Abstract
Background
Gestational diabetes mellitus (GDM) threatens GDM mothers and their offspring’s health and breastfeeding is one of the most effective ways to decrease the risk. However, the prevalence of breastfeeding among GDM mothers is far from optimal and how GDM mothers develop their feeding behavior is still unclear. Thus, this study aimed to explore the formation of GDM mothers’ breastfeeding behaviors based on the health belief model (HBM).
Methods
A questionnaire survey was conducted on 324 GDM mothers who have given birth within 6 months from January 1 to February 6, 2022. According to HBM, GDM mothers’ knowledge, the perceived threat from GDM, the perceived value of breastfeeding, self-efficacy, social support and GDM mothers’ breastfeeding behavior were measured. Exclusive breastfeeding (EBF) was defined as an infant who received only breast milk in the past 24 h before the survey. Structural equation modeling (SEM) was applied to explore how GDM mothers form their breastfeeding behaviors based on HBM.
Results
The prevalence of EBF among GDM mothers was 33.95%. GDM mothers had limited knowledge of GDM (average 63.14% correct answer to 7 questions), especially poor on the long-term effect of GDM (39.81%) and protective effect of breastfeeding (34.57%-45.99%). Although GDM mothers showed high perceived benefits (Mean: 3.35, SD: 0.46), high self-efficacy (Mean: 3.43, SD: 0.97) and high level of social support for breastfeeding (Mean: 3.74, SD: 0.74), the various barriers (Mean: 2.20, SD: 0.47) hindered their success in EBF. The SEM results showed that a higher level of social support and more self-efficacy of breastfeeding resulted in a higher likelihood of EBF, while the higher level of knowledge of GDM, perceived higher barriers and benefits of breastfeeding and higher susceptibility to GDM consequences led to less EBF.
Conclusion
To promote EBF, physicians’ education, emphasizing the protective effect of breastfeeding and how to correct breastfeeding, is highly recommended. In addition, social support for GDM mothers is also important to reduce their barriers to breastfeeding and help enhance self-efficacy in breastfeeding.
Similar content being viewed by others
Introduction
As an important type of diabetes, Gestational Diabetes Mellitus (GDM) is a condition of glucose intolerance develo** during pregnancy. According to International Diabetes Federation (IDF), 17% of the maternal population (aged 21–49 years old) suffered from GDM worldwide in 2021, affecting 21 million newborns [1]. The prevalence of the maternal population suffering from GDM during 2012–2015 in China was 17.5%, which showed an increasing trend in recent years [2].
Although GDM resolves after delivery for the majority of women, it is not uncommon for mothers and their offspring to suffer from multiple long-term health outcomes [3,4,5,8]. In addition, breastfeeding has been reported to be associated with a reduced risk of obesity and diabetes mellitus in GDM mothers’ offspring [9, 10]. Thus, GDM mothers are supposed to insist on breastfeeding to mitigate the health risks for themselves and their offspring.
However, the prevalence of breastfeeding among GDM mothers was far from optimal around the world, with 34.8% of GDM mothers exclusively breastfeeding (EBF) their infants which was far less than the target of 50% of the recommended criteria from the World Health Organization [11, 12]. The prevalence of exclusive breastfeeding (EBF) in infants under 6 months was 29.2% according to a national survey in China and the prevalence was lower in GDM mothers [13].
However, GDM mothers’ formation and decision-making process regarding their feeding behavior was still unclear. Existing studies concentrated on healthy mothers and found that pathological factors [14], psychological factors [13], knowledge of breastfeeding [15], perceived barriers to breastfeeding [16], self-efficacy [17], social support [16] and personal characteristics [12, 15] was associated with maternal breastfeeding intention and actual behavior. However, this is not the situation for GDM mothers [18,19,20]. It was shown that GDM mothers were at greater risk of delayed lactation initiation [21] and higher risk of adverse outcomes from GDM (such as neonatal hypoglycemia, macrosomia and cesarean section) [22], which put more burden and barriers compared with healthy mothers. Studies also found that mothers with GDM required more social support from professionals and their families and more self-efficacy in breastfeeding to insist on breastfeeding compared with mothers without GDM [16, 3).
