Abstract
Background
The safety and proper utilization of a drug depends not only on its pharmacological action, but also its interactions with other drugs and their metabolites. Therefore, a multifaceted biochemical system must be considered when prescribing any drug.
Objective
The purpose of the present study is to identify potential drug–drug interactions (pDDIs) and investigate their level of severity, onset of action, mechanism of action, and incidence in the medical wards of Benazir Bhutto Shaheed Teaching Hospital, Abbottabad, Pakistan.
Methods
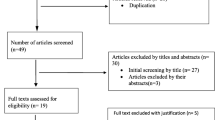
A prospective cross-sectional study was conducted from November 2016 to January 2017 in the medical wards of a teaching hospital. A systematic random sampling technique was used to select patients from the available settings with one in every seven patients selected to provide a sample of 384 patients.
Results
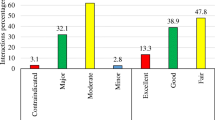
A total of 388 pDDIs were identified, which comprised 86 types of drug combinations. Across all pDDIs, most were of major severity (39.9%), followed by moderate (39.6%) and minor (19.5%) severity and contraindicated (0.7%). A majority of the study participants were male (292; 76%) and the mean age of the patients was 50 years. Overall, 51.0% patients had at least one pDDI.
Conclusion
The overall prevalence of pDDIs is very high in medical wards, and the incidence of pDDIs is primarily associated with polypharmacy and patient age.

Similar content being viewed by others
References
Murtaza G, Khan MYG, Azhar S, et al. Assessment of potential drug–drug interactions and its associated factors in the hospitalized cardiac patients. Saudi Pharm J. 2016;24(2):220–5.
Dai D, Feinstein JA, Morrison W, et al. Epidemiology of polypharmacy and potential drug-drug interactions among pediatric patients in intensive care units of US children’s Hospitals. Pediatr Crit Care Med. 2016;17(5):e218.
Rao C, Shenoy V, Udaykumar P. Potential drug–drug interactions in the pediatric intensive care unit of a tertiary care hospital. J Pharmacol Pharmacother. 2019;10(2):63.
Krähenbühl-Melcher A, Schlienger R, Lampert M, et al. Drug-related problems in hospitals. Drug Saf. 2007;30(5):379–407.
Rodvold KA, Kraus DM. Drug interactions involving anti-infective agents. In: Finch RG, Greenwood D, Norrby SR, Whitley RJ, editors. Antibiotic and chemotherapy: anti-infective agents and their use in therapy. 9th ed. Chatham: Churchill Livingstone; 2010. p. 68–103.
Van Roon EN, Flikweert S, le Comte M, et al. Clinical relevance of drug–drug interactions. Drug Saf. 2005;28(12):1131–9.
Akbar J, Munir AB, Qamar-uz-Zaman M, et al. Potential drug–drug interactions; a study among patients of intensive care unit (ICU) of a tertiary care hospital of South Punjab, Pakistan. J Pharm Pharm Sci. 2019;7(2):78–83.
Ismail M, Iqbal Z, Khattak MB, et al. Potential drug-drug interactions in internal medicine wards in hospital setting in Pakistan. Int J Clin Pharm. 2013;35(3):455–62.
Ismail M, Noor S, Harram U, et al. Potential drug-drug interactions in outpatient department of a tertiary care hospital in Pakistan: a cross-sectional study. BMC Health Serv Res. 2018;18(1):762.
Jia J, Zhu F, Ma X, et al. Mechanisms of drug combinations: interaction and network perspectives. Nat Rev Drug Discov. 2009;8(2):111–28.
Swathi V, Lavanya B, Spandana B, et al. Identification of major drug-drug interactions at tertiary care hospital. Indian J Appl Res. 2019;9(6):42–4.
Zwart-van Rijkom JE, Uijtendaal EV, Ten Berg MJ, et al. Frequency and nature of drug–drug interactions in a Dutch university hospital. Br J Clin Pharmacol. 2009;68(2):187–93.
Bhagavathula AS, Berhanie A, Tigistu H, et al. Prevalence of potential drug-drug interactions among internal medicine ward in University of Gondar Teaching Hospital, Ethiopia. Asian Pac J Trop Biomed. 2014;4:S204–8.
Şimşek A, Macit Ç, Taner N, et al. The importance of computerized drug interaction checker programs to avoid potential drug-drug interactions used in community pharmacies: a preliminary study with clarithromycin. Istanb Med J. 2018;19(3).
Şimşek A, Taner N, Macit Ç, et al. The importance of computerized drug interaction checker programs used in community pharmacies to avoid potential drug interactions: a preliminary study with clarithromycin. Istanb Med J. 2019;20(1):67–71.
Micromedex Database. Greenwood village: Truven health analytics. https://www.micromedexsolutions.com/micromedex2/librarian. Accessed 15 Mar 2018.
