Abstract
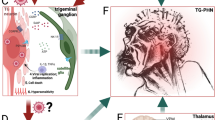
The purpose of this study is to diagnose herpesvirus infections in refractory atypical trigeminal neuralgia, to assess pathogenetic links, and to explore the efficacy of antiviral treatment. In a prospective controlled study, 95 patients with trigeminal neuralgia received antiviral therapy (valacyclovir + alpha2b-interferon) (experimental group, EG). Other patients refused to receive treatment (control group 1 (CG1), n = 31). Control group 2 (CG2) included 32 healthy individuals of the same age and sex. Herpesvirus infection was diagnosed in blood leukocytes by PCR (Biocom, Russian Federation). Serum concentrations of IgM, IgA and IgG to HSV-1/2, VZV (ELISA, Vector-Best, Russian Federation) were determined. Reactivation of herpesvirus infections was observed in the EG in 87% of cases. The heterogeneity of herpesvirus-associated damage of trigeminal nerves and anatomically related areas of the central nervous system (CNS) has been demonstrated. The treatment applied was effective for herpesvirus infection (77%) and pain (61%) and ineffective for immunity correction (26% of cases). Atypical refractory trigeminal neuralgia is associated with herpesvirus infections that reactivate due to minor immunodeficiencies. Antiviral treatment suppresses herpesviruses and reduces the intensity of pain.




Similar content being viewed by others

Data availability
Data will be available on request.
References
Guasp M, Landa J, Martinez-Hernandez E, Sabater L, Iizuka T, Simabukuro M, et al. Thymoma and autoimmune encephalitis: clinical manifestations and antibodies. Neurol Neuroimmunol Neuroinflamm. 2021;8(5): e1053. https://doi.org/10.1212/NXI.0000000000001053.
Handa S, Keith DA, Abou-Ezzi J, Rosèn A, et al. Neuropathic orofacial pain Characterization of different patient groups using the ICOP first edition, in a tertiary level Orofacial Pain Clinic. Oral Surg Oral Med Oral Pathol Oral Radiol. 2021;132(6):653–61. https://doi.org/10.1016/j.oooo.2021.07.021.
Singhal S, Danks RA. Radiological and neurosurgical diagnosis of arterial neurovascular conflict on MRI for trigeminal neuralgia. World Neurosurg. 2021;157:e166–72. https://doi.org/10.1016/j.wneu.2021.09.115.
Adachi M. A case of Varicella zoster virus polyneuropathy: involvement of the glossopharyngeal and vagus nerves mimicking a tumor. AJNR Am J Neuroradiol. 2008;29(9):1743–5. https://doi.org/10.3174/ajnr.A1141.
Gilden DH, Cohrs RJ, Hayward AR, Wellish M, Mahalingam R. Chronic varicella-zoster virus ganglionitis—a possible cause of postherpetic neuralgia. J Neurovirol. 2003;9(3):404–7. https://doi.org/10.1080/13550280390201722.
Krohel GB, Richardson JR, Farrell DF. Herpes simplex neuropathy. Neurology. 1976;26(6 PT 1):596–7. https://doi.org/10.1212/wnl.26.6.596.
Fedirko V. On pathogenesis of Cranial nerves hyperactive dysfunction syndrome. 13