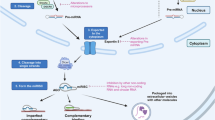
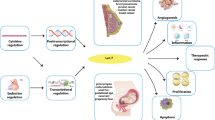
Abstract
The prevalence of papillary thyroid cancer (PTC) has been rising in recent years. Despite its relatively low mortality, PTC frequently metastasizes to lymph nodes and often recurs, posing significant health and economic burdens. The role of iodine in the pathogenesis and advancement of thyroid cancer remains poorly understood. Circular RNAs (circRNAs) are recognized to function as competing endogenous RNAs (ceRNAs) that modulate gene expression and play a role in various cancer stages. Consequently, this research aimed to elucidate the mechanism by which circRNA influences the impact of iodine on PTC. Our research indicates that high iodine levels can exacerbate the malignancy of PTC via the circ_0004851/miR-296-3p/FGF11 axis. These insights into iodine’s biological role in PTC and the association of circRNA with the disease could pave the way for novel biomarkers and potentially effective therapeutic strategies to mitigate PTC progression.
Similar content being viewed by others
Introduction
On a global scale, thyroid cancer (TC) is recognized as the most prevalent endocrine malignancy. Recent decades have seen a steady incline in TC incidence [1], with papillary thyroid cancer (PTC)—prevalent in iodine-sufficient regions like China—constituting over 70% of these cases [2]. PTC, typically highly differentiated, boasts a post-5-year survival rate exceeding 90% [3]. However, recurrence occurs in 10-15% of PTC cases, significantly impacting survival and life quality for these patients.
Iodine significantly influences PTC development, with its role in thyroid cell proliferation and differentiation being well-documented. Abnormal iodine levels, either deficient or excessive, are implicated in thyroid pathology [4]. Epidemiological evidence suggests a higher PTC incidence in iodine-deficient than in iodine-excess regions, indicating iodine’s critical role in thyroid cancer progression [5]. Furthermore, the BRAF V600E gene mutation is the most common genetic mutation in PTC, with an average incidence of about 45% [6]. Interestingly, previous studies have concluded that among the iodine metabolism genes, BRAF V600E is a highly specific target for PTC [7]. Nonetheless, the impact of high iodine levels on existing thyroid cancer and its underlying mechanisms warrant further investigation.
Non-coding RNAs (ncRNAs) is identified as pivotal in tumorigenesis, encompassing various forms such as transfer RNAs, ribosomal RNAs, long ncRNAs (lncRNAs), small ncRNAs—including microRNAs, piRNAs, snoRNAs, snRNAs, exRNAs—and circular RNAs (circRNAs) [8]. CircRNAs, a novel class of ncRNAs, are gaining prominence as clinical biomarkers due to their differential expression in tumors and associations with diagnosis and prognosis [Full size image
Silencing of mir-296-3p reverses the effects of si-circ_0004851 in PTC cells
Considering our hypothesis that circ_0004851 primarily modulates PTC progression by sequestering miR-296-3p, it was crucial to investigate whether miR-296-3p could counteract the impact of si-circ_0004851 on PTC cells. We conducted rescue experiments in TPC-1 and BCPAP cells co-transfected with si-circ_0004851 and si-NC, using a miR-296-3p inhibitor or control vector. qRT-PCR and western blot analyses demonstrated (Fig. 7A-B) that circ_0004851 knockdown in PTC cells resulted in the inhibition of FGF11 expression, while the miR-296-3p inhibitor reversed the inhibitory effect of si-circ_0004851 on FGF11. CCK-8 assessment revealed that exogenous down-regulation of miR-296-3p expression counteracted the growth inhibitory effect of si-circ_0004851 (Fig. 7C). In comparison to the NC group, miR-296-3p inhibition and si-circ_0004851 co-transfection partially rescued the impaired motility of si-circ_0004851 in PTC cell lines, as evidenced by cell scratch migration assays and Transwell invasion assays (Fig. 7C-D). Furthermore, apoptosis assays confirmed that miR-296-3p inhibition, along with si-circ_0004851, mitigated the apoptotic effect of si-circ_0004851 in PTC cells (Fig. 7F). Western blot also showed that miR-296-3p inhibition reversed the up-regulation of si-circ_0004851 on apoptosis-related proteins in PTC cells (Fig. 7G).
