Abstract
Purpose
To evaluate and compare the efficacy of the hands–eyes–mouth distraction technique (HEM-DT) in reducing anxiety and pain levels and improving the behaviour of pre-school children during inferior alveolar nerve block (IANB) administration to that of the covering patient’s vision technique (CPV-T).
Methods
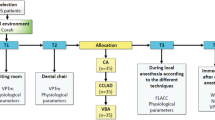
This study included 52 children aged 3–5 years old with primary dentition, no history of receiving local anaesthesia, and whose treatments required an IANB. These children were randomly assigned into two groups: HEM-DT (G1; n = 26) and CPV-T (G2; n = 26). Anxiety and pain levels were assessed using the Facial Image Scale and the Wong–Baker Scale, respectively, while the patient’s behaviour was evaluated using the Frankl Behaviour Scale. This study was divided into two sessions including the treatment session (administration of IANB) and the control session (7 days after anaesthesia). Chi-square test, the Mann–Whitney U test and Wilcoxon test were used for statistical analyses.
Results
The patients’ anxiety levels did not increase 7 days after IANB in G1 (p value = 0.798); however, higher anxiety levels were observed in the G2 group (p value = 0.039). No significant differences in pain levels and behaviour were observed between the groups during administration of anaesthesia (p value > 0.005).
Conclusion
HEM-DT and CPV-T showed efficacy in terms of pain and behaviour during IANB administration. Pre-school children in the HEM-DT group exhibited lower anxiety levels in the control session.
Trial registration number and date of registration
ClinicalTrials.gov (NCT02591797). October 28, 2015.

Similar content being viewed by others
References
Abdelmoniem SA, Mahmoud SA. Comparative evaluation of passive, active, and passive-active distraction techniques on pain perception during local anesthesia administration in children. J Adv Res. 2016;7:551–6. https://doi.org/10.1016/j.jare.2015.10.001.
Aditya PVA, Prasad MG, Nagaradhakrishna A, Raju NS, Babu DN. Comparison of effectiveness of three distraction techniques to allay dental anxiety during inferior alveolar nerve block in children: a randomized controlled clinical trial. Heliyon. 2021;7: e08092. https://doi.org/10.1016/j.heliyon.2021.e08092.
American Academy of Pediatric Dentistry. Behavior guidance for the pediatric dental patient. The reference manual of pediatric dentistry. Chicago: American Academy of Pediatric Dentistry; 2021. p. 306–24.
Bartlett G, Mansoor J. Articaine buccal infiltration vs lidocaine inferior dental block—a review of the literature. Br Dent J. 2016;220:117–20. https://doi.org/10.1038/sj.bdj.2016.93.
Birnie KA, Noel M, Chambers CT, Uman LS, Parker JA. Psychological interventions for needle-related procedural pain and distress in children and adolescents. Cochrane Database Syst Rev. 2018;10:005179. https://doi.org/10.1002/14651858.CD005179.pub4.
Buchanan H, Niven N. Validation of a Facial Image Scale to assess child dental anxiety. Int J Paediatr Dent. 2002;12:47–52. https://doi.org/10.1046/j.0960-7439.2001.00322.x.
Davoudi A, Rismanchian M, Akhavan A, Nosouhian S, Bajoghli F, Haghighat A, Arbabzadeh F, Samimi P, Fiez A, Shadmehr E, Tabari K, Jahadi S. A brief review on the efficacy of different possible and nonpharmacological techniques in eliminating discomfort of local anesthesia injection during dental procedures. Anesth Essays Res. 2016;10:13–6. https://doi.org/10.4103/0259-1162.167846.
De Menezes Abreu DM, Leal SC, Mulder J, Frencken JE. Dental anxiety in 6–7-year-old children treated in accordance with conventional restorative treatment, ART and ultra-conservative treatment protocols. Acta Odontol Scand. 2011;69:410–6. https://doi.org/10.3109/00016357.2011.572561.
Elheeny AAH. Articaine efficacy and safety in young children below the age of four years: an equivalent parallel randomized control trial. Int J Paediatr Dent. 2020;30:547–55. https://doi.org/10.1111/ipd.12640.