Regarding the perceived value of breastfeeding, respondents commonly reported perceived the benefits of breastfeeding (3.35 ± 0.46) (Table 3), agreeing that breastfeeding is nutritious and safe and can enhance the parent–child bond and improve the child’s immunity (Mean score > 3.24, SD: 0.49–0.73). However, maternal awareness of the benefits of breastfeeding to reduce the future diabetes of themselves (3.06 ± 0.75) and their child (3.04 ± 0.76) was insufficient (Supplementary S3). On the other hand, respondents reported a high level of perceived barriers to breastfeeding (2.20 ± 0.47). Insufficient breast milk supply, believing that formula milk could provide the same nutrition as breast milk, and the impact of breastfeeding on daily life were considered important barriers to breastfeeding (Mean score > 2.3, SD: 0.78–0.93). In contrast, neonatal jaundice and breast distension engorgement were not major obstacles to breastfeeding (Mean score < 2.3, SD: 0.63–0.67).
Generally, respondents showed a high level of self-efficacy in breastfeeding (3.43 ± 0.97) (Table 3) and received a high level of social support from families, friends and society (3.74 ± 0.74). The details of responses could be found in supplementary S3.
Formation of breastfeeding behavior based on HBM
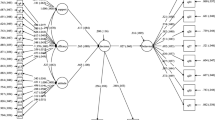
The SEM confirmed the theoretical framework for the breastfeeding behavior of GDM based on HBM (Fig. 3) with an excellent model fit index (RMESA = 0.033, CFI = 0.969, TLI = 0.965, WRME≈1 (1.087)).
Higher knowledge scores were found to be linked with fewer perceived barriers (β = -0.154, p = 0.034) and more perceived benefits (β = 0.375, p < 0.0001) of breastfeeding. It was also associated with a higher level of perceived severity (β = 0.253, p = 0.010), but not significantly related to higher perceived susceptibility (p = 0.697) of GDM long-term consequences. Moreover, a higher level of social support was associated with higher perceived benefits (β = 0.331, p < 0.0001) and fewer perceived barriers (β = -0.370, p < 0.0001).
Furthermore, higher perceived barriers (β = -0.636, p < 0.0001), higher perceived susceptibility (β = -0.157, p = 0.005) and less level of social support (β = 0.127, p = 0.006) were associated with GDM mothers’ less self-efficacy of breastfeeding. Respondents who showed higher self-efficacy (β = 0.661, p < 0.0001) and perceived less benefit of breastfeeding (β = -0.329, p < 0.0001) were more likely to breastfeed the newborns.
To explore whether the relationship of breastfeeding behavior based on HBM varied between subgroups of mothers. Respondents’ characteristics (such as age, mode of delivery, and history of smoking) were further included as covariates. Age, genetic history of diabetes, drinking history, education level, parity, working status, age of neonatal, and occupation were found to be significantly associated with GDM mothers’ perceived health belief towards breastfeeding. (Details see Supplementary S4).
In sum, knowledge of GDM had indirect effects on breastfeeding via changing mothers’ perceived benefits and barriers of breastfeeding and the total effect is negative (total effect: -0.030). GDM mothers’ perceived barriers to breastfeeding (total effect: -0.303), perceived susceptibility of GDM long-term consequences (total effect: -0.104), and reception of social support (total effect: 0.137) were able to influence their breastfeeding behaviors via changing self-efficacy. However, only an increase in social support can result in a higher likelihood of GDM mothers’ breastfeeding. Finally, mothers’ self-efficacy (total effect: 0.596) and perceived benefits of breastfeeding (total effect: -0.372) directly influenced their feeding behaviors.
Discussion
Main findings
The study adopted HBM to explore how GDM mothers form their feeding behaviors as well as its potential determinants. It seemed that GDM mothers showed a relatively low rate of breastfeeding and they commonly did not recognize the long-term effect of GDM and the protective effect of breastfeeding on themselves and their offspring. Although GDM mothers showed high self-efficacy and a high level of social support for breastfeeding, the various barriers hindered their success in the such feeding patterns. Based on the well-fitting SEM results, it was shown that knowledge of GDM can shape one’s perceived benefits and barriers of EBF and the perceived severity of GDM. Perceived barriers to breastfeeding and perceived susceptibility and social support may alter feeding behaviors by changing GDM mothers’ self-efficacy. Perceived benefits and self-efficacy of breastfeeding were identified as two main significant predictors of EBF.
