Abstract
Background
The outcome of renal vein thrombosis, in particular as for the long-term impact on kidney function, is not fully known. We aimed to study the natural course and outcomes of patients with renal vein thrombosis, in a large, single-center cohort.
Methods
A single-center retrospective cohort study including patients who were diagnosed with renal vein thrombosis between January 2006 and September 2021 was analyzed. The main outcomes analyzed were worsening kidney function, defined as a decrease in eGFR of at least 40% from baseline, and all-cause mortality.
Results
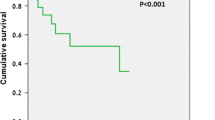
Eighty-seven patients were included, 56.3% were female, median age was 57 years. Malignancy was the most common cause of renal vein thrombosis (60.9%), followed by post-surgery and trauma (16.1%) and nephrotic syndrome (12.6%). At initial presentation, 65.5% of the patients were asymptomatic; the main signs and symptoms were gross hematuria (20.7%), flank pain (18.4%), and flank tenderness (9.2%). During follow-up, 18 (21.4%) patients experienced worsening kidney function and 57 (65.5%) died. Multivariable analyses showed that the risk of worsening kidney function was higher in patients with nephrotic syndrome (hazard ratio [HR] 18.41; 95% confidence interval [CI], 1.57–216.04), body weight ≥ 60 kg (HR 4.82; 95% CI 1.43–16.32), and malignancy (HR 9.10; 95% CI 1.05–78.63). Symptomatic acute renal vein thrombosis was associated with a lower risk of worsening kidney function compared to asymptomatic or symptomatic chronic renal vein thrombosis (HR 0.12; 95% CI 0.01–0.96). Malignancy (HR 5.45; 95% CI 2.58–11.54), age ≥ 75 years (HR 3.44; 95% CI 1.49–7.93), and serum albumin < 3.0 g/dL (HR 2.88; 95% CI 1.65–5.05) were associated with an increased mortality risk.
Conclusion
Renal vein thrombosis is associated with a high rate of worsening kidney function and mortality. It is crucial to promptly identify patients at high risk and initiate early treatment to prevent negative outcomes.
Graphical abstract



Similar content being viewed by others
Data availability
This study does not cover data posting in public databases. However, data are available upon reasonable request to the corresponding author and are subject to approval by Faculty of Medicine, Chiang Mai University Ethics Committee.
References
Asghar M, Ahmed K, Shah SS, Siddique MK, Dasgupta P, Khan MS (2007) Renal vein thrombosis. Eur J Vasc Endovasc Surg 34(2):217–223. https://doi.org/10.1016/j.ejvs.2007.02.017
Bagot CN, Arya R (2008) Virchow and his triad: a question of attribution. Br J Haematol 143(2):180–190. https://doi.org/10.1111/j.1365-2141.2008.07323.x
Tavakkoli M, Zafarghandi RM, Taghavi R, Ghoreifi A, Zafarghandi MM (2017) Immediate vascular complications after kidney transplant: experience from 2100 recipients. Exp Clin Transplant 15(5):504–508. https://doi.org/10.6002/ect.2016.0057
Date Y, Nagamine H, Hara H, Kawase Y (2019) Renal vein thrombosis after open repair of abdominal aortic aneurysm successfully treated by direct oral anticoagulants. Vasc Endovasc Surg 53(5):408–410. https://doi.org/10.1177/1538574419839251
Ouellette AC, Darling EK, Sivapathasundaram B, Babe G, Perez R, Chan AKC, Chanchlani R (2020) Incidence, risk factors, and outcomes of neonatal renal vein thrombosis in Ontario: population-based cohort study. Kidney360 1(7):640–647. https://doi.org/10.34067/kid.0000912019
Gozzo C, Farina R, Foti PV, Iannace FA, Conti A, Pennisi I, Santonocito S, Palmucci S, Basile A (2021) Posterior nutcracker syndrome: a case report. J Med Case Rep 15(1):42. https://doi.org/10.1186/s13256-020-02617-0