Muhammad N, Afridi R. Prevalence, types and predictors of potential drug–drug interactions in an internal medicine ward of the Mardan Medical Complex, Mardan, Kpk, Pakistan. Int J Basic Med Sci Pharm. 2017;6(2):28–32.
de Carvalho RE, Reis AM, de Faria LM, et al. Prevalence of drug interactions in intensive care units in Brazil. Acta Paulista Enfermagem. 2013;26(2):150–7.
El Samia Mohamed S, Gad Z, El-Nimr N, et al. Prevalence and pattern of potential drug–drug interactions in the critical care units of a tertiary hospital in Alexandria, Egypt. Adv Pharmacoepidemiol Drug Saf. 2013;2(144):2167–252.
Reimche L, Forster AJ, van Walraven C. Incidence and contributors to potential drug–drug interactions in hospitalized patients. J Clin Pharmacol. 2011;51(7):1043–50.
Shareef J, Menezes SL, Bhat T. A study on potential drug–drug interactions in medicine department of a multi specialty teaching hospital. J Drug Deliv Ther. 2017;7(6):81–7.
Ahmad A, Khan MU, Haque I, et al. Evaluation of potential drug–drug interactions in general medicine ward of teaching hospital in southern India. J Clin Diagn Res. 2015;9(2):FC10.
Diksis N, Melaku T, Assefa D, et al. Potential drug-drug interactions and associated factors among hospitalized cardiac patients at Jimma University Medical Center, Southwest Ethiopia. SAGE Open Med. 2019;7:2050312119857353.
Kumaraswamy R, Ramani J, Ramesh B, et al. Prevalence of polypharmacy and drug to drug interactions in a tertiary care teaching hospital. Int Res J Pharm. 2014;5(10):778–82.
Kaliamurthy K, Kumar A, Punniyakotti S, et al. Study of drug-drug interactions in general medicine department of a tertiary care hospital. J Appl Pharm Sci. 2015;5(12):122–4.
Tesfaye ZT, Nedi T. Potential drug–drug interactions in inpatients treated at the internal medicine ward of Tikur Anbessa Specialized Hospital. Drug Healthc Patient Saf. 2017;9:71–6.
Bajracharya N, Swaroop AM, Rajalekshmi SG, et al. Incidence of drug-drug interactions among patients admitted to the department of general medicine in a tertiary care hospital. J Young Pharm. 2018;10(4):450–5.
Jimmy O, ShobhaRani R, Indira R, et al. Study of drug-drug interactions in the medication charts in medicine wards at a tertiary care hospital, Bangalore. Indian J Pharm Pract. 2012;5(4):61–4.
Getachew H, Assen M, Dula F, et al. Potential drug–drug interactions in pediatric wards of Gondar University Hospital, Ethiopia: a cross sectional study. Asian Pac J Trop Biomed. 2016;6(6):534–8.
Santibáñez C, Roque J, Morales G, et al. Characteristics of drug interactions in a pediatric intensive care unit. Rev Chil Pediatr. 2014;85(5):546–53.
Vonbach P, Dubied A, Krähenbühl S, et al. Prevalence of drug–drug interactions at hospital entry and during hospital stay of patients in internal medicine. Eur J Inter Med. 2008;19(6):413–20.
Shakeel F, Aamir M, Khan AF, et al. Epidemiology of potential drug-drug interactions in elderly population admitted to critical care units of Peshawar, Pakistan. BMC Pharmacol Toxicol. 2018;19(1):85.
Shalavadi M, Chandrashekhar V, Manohar K, et al. A prospective study on prescription pattern of antihypertensive drugs and drug interactions at a tertiary care teaching hospital. Am J Pharmacol. 2018;1(2):1010.
Vonbach P, Dubied A, Krähenbühl S, et al. Evaluation of frequently used drug interaction screening programs. Pharm World Sci. 2008;30(4):367–74.
Acknowledgements
The authors are thankful to the medical superintendent of the Benazir Bhutto Shaheed Hospital (BBSH), Abbottabad, Pakistan for providing facilities and co-operation during this study and also to the patients who gave their informed consent.
Author information
Authors and Affiliations
Contributions
TK, KM, and NUR were involved in the concept, design, and data collection of the study. FS and ZK carried out the statistical analysis. All authors were involved in the interpretation of the data. TK wrote the first draft of the manuscript, and all authors contributed to subsequent drafts.
Corresponding author
Ethics declarations
Funding
The study was not funded.
Conflict of interest
Tariq Khan, Khayal Muhammad, Fazal Subhan, Zakir Khan, and Nisar-Ur-Rehman declare no potential conflicts of interest related to the content of this study.
Ethical approval
Ethical approval was granted by the ethical committee of COMSATS University Islamabad, Abbottabad campus. Approval was also received from the Medical superintendent of BBSH Abbottabad (ref. no. 1123/09-2016).
Consent
The purpose and protocols of the study were explained to patients, and written or oral consent was obtained.
Rights and permissions
About this article
Cite this article
Khan, T., Muhammad, K., Subhan, F. et al. Frequency and nature of potential drug–drug interaction in medical wards: a cross-sectional study in a teaching hospital. Drugs Ther Perspect 36, 158–165 (2020). https://doi.org/10.1007/s40267-020-00710-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40267-020-00710-4