nitric oxide, which inhibits cytochrome oxidase(19, 20). Hypothermia also reduces the formation of other free radicals(21) and may protect neurones from irreversible damage by this mechanism. This would reduce the stimulus for the invasion and activation of macrophages, which may otherwise contribute to the delayed Lac accumulation(22).
Reductions in cerebral Naa, as well as increases in Lac peak-area ratios carry a poor prognosis in birth-asphyxiated infants(7–10), and we have found evidence in the piglet model suggesting that Naa ratios were reduced 48 h after resuscitation(6). A subsidiary aim of the present study was, therefore, to investigate whether the Naa ratios were preserved after hypothermia. The trend shown by the data in Table 2b is consistent with this proposition, although statistical differences between the hypothermic and normothermic piglets were not found. Naa is largely neuronal(23), and its preservation could indicate less neuronal loss.
The results of this study are consistent with earlier ones in adult animals, showing a cerebroprotective effect of postischemic mild hypothermia(24, 25). Dietrich et al.(26) found that the protective effect of 3-h postischemic hypothermia was not permanent, but chronic neuroprotection was achieved by the addition of MK-801(27, 28). Recently, the potential benefit of extending the duration of hypothermia has been highlighted by Colbourne and Corbett(29). After 24 h of postischemic hypothermia alone, they confirmed substantial and long-standing neuroprotection by both behavioral and histologic assessment 6 mo later(30). Few similar studies of neonatal animals have been done. Yager et al.(31) failed to find evidence of a protective effect of 3 h of postinsult mild hypothermia in rat pups subjected to unilateral carotid artery ligation and transient hypoxemia. However, in the same model with the same duration and a similar degree of hypothermia, Thoresen et al.(32) demonstrated significant neuropathologic protection in unrestrained animals. Sirimanne et al.(33) also found protection from postinsult hypothermia lasting 72 h in the rat pup.
The results of this and previous studies, taken together with recent evidence indicating that mild hypothermia markedly improved outcome after adult stroke(34), provide support for the consideration of trials of mild hypothermia in severely birth-asphyxiated human infants. Before these trials are undertaken, further studies are required in newborn animals, such as the piglet, to find out if the cerebroprotective effects are permanent, to assess the incidence of systemic side effects, and to design the optimal protocol.
Abbreviations
- Cho:
-
choline-containing compounds
- Cr:
-
creatine plus phosphocreatine
- EPP:
-
exchangeable phosphate pool
- Fio2:
-
inspired oxygen fraction
- 1H:
-
proton
- Lac:
-
lactate
- MABP:
-
mean arterial blood pressure
- MRS:
-
magnetic resonance spectroscopy
- Naa:
-
N-acetylaspartate
- PCr:
-
phosphocreatine
- Pi:
-
inorganic phosphate
- ANOVA:
-
analysis of variance
References
Volpe JJ 1995 Neurology of the Newborn, 3rd Ed. WB Saunders, Philadelphia, pp 260–313.
Lorek A, Takei Y, Cady EB, Wyatt JS, Penrice J, Edwards AD, Peebles D, Wylezinska M, Owen-Reece H, Kirkbride V, Cooper CE, Aldridge RF, Roth S, Brown G, Delpy DT, Renolds EOR 1994 Delayed(“secondary”) cerebral energy failure after acute hypoxia-ischemia in the newborn piglet: continuous 48-hour studies by phosphorous magnetic resonance spectroscopy. Pediatr Res 36: 699–706.
Azzopardi D, Wyatt JS, Cady EB, Delpy DT, Baudin J, Stewart AS, Hope PL, Hamilton PA, Reynolds EOR 1989 Prognosis of newborn infants with hypoxic-ischemic brain injury assessed by phosphorous magnetic resonance spectroscopy. Pediatr Res 25: 445–451.
Roth SC, Edwards AD, Cady EB, Delpy DT, Wyatt JS, Azzopardi D, Baudin J, Townsend J, Stewart AS, Reynolds EOR 1992 Relation between cerebral oxidative metabolism following birth asphyxia and neurodevelopmental outcome and brain growth at one year. Dev Med Child Neurol 34: 285–295.
