Abstract
Diabetes mellitus, known for its complications, especially vascular complications, is becoming a globally serious social problem. Atherosclerosis has been recognized as a common vascular complication mechanism in diabetes. The diacylglycerol (DAG)–protein kinase C (PKC) pathway plays an important role in atherosclerosis. PKCs can be divided into three subgroups: conventional PKCs (cPKCs), novel PKCs (nPKCs), and atypical PKCs (aPKCs). The aim of this review is to provide a comprehensive overview of the role of the PKCδ pathway, an isoform of nPKC, in regulating the function of endothelial cells, vascular smooth muscle cells, and macrophages in diabetic atherosclerosis. In addition, potential therapeutic targets regarding the PKCδ pathway are summarized.
Video Abstract
Similar content being viewed by others
Introduction
Diabetes mellitus, characterized by abnormally elevated blood glucose levels, is one of the twenty-first century's fastest growing challenges. According to the International Diabetes Federation (IDF), 1 in 10 adults (age 20–79 years; 537 million individuals) had diabetes in 2021, with the number expected to reach 783 million by 2045 [1]. Patients suffer mostly from chronic complications, including macrovascular and microvascular disease. Macrovascular complications result from lesions to the arteries, leading to large vessel obstructions such as coronary artery disease, atherosclerosis, and peripheral vascular disease [2]. Microvascular complications, characterized by microvascular injuries, include retinopathy, nephropathy, and neuropathy. Atherosclerotic cardiovascular disease (ASCVD), which manifests as coronary heart disease, ischemic stroke, peripheral artery disease, and heart failure, remains the leading cause of death and disability among patients with diabetes mellitus [3]. Hyperglycemia is regarded as the most important factor in the mechanism of diabetic complications, and it has been shown to activate several pathways, including the polyol, nonenzymatic glycation, and advanced glycation end product (AGE) pathways, the production of reactive oxygen species (ROS), and the diacylglycerol (DAG)-protein kinase C (PKC) pathway [2].
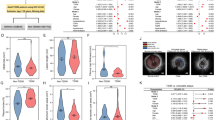
The PKCs are a family of serine/threonine-related protein kinases that play indispensable roles in several signal transduction pathways and cellular functions [2]. PKCδ is a PKC isoform belonging to the novel PKC (nPKC) subgroup that is Ca2+-independent and phospholipid- and DAG-activated [4]. PKCδ was found to be activated in a number of atherosclerotic cardiovascular diseases as well as diabetic complications, indicating that it may be a mediator of diabetes-related atherosclerosis. Atherosclerosis is a complex process involving various types of cells, including endothelial cells (ECs), vascular smooth muscle cells (VSMCs), monocytes/macrophages, and so on. To determine the expression of PKCδ in ECs, VSMCs, and macrophages in human vessels, we stained paraffin sections of a vessel from the amputated limb of a male diabetes patient, with his informed consent (Fig. 1). He experienced pain at rest due to severe arterial atherosclerotic occlusions in the left lower extremity and amputation was indicated. The patient was well informed, and several vessels were collected after amputation. The staining was from a non-occluded artery with thin neointima. Markers of ECs (CD31), VSMCs (α-SMA), and macrophages (CD68) were stained green and the marker of PKCδ was stained red. Although the functions of PKCδ have been discussed in previous reviews, they have not been reviewed in detail [5, 6]. In this review, we summarize the role of PKCδ in regulating the dysfunction of endothelial cells, vascular smooth muscle cells, and monocytes/macrophages in non-DM and DM conditions to provide a comprehensive understanding of the role of PKCδ in diabetic atherosclerosis.
PKCδ, CD31, α-SMA, and CD68 staining in a femoral artery tissue from lower limb of a 60 years diabetes patient who had underwent an amputation surgery (A, B). Representative images of HE staining of vessels. C Positive co-staining of CD31/PKCδ was observed in intimal layer. CD31 shown in green, PKCδ in red, and DAPI in blue. D Positive co-staining of α-SMA/PKCδ was observed in media layer. α-SMA shown in green, PKCδ in red, and DAPI in blue. E Positive co-staining of CD68/PKCδ was observed in neointimal and adventitial layers. CD68 shown in green, PKCδ in red, and DAPI in blue. The magnification scale of HE image was 5X. Arrows show positive colocalized staining. L, lumen; M, media; N, neointima; Adv, adventitia
PKCδ in the dysfunction of endothelial cells
Endothelial cells dysfunction leads to the earliest detectable changes, such as focal permeation, trap**, and physicochemical modification of circulating lipoprotein particles in the sub-endothelial space, and plays a vital role in the pathophysiology of atherosclerosis. Endothelial dysfunction is characterized by impaired endothelium-dependent vasodilation, hyperpermeability, leukocytes adhesion, chronic inflammation, heightened oxidative stress, endothelial-to-mesenchymal transition, and endothelial cells senescence and apoptosis [7].
