Abstract
Purpose
Mohs’ paste, which is composed of zinc chloride and zinc oxide starch, is used for hemostasis of superficial malignancy in the clinical setting. We investigated the concentration of intramuscular zinc in mice after Mohs’ paste application and evaluated its relationship with angiogenesis from the perspective of blood flow levels within 24 h.
Methods
Male C57BL/6JJmsSlc mice were administered single dose of Mohs’ paste at 25%, 50%, and 75% after unilateral hind limb surgery, and glycerin, a viscosity modifier, was administered to the control group (0%). Hind limb blood flow levels were measured with a laser Doppler perfusion imaging system (n = 6). The amounts of intramuscular zinc and vascular endothelial growth factor-A (VEGF-A) expression were analyzed using inductively coupled plasma mass spectrometry (ICP-MS) and western blotting, respectively (n = 5 or 3).
Results
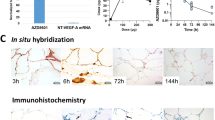
Blood flow levels were significantly decreased in the 50% group after 8 h, and significantly decreased in the 25% and 50% groups after 24 h. Intramuscular zinc was significantly increased in the 50% and 75% groups after 8 h. Western blotting showed that VEGF-A levels were significantly increased in the 25% and 50% groups after 8 h. Based on analytical experiments and biological investigation, we predicated the pharmacological effect of Mohs’ paste and found over 50% of it is critical in the blood flow and angiogenesis suppression after more than 8 h of its application.
Conclusions
The results suggest that the mechanism of blood flow suppression is independent of VEGF-A levels and might suppress future angiogenesis. Our findings support that of previous studies, in which Mohs’ paste was expected to induce hemostasis and suppress angiogenesis. It is an excellent ointment that facilitates hemostasis by suppressing blood flow regardless of angiogenesis, and may be apt for situations where hemostasis is required in the clinical setting.
Graphical abstract




Similar content being viewed by others
Data Availability
The data supporting the findings of this study are available from the corresponding author, [NI], upon reasonable request.
Code availability
All source codes are available from the corresponding author, [NI], upon reasonable request.
Abbreviations
- ICP-MS:
-
Inductively coupled plasma mass spectrometry
- VEGF:
-
Vascular endothelial growth factor
- iNOS:
-
Inducible nitric oxide synthase
- ZIP:
-
Zrt- and Irt-like protein
- ZFP:
-
Zinc finger proteins
- ZnT:
-
Zinc transporter
- ZnR:
-
Zinc-sensing receptor
- ADP:
-
Adenosine diphosphate
- GPR39:
-
G protein-coupled receptor 39
- PLC:
-
Phospholipase C
- PI3:
-
Phosphoinositide 3
- MAP:
-
Mitogen-activated protein
- HIF:
-
Hypoxia-inducible factor
References
Prommer E. Management of bleeding in the terminally ill patient. Hematology. 2005;10:167–75.
Mohs FE, Guyer MF. Pre-excisional fixation of tissues in the treatment of cancer in rats. Can Res. 1941;1:49–51.
Mohs FE. Chemosurgery: a microscopically controlled method of cancer excision. Arch Surg. 1941;42:279–95.
Tsunemasa O, Tsutomu O, Yuji U, Kiyohisa O, Masato S, Toyoaki O. Chemosurgical ointment (in Japanese). Medical Journal of Takayama Red Cross Hospital. 2000;24:8–11.
Tsukada T, Nakano T, Matoba M, Matsui D, Sasaki S. Locally advanced breast cancer made amenable to radical surgery after a combination of systemic therapy and Mohs paste: two case reports. J Med Case Rep. 2012;6:360.
Shigeyama M, Ohkubo T. No.2 (in Japanese). medical forum CHUGAI. 2010;14:1–8.
Shigeyama M, Ogaya T, Ookubo T. Participation in chemosurgical treatment for patients with unresectable cancer (in Japanese). Iyaku J. 2005;41:131–6.