Roth SC, Baudin J, Cady EB, Townsend J, Wyatt J, Reynolds O, Stewart A 1995 Deranged cerebral oxidative phosphorylation following birth asphyxia and neurodevelopmental outcome at four years. Pediatr Res 38: 452
Penrice J, Lorek A, Cady EB, Amess PN, Wylezinska M, Cooper CE, D'Souza P, Brown GC, Kirkbride V, Edwards AD, Wyatt JS, Reynolds EOR 1997 Proton magnetic resonance spectroscopy of the brain during acute hypoxia-ischemia and delayed cerebral energy failure in the newborn piglet. Pediatr Res 41: 795–802.
Groenendaal F, Veenhoven RH, Van Der Grond J, Jansen GH, Witkamp TD, De Vries LS 1994 Cerebral lactate and N- acetylaspartate/choline ratios in asphyxiated full-term neonates demonstrated in vivo using proton magnetic resonance spectroscopy. Pediatr Res 35: 148–151.
Leth H, Toft PB, Pryds O, Peitersen B, Lou H, Henriksen O 1994 Proton MR spectroscopy and CBF to predict outcome after perinatal asphyxia. Pediatr Res 36: 23A
Hanrahan JD, Sargentoni J, Azzopardi D, Manji K, Cowan FM, Rutherford MA, Cox IJ, Bell JD, Bryant DJ, Edwards AD 1996 Cerebral metabolism within 18 hours of birth asphyxia: a proton magnetic resonance spectroscopy study. Pediatr Res 39: 584–590.
Penrice J, Cady EB, Lorek A, Wylezinska M, Amess PN, Aldridge RF, Stewart A, Wyatt JS, Reynolds EOR 1996 Proton magnetic resonance spectroscopy of the brain in normal preterm and term infants and early changes after perinatal hypoxia-ischemia. Pediatr Res 40: 6–14.
Amess PN, Cady EB, Penrice J, Wylezinska M, Stewart A, Wyatt JS, Reynolds EOR 1996 Cerebral proton metabolite concentrations in term infants following perinatal hypoxia-ischaemia and neurodevelopmental outcome at one year. Proceedings of the British Paediatric Association Annual Meeting 68: 25
Thoresen M, Penrice J, Lorek A, Cady EB, Wylezinska M, Kirkbride V, Cooper CE, Brown GC, Edwards AD, Wyatt JS, Renolds EOR 1995 Mild hypothermia after severe transient hypoxia-ischemia ameliorates delayed cerebral energy failure in the piglet. Pediatr Res 37: 667–670.
Edwards AD, Yue X, Squier MV, Thoresen M, Cady EB, Penrice J, Cooper CE, Wyatt JS, Reynolds EOR, Mehmet H 1995 Specific inhibition of apoptosis after cerebral hypoxia-ischaemia by moderate post-insult hypothermia. Biochem Biophys Res Commun 217: 1193–1199.
Hannon JP, Bossone CA, Nade CE 1990 Normal physiological values for conscious pigs used in biomedical research. Lab Anim Sci 40: 293–298.
Mount LE, Rowell JG 1960 Body size, body temperature and age in relation to the metabolic rate of the pig in the first five weeks after birth. J Physiol 154: 408–416.
Hore PJ 1983 Solvent suppression in Fourier transform nuclear magnetic resonance spectroscopy. J Magn Reson 55: 283–300.
Rothman SM, Olney JW 1987 Excitotoxicity and the NMDA receptor. Trends Neurosci 10: 299–302.
Schapira AVH, Cooper JM 1994 Inborn and induced defects of the mitochondrial respiratory chain. Biochem Soc Trans 22: 996–1001.
Brown GC, Bolanos JP, Heales SJR, Clark JB 1995 Nitric oxide produced by activated astrocytes rapidly and reversibly inhibits cellular respiration. Neurosci Lett 193: 201–204.
Brown GC, Cooper CE 1994 Nanomolar concentrations of nitric oxide reversibly inhibit synaptosomal cytochrome oxidase respiration by competing with oxygen at cytochrome oxidase. FEBS Lett 356: 295–298.
Globus M-YT, Busto R, Lin BW, Schnippering H, Ginsberg MD 1995 Detection of free radical activity during transient global ischaemia and recirculation: Effects of intraischaemic brain temperature modulation. J Neurochem 65: 1250–1256.
López-Villegas D, Lenkinski RE, Wehrli SL, Wen-Zhe H, Douglas SD 1995 Lactate production by human monocytes/macrophages determined by proton MR spectroscopy. Magn Reson Med 34: 32–38.