Healthy endothelium regulates vascular tone and structure and protects vessels from thrombosis [8]. Impaired vascular tone can lead to increased endothelial permeability, platelet aggregation, leukocytes adhesion, and the generation of cytokines. Hyperpermeability can be induced by a variety of cytokines, including vascular endothelial growth factor (VEGF), histamine, and thrombin, as well as other factors, such as high levels of oxidative stress and inflammation [7]. Damage to endothelial barrier integrity leads to lower NO availability, vascular swelling/edema, and abnormal hemostasis. Under pathologic conditions, the expression of adhesion molecules such as VCAM-1, ICAM-1, E-selectin, and MCP-1 is induced by proinflammatory mediators. These adhesion molecules enhance leukocytes adhesion and transmigration while also triggering inflammation, which is at the core of atherosclerosis. Furthermore, heightened oxidative stress facilitates the formation of ox-LDL, activates endothelial cells, upregulates adhesion molecule expression, alters vascular tone, and leads to EC apoptosis [9, In this review, we discussed the role of PKCδ in regulating several pathophysiologic changes of VSMCs, ECs, and monocytes/macrophages in the process of atherosclerotic plaque formation under DM and non-DM conditions. However, both upregulation and downregulation of PKCδ can lead to similar effects (Supplementary table 1). We reviewed literatures focusing on the function of PKCδ in PKCδ-overexpressed mice but found little evidence. Mice with liver-specific overexpression of PKCδ showed decreased insulin signaling, enhanced lipogenic gene expression, and hepatosteatosis [114]. Epidermis-specific overexpression of PKCδ inhibited skin tumor formation [146]. Thus, more high-quality evidence from PKCδ downregulated or overexpressed DM animals is required. In addition, atherosclerosis is a complex inflammatory disease that involves not just those three types of cells, but also lymphocytes, NK cells, dendritic cells, neutrophils, and others. The importance of these cells in the formation of atherosclerotic lesions and of PKCδ needs to be further explored. Calcium dobesilate is a clinically available drug mainly used in the treatment of diabetic retinopathy and deep venous insufficiency. It was also shown to inhibit monocytes differentiation via PKCδ inhibition, indicating a possible role of calcium dobesilate in the treatment of atherosclerosis. Rottlerin and siRNA, the two most commonly used PKCδ inhibitors, have been proven to alleviate the VSMCs, ECs, and monocytes/macrophages dysfunction. Other natural extracts, such as polydatin and curcumin, have also been proven to protect endothelial cells via PKCδ suppression. Their application in clinical practice is also worth investigating.Perspectives
Availability of data and materials
The datasets used and analyzed during the current study are available from the corresponding author on reasonable request.
References
Sun H, et al. IDF Diabetes Atlas: Global, regional and country-level diabetes prevalence estimates for 2021 and projections for 2045. Diabetes Res Clin Pract. 2022;183: 109119.
Geraldes P, King GL. Activation of protein kinase C isoforms and its impact on diabetic complications. Circ Res. 2010;106(8):1319–31.
Low Wang CC, Hess CN, Hiatt WR, Goldfine AB. Clinical update: Cardiovascular disease in diabetes mellitus. Circulation. 2016;133(24):2459–502.
Kikkawa U, Matsuzaki H, Yamamoto T. Protein kinase Cδ(PKC δ): activation mechanisms and functions. J Biochem. 2002;132(6):831–9.
Miao LN, et al. Role and mechanism of PKC-δ for cardiovascular disease: current status and perspective. Front Cardiovasc Med. 2022;9(February):1–16.
Lien CF, Chen SJ, Tsai MC, Lin CS. Potential role of protein kinase C in the pathophysiology of diabetes-associated atherosclerosis. Front Pharmacol. 2021;12:1–12.
Xu S, et al. Endothelial dysfunction in atherosclerotic cardiovascular diseases and beyond: from mechanism to pharmacotherapies. Pharmacol Rev. 2021;73(3):924–67.
Davignon J, Ganz P. Role of endothelial dysfunction in Atherosclerosis. Circulation. 2004;109(23 suppl 1):III–27.
Kattoor AJ, Pothineni NVK, Palagiri D, Mehta JL. Oxidative stress in Atherosclerosis. Curr Atheroscler Rep. 2017;19(11):42.
Förstermann U, **a N, Li H. Roles of vascular oxidative stress and nitric oxide in the pathogenesis of atherosclerosis. Circulation Res. 2017;120(4):713–35.
Paone S, Baxter AA, Hulett MD, Poon IKH. Endothelial cell apoptosis and the role of endothelial cell-derived extracellular vesicles in the progression of atherosclerosis. Cell Mol Life Sci. 2019;76(6):1093–106.
Wu CM, Zheng L, Wang Q, Hu YW. The emerging role of cell senescence in atherosclerosis. Clin Chem Lab Med. 2020;59(1):27–38.
Klymenko K, Novokhatska T, Kizub I, Parshikov A, Dosenko V, Soloviev A. PKC-δ isozyme gene silencing restores vascular function in diabetic rat. J Basic Clin Physiol Pharmacol. 2014;25:1–9.
