Key summary points
This study aimed to detect factors that could impede the continuation of day-care services of older people cared for at home.
AbstractSection FindingsUsing clinical data of 132 older users utilizing our day-care center from April 2019 to March 2020, our study reveals statistical significance in Parkinson disease/Parkinsonism, pain complaints, day-service use, short-stay service use, day-care center use to reduce care burden, physical ability including ambulation, availability of the major caregiver, and day-care service use to reduce care burden.
AbstractSection MessageSince the use of short-stay and day-care services and low independent ambulation were the likely factors for suspended use, an effective program for day-service and short-stay services to improve the activities of daily living of older users and reduce care burden is required in day-care centers.
Abstract
Purpose
Day-care services contribute to maintaining the daily living ability of older people cared for at home. This study aimed to detect factors that could impede the continuation of day-care services.
Methods
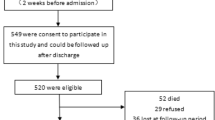
We collected clinical data of 132 older users (age = 82.8 ± 7.5 years; male:female = 49:83) utilizing our day-care center from April 2019 to March 2020. We evaluated age, sex, underlying disease, medication, family background, care level, food texture, physical ability, reasons for frequenting day-care centers, and combined medical/nursing care plans. Participants were divided into two groups: continuation (n = 51) and suspension (n = 81). The collected items were evaluated statistically using the chi-square test, Mann–Whitney test, and unpaired t test. Multivariate logistic analysis (forward–backward stepwise selection method) was added to the statistically significant items. Statistical significance was defined as p < 0.05.
Results
The comparison test detected statistical significance in Parkinson disease/Parkinsonism, pain complaints, day-service use, short-stay service use, day-care center use to reduce care burden, physical ability including ambulation, and availability of the major caregiver (p < 0.05). Day-care service use to reduce care burden (odds ratio 5.646, p < 0.05), use of short-stay and day-care services (odds ratio 4.798, p < 0.05), and low independent ambulation (odds ratio 0.585, p < 0.05) were the likely factors for suspended use (percentage of correct classification = 68.5%).
Conclusion
An unreplaceable and effective program for day-service and short-stay services to improve the activities of daily living of older users and reduce care burden is required in day-care centers.
Similar content being viewed by others
References
Kurasawa S, Yoshimasu K, Washio M, Fukumoto J, Takemura S, Yokoi K et al (2012) Factors influencing caregivers’ burden among family caregivers and institutionalization of in-home elderly people cared for by family caregivers. Environ Health Prev Med 17:474–483. https://doi.org/10.1007/s12199-012-0276-8
Logsdon RG, Pike KC, Korte L, Goehring C (2016) Memory care and wellness services: efficacy of specialized dementia care in adult day services. Gerontologist 56:318–325. https://doi.org/10.1093/geront/gnu012
Kasai M, Meguro K, Akanuma K, Yamaguchi S (2015) Alzheimer’s disease patients institutionalized in group homes run by long-term care insurance exhibit fewer symptoms of behavioural problems as evaluated by the Behavioural Pathology in Alzheimer’s disease Rating Scale. Psychogeriatrics 15:102–108. https://doi.org/10.1111/psyg.12079
Femia EE, Zarit SH, Stephens MA, Greene R (2007) Impact of adult day services on behavioral and psychological symptoms of dementia. Gerontologist 47:775–788. https://doi.org/10.1093/geront/47.6.775
Zank S, Schacke C (2002) Evaluation of geriatric day care units: effects on patients and caregivers. J Gerontol B Psychol Sci Soc Sci 57:348–357. https://doi.org/10.1093/geronb/57.4.p348’
Maruta M, Tabira T, Makizako H, Sagari A, Miyata H, Yoshimitsu K et al (2019) Impact of outpatient Rehabilitation Service in preventing the deterioration of the care-needs level among Japanese older adults availing long-term care insurance: a propensity score matched retrospective study. Int J Environ Res Public Health. https://doi.org/10.3390/ijerph16071292
Sakamoto R, Miura Y (2016) The effect of exercise intervention on frail elderly in need of care: half-day program in a senior day-care service facility specializing in functional training. J Phys Ther Sci 28:1957–1963. https://doi.org/10.1589/jpts.28.1957
Lee TW, Yim ES, Choi HS, Chung J (2019) Day care vs home care: effects on functional health outcomes among long-term care beneficiaries with dementia in Korea. Int J Geriatr Psychiatry 34:97–105. https://doi.org/10.1002/gps.4992