Erfanparast L, Rahbar M, Pourkazemi M, Vatandoust M, Balar S, Vafaei A. Comparison of effects exerted by 4% articaine buccal infiltration and 2% lidocaine inferior alveolar nerve block on pain perception and behavioral feedback of children during pulp treatment of mandibular second primary molars. Maedica (bucur). 2020;15:477–83. https://doi.org/10.26574/maedica.2020.15.4.477.
Farhat-McHayleh N, Harfouche A, Souaid P. Techniques for managing behaviour in pediatric dentistry: comparative study of live modelling and tell-show-do based on children’s heart rates during treatment. J Can Dent Assoc. 2009;75:283. https://doi.org/10.1186/s12903-021-01678-x.
Frankl S, Shire R, Fogels H. Should the parent remain with the child in the dental operatory? J Dent Child. 1962;29:150–63.
Ghadimi S, Shahrabi M, Khosravi Z, Behroozi R. Efficacy of articaine infiltration versus lidocaine inferior alveolar nerve block for pulpotomy in mandibular primary second molars: a randomized clinical trial. J Dent Res Dent Clin Dent Prospects. 2018;12:97–101. https://doi.org/10.15171/joddd.2018.015.
Goettems ML, Zborowski EJ, Costa FD, Costa VP, Torriani DD. Nonpharmacologic intervention on the prevention of pain and anxiety during pediatric dental care: a systematic review. Acad Pediatr. 2017;17:110–9. https://doi.org/10.1016/j.acap.2016.08.012.
Hassanein PH, Khalil A, Talaat DM. Pain assessment during mandibular nerve block injection with the aid of dental vibe tool in pediatric dental patients: a randomized clinical trial. Quintessence Int. 2020;51:310–7. https://doi.org/10.3290/j.qi.a44145.
Haytham FA, El Sharkawi BDS, et al. Effectiveness of new distraction technique on pain associated with injection of local anesthesia of children. Pediatr Dent. 2012;34:35–8.
Hegde KM, Neeraja R, Srinivasan I, Murali Krishna DR, Melwani A, Radhakrishna S. Effect of vibration during local anesthesia administration on pain, anxiety, and behavior of pediatric patients aged 6–11 years: a crossover split-mouth study. J Dent Anesth Pain Med. 2019;19:143–9. https://doi.org/10.17245/jdapm.2019.19.3.143.
Hoge MA, Howard MR, Wallace DP, Allen KD. Use of video eyewear to manage distress in children during restorative dental treatment. Pediatr Dent. 2012;34:378–82. https://doi.org/10.17796/jcpd.38.1.265807t236570hx7.
Kamath PS. A novel distraction technique for pain management during local anesthesia administration in pediatric patients. J Clin Pediatr Dent. 2013;38:45–7. https://doi.org/10.17796/jcpd.38.1.265807t236570hx7.
Klingberg G, Broberg AG. Dental fear/anxiety and dental behaviour management problems in children and adolescents: a review of prevalence and concomitant psychological factors. Int J Paediatr Dent. 2007;17:391–406. https://doi.org/10.1111/j.1365-263X.2007.00872.x.
Kuscu O, Akyuz S. Children preferences concerning the physical appearance of dental injectors. ASDC J Dent Child. 2006;73:116–21.
Kuscu OO, Akyuz S. Is it the injection device or the anxiety experienced that causes pain during dental local anaesthesia? Int J Paediatr Dent. 2008;18:139–45. https://doi.org/10.1111/j.1365-263X.2007.00875.x.
Lin CS, Wu SY, Yi CA. Association between anxiety and pain in dental treatment: a systematic review and meta-analysis. J Dent Res. 2017;96:153–62. https://doi.org/10.1177/0022034516678168.
Majstorovic M, Veerkamp JSS. Relationship between needle phobia and dental anxiety. J Dent Child (chic). 2004;71:201–5.
Meechan JG, Cole B, Welbury RR. The influence of two different dental local anaesthetic solutions on the haemodynamic responses of children undergoing restorative dentistry: a randomised, single-blind, split-mouth study. Br Dent J. 2001;190:502–4.