Ishida K, Matsumoto T, Taguchi K, Kamata K, Kobayashi T. Protein kinase C delta contributes to increase in EP3 agonist-induced contraction in mesenteric arteries from type 2 diabetic Goto-Kakizaki rats. Pflugers Arch. 2012;463(4):593–602.
Mondrinos MJ, et al. Pulmonary endothelial protein kinase C-Delta (PKCδ) regulates neutrophil migration in acute lung inflammation. Am J Pathol. 2014;184(1):200–13.
Ahn JJ, Jung JP, Park SE, Lee M, Kwon B, Cho HR. Involvement of protein kinase C-δ in vascular permeability in acute lung injury. Immune Netw. 2015;15(4):206.
Soroush F, et al. Protein kinase C-Delta (PKCδ) tyrosine phosphorylation is a critical regulator of neutrophil-endothelial cell interaction in inflammation. Shock. 2019;51(5):538–47.
Tang Y, et al. Protein kinase C-delta inhibition protects blood-brain barrier from sepsis-induced vascular damage. J Neuroinflammation. 2018;15(1):1–12.
Kim J-H, Kim JH, Jun H-O, Yu YS, Kim K-W. Inhibition of protein kinase C delta attenuates blood-retinal barrier breakdown in diabetic retinopathy. Am J Pathol. 2010;176(3):1517–24.
Gimbrone MA Jr, García-Cardeña G. Endothelial cell dysfunction and the pathobiology of atherosclerosis. Circ Res. 2016;176(1):139–48.
Motley ED, Eguchi K, Patterson MM, Palmer PD, Suzuki H, Eguchi S. Mechanism of endothelial nitric oxide synthase phosphorylation and activation by thrombin. Hypertension. 2007;49(3):577–83.
Fetterman JL, et al. Restoration of autophagy in endothelial cells from patients with diabetes mellitus improves nitric oxide signaling. Atherosclerosis. 2016;247:207–17.
Bharath LP, et al. Endothelial cell autophagy maintains shear stress-induced nitric oxide generation via glycolysis-dependent purinergic signaling to endothelial nitric oxide synthase. Arterioscler Thromb Vasc Biol. 2017;37(9):1646–56.
Kumar S, Sud N, Fonseca FV, Hou Y, Black SM. Shear stress stimulates nitric oxide signaling in pulmonary arterial endothelial cells via a reduction in catalase activity: Role of protein kinase Cδ. Am J Physiol Lung Cell Mol Physiol. 2010;298(1):L105-16.
Sud N, Black SM. Endothelin-1 impairs nitric oxide signaling in endothelial cells through a protein kinase cδ-dependent activation of STAT3 and decreased endothelial nitric oxide synthase expression. DNA Cell Biol. 2009;28(11):543–53.
Sud N, Kumar S, Wedgwood S, Black SM. Modulation of PKCδ signaling alters the shear stress-mediated increases in endothelial nitric oxide synthase transcription: role of STAT3. Am J Physiol Lung Cell Mol Physiol. 2009;296(3):519–26.
Cosentino F, et al. High glucose causes upregulation of cyclooxygenase-2 and alters prostanoid profile in human endothelial cells: Role of protein kinase C and reactive oxygen species. Circulation. 2003;107(7):1017–23.
Panicker SR, Biswas I, Giri H, Cai X. PKC (Protein Kinase C)-δ modulates at (Antithrombin) signaling in vascular endothelial cells. Arterioscler Thromb Vasc Biol. 2020;4:1748–62.
Khamaisi M, Dahan R, Hamed S, Abassi Z, Heyman SN, Raz I. Role of protein kinase C in the expression of endothelin converting enzyme-1. Endocrinology. 2009;150(3):1440–9.
Park JY, et al. Induction of endothelin-1 expression by glucose: an effect of protein kinase C activation. Diabetes. 2000;49(7):1239–48.
Gaudreault N, Perrin RM, Guo M, Clanton CP, Wu MH, Yuan SY. Counter regulatory effects of PKCbetaII and PKCdelta on coronary endothelial permeability. Arterioscler Thromb Vasc Biol. 2008;28(8):1527–33.
Kim YA, et al. Role of PKCβII and PKCδ in blood-brain barrier permeability during aglycemic hypoxia. Neurosci Lett. 2010;468(3):254–8.
Tinsley JH, Teasdale NR, Yuan SY. Involvement of PKCδ and PKD in pulmonary microvascular endothelial cell hyperpermeability. Am J Physiol Cell Physiol. 2004;286(1):55–61.
**e L, et al. Regulation of thrombin-induced lung endothelial cell barrier disruption by protein kinase C delta. PLoS ONE. 2016;11(7):1–17.
Sheats MK, Sung EJ, Adler KB, Jones SL. In vitro neutrophil migration requires protein kinase C-Delta (δ-PKC)-Mediated Myristoylated Alanine-Rich C-Kinase Substrate (MARCKS) phosphorylation. Inflammation. 2015;38(3):1126–41.
van den Oever IA, Raterman HG, Nurmohamed MT, Simsek S. Endothelial dysfunction, inflammation, and apoptosis in diabetes mellitus. Mediators Inflamm. 2010;2010:1–15.
