Abstract
Background
Numerous studies have shown a significant association between blood pressure (BP) and cognition, but little is known about the effect of BP on the rate of cognitive decline.
Aims
To investigate the relationship between blood pressure and the subsequent rate of cognitive decline in elderly people.
Methods
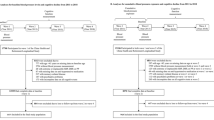
Based on a prospective cohort that has been followed since 2014, we collected baseline blood pressures and other covariates in 7874 Chinese individuals aged 60 years or older, and followed their cognitive change using the Mini-Mental State Examination (MMSE) until Dec 31, 2016. Linear mixed-effects models were used to measure changes in MMSE scores over time in relation to blood pressure values, and in addition to the covariates, we included random effects for intercepts and slopes.
Results
In the non-hypertension group, we observed that faster cognitive decline was associated with higher systolic blood pressure, lower diastolic blood pressure, lower mean arterial pressure, and higher pulse pressure. In the hypertension group, lower diastolic blood pressure, lower mean arterial pressure, and higher pulse pressure were associated with faster cognitive decline, but not systolic blood pressure.
Conclusion
Higher systolic blood pressure, lower diastolic blood pressure, lower mean arterial pressure, and higher pulse pressure accelerate the subsequent rate of cognitive decline in elderly people. The results of this study may help improve blood-pressure control strategies to prevent cognitive decline.

Similar content being viewed by others
Availability of data and materials
The data that support the findings of this study are available from the ethics committee of Zhejiang Provincial Center for Disease Control and Prevention but restrictions apply to the availability of these data, which were used under license for the current study, and so are not publicly available. Data are, however, available from the authors upon reasonable request and with permission of the ethics committee of Zhejiang Provincial Center for Disease Control and Prevention.
References
Alzheimer’s Disease International (2019) World Alzheimer Report 2019: attitudes to dementia. Alzheimer’s Disease International, London
The Lancet (2017) Dementia burden coming into focus. Lancet 390:2606
Alzheimer’s Disease International (2016) World Alzheimer Report 2016: improving healthcare for people with dementia coverage, quality and costs now and in the future. Alzheimer’s Disease International, London
Zhang T, Yan R, Chen Q et al (2018) Body mass index, waist-to-hip ratio and cognitive function among Chinese elderly: a cross-sectional study. BMJ Open 8:e022055
Lv X, Li W, Ma Y et al (2019) Cognitive decline and mortality among community-dwelling Chinese older people. BMC Med 17:63
Peters R, Beckett N, Forette F et al (2008) Incident dementia and blood pressure lowering in the Hypertension in the Very Elderly Trial cognitive function assessment (HYVET-COG): a double-blind, placebo controlled trial. Lancet Neurol 7:683–689
Walker KA, Sharrett AR, Wu A et al (2019) Association of midlife to late-life blood pressure patterns with incident dementia. JAMA 322:535–545
Faraco G, Park L, Zhou P et al (2016) Hypertension enhances Abeta-induced neurovascular dysfunction, promotes beta-secretase activity, and leads to amyloidogenic processing of APP. J Cereb Blood Flow Metab 36:241–252
Stewart R, Xue QL, Masaki K et al (2009) Change in blood pressure and incident dementia: a 32-year prospective study. Hypertension 54:233–240
van Dijk EJ, Breteler MM, Schmidt R et al (2004) The association between blood pressure, hypertension, and cerebral white matter lesions: cardiovascular determinants of dementia study. Hypertension 44:625–630
Levine DA, Galecki AT, Langa KM et al (2019) Blood pressure and cognitive decline over 8 years in middle-aged and older black and white americans. Hypertension 73:310–318
Li F, He F, Chen T et al (2016) Reproductive history and risk of cognitive impairment in elderly women: a cross-sectional study in Eastern China. J Alzheimers Dis 49:139–147
Zheng F, Yan L, Zhong B et al (2019) Progression of cognitive decline before and after incident stroke. Neurology 93:e20–e28
Raymont V, Greathouse A, Reding K et al (2008) Demographic, structural and genetic predictors of late cognitive decline after penetrating head injury. Brain 131:543–558
Kisser JE, Allen AJ, Katzel LI et al (2016) Relations of blood pressure and head injury to regional cerebral blood flow. J Neurol Sci 365:9–14
Wang Z, Zhang M (1989) Application of Chinese version of Mini-Mental State examination (MMSE). Shanghai Arch Psychiatry 7:108–111
Yuan J, Lv Y, Chen H et al (2019) Association between late-life blood pressure and the incidence of cognitive impairment: a community-based prospective cohort study. J Am Med Dir Assoc 20:177–182 (e172)