Lizama L, Bran S, Kuestermann S, García-Gallont R (2020) Renal vein thrombosis due to posterior nutcracker syndrome. Methodist Debakey Cardiovasc J 16(4):e5–e7. https://doi.org/10.14797/mdcj-16-4-e5
Ross O, Pourmoussa A, Batech M, Sim JJ (2017) Characteristics of patients diagnosed with renal vein thrombosis and glomerulopathy: a case series. Int Urol Nephrol 49(2):285–293. https://doi.org/10.1007/s11255-016-1442-5
Wysokinski WE, Gosk-Bierska I, Greene EL, Grill D, Wiste H, McBane RD 2nd (2008) Clinical characteristics and long-term follow-up of patients with renal vein thrombosis. Am J Kidney Dis 51(2):224–232. https://doi.org/10.1053/j.ajkd.2007.10.030
Rottenstreich A, Barzilai M, Da’as N, Kleinstern G, Varon D, Kalish Y (2017) Active malignancy in patients with renal vein thrombosis: influence upon clinical course and survival. Clin Exp Nephrol 21(1):49–54. https://doi.org/10.1007/s10157-016-1245-0
Tektonidou MG (2018) Antiphospholipid syndrome nephropathy: from pathogenesis to treatment. Front Immunol 9:1181. https://doi.org/10.3389/fimmu.2018.01181
El-Reshaid K, Al-Bader S, Sallam H (2016) Multiple visceral venous thromboses associated with oral contraceptive use. Saudi J Kidney Dis Transpl 27(6):1256–1259. https://doi.org/10.4103/1319-2442.194683
McCarthy LJ, Titus JL, Daugherty GW (1963) Bilateral renal-vein thrombosis and the nephrotic syndrome in adults. Ann Intern Med 58:837–857. https://doi.org/10.7326/0003-4819-58-5-837
Zubarev AV (2001) Ultrasound of renal vessels. Eur Radiol 11(10):1902–1915. https://doi.org/10.1007/s003300101012
Urban BA, Ratner LE, Fishman EK (2001) Three-dimensional volume-rendered CT angiography of the renal arteries and veins: normal anatomy, variants, and clinical applications. Radiographics 21(2):373–386. https://doi.org/10.1148/radiographics.21.2.g01mr19373
Kidney Disease: Improving Global Outcomes Glomerular Diseases Work G (2021) KDIGO 2021 clinical practice guideline for the management of glomerular diseases. Kidney Int 100(4S):S1–S276. https://doi.org/10.1016/j.kint.2021.05.021
Inker LA, Eneanya ND, Coresh J, Tighiouart H, Wang D, Sang Y, Crews DC, Doria A, Estrella MM, Froissart M, Grams ME, Greene T, Grubb A, Gudnason V, Gutierrez OM, Kalil R, Karger AB, Mauer M, Navis G, Nelson RG, Poggio ED, Rodby R, Rossing P, Rule AD, Selvin E, Seegmiller JC, Shlipak MG, Torres VE, Yang W, Ballew SH, Couture SJ, Powe NR, Levey AS, Chronic Kidney Disease Epidemiology C (2021) New creatinine- and cystatin C-based equations to estimate GFR without race. N Engl J Med 385(19):1737–1749. https://doi.org/10.1056/NEJMoa2102953
Kaatz S, Ahmad D, Spyropoulos AC, Schulman S, Subcommittee on Control of A (2015) Definition of clinically relevant non-major bleeding in studies of anticoagulants in atrial fibrillation and venous thromboembolic disease in non-surgical patients: communication from the SSC of the ISTH. J Thromb Haemost 13(11):2119–2126. https://doi.org/10.1111/jth.13140
Ruf W, Edgington TS (1994) Structural biology of tissue factor, the initiator of thrombogenesis in vivo. Faseb j 8(6):385–390
Falanga A, Panova-Noeva M, Russo L (2009) Procoagulant mechanisms in tumour cells. Best Pract Res Clin Haematol 22(1):49–60. https://doi.org/10.1016/j.beha.2008.12.009
Abdol Razak NB, Jones G, Bhandari M, Berndt MC, Metharom P (2018) Cancer-associated thrombosis: an overview of mechanisms, risk factors, and treatment. Cancers (Basel) 10(10):380. https://doi.org/10.3390/cancers10100380
Lechner D, Kollars M, Gleiss A, Kyrle PA, Weltermann A (2007) Chemotherapy-induced thrombin generation via procoagulant endothelial microparticles is independent of tissue factor activity. J Thromb Haemost 5(12):2445–2452. https://doi.org/10.1111/j.1538-7836.2007.02788.x