Rahman A, et al. Protein Kinase C-δ regulates thrombin-induced ICAM-1 gene expression in endothelial cells via activation of p38 mitogen-activated protein kinase. Mol Cell Biol. 2001;21(16):5554–65.
Minami T, Abid RM, Zhang J, King G, Kodama T, Aird WC. Thrombin stimulation of vascular adhesion molecule-1 in endothelial cells is mediated by protein kinase C (PKC)-δ-NF-κB and PKC-ζ-GATA signaling pathways. J Biol Chem. 2003;278(9):6976–84.
Shimamura K, Takashiro Y, Akiyama N, Hirabayashi T, Murayama T. Expression of adhesion molecules by sphingosine 1-phosphate and histamine in endothelial cells. Eur J Pharmacol. 2004;486(2):141–50.
Hampson P, Kavanagh D, Smith E, Wang K, Lord JM, Ed Rainger G. The anti-tumor agent, ingenol-3-angelate (PEP005), promotes the recruitment of cytotoxic neutrophils by activation of vascular endothelial cells in a PKC-δ dependent manner. Cancer Immunol Immunother. 2008;57(8):1241–51.
Kattoor AJ, Pothineni NV, Palagiri D, Mehta JL. Oxidative Stress in Atherosclerosis. Curr Atheroscler Rep. 2017;19(11):42.
Cai W, et al. AGER1 regulates endothelial cell NADPH oxidase-dependent oxidant stress via PKC-delta: implications for vascular disease. Am J Physiol Cell Physiol. 2010;298(3):C624–34.
Monti M, Donnini S, Giachetti A, Mochly-Rosen D, Ziche M. δPKC inhibition or e{open}PKC activation repairs endothelial vascular dysfunction by regulating eNOS post-translational modification. J Mol Cell Cardiol. 2010;48(4):746–56.
Qiao H, et al. Polydatin attenuates H 2 O 2 -induced oxidative stress via PKC pathway. Oxid Med Cell Longev. 2016;2016:1–10.
Lee SE, et al. Upregulation of heme oxygenase-1 as an adaptive mechanism for protection against crotonaldehyde in human umbilical vein endothelial cells. Toxicol Lett. 2011;201(3):240–8.
Souilhol C, Harmsen MC, Evans PC, Krenning G. Endothelial-mesenchymal transition in atherosclerosis. Cardiovasc Res. 2018;114(4):565–77.
Li Z, Jimenez SA. Protein kinase Cδ and c-Abl kinase are required for transforming growth factor β induction of endothelial-mesenchymal transition in vitro. Arthritis Rheum. 2011;63(8):2473–83.
Sun F, Zhou B, Lin X, Duan L. Proteomic analysis identifies nuclear protein effectors in PKC-delta signaling under high glucose-induced apoptosis in human umbilical vein endothelial cells. Mol Med Rep. 2011;4(5):865–72.
Yu C, **ao JH. The Keap1-Nrf2 system: a mediator between oxidative stress and aging. Oxid Med Cell Longev. 2021;2021:1–6.
Niwa K, et al. Roles of protein kinase C δ in the accumulation of P53 and the induction of apoptosis in H2O2-treated bovine endothelial cells. Free Radic Res. 2002;36(11):1147–53.
Kim YR, et al. Apoptosis signal-regulating Kinase1 is inducible by protein kinase Cδ and contributes to phorbol ester-mediated G1 phase arrest through persistent JNK activation. Cell Biochem Biophys. 2011;61(1):199–207.
Yokoi T, et al. Apoptosis signal-regulating kinase 1 mediates cellular senescence induced by high glucose in endothelial cells. Diabetes. 2006;55(6):1660–5.
Vasa M, Breitschopf K, Zeiher AM, Dimmeler S. Nitric oxide activates telomerase and delays endothelial cell senescence. Circ Res. 2000;87(7):540–2.
Libby P, et al. Atherosclerosis. Nat Rev Dis Prim. 2019;5(1):1–18.
Kockx MM, Herman AG. Apoptosis in atherosclerosis: Beneficial or detrimental? Cardiovasc Res. 2000;45(3):736–46.
Yamaguchi H, et al. Altered PDGF-BB-induced p38 MAP kinase activation in diabetic vascular smooth muscle cells: roles of protein kinase C-delta. Arterioscler Thromb Vasc Biol. 2004;24(11):2095–101.
Leitges M, et al. Exacerbated vein graft arteriosclerosis in protein kinase Cδ-null mice. J Clin Invest. 2001;108(10):1505–12.
Liu B, et al. Protein kinase C-δ regulates migration and proliferation of vascular smooth muscle cells through the extracellular signal-regulated kinase 1/2. J Vasc Surg. 2007;45(1):160–8.