Comparison to existing studies
Breastfeeding behavior
Despite the well-known importance of breastfeeding for mothers with GDM and their offspring, few studies had reported the rate of EBF among GDM mothers in China. The prevalence of EBF in this study among mothers with GDM was 33.95%, which was consistent with results from western China, in which a prevalence of EBF of 36.9% in mothers with GDM was identified (at 6 months postpartum) [ Mothers with GDM showed a low rate of breastfeeding and they commonly did not recognize the long-term effect of GDM and the protective effect of breastfeeding on themselves and their offspring. Although GDM mothers showed high self-efficacy and a high level of social support for breastfeeding, the various barriers hindered their success in the such feeding pattern. During the formation of feeding behaviors, GDM mothers’ self-efficacy, perceived benefits and barriers of breastfeeding, perceived severity of GDM long-term consequence, knowledge of GDM and social support played roles. To improve EBF for GDM mothers, physicians’ education, emphasizing the protecting effect of breastfeeding and how to correct breastfeeding, is highly recommended. In addition, social support for GDM mothers is also important to reduce their barriers to breastfeeding and help enhance self-efficacy in breastfeeding.Conclusion
Availability of data and materials
The datasets used and analyzed during the current study are available from the corresponding author on reasonable requests.
Abbreviations
- GDM:
-
Gestational Diabetes Mellitus
- HBM:
-
Health Belief Model
- EBF:
-
Exclusive Breastfeeding
- IDF:
-
International Diabetes Federation
- CAD:
-
Cardiovascular Disease
- BSES-SF:
-
Breastfeeding Self-Efficacy Scale-Short Form
- CFA:
-
Confirmatory Factor Analysis
- CFI:
-
Comparative Fit Index
- TLI:
-
Tucker-Lewis Index
- WRMR:
-
Weighted Root Mean Square Residual
- OGTT:
-
Oral Glucose Tolerance Test
- WHO:
-
World Health Organization
References
International Diabetes Federation E. IDF Diabetes Atlas 10th edition 2021 [Available from: https://diabetesatlas.org/atlas/tenth-edition/.
Guan H, Shang L. the prevalence of gestational diabetes mellitus. Chin J Prat Gynecol Obstetr. 2015;31(01):91–4.
Metzger BE. Long-term outcomes in mothers diagnosed with gestational diabetes mellitus and their offspring. Clin Obstet Gynecol. 2007;50(4):972–9.
Zhu Y, Zhang C. Prevalence of gestational diabetes and risk of progression to type 2 diabetes: a global perspective. Curr Diab Rep. 2016;16(1):7.
Pastore I, Chiefari E, Vero R, Brunetti A. Postpartum glucose intolerance: an updated overview. Endocrine. 2018;59(3):481–94.
Buchanan TA, **ang AH, Page KA. Gestational diabetes mellitus: risks and management during and after pregnancy. Nat Rev Endocrinol. 2012;8(11):639–49.
West NA, Crume TL, Maligie MA, Dabelea D. Cardiovascular risk factors in children exposed to maternal diabetes in utero. Diabetologia. 2011;54(3):504–7.
Gunderson EP. Lactation and progression to type 2 diabetes mellitus after gestational diabetes mellitus. Ann Intern Med. 2016;165(4):299–300.
AmorimRde J, Coelho AF, de Lira PI, Lima MC. Is breastfeeding protective for blood pressure in schoolchildren? A cohort study in northeast Brazil. Breast Med: J Acad Breast Med. 2014;9(3):149–56.
Much D, Beyerlein A, Roßbauer M, Hummel S, Ziegler AG. Beneficial effects of breastfeeding in women with gestational diabetes mellitus. Mol Metab. 2014;3(3):284–92.
Trout KK, Averbuch T, Barowski M. Promoting breastfeeding among obese women and women with gestational diabetes mellitus. Curr Diab Rep. 2011;11(1):7–12.
Jirakittidul P, Panichyawat N, Chotrungrote B, Mala A. Prevalence and associated factors of breastfeeding in women with gestational diabetes in a University Hospital in Thailand. Int Breastfeed J. 2019;14:34.
Duan Y, Yang Z, Bi Y, Wang J, Pang X, Jiang S, et al. What are the determinants of low exclusive breastfeeding prevalence in China? A cross-sectional study. Matern Child Nutr. 2022;18(2): e13324.