Mikesell P, Nusstein J, Reader A, Beck M, Weaver J. A comparison of articaine and lidocaine for inferior alveolar nerve blocks. J Endod. 2005;31:265–70. https://doi.org/10.1097/01.don.0000140576.36513.cb.
Mittal M, Sharma S, Kumar A, Chopra R, Srivastava D. Comparison of anesthetic efficacy of articaine and lidocaine during primary maxillary molar extractions in children. Pediatr Dent. 2015;37:520–4.
Paryab M, Arab Z. The effect of Filmed modeling on the anxious and cooperative behavior of 4–6 years old children during dental treatment: a randomized clinical trial study. Dent Res J (isfahan). 2014;11:502–7. https://doi.org/10.4103/1735-3327.139426.
Peretz B, Gluck GM. Assessing an active distracting technique for local anesthetic injection in pediatric dental patients: repeated deep breathing and blowing out air. J Clin Pediatr Dent. 1999;24:5–8.
Prabhakar AR, Marwah N, Raju OS. A comparison between audio and audiovisual distraction techniques in managing anxious pediatric dental patients. J Indian Soc Pedod Prev Dent. 2007;25:177–82. https://doi.org/10.4103/0970-4388.37014.
Primosch RE, Rolland-Asensi G. Comparison of topical EMLA 5% oral adhesive to benzocaine 20% on the pain experienced during palatal anesthetic infiltration in children. Pediatr Dent. 2001;2001(23):11–4.
Ram D, Peretz B. Reactions of children to maxillary infiltration and mandibular block injections. Pediatr Dent. 2001;23:343–6.
Ram D, Amir E, Keren R, Shapira J, Davidovich E. Mandibular block or maxillary infiltration: does it influence children’s opposition to a subsequent dental visit? J Clin Pediatr Dent. 2012;36:245–9.
Raseena KT, Jeeva PP, Kumar A, Balachandran D, Anil A, Ramesh R. A comparative study of tell-show-do technique with and without the aid of a virtual tool in the behavior management of 6–9-year-old children: a nonrandomized, clinical trial. J Indian Soc Pedod Prev Dent. 2020;38:393–9. https://doi.org/10.4103/JISPPD.JISPPD_280_20.
Singh D, Samadi F, Jaiswal JN, Tripathi AM. Stress reduction through audio distraction in anxious pediatric dental patients: an adjunctive clinical study. Int J Clin Pediatr Dent. 2014;7:149–52. https://doi.org/10.5005/jp-journals-10005-1254.
Tirupathi SP, Rajasekhar S. Can single buccal infiltration with 4% articaine induce sufficient analgesia for the extraction of primary molars in children: a systematic literature review. J Dent Anesth Pain Med. 2020;20:179–86. https://doi.org/10.17245/jdapm.2020.20.4.179.
Wong DL, Baker CM. Pain in children: comparison of assessment scales. Pediatr Nurs. 1988;14:9–17.
Acknowledgements
The authors are very grateful to Ms. Antonia Saez for her help in the statistical analysis of the study data and to Dr. María Ledrán for her work in translating the original document into English.
Author information
Authors and Affiliations
Contributions
JA and AML conceived the idea of the study and its general characteristics. JA, AML and EÁ designed the study, defined the sample, established the variables, and chose the techniques and instruments used. AML and MR selected the sample and collected the data. All the authors discussed the results and contributed to the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors did not receive support from any organisation for the piece of work submitted here. The authors have no relevant financial or non-financial interests to disclose.
Ethical approval
The present study was approved by the commission for research and ethics at the CEU-Cardenal Herrera University, Valencia, Spain and was performed in accordance with the 1964 Declaration of Helsinki.
Consent to participate
Prior to commencement of the study, the patients’ parents/guardians were informed, both verbally and in writing, of the study’s objectives and procedures, and signed informed consent for their child’s participation was collected.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Leyda-Menéndez, A.M., Vidigal, E.A., Abanto, J. et al. Efficacy of two behavioural management techniques during inferior alveolar nerve block administration in pre-school children: a randomised clinical trial. Eur Arch Paediatr Dent 24, 85–93 (2023). https://doi.org/10.1007/s40368-022-00758-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40368-022-00758-y