Kamiya K, Ryer E, Sakakibara K, Zohlman A, Kent KC, Liu B. Protein kinase C δ activated adhesion regulates vascular smooth muscle cell migration. J Surg Res. 2007;141(1):91–6.
Li C, Wernig F, Leitges M, Hu Y, Xu Q. Mechanical stress-activated PKCdelta regulates smooth muscle cell migration. FASEB J. 2003;17(14):2106–8.
Yamanouchi D, Kato K, Ryer EJ, Zhang F, Liu B. Protein kinase C delta mediates arterial injury responses through regulation of vascular smooth muscle cell apoptosis. Cardiovasc Res. 2010;85(3):434–43.
Mayr M, Siow R, Chung YL, Mayr U, Griffiths JR, Xu Q. Proteomic and metabolomic analysis of vascular smooth muscle cells: role of PKCdelta. Circ Res. 2004;94(10):e87-96.
Fukumoto S, et al. Protein kinase C δ inhibits the proliferation of vascular smooth muscle cells by suppressing G1 cyclin expression. J Biol Chem. 1997;272(21):13816–22.
Bowles DK, Maddali KK, Dhulipala VC, Korzick DH. PKCδ mediates anti-proliferative, pro-apoptic effects of testosterone on coronary smooth muscle. Am J Physiol Cell Physiol. 2007;293(2):805–13.
Lim S, et al. Regulation of mitochondrial morphology by positive feedback interaction between PKCδ and Drp1 in vascular smooth muscle cell. J Cell Biochem. 2015;116(4):648–60.
Hsieh HL, Sun CC, Wang TS, Yang CM. PKC-δ/c-Src-mediated EGF receptor transactivation regulates thrombin-induced COX-2 expression and PGE2 production in rat vascular smooth muscle cells. Biochim Biophys Acta Mol Cell Res. 2008;1783(9):1563–75.
Leng L, Du B, Consigli S, McCaffrey TA. Translocation of protein kinase C-delta by PDGF in cultured vascular smooth muscle cells: inhibition by TGF-beta 1. Artery. 1996;22(3):140–54.
Ginnan R, Singer HA. PKC-δ-dependent pathways contribute to PDGF-stimulated ERK1/2 activation in vascular smooth muscle. Am J Physiol Cell Physiol. 2005;288(6):57–66.
Ramana KV, Friedrich B, Tammali R, West MB, Bhatnagar A, Srivastava SK. Requirement of aldose reductase for the hyperglycemic activation of protein kinase C and formation of diacylglycerol in vascular smooth muscle cells. Diabetes. 2005;54(3):818–29.
Ramana KV, Tammali R, Reddy ABM, Bhatnagar A, Srivastava SK. Aldose reductase-regulated tumor necrosis factor-alpha production is essential for high glucoe-induced vascular smooth muscle cell growth. Endocrinology. 2007;148(9):4371–84.
Reddy ABM, Ramana KV, Srivastava S, Bhatnagar A, Srivastava SK. Aldose reductase regulates high glucose-induced ectodomain shedding of tumor necrosis factor (TNF)-alpha via protein kinase C-delta and TNF-alpha converting enzyme in vascular smooth muscle cells. Endocrinology. 2009;150(1):63–74.
Dangwal S, et al. High glucose enhances thrombin responses via protease-activated receptor-4 in human vascular smooth muscle cells. Arterioscler Thromb Vasc Biol. 2011;31(3):624–33.
Shizukuda Y, Reyland ME, Buttrick PM. Protein kinase C-delta modulates apoptosis induced by hyperglycemia in adult ventricular myocytes. Am J Physiol Heart Circ Physiol. 2002;282(5):H1625–34.
Geraldes P, et al. Activation of PKC-δand SHP-1 by hyperglycemia causes vascular cell apoptosis and diabetic retinopathy. Nat Med. 2009;15(11):1298–306.
Mima A, et al. Glomerular VEGF resistance induced by PKCδ/SHP-1 activation and contribution to diabetic nephropathy. FASEB J. 2012;26(7):2963–74.
Ryer EJ, et al. Protein kinase C delta induces apoptosis of vascular smooth muscle cells through induction of the tumor suppressor p53 by both p38-dependent and p38-independent mechanisms. J Biol Chem. 2005;280(42):35310–7.
Larroque-Cardoso P, et al. Role of protein kinase C δ in ER stress and apoptosis induced by oxidized LDL in human vascular smooth muscle cells. Cell Death Dis. 2013;4(2):1–10.
Yue J, López JM. Understanding MAPK signaling pathways in apoptosis. Int J Mol Sci. 2020;21(7):2346.
Igarashi M, et al. Glucose or diabetes activates p38 mitogen-activated protein kinase via different pathways. J Clin Invest. 1999;103(2):185–95.
Yoshida K, Liu H, Miki Y. Protein kinase C δ regulates Ser46 phosphorylation of p53 tumor suppressor in the apoptotic response to DNA damage. J Biol Chem. 2006;281(9):5734–40.