Zou PM, Li H, Cai JF, Chen ZJ, Li C, Xu P, Li MX, Chen LM, Li XM, Li XW (2018) A cohort study of incidences and risk factors for thromboembolic events in patients with idiopathic membranous nephropathy. Chin Med Sci J 33(2):91–99. https://doi.org/10.24920/11809
Singhal R, Brimble KS (2006) Thromboembolic complications in the nephrotic syndrome: pathophysiology and clinical management. Thromb Res 118(3):397–407. https://doi.org/10.1016/j.thromres.2005.03.030
van den Brand JA, van Dijk PR, Hofstra JM, Wetzels JF (2014) Long-term outcomes in idiopathic membranous nephropathy using a restrictive treatment strategy. J Am Soc Nephrol 25(1):150–158. https://doi.org/10.1681/ASN.2013020185
Laluck BJ Jr, Cattran DC (1999) Prognosis after a complete remission in adult patients with idiopathic membranous nephropathy. Am J Kidney Dis 33(6):1026–1032. https://doi.org/10.1016/s0272-6386(99)70138-1
Ryu S, Chang Y, Woo HY, Kim SG, Kim DI, Kim WS, Suh BS, Choi NK, Lee JT (2008) Changes in body weight predict CKD in healthy men. J Am Soc Nephrol 19(9):1798–1805. https://doi.org/10.1681/ASN.2007121286
Olivo RE, Davenport CA, Diamantidis CJ, Bhavsar NA, Tyson CC, Hall R, Bidulescu A, Young B, Mwasongwe SE, Pendergast J, Boulware LE, Scialla JJ (2018) Obesity and synergistic risk factors for chronic kidney disease in African American adults: the Jackson Heart Study. Nephrol Dial Transplant 33(6):992–1001. https://doi.org/10.1093/ndt/gfx230
Zigman A, Yazbeck S, Emil S, Nguyen L (2000) Renal vein thrombosis: a 10-year review. J Pediatr Surg 35(11):1540–1542. https://doi.org/10.1053/jpsu.2000.18302
Soeters PB, Wolfe RR, Shenkin A (2019) Hypoalbuminemia: pathogenesis and clinical significance. JPEN J Parenter Enteral Nutr 43(2):181–193. https://doi.org/10.1002/jpen.1451
Funding
No funding was received for conducting this study.
Author information
Authors and Affiliations
Contributions
Conceptualization: PW, CC-A, KN; Methodology: PW, CC-A, NI; Formal analysis and investigation PW, CC-A, KN; Writing—original draft preparation: PW, CC-A; Writing—review and editing: CC-A, KN; Supervision: CC-A, KN. Each author contributed important intellectual content during manuscript drafting or revision and agrees to be personally accountable for the individual’s own contributions and to ensure that questions pertaining to the accuracy or integrity of any portion of the work, even one in which the author was not directly involved, are appropriately investigated and resolved, including with documentation in the literature if appropriate.
Corresponding authors
Ethics declarations
Conflict of interest
The authors did not receive support from any organization for the submitted work. All authors certify that they have no affiliations with, or involvement in, any organization or entity with any financial interest or non-financial interest in the subject matter or materials discussed in this manuscript.
Ethical approval
The study was performed in accordance with the Declaration of Helsinki and the Declaration of Istanbul. It was approved by the Institutional Review Boards of Chiang Mai University (approval number: MED-2564-08529).
Informed consent
Informed consent was waived because of the retrospective nature of the study, and the analysis used anonymous clinical data.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wanaratwichit, P., Chai-Adisaksopha, C., Inmutto, N. et al. Risk factors of worsening kidney function and mortality in patients with renal vein thrombosis: a retrospective study. J Nephrol 37, 131–140 (2024). https://doi.org/10.1007/s40620-023-01761-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40620-023-01761-2