Kakimoto M, Tokita H, Okamura T, Yoshino K. A chemical hemostatic technique for bleeding from malignant wounds. J Palliat Med. 2010;13:11–3.
Izumo N, Shigeyama M, Taguchi M, Nagashima D, Nagano S, Kikuchi E, et al. Application of mohs’ paste to treat hemorrhages induced by disintegrated breast cancer tumors and evaluation of this hemostatic mechanism using an animal model. Jpn Iryo Yakugaku (Japanese Journal of Pharmaceutical Health Care and Sciences). 2016;42:246–54.
Yanazume S, Douzono H, Yanazume Y, Iio K, Douchi T. New hemostatic method using Mohs’ paste for fatal genital bleeding in advanced cervical cancer. Gynecol Oncol Case Rep. 2013;4:47–9.
Roohani N, Hurrell R, Kelishadi R, Schulin R. Zinc and its importance for human health: an integrative review. J Res Med Sci. 2013;18:144–57.
Beyersmann D. Homeostasis and cellular functions of zinc. Mat Wiss U Werkstofftech. 2002;33:764–9.
Chasapis CT, Loutsidou AC, Spiliopoulou CA, Stefanidou ME. Zinc and human health: an update. Arch Toxicol. 2012;86:521–34.
Andersen MK, Krossa S, Høiem TS, Buchholz R, Claes BSR, Balluff B, et al. Simultaneous detection of zinc and its pathway metabolites using MALDI MS imaging of prostate tissue. Anal Chem. 2020;92:3171–9.
Carmeliet P. Angiogenesis in life, disease and medicine. Nature. 2005;438:932–6.
Chen CH, Walterscheid JP. Plaque angiogenesis versus compensatory arteriogenesis in atherosclerosis. Circ Res. 2006;99:787–9.
Shibuya M. Vascular endothelial growth factor and its receptor system: physiological functions in angiogenesis and pathological roles in various diseases. J Biochem. 2013;153:13–9.
Apte RS, Chen DS, Ferrara N. VEGF in signaling and disease: Beyond discovery and development. Cell. 2019;176:1248–64.
Hozain S, Hernandez A, Fuller J, Sharp G, Cottrell J. Zinc chloride affects chondrogenesis via VEGF signaling. Exp Cell Res. 2021;399:112436.
Zhu D, Su Y, Zheng Y, Fu B, Tang L, Qin YX. Zinc regulates vascular endothelial cell activity through zinc-sensing receptor ZnR/GPR39. Am J Physiol Cell Physiol. 2018;314:C404–14.
Pasqualini R, Barbas CF 3rd, Arap W. Vessel maneuvers: zinc fingers promote angiogenesis. Nat Med. 2002;8:1353–4.
Hao G, Dawson J, Lee G, Longley R. Zinc supplementation protects human endostatin Fc fusion against proteolytic degradation during cell culture. Protein Expr Purif. 2014;93:18–22.
Boehm T, O’reilly MS, Keough K, Shiloach J, Shapiro R, Folkman J. Zinc-binding of endostatin is essential for its antiangiogenic activity. Biochem Biophys Res Commun. 1998;252:190–4.
Gordon PR, Woodruff CW, Anderson HL, O’Dell BL. Effect of acute zinc deprivation on plasma zinc and platelet aggregation in adult males. Am J Clin Nutr. 1982;35:113–9.
Mammadova-Bach E, Braun A. Zinc homeostasis in platelet-related diseases. Int J Mol Sci. 2019;20:5258.
Couffinhal T, Silver M, Zheng LP, Kearney M, Witzenbichler B, Isner JM. Mouse model of angiogenesis. Am J Pathol. 1998;152:1667–79.
Ruvinov E, Leor J, Cohen S. The effects of controlled HGF delivery from an affinity-binding alginate biomaterial on angiogenesis and blood perfusion in a hindlimb ischemia model. Biomaterials. 2010;31:4573–82.