Kato K, et al. Caspase-mediated protein kinase C-δ cleavage is necessary for apoptosis of vascular smooth muscle cells. Am J Physiol Hear Circ Physiol. 2009;297(6):2253–61.
Wang Q, Liu Z, Ren J, Morgan S, Assa C, Liu B. Receptor-interacting protein kinase 3 contributes to abdominal aortic aneurysms via smooth muscle cell necrosis and inflammation. Circ Res. 2015;116(4):600–11.
Hall JL, Matter CM, Wang X, Gibbons GH. Hyperglycemia inhibits vascular smooth muscle cell apoptosis through a protein kinase C-dependent pathway. Circ Res. 2000;87(7):574–80.
Seimon T, Tabas I. Mechanisms and consequences of macrophage apoptosis in atherosclerosis. J Lipid Res. 2009;50:S382–7.
Li Q, et al. Regulation of Macrophage Apoptosis and Atherosclerosis by Lipid-Induced PKCδ Isoform Activation. Circ Res. 2017;121(10):1153–67.
Jialal I, Machha A, Devaraj S. Small interfering-RNA to protein kinase C-delta reduces the proinflammatory effects of human C-reactive protein in biobreeding diabetic rats. Horm Metab Res. 2013;45(4):326–8.
Szilagyi K, et al. PKCδ is dispensible for oxLDL uptake and foam cell formation by human and murine macrophages. Cardiovasc Res. 2014;104(3):467–76.
Dasu MR, Devaraj S, Zhao L, Hwang DH, Jialal I. High glucose induces toll-like receptor expression in human monocytes. Diabetes. 2008;57(11):3090–8.
Tiwari RL, et al. PKC -IRAK1 axis regulates oxidized LDL-induced IL-1 production in monocytes. J Lipid Res. 2014;55(7):1226–44.
Hsu HY, Chu LC, Hua KF, Chao LK. Heme oxygenase-1 mediates the anti-inflammatory effect of curcumin within LPS-stimulated human monocytes. J Cell Physiol. 2008;215(3):603–12.
Roy A, Saqib U, Wary K, Baig MS. Macrophage neuronal nitric oxide synthase (NOS1) controls the inflammatory response and foam cell formation in atherosclerosis. Int Immunopharmacol. 2020;83:106382.
Huang H, et al. Induction of inducible nitric oxide synthase (iNOS) expression by oxLDL inhibits macrophage derived foam cell migration. Atherosclerosis. 2014;235(1):213–22.
Detmers PA, et al. Deficiency in inducible nitric oxide synthase results in reduced atherosclerosis in apolipoprotein E-deficient mice. J Immunol. 2000;165(6):3430–5.
Kuhlencordt PJ, Chen J, Han F, Astern J, Huang PL. Genetic deficiency of inducible nitric oxide synthase reduces atherosclerosis and lowers plasma lipid peroxides in apolipoprotein E-knockout mice. Circulation. 2001;103(25):3099–104.
Leppänen T, Korhonen R, Laavola M, Nieminen R, Tuominen RK, Moilanen E. Down-regulation of protein kinase Cδ inhibits inducible nitric oxide synthase expression through IRF1. PLoS ONE. 2013;8(1): e52741.
Wu C-H, Chang C-H, Lin H-C, Chen C-M, Lin C-H, Lee H-M. Role of protein kinase C in BSA-AGE-mediated inducible nitric oxide synthase expression in RAW 264.7 macrophages. Biochem Pharmacol. 2003;66(2):203–12.
Hua KF, Wang SH, Dong WC, Lin CY, Ho CL, Wu TH. High glucose increases nitric oxide generation in lipopolysaccharide-activated macrophages by enhancing activity of protein kinase C-α/δ and NF-κB. Inflamm Res Off J Eur Histamine Res Soc. 2012;61(10):1107–16.
Bhatt KH, Pandey RK, Dahiya Y, Sodhi A. Protein kinase Cδ and protein tyrosine kinase regulate peptidoglycan-induced nuclear factor-κB activation and inducible nitric oxide synthase expression in mouse peritoneal macrophages in vitro. Mol Immunol. 2010;47(4):861–70.
Moore KJ, Tabas I. Macrophages in the pathogenesis of atherosclerosis. Cell. 2011;145(3):341–55.
Fan H-C, Fernández-Hernando C, Lai J-H. Protein kinase C isoforms in atherosclerosis: Pro- or anti-inflammatory? Biochem Pharmacol. 2014;88(2):139–49.
Jablonski KA, et al. Novel markers to delineate murine M1 and M2 macrophages. PLoS ONE. 2015;10(12): e0145342.
Feldmann K, et al. Decreased M1 macrophage polarization in dabigatran-treated Ldlr-deficient mice: implications for atherosclerosis and adipose tissue inflammation. Atherosclerosis. 2019;287:81–8.
Zhou L, et al. LincRNA-p21 knockdown reversed tumor-associated macrophages function by promoting MDM2 to antagonize* p53 activation and alleviate breast cancer development. Cancer Immunol Immunother. 2020;69(5):835–46.
