Summary:
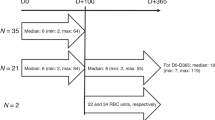
We retrospectively analyzed red blood cell (RBC) support and alloimmunization rate in 218 consecutive patients – 128 from the Pediatric Department and 90 from the adult Hematology Department – undergoing hematopoietic stem cell transplantation (HSCT) between 1994 and 2000. In the pre-HSCT period, the pediatric patients undergoing auto-HSCT required more RBC support. In the post-HSCT period, pediatric patients transplanted with an unrelated donor required more RBC support (median 13.5 U/10 kg bw) than patients receiving HSCT from a related donor (median 6 U/10 kg bw) or from an autologous source (median 4 U/10 kg bw, P=0.0004). In the pre-HSCT period, 159 out of 218 patients (73%) received a total of 1843 RBC units, with an overall median of 9 U/patient over a median of 24 months (range 4–62); 10 patients (6%) developed a total of 12 alloantibodies, with an alloimmunization rate of 5.4/1000 RBC units. In the post-HSCT period, all but three patients were given a total of 2420 RBC units, with an overall median of 6 U/patient over a median of 4 months (range 1–18); all but one of the pre-existing alloantibodies disappeared and three patients (1%) developed new alloantibodies with an alloimmunization rate of 1.2/1000 RBC units. These newly produced alloantibodies (one anti-M and two anti-E) were detected at +58, +90 and +210 days after HSCT. These findings might suggest a different approach to alloantibody screening tests in patients receiving HSCT, with a subsequent reduction of costs and laboratory workload.

Similar content being viewed by others
References
Powles R, Mehta J, Kulkarni S et al. Allogeneic blood and bone-marrow stem cell transplantation in haematological malignant diseases: a randomised trial. Lancet 2000; 335: 1231–1237.
Gratwohl A, Passweg J, Baldomero H et al. Hematopoietic stem cell transplantation activity in Europe 1999. Bone Marrow Transplant 2001; 27: 899–916.
Jantunen E, Myllykangas-Luosujarvi R . Stem cell transplantation for treatment of severe autoimmune diseases: current status and future perspectives. Bone Marrow Transplant 2000; 25: 351–356.
Krivit W, Peters C, Shapiro EG . Bone marrow transplantation as effective treatment of CNS disease in globoid cell leukodystrophy, metachromatic leukodystrophy, adrenoleukodystrophy, mannosidosis, fucosidosis, aspartylglucosaminuria, Hurler, Maroteaux-Lamy and Sly syndromes, and Gaucher disease type III. Neurology 1999; 12: 167–176.
Rubinstein P, Carrier C, Scaradavou A et al. Outcomes among 562 recipients of placental-blood transplants from unrelated donors. N Engl J Med 1998; 339: 1565–1577.
Haas R, Witt B, Mohle R et al. Sustained long-term hematopoiesis after myeloablative therapy with peripheral blood progenitor cell support. Blood 1995; 85: 3754–3761.
Mohandas K, Aledort L . Transfusion requirements, risks, and costs for patients with malignancy. Transfusion 1995; 35: 427–430.
Mehta J, Powles R, Singhal S et al. Transfusion requirements after bone marrow transplantation from HLA-identical siblings: effects of donor–recipient ABO incompatibility. Bone Marrow Transplant 1996; 18: 151–156.
Lapierre V, Kuentz M, Tiberghien P et al. Allogeneic peripheral blood hematopoietic stem cell transplantation: guidelines for red blood cell immuno-hematological assessment and transfusion practice. Bone Marrow Transplant 2000; 25: 507–512.
de la Rubia J, Arriaga F, Andreu R et al. Development of non-ABO RBC allo-antibodies in patients undergoing allogeneic HPC transplantation. Is ABO incompatibility a predisposing factor? Transfusion 2001; 41: 106–110.
Schonewille H, Haak HL, van Zijl AM . Alloimmunization after blood transfusion in patients with hematological and oncologic diseases. Transfusion 1999; 39: 763–771.
Przepiorka D, Weisdorf D, Martin P et al. 1994 Consensus conference on acute GvHD grading. Bone Marrow Transplant 1995; 15: 825–828.
Dreger P, Viehmann K, von Neuhoff N et al. Autografting of highly purified peripheral blood progenitor cells following myeloablative therapy in patients with lymphoma: a prospective study of the long-term effects on tumour eradication, reconstitution of hematopoiesis and immune recovery. Bone Marrow Transplant 1999; 24: 153–161.