Gerber N, Brogioli R, Hattendorf B, Scheeder MR, Wenk C, Günther D. Variability of selected trace elements of different meat cuts determined by ICP-MS and DRC-ICPMS. Animal. 2009;3:166–72.
Moore RE, Larner F, Coles BJ, Rehkämper M. High precision zinc stable isotope measurement of certified biological reference materials using the double spike technique and multiple collector-ICP-MS. Anal Bioanal Chem. 2017;409:2941–50.
Yamauchi T, Yamano Y, Yamanaka K, Hata A, Nakadate T, Kuroda Y, et al. Possible production of arsenic hemoglobin adducts via exposure to arsine. J Occup Health. 2015;57:161–8.
Yokoyama Y, Sato K, Furuta N. Determination of Fe, Cu, Zn, Se and As in biological samples using ICP-ion trap mass spectrometer. Bunseki Kagaku. 2006;55:587–94.
Terada K, Kojima Y, Watanabe T, Izumo N, Chiba K, Karube Y. Inhibition of nerve growth factor-induced neurite outgrowth from PC12 cells by dexamethasone: signaling pathways through the glucocorticoid receptor and phosphorylated Akt and ERK1/2. PLOS ONE. 2014;9:e93223.
Nagashima D, Zhang L, Kitamura Y, Ichihara S, Watanabe E, Zong C, et al. Proteomic analysis of hippocampal proteins in acrylamide-exposed Wistar rats. Arch Toxicol. 2019;93:1993–2006.
King JC, Shames DM, Woodhouse LR. Zinc homeostasis in humans. J Nutr. 2000;130:1360S-S1366.
Condomina J, Zornoza-Sabina T, Granero L, Polache A. Kinetics of zinc transport in vitro in rat small intestine and colon: Interaction with copper. Eur J Pharm Sci. 2002;16:289–95.
Kondaiah P, Yaduvanshi PS, Sharp PA, Pullakhandam R. Iron and zinc homeostasis and interactions: Does enteric zinc excretion cross-talk with intestinal iron absorption? Nutrients. 2019;11:1885.
Tomas-Sanchez C, Blanco-Alvarez VM, Gonzalez-Barrios JA, Martinez-Fong D, Garcia-Robles G, Soto-Rodriguez G, et al. Prophylactic chronic zinc administration increases neuroinflammation in a hypoxia-ischemia model. J Immunol Res. 2016;2016:4039837.
Boehm T, O’Reilly MS, Keough K, Shiloach J, Shapiro R, Folkman J. Zinc-binding of endostatin is essential for its antiangiogenic activity. Biochem Biophys Res Commun. 1998;252:190–4.
Fu Y, Tang H, Huang Y, Song N, Luo Y. Unraveling the mysteries of endostatin. IUBMB Life. 2009;61:613–26.
Jazwa A, Florczyk U, Grochot-Przeczek A, Krist B, Loboda A, Jozkowicz A, et al. Limb ischemia and vessel regeneration: Is there a role for VEGF? Vasc Pharmacol. 2016;86:18–30.
Samura M, Hosoyama T, Takeuchi Y, Ueno K, Morikage N, Hamano K. Therapeutic strategies for cell-based neovascularization in critical limb ischemia. J Transl Med. 2017;15:49.
Acknowledgements
We thank Mr. Shota Nagano for his generous help in the experiment. We thank Ms. Yuki Yagihara for her excellent secretarial support. We also acknowledge the help and support of Masato Shigeyama, Graduate School of Health and Medicine, Gifu University of Medical Science, throughout the study. We would like to thank Editage (www.editage.com) for English language editing.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Nagashima, D., Furukawa, M., Yamano, Y. et al. Zinc-containing Mohs’ paste affects blood flow and angiogenesis suppression. DARU J Pharm Sci 29, 321–328 (2021). https://doi.org/10.1007/s40199-021-00409-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40199-021-00409-5