Huang S-L, Chen P-Y, Wu M-J, Tai M-H, Ho C-T, Yen J-H. Curcuminoids modulate the PKCδ/NADPH oxidase/reactive oxygen species signaling pathway and suppress matrix invasion during monocyte-macrophage differentiation. J Agric Food Chem. 2015;63(40):8838–48.
Tsai C-S, et al. Thrombomodulin regulates monocye differentiation via PKCδ and ERK1/2 pathway in vitro and in atherosclerotic artery. Sci Rep. 2016;6(1):38421.
Njau F, Haller H. Calcium dobesilate modulates PKCδ-NADPH Oxidase- MAPK-NF-κB signaling pathway to reduce CD14, TLR4, and MMP9 expression during monocyte-to-macrophage differentiation: potential therapeutic implications for atherosclerosis. Antioxidants. 2021;10(11):1798.
Chen J-S, Greenberg AS, Wang S-M. Oleic acid-induced PKC isozyme translocation in RAW 264.7 macrophages. J Cell Biochem. 2002;86(4):784–91.
Ma H-T, et al. Protein kinase C β and δ isoenzymes mediate cholesterol accumulation in PMA-activated macrophages. Biochem Biophys Res Commun. 2006;349(1):214–20.
Lin C-S, et al. PKCδ signalling regulates SR-A and CD36 expression and foam cell formation. Cardiovasc Res. 2012;95(3):346–55.
Yakubenko VP, Hsi LC, Cathcart MK, Bhattacharjee A. From macrophage interleukin-13 receptor to foam cell formation. J Biol Chem. 2013;288(4):2778–88.
Wang Y, Oram JF. Unsaturated fatty acids phosphorylate and destabilize ABCA1 through a protein kinase C delta pathway. J Lipid Res. 2007;48(5):1062–8.
Ku CS, Park Y, Coleman SL, Lee J. Unsaturated fatty acids repress expression of ATP binding cassette transporter A1 and G1 in RAW 264.7 macrophages. J Nutr Biochem. 2012;23(10):1271–6.
Vogl F, et al. Role of protein kinase C δ in apoptotic signaling of oxidized phospholipids in RAW 264.7 macrophages. Biochim Biophys Acta Mol Cell Biol Lipids. 2016;1861(4):320–30.
Bezy O, et al. PKCδ regulates hepatic insulin sensitivity and hepatosteatosis in mice and humans. J Clin Invest. 2011;121(6):2504–17.
Ai D, et al. Regulation of hepatic LDL receptors by mTORC1 and PCSK9 in mice. J Clin Invest. 2012;122(4):1262–70.
Choi H, et al. Monosialyl ganglioside GM3 decreases apolipoprotein B-100 secretion in liver cells. J Cell Biochem. 2017;118(8):2168–81.
Kong W, et al. Berberine is a novel cholesterol-lowering drug working through a unique mechanism distinct from statins. Nat Med. 2004;10(12):1344–51.
Liang H, Wang Y. Berberine alleviates hepatic lipid accumulation by increasing ABCA1 through the protein kinase C δ pathway. Biochem Biophys Res Commun. 2018;498(3):473–80.
Mayr M, et al. Loss of PKC-δ alters cardiac metabolism. Am J Physiol Circ Physiol. 2004;287(2):H937–45.
Hansson GK, Hermansson A. The immune system in atherosclerosis. Nat Immunol. 2011;12(3):204–12.
Miyamoto A, et al. Increased proliferation of B cells and auto-immunity in mice lacking protein kinase Cδ. Nature. 2002;416(6883):865–9.
Mecklenbräuker I, Saijo K, Zheng N, Leitges M, Tarakhovsky A. Protein kinase Cδ controls self-antigen-induced B-cell tolerance. Nature. 2002;416(6883):860–5.
Kuehn HS, et al. Loss-of-function of the protein kinase C δ (PKCδ) causes a B-cell lymphoproliferative syndrome in humans. Blood. 2013;121(16):3117–25.
Hamdorf M, Berger A, Schüle S, Reinhardt J, Flory E. PKCδ-Induced PU.1 phosphorylation promotes hematopoietic stem cell differentiation to dendritic cells. Stem Cells. 2011;29(2):297–306.
Majewski M, Bose TO, Sillé FCM, Pollington AM, Fiebiger E, Boes M. Protein kinase C delta stimulates antigen presentation by Class II MHC in murine dendritic cells. Int Immunol. 2007;19(6):719–32.
Singla B, Ghoshal P, Lin H, Wei Q, Dong Z, Csányi G. PKCδ-mediated Nox2 activation promotes fluid-phase pinocytosis of antigens by immature dendritic cells. Front Immunol. 2018;9:537.
Zhu M, Zhou J, Zhou D, Yang K, Li B, Cheng Z. The CCCH-type zinc finger antiviral protein relieves immunosuppression of T cells induced by avian leukosis virus subgroup J via the NLP–PKC-δ–NFAT pathway. J Virol. 2022;96(2):e0134421.