Gaugler JE, Jarrott SE, Zarit SH, Stephens MA, Townsend A, Greene R (2003) Adult day service use and reductions in caregiving hours: effects on stress and psychological well-being for dementia caregivers. Int J Geriatr Psychiatry 18:55–62. https://doi.org/10.1002/gps.772
Tretteteig S, Vatne S, Rokstad AM (2017) The influence of day care centres designed for people with dementia on family caregivers—a qualitative study. BMC Geriatr 17:5. https://doi.org/10.1186/s12877-016-0403-2
Mossello E, Caleri V, Razzi E, Di Bari M, Cantini C, Tonon E et al (2008) Day care for older dementia patients: favorable effects on behavioral and psychological symptoms and caregiver stress. Int J Geriatr Psychiatry 23:1066–1072. https://doi.org/10.1002/gps.2034
Zarit SH, Kim K, Femia EE, Almeida DM, Savla J, Molenaar PC (2011) Effects of adult day care on daily stress of caregivers: a within-person approach. J Gerontol B Psychol Sci Soc Sci 66:538–546. https://doi.org/10.1093/geronb/gbr030
Ministry of Health, Labour and Welfare. https://www.kaigokensaku.mhlw.go.jp/publish/. Accessed 20 Jan 2022
Nakagoshi R, Takemasa S, Nakayama K, Morioka H, Oyama M (2014) Factors affecting longitudinal changes in activities of daily living of home-bound elderly disabled, and quality of life and burden of their family caregivers. Rigakuryoho Kagaku 29:87–95. https://doi.org/10.1589/rika.29.87
Mazurek J, Szczésniak D, Trypka E, Lion KM, Wallner R, Rymaszewska J (2020) Needs of older people attending day care centres in Poland. Healthcare (Basel) 8:310. https://doi.org/10.3390/healthcare8030310
Hori Y, Hoshino J, Suzuki K (2011) Physical and psychological health problems among Japanese family caregivers. Nagoya J Med Sci 73:107–115
Oliveira A, Nossa P, Mota-Pinto A (2019) Assessing functional capacity and factors determining functional decline in the elderly: a cross-sectional study. Acta Med Port 32:654–660. https://doi.org/10.20344/amp.11974
Ellen ME, Demaio P, Lange A, Wilson MG (2017) Adult day center programs and their associated outcomes on clients, caregivers, and the health system: a sco** review. Gerontologist 57:e85-94. https://doi.org/10.1093/geront/gnw165
Lin CF, Wu JJ, Huang YH, Ju LY, Lin SY, Chou YC et al (2021) Impact of day care services on physical and cognitive functions in old people with dementia in a medical center in central Taiwan. Health Qual Life Outcomes 19:170. https://doi.org/10.1186/s12955-021-01806-9
Orellana K, Manthorpe J, Tinker A (2020) Day centres for older people—attender characteristics, access routes and outcomes of regular attendance: findings of exploratory mixed methods case study research. BMC Geriatr 20:158. https://doi.org/10.1186/s12877-020-01529-4
Temlett JA, Thompson PD (2006) Reasons for admission to hospital for Parkinson’s disease. Intern Med J 36:524–526. https://doi.org/10.1111/j.1445-5994.2006.01123.x
Ferrell BA (1991) Pain management in elderly people. J Am Geriatr Soc 39:64–73. https://doi.org/10.1111/j.1532-5415.1991.tb05908.x
Roy R (1986) A psychosocial perspective on chronic pain and depression in the elderly. Soc Work Health Care 12:27–36. https://doi.org/10.1300/j010v12n02_03
Werner P, Cohen-Mansfield J, Watson V, Pasis S (1998) Pain in participants of adult day care centers: assessment by different raters. J Pain Symptom Manag 15:8–17. https://doi.org/10.1016/S0885-3924(97)00274-1
Makizako H, Abe T, Abe K, Kobayashi S, Koguchi R, Onuma T et al (2008) Factors burdening the caregiving relatives of community-dwelling disable Japanese people. Nihon Ronen Igakkai Zasshi 45:59–67. https://doi.org/10.3143/geriatrics.45.59
Ministry of Health, Labour and Welfare. https://www.kaigokensaku.mhlw.go.jp/publish/. Accessed 9 Nov 2021
Acknowledgements
We would like to thank Editage (www.editage.com) for English language editing.
Funding
No funding was received to assist with the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
Conceptualization and investigation: TY; Formal analysis: AG; Writing—original draft preparation: YM; Writing—review and editing: AG; Investigation: AT, TK, KA, YO; Project administration: JK; Project administration and final approval of the draft: KY.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no competing interests to declare that are relevant to the content of this article.
Ethics approval
Approval was obtained from the ethical committee of Hikari hospital. The procedures used in this study adhere to the tenets of the Declaration of Helsinki.
Consent to participate
Verbal informed consent was obtained prior to the interview. The participants were guaranteed that their clinical data would be anonymized.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yamamoto, T., Goda, A., Maki, Y. et al. Factors related to suspension of day-care services: an effective program for older users with declined ambulation to reduce care burden. Eur Geriatr Med 13, 951–957 (2022). https://doi.org/10.1007/s41999-022-00621-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s41999-022-00621-9