Doughty KN, Taylor SN. Barriers and benefits to breastfeeding with gestational diabetes. Semin Perinatol. 2021;45(2): 151385.
Wang Y, You HX, Luo BR. Exploring the breastfeeding knowledge level and its influencing factors of pregnant women with gestational diabetes mellitus. BMC Pregnancy Childbirth. 2020;20(1):723.
Matsunaga M, Kataoka Y, Igarashi Y, Fukui T, Imura M, Horiuchi S. Breastfeeding support and barriers to women with gestational diabetes mellitus: a nationwide cross-sectional survey of hospitals in Japan. BMC Pregnancy Childbirth. 2021;21(1):555.
Kim Y, Lee JL, Jang IS, Park S. Knowledge and health beliefs of gestational diabetes mellitus associated with breastfeeding intention among pregnant women in Bangladesh. Asian Nurs Res. 2020;14(3):144–9.
Haile ZT, Oza-Frank R, Chertok IR, Passen N. Association between history of gestational diabetes and exclusive breastfeeding at hospital discharge. J Hum Lact : J Int Lact Consult Assoc. 2016;32(3):Np36-43.
Haile ZT, Chertok IRA, Chavan BB, Teweldeberhan AK, Stocum R. Combined influence of gestational diabetes and gestational weight gain on exclusive breastfeeding. Breast Med : J Acad Breastfeeding Med. 2019;14(8):538–50.
Oza-Frank R, Moreland JJ, McNamara K, Geraghty SR, Keim SA. Early lactation and infant feeding practices differ by maternal gestational diabetes history. J Human Lact : J Int Lact Consult Asso. 2016;32(4):658–65.
Mullen AJ, O’Connor DL, Hanley AJ, Piedimonte G, Wallace M, Ley SH. Associations of metabolic and obstetric risk parameters with timing of lactogenesis II. Nutrients. 2022;14(4):876.
Hartling L, Dryden DM, Guthrie A, Muise M, Vandermeer B, Donovan L. Diagnostic thresholds for gestational diabetes and their impact on pregnancy outcomes: a systematic review. Diabet Med. 2014;31(3):319–31.
You H, Lei A, **ang J, Wang Y, Luo B, Hu J. Effects of breastfeeding education based on the self-efficacy theory on women with gestational diabetes mellitus: A CONSORT-compliant randomized controlled trial. Medicine (Baltimore). 2020;99(16): e19643.
Park S, Lee JL, In Sun J, Kim Y. Knowledge and health beliefs about gestational diabetes and healthy pregnancy’s breastfeeding intention. J Clin Nurs. 2018;27(21–22):4058–65.
Wayne W. LaMorte. Behavior Change Model – Health Belief Model (HBM) 2019 [Available from: https://sphweb.bumc.bu.edu/otlt/MPH-Modules/SB/BehavioralChangeTheories/BehavioralChangeTheories2.html.
Qian P, Duan L, Lin R, Du X, Wang D, Liu C, et al. How breastfeeding behavior develops in women with gestational diabetes mellitus: A qualitative study based on health belief model in China. Front Endocrinol (Lausanne). 2022;13:955484.
Wong MCS, Wong ELY, Huang J, Cheung AWL, Law K, Chong MKC, et al. Acceptance of the COVID-19 vaccine based on the health belief model: a population-based survey in Hong Kong. Vaccine. 2021;39(7):1148–56.
DiMillo J, Hall NC, Ezer H, Schwarzer R, Körner A. The Berlin social support scales: validation of the received support scale in a Canadian sample of patients affected by melanoma. J Health Psychol. 2019;24(13):1785–95.
Ip WY, Gao LL, Choi KC, Chau JP, **ao Y. The short form of the breastfeeding self-efficacy scale as a prognostic factor of exclusive breastfeeding among Mandarin-speaking Chinese mothers. J Hum Lact : J Int Lact Consult Assoc. 2016;32(4):711–20.
China NhCotPsRo. Diagnosis of gestational diabetes mellitus 2011 [Available from: http://www.nhc.gov.cn/wjw/s9494/201107/d3c26b9076d445c09b162ad1d0f01dc0.shtml.
World Health Organization. Indicators for assessing infant and young child feeding practices: definitions and measurement methods. 2021. Avaliable from: https://www.who.int/publications/i/item/9789240018389.