Bertho N. MHC class II-mediated apoptosis of mature dendritic cells proceeds by activation of the protein kinase C-delta isoenzyme. Int Immunol. 2002;14(8):935–42.
Scheel-Toellner D, et al. Inhibition of T cell apoptosis by IFN-β rapidly reverses nuclear translocation of protein kinase C-δ. Eur J Immunol. 1999;29(8):2603–12.
Wei SY, Lin TE, Wang WL, Lee PL, Tsai MC, Chiu JJ. Protein kinase C-δ and -β coordinate flow-induced directionality and deformation of migratory human blood T-lymphocytes. J Mol Cell Biol. 2014;6(6):458–72.
Valacchi G, et al. Rottlerin exhibits antiangiogenic effects in vitro. Chem Biol Drug Des. 2011;77(6):460–70.
Solà-Adell C, et al. Calcium dobesilate prevents neurodegeneration and vascular leakage in experimental diabetes. Curr Eye Res. 2017;42(9):1273–86.
Hempel A, et al. High glucose concentrations increase endothelial cell permeability via activation of protein kinase C alpha. Circ Res. 1997;81(3):363–71.
Devaraj S, Venugopal SK, Singh U, Jialal I. Hyperglycemia induces monocytic release of interleukin-6 via induction of protein kinase C-α and -β. Diabetes. 2005;54(1):85–91.
Mehta NN, et al. Selective PKC beta inhibition with ruboxistaurin and endothelial function in type-2 diabetes mellitus. Cardiovasc Drugs Ther. 2009;23(1):17–24.
Kong L, et al. PKCβ promotes vascular inflammation and acceleration of atherosclerosis in diabetic ApoE null mice. Arterioscler Thromb Vasc Biol. 2013;33(8):1779–87.
Durpès M-C, et al. PKC-β activation inhibits IL-18-binding protein causing endothelial dysfunction and diabetic atherosclerosis. Cardiovasc Res. 2015;106(2):303–13.
Wu Y, et al. Protein kinase C β inhibitor LY333531 attenuates intercellular adhesion molecule-1 and monocyte chemotactic protein-1 expression in the kidney in diabetic rats. J Pharmacol Sci. 2006;101(4):335–43.
Xu Y, Wang S, Feng L, Zhu Q, **ang P, He B. Blockade of PKC-beta protects HUVEC from advanced glycation end products induced inflammation. Int Immunopharmacol. 2010;10(12):1552–9.
Ren J, et al. Novel paracrine functions of smooth muscle cells in supporting endothelial regeneration following arterial injury. Circ Res. 2019;124(8):1253–65.
Lee WJ, et al. M2 macrophage polarization mediates anti-inflammatory effects of endothelial nitric oxide signaling. Diabetes. 2015;64(8):2836–46.
Van Hove CE, Van Der Donckt C, Herman AG, Bult H, Fransen P. Vasodilator efficacy of nitric oxide depends on mechanisms of intracellular calcium mobilization in mouse aortic smooth muscle cells. Br J Pharmacol. 2009;158(3):920–30.
Dubey RK, Jackson EK, Lüscher TF. Nitric oxide inhibits angiotensin II-induced migration of rat aortic smooth muscle cell. Role of cyclic-nucleotides and angiotensin1 receptors. J Clin Invest. 1995;96(1):141–9.
Ren J, et al. Novel paracrine functions of smooth muscle cells in supporting endothelial regeneration following arterial injury. 2019.
Matesanz N, et al. Linoleic acid increases monocyte chemotaxis and adhesion to human aortic endothelial cells through protein kinase C- and cyclooxygenase-2-dependent mechanisms. J Nutr Biochem. 2012;23(6):685–90.
Reddig PJ, et al. Transgenic mice overexpressing protein kinase Cdelta in the epidermis are resistant to skin tumor promotion by 12-O-tetradecanoylphorbol-13-acetate. Cancer Res. 1999;59(22):5710–8.
Acknowledgements
None.
Funding
This research was supported by National Natural Science Foundation of China (NO.82000729).
Author information
Authors and Affiliations
Contributions
P.Q. and C.H. analyzed and interpreted the patient data and reviewed the manuscript. P.Q., C.H. and P.Y. were the major contributors in writing the manuscript. Q.L., Y.L. and C.C. designed this study and interpreted the patient data. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Ethics approval and consent to participate
The Ethical Committee of Wuhan Union Hospital has approved this study. Informed consent was obtained from this patient. The informed consent of the participant was acquired.
Consent for publication
Written informed consent to publish this case was obtained from study participant. Proof of consent to publish from study participant can be requested at any time.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Additional file 1:
Supplementary table 1. PKCδ regulates cellular functions under non-DM and DM conditions.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Qin, P., He, C., Ye, P. et al. PKCδ regulates the vascular biology in diabetic atherosclerosis. Cell Commun Signal 21, 330 (2023). https://doi.org/10.1186/s12964-023-01361-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12964-023-01361-4