Urenjak J, Williams SR, Gadian DE, Noble M 1993 Proton nuclear magnetic resonance spectroscopy unambiguously identifies different neural types. J Neurosci 13: 981–989.
Carroll M, Beek O 1992 Protection against hippocampal CA1 cell loss by postischemic hypothermia is dependent on delay of initiation and duration. Metab Brain Dis 7: 45–50.
Coimbra C, Wieloch T 1994 Moderate hypothermia mitigates neuronal damage in the rat brain when initiated several hours following transient cerebral ischemia. Acta Neuropathol 87: 325–331.
Dietrich WD, Busto R, Alonso O, Globus MY-T, Ginsberg MD 1993 Intraischemic but not postischemic brain hypothermia protects chronically following global forebrain ischemia in rats. J Cereb Blood Flow Metab 13: 541–549.
Dietrich WD, Lin B, Globus MY-T, Green EJ, Ginsberg MD, Busto R 1995 Effect of delayed MK-801 (dizocilpine) treatment with or without postischaemic hypothermia on chronic neuronal survival after global forebrain ischaemia in the rat. J Cereb Blood Flow Metab 15: 960–968.
Green EJ, Pazos AJ, Dietrich WD, McCabe PM, Schneiderman N, Lin B, Busto R, Globus MY-T, Ginsberg MD 1995 Combined postischaemic hypothermia and delayed MK-801 treatment attenuates neurobehavioral deficits associated with transient global ischaemia in rats. Brain Res 702: 145–152.
Colbourne F, Corbett D 1994 Delayed and prolonged post-ischaemic hypothermia is neuroprotective in the gerbil. Brain Res 654: 265–272.
Colbourne F, Corbett D 1995 Delayed postischaemic hypothermia: a six month survival study using behavioral and histological assessments of neuroprotection. J Neurosci 15: 7250–7260.
Yager J, Towfighi J, Vannucci RC 1993 Influence of mild hypothermia on hypoxic-ischemic brain damage in the immature rat. Pediatr Res 34: 525–529.
Thoresen M, Bagenholm R, Loberg EM, Apricena F, Kjellmer I 1996 Posthypoxic cooling of neonatal rats provides protection against brain injury. Arch Dis Child 74: F3–F9.
Sirimanne ES, Blumberg RM, Bossano D, Gunning M, Edwards AD, Gluckman PD, Williams CE 1996 The effect of prolonged modification of cerebral temperature on the outcome after hypoxic-ischemic brain injury in the infant rat. Pediatr Res 39: 591–597.
Reith J, Jorgensen HS, Pedersen PM, Nakayama H, Raaschou HO, Jeppesen LL, Olsen TS 1996 Body temperature in acute stroke: relation to stroke severity, infarct size, mortality, and outcome. Lancet 347: 422–425.
Acknowledgements
The authors thank Richard Aldridge for his invaluable technical assistance.
Author information
Authors and Affiliations
Additional information
Supported by the Medical Research Council, UK, the Wellcome Trust, the Norwegian Research Council, the Laerdal Foundation for Acute Medicine, and the Norwegian Cardiovascular Research Society.
Rights and permissions
About this article
Cite this article
Amess, P., Penrice, J., Cady, E. et al. Mild Hypothermia after Severe Transient Hypoxia-Ischemia Reduces the Delayed Rise in Cerebral Lactate in the Newborn Piglet. Pediatr Res 41, 803–808 (1997). https://doi.org/10.1203/00006450-199706000-00002
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199706000-00002
- Springer Nature America, Inc.
This article is cited by
-
Hypothermie pour la neuroprotection cérébrale de l’encéphalopathie anoxo-ischémique: certitudes et incertitudes
Revue de médecine périnatale (2013)
-
Safety and efficacy of topiramate in neonates with hypoxic ischemic encephalopathy treated with hypothermia (NeoNATI)
BMC Pediatrics (2012)
-
The Efficacy of Hypothermia in Hypoxic-Ischemic Encephalopathy at 18 Mo or More
The Indian Journal of Pediatrics (2012)
-
Patterns of neonatal hypoxic–ischaemic brain injury
Neuroradiology (2010)
-
The TOBY Study. Whole body hypothermia for the treatment of perinatal asphyxial encephalopathy: A randomised controlled trial
BMC Pediatrics (2008)