Nagai M, Hoshide S, Ishikawa J et al (2008) Ambulatory blood pressure as an independent determinant of brain atrophy and cognitive function in elderly hypertension. J Hypertens 26:1636–1641
Glodzik L, Mosconi L, Tsui W et al (2012) Alzheimer’s disease markers, hypertension, and gray matter damage in normal elderly. Neurobiol Aging 33:1215–1227
Don-Doncow N, Vanherle L, Zhang Y et al (2019) T-cell accumulation in the hypertensive brain: a role for sphingosine-1-phosphate-mediated chemotaxis. Int J Mol Sci 20:537
Holscher C (2019) Insulin signaling impairment in the brain as a risk factor in Alzheimer’s disease. Front Aging Neurosci 11:88
Pan H, Huang X, Li F et al (2019) Association among plasma lactate, systemic inflammation, and mild cognitive impairment: a community-based study. Neurol Sci 40:1667–1673
Nation DA, Edmonds EC, Bangen KJ, Alzheimer’s Disease Neuroimaging Initiative I et al (2015) Pulse pressure in relation to tau-mediated neurodegeneration, cerebral amyloidosis, and progression to dementia in very old adults. JAMA Neurol 72:546–553
Nation DA, Edland SD, Bondi MW et al (2013) Pulse pressure is associated with Alzheimer biomarkers in cognitively normal older adults. Neurology 81:2024–2027
Scuteri A, Mandas A (2019) The hidden treasure of 24-hours ambulatory blood pressure monitoring-Assessing BP variability. J Clin Hypertens (Greenwich) 21:1795–1796
Scuteri A, Chen C, Yin F et al (2001) Functional correlates of central arterial geometric phenotypes. Hypertension 38:1471–1475
Farasat SM, Morrell CH, Scuteri A et al (2008) Pulse pressure is inversely related to aortic root diameter implications for the pathogenesis of systolic hypertension. Hypertension 51:196–202
Scuteri A, Rovella V, Alunni Fegatelli D et al (2018) An operational definition of SHATS (Systemic Hemodynamic Atherosclerotic Syndrome): role of arterial stiffness and blood pressure variability in elderly hypertensive subjects. Int J Cardiol 263:132–137
Bracko O, Njiru BN, Swallow M et al (2020) Increasing cerebral blood flow improves cognition into late stages in Alzheimer’s disease mice. J Cereb Blood Flow Metab 40:1441–1452
Zhao Y, Gong CX (2015) From chronic cerebral hypoperfusion to Alzheimer-like brain pathology and neurodegeneration. Cell Mol Neurobiol 35:101–110
Haberman RP, Branch A, Gallagher M (2017) Targeting neural hyperactivity as a treatment to stem progression of late-onset Alzheimer’s disease. Neurotherapeutics 14:662–676
Staffaroni AM, Cobigo Y, Elahi FM et al (2019) A longitudinal characterization of perfusion in the aging brain and associations with cognition and neural structure. Hum Brain Mapp 40:3522–3533
Scuteri A, Tesauro M, Guglini L et al (2013) Aortic stiffness and hypotension episodes are associated with impaired cognitive function in older subjects with subjective complaints of memory loss. Int J Cardiol 169:371–377
Scuteri A, Wang H (2014) Pulse wave velocity as a marker of cognitive impairment in the elderly. J Alzheimers Dis 42:S401–410
Walker KA, Power MC, Gottesman RF (2017) Defining the relationship between hypertension, cognitive decline, and dementia: a review. Curr Hypertens Rep 19:24
Streit S, Poortvliet RKE, Elzen W et al (2019) Systolic blood pressure and cognitive decline in older adults with hypertension. Ann Fam Med 17:100–107
Lakatta EG, AlunniFegatelli D, Morrell CH et al (2020) Impact of stiffer arteries on the response to antihypertensive treatment: a longitudinal study of the SardiNIA cohort. J Am Med Dir Assoc 21:720–725
Acknowledgements
We acknowledge the invaluable contributions made by all the interviewers in this study. We would also like to express our gratitude to all the participants.
Funding
Fudong Li was supported by Natural Science Foundation of Zhejiang Province (Q19H260001), and Fan He was supported by Zhejiang Provincial Public Welfare Technology Application Research Foundation (LGF19H260003).
Author information
Authors and Affiliations
Contributions
TZ, FH, JH, JL, XW, FL, YZ, XG, and MW participated in the design of the study, collection of data, data cleaning. TZ and FH conducted the statistical analyses. TZ wrote the manuscript. JH, FH, and JL contributed to the interpretation of the results and revised the manuscript critically. All authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Statement of human and animal rights
The study was approved by the ethics committee of Zhejiang Provincial Center for Disease Control and Prevention.
Informed consent
Informed consent was obtained from each participant or their legally authorized representative (low literacy and/or physically disabled participants).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhang, T., He, F., Hu, J. et al. Blood pressure and cognitive decline over the course of 2 years in elderly people: a community-based prospective cohort study. Aging Clin Exp Res 33, 1903–1908 (2021). https://doi.org/10.1007/s40520-020-01717-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-020-01717-7