Zong X, Wu H, Zhao M, Magnussen CG, ** B. Global prevalence of WHO infant feeding practices in 57 LMICs in 2010–2018 and time trends since 2000 for 44 LMICs. EClinicalMedicine. 2021;37: 100971.
China NHCotPsRo. Notice on publication of Action Plan for Breastfeeding Promotion (2021–2025) 2021 [updated 2021–11–23. Available from: http://www.nhc.gov.cn/fys/s3585/202111/96aa8421ae0045708f3f06e776355193.shtml.
Prabhu J K, Deepthi Kondamuri S, Samal S, Sen M. Knowledge of gestational diabetes mellitus among pregnant women in a semiurban hospital - A cross -sectional study. Clin Epidemiol Glob Health. 2021;12:100854.
Shriraam V, Rani MA, Sathiyasekaran BW, Mahadevan S. Awareness of gestational diabetes mellitus among antenatal women in a primary health center in South India. Ind J Endocrinol Metab. 2013;17(1):146–8.
Gesa G, Sasikala T, Remya C. A study to assess the knowledge regarding gestational diabetes mellitus among pregnant mothers and self care practice of gestational diabetes mellitus management among mothers with diabetes in pregnancy attending selected hospitals of Kottayam District. Medico Legal Update. 2021;21(2):539–42.
Kumari K, Vyas H, Singh P, Thirunavukkarasu D. Knowledge and lifestyle modification regarding gestational diabetes mellitus among antenatal mothers at a tertiary care teaching hospital. Nurs Midwifery Res J. 2021;17(1):20–30.
Zarina Binti Haron NMJ, Salimah Japar, Santhi Yew Roan Nee, Azura Abdul Halain, Kim Geok Sok, Kim Lam So. Knowledge of gestational diabetes mellitus among antenatal women in obstetrics and gynaecology clinic, public hospital Malaysia. J Cardiovasc Dis Res. 2021;12(2):260–5.
Bhavadharini B DM, Nallaperumal S, Anjana RM, Mohan V. Knowledge about gestational diabetes mellitus amongst pregnant women in South Tamil Nadu.: J Diabetol [serial online]; 2017 [Available from: https://www.journalofdiabetology.org/text.asp?2017/8/1/22/205980.
Zera CA, Nicklas JM, Levkoff SE, Seely EW. Diabetes risk perception in women with recent gestational diabetes: delivery to the postpartum visit. J Maternal-fetal Neonatal Med : J Eur Assoc Perinatal Med Fed Asia Oceania Perinatal Soc, Int Soc Perinatal Obstet. 2013;26(7):691–6.
Kim C, McEwen LN, Piette JD, Goewey J, Ferrara A, Walker EA. Risk perception for diabetes among women with histories of gestational diabetes mellitus. Diabetes Care. 2007;30(9):2281–6.
Bhugra D. Culture health and illness, 5th edition. Int Rev Psychiatry. 2009;21(5):489.
Ge L, Wikby K, Rask M. Lived experience of women with gestational diabetes mellitus living in China: a qualitative interview study. BMJ Open. 2017;7(11):e017648.
Foundation tCDR. Investigation on influencing factors of breastfeeding in China [In Chinese] 2019 [Available from: https://www.cdrf.org.cn/jjh/pdf/mu.pdf.
Morrison MK, Collins CE, Lowe JM, Giglia RC. Factors associated with early cessation of breastfeeding in women with gestational diabetes mellitus. Women Birth. 2015;28(2):143–7.
Oza-Frank R, Moreland JJ, McNamara K, Geraghty SR, Keim SA. Early lactation and infant feeding practices differ by maternal gestational diabetes history. J Hum Lact. 2016;32(4):658–65.
Doughty KN, Ronnenberg AG, Reeves KW, Qian J, Sibeko L. Barriers to exclusive breastfeeding among women with gestational diabetes mellitus in the United States. JOGNN-J Obstetr Gynecol Neonatal Nurs. 2018;47(3):301–15.
Li L, Wu Y, Wang Q, Du Y, Friesen D, Guo Y, et al. Determinants of breastfeeding self-efficacy among postpartum women in rural China: a cross-sectional study. PLoS ONE. 2022;17(4):e0266273.
Shi H, Yang Y, Yin X, Li J, Fang J, Wang X. Determinants of exclusive breastfeeding for the first six months in China: a cross-sectional study. Int Breastfeed J. 2021;16(1):40.