Silencing miR-296-3p reverses the effect of si-circ0004851 on PTC cells. A. mRNA expression of miR-296-3p inhibitor FGF11 in si-circ_0004851 or si-NC PTC cells with or without transfection; B. si-circ_0004851 or si-NC PTC cells transfected or did not transfect miR-296-3p inhibitor FGF11 protein levels; C. CCK-8 detection showed that circ_0004851 could eliminate the inhibition of cell growth by down-regulating miR-296-3p; C. Assessment of the ability of cell scratches to migrate; D. Assessment of invasive capacity through the Transwell test; F. Apoptotic capacity was detected by flow cytometry; G. The expressions of apoptosis-related proteins were detected by Western blot
Circ_0004851’s impact on PTC progression through FGF11
Although FGF11 has been identified as an oncogene in a number of cancer types, its function in PTC is unknown. In order to elucidate the association involving endogenous FGF11 expression and PTC pathogenesis, we generated an FGF11 overexpression plasmid and transfected it into circ_0004851-silenced TPC-1 and BCPAP cells. This aimed to investigate whether circ_0004851 influences PTC progression by targeting FGF11. We assessed proliferative, migratory, invasive, and apoptotic capabilities to delve into the effects of FGF11 overexpression on circ_0004851-deficient PTC cells. qRT-PCR and Western blot analyses demonstrated that the FGF11 overexpression plasmid significantly upregulated FGF11 expression. Furthermore, the overexpression of FGF11 upregulated circ_0004851-deficient cellular FGF11 expression (Fig. 8A-B). In addition, we observed that the proliferation, migration, and invasion abilities of cells, as assessed by cck-8, cell scratch, and Transwell assays, were enhanced upon FGF11 overexpression, while apoptosis was inhibited when compared to cells treated with the NC group. Moreover, overexpression of FGF11 in circ_0004851-deficient cells mitigated the inhibitory effects of si-circ_0004851 on proliferation, migration, invasion, and promoted apoptotic effects (Fig. 8C-F). Collectively, these findings suggest that circ_0004851 primarily contributes to PTC progression by targeting FGF11.
Circ0004851 affects PTC progress through FGF11. A. The expression of FGF11 mRNA in PTC cells co-transfected with si-NC + empty vector, si-NC + FGF11 over-expressing plasmid and si-Circ_0004851 + FGF11 over-expressing plasmid was detected by qRT-PCR; B. Western blot detection of FGF11 protein levels in PTC cells; C. CCK-8 assay showed that overexpression of FGF11 could eliminate the effect of Circ-004851 silencing on cell growth; D. Cell scratch detection of the effect of FGF11 overexpression on migration ability; E. Transwell invasion assay to detect the effect of FGF11 overexpression on invasion ability; F. Apoptosis was detected by flow cytometry
Establishment of a nude mouse model to investigate high iodine’s promotion of PTC cell growth in vitro
Elevated levels of iodine are strongly implicated in thyroid cancer development [20]. To elucidate the role of high iodine in PTC progression, we established a xenograft tumor model. As depicted in Fig. 9A-B, the tumor volume and weight of mice in the high-iodine group exceeded those in the control group (p less than 0.05). Notably, the mice’s weight did not significantly differ between the two groups throughout the experiment (Fig. 9C). Furthermore, PCR and Western blot outcomes revealed that circ_0004851 expression elevated, while miR-296-3p expression reduced in the high iodine group. Additionally, FGF11 mRNA and protein expression levels were elevated in the high iodine group (Fig. 9D-E). These outcomes indicate that high iodine promotes tumor growth in the xenograft tumor model and significantly influences the expression of circ_0004851/miR-296-3p/FGF11 in this model.
High iodine promoted tumor growth in xenograft tumor models of PTC cells. A. BCPAP cells were subcutaneously injected into nude mice under exposure to high iodine and tumor weights were measured at the end of the day 29; B-C. Relative tumor volumes and mice weight of different groups monitored every 3 days during treatment with or without high iodine; D. PCR for circ_0004851、miR-296-3p、FGF11 in xenograft tumor models; E. Western blot for FGF11 in xenograft tumor models. *p < 0.05, **p < 0.01, ***p < 0.001