Rambaldi A, Borleri G, Dotti G et al. Innovative two-step negative selection of granulocyte colony-stimulating factor mobilized circulating progenitor cells: adequacy for autologous and allogeneic transplantation. Blood 1998; 91: 2189–2196.
Balduzzi A, Gaipa G, Bonanomi S et al. Purified autologous grafting in childhood acute lymphoblastic leukemia in second remission: evidence for long-term clinical and molecular remission. Leukemia 2001; 15: 50–55.
Conover WJ . Practical Nonparametric Statistics. 2nd edn. Wiley: New York, 1980.
Ting A, Pun A, Dodds AJ et al. Red cell alloantibodies produced after bone marrow transplantation. Transfusion 1987; 27: 145–147.
Dumont-Girad F, Roux E, van Lier RA et al. Reconstitution of the T-cell compartment after bone marrow transplantation: restoration of the repertoire by thymic emigrants. Blood 1998; 92: 4464–4471.
Nordøy T, Kolstad A, Endresen P et al. Persistent changes in the immune system 4–10 years after ABMT. Bone Marrow Transplant 1999; 24: 873–878.
de Vries E, van Tol MJD, van der Bergh RL et al. Reconstitution of lymphocyte subpopulations after pediatric bone marrow transplantation. Bone Marrow Transplant 2000; 25: 267–275.
Steingrimsdottir H, Gruber A, Björkholm M et al. Immune reconstitution after autologous hematopoietic stem cell transplantation in relation to underlying disease, type of high-dose therapy and infectious complications. Haematologica 2000; 85: 832–838.
Uderzo C, Fumagalli M, De Lorenzo P et al. Impact of thrombotic thrombocytopenic purpura on leukemic children undergoing bone marrow transplantation. Bone Marrow Transplant 2000; 26: 1005–1009.
Corti P, Uderzo C, Tagliabue A et al. Defibrotide as a promising treatment for thrombotic thrombocytopenic purpura in patients undergoing bone marrow transplantation. Bone Marrow Transplant 2002; 29: 542–543.
Balduzzi A, Valsecchi MG, Silvestri D et al. Transplant-related toxicity and mortality: an AIEOP prospective study in 636 pediatric patients transplanted for acute leukemia. Bone Marrow Transplant 2002; 29: 93–100.
Gustafsson Å, Remberger M, Winiarski J, Ringdén O . Unrelated bone marrow transplantation in children: outcome and a comparison with sibling donor grafting. Bone Marrow Transplant 2000; 25: 1059–1065.
Worel N, Greinix HT, Schneider B et al. Regeneration of erythropoiesis after related- and unrelated-donor BMT or peripheral blood HPC transplantation: a major ABO mismatch means problems. Transfusion 2000; 40: 543–550.
Rowley SD, Liang PS, Ulz L . Transplantation of ABO-incompatible bone marrow and peripheral blood stem cell components. Bone Marrow Transplant 2000; 26: 749–757.
Redman M, Regan F, Contreras M . A prospective study of the incidence of red cell alloimmunisation following transfusion. Vox Sang 1996; 71: 216–220.
Garratty G . Evaluating the clinical significance of blood group alloantibodies that are causing problems in pretransfusion testing. Vox Sang 1998; 74(Suppl. 2): 285–290.
Godthelp BC, van Tol MJD, Vossen JM, van der Elser PJ . T-cell immune reconstitution in pediatric leukemic patients after allogeneic bone marrow transplantation with T-cell-depleted or unmanipulated grafts: evaluation of overall and antigen-specific T-cell repertoires. Blood 1999; 12: 4358–4369.
Abou-Elella AA, Camarillo TA, Allen MB et al. Low incidence of red cell and HLA antibody formation by bone marrow transplant patients. Transfusion 1995; 35: 931–935.
Acknowledgements
We gratefully acknowledge Mrs Joanna Upton for her linguistic assistance.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Perseghin, P., Balduzzi, A., Galimberti, S. et al. Red blood cell support and alloimmunization rate against erythrocyte antigens in patients undergoing hematopoietic stem cell transplantation. Bone Marrow Transplant 32, 231–236 (2003). https://doi.org/10.1038/sj.bmt.1704114
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1704114
- Springer Nature Limited
Keywords
We’re sorry, something doesn't seem to be working properly.
Please try refreshing the page. If that doesn't work, please contact support so we can address the problem.