Nursan C, Dilek K, Sevin A. Breastfeeding self-efficacy of mothers and the affecting factors. J Aquichan. 2014;14:327–35.
Brockway M, Benzies K, Hayden KA. Interventions to improve breastfeeding self-efficacy and resultant breastfeeding rates: a systematic review and meta-analysis. J Hum Lact : J Int Lact Consult Assoc. 2017;33(3):486–99.
Raj VK, Plichta SB. The role of social support in breastfeeding promotion. Lit Rev. 1998;14(1):41–5.
Fadjriah RN, Krisnasari S, Gugu Y. Relationship between Family Social Support and Exclusive Breastfeeding Behavior at Talise Health Center, Indonesia. Open Access Maced J Med Sci. 2021;9(E):312–6. Available from: https://oamjms.eu/index.php/mjms/article/view/5987. [cited 2023 Apr. 6].
Faridvand F, Mirghafourvand M, Malakouti J, Mohammad-Alizadeh-Charandabi S. Relationship between social support and breastfeeding self-efficacy among women in Tabriz, Iran. Br J Midwifery. 2017;25(2):103–9.
Maleki-Saghooni N, AmelBarez M, Karimi FZ. Investigation of the relationship between social support and breastfeeding self-efficacy in primiparous breastfeeding mothers. J Maternal-fetal Neonatal Med : J Eur Assoc Perinatal Med, Fed Asia Oceania Perinatal Soc, Int Soc Perinatal Obstet. 2020;33(18):3097–102.
McCarter D, Gore R. Social support improves breastfeeding self-efficacy in a sample of black women. Clin Lact. 2012;3:112–5.
Stuebe AM, Bonuck K. What predicts intent to breastfeed exclusively? Breastfeeding knowledge, attitudes, and beliefs in a diverse urban population. Breast Med : J Acad Breast Med. 2011;6(6):413–20.
Scott JA, Binns CW, Oddy WH, Graham KI. Predictors of breastfeeding duration: evidence from a cohort study. Pediatrics. 2006;117(4):e646–55.
Cox K, Binns CW, Giglia R. Predictors of breastfeeding duration for rural women in a high-income country: evidence from a cohort study. Acta Paediatrica (Oslo, Norway 1992). 2015;104(8):350–9.
Stuebe AM, Bonuck K, Adatorwovor R, Schwartz TA, Berry DC. A Cluster Randomized Trial of Tailored Breastfeeding Support for Women with Gestational Diabetes. Breastfeed Med. 2016;11(10):504–13.
Acknowledgements
None.
Funding
This study was supported by the National Natural Science Foundation of China (No. 71974061). The funding bodies were not involved in the design of the study, data collection, analyses, and interpretation of data or in writing of the manuscript.
Author information
Authors and Affiliations
Contributions
L.D. performed the data collection, analysis and contributed to the writting of the manuscript. P.Q. performed the data collection. C.L. conceived and designed the study, contributed to the writting of the manuscript. T.Z. conceived and designed the study. R.L. performed the data collection. D.W. conceived and designed the study. X.D. performed the data analysis. All authors reviewed the manuscript. The author(s) read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Informed consent was obtained before the survey from each participant in the current study. We got permission for our study from the Tongji hospital ethics committee. All methods were carried out in accordance with relevant guidelines and regulations. The ethic number is NO.TJ-IRB20210755.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Additional file 1: Supplementary File 1.
Questionnaire on breastfeeding behavior and its determinants in patients with gestational diabetes mellitus. Table S1-1. Supplementary File 2. Analysis of demographic characteristics between 324 respondents and 885 pregnant women with gestational diabetes mellitus. Supplementary File 3. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) checklist. Supplementary File 4. Respondents’ determinants of breastfeeding based on HBM. Table S4-1. Perceived susceptibility. Table S4-2. Perceived severity. Table S4-3. Perceived barrier. Table S4-4. Perceived benefit. Table S4-5. Social support. Table S4-6. Self-efficacy. Supplementary File 5. Results of covariates on the breastfeeding behavior based on HBM.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visithttp://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Qian, P., Duan, L., Lin, R. et al. Decision-making process of breastfeeding behavior in mothers with gestational diabetes mellitus based on health belief model. BMC Pregnancy Childbirth 23, 242 (2023). https://doi.org/10.1186/s12884-023-05527-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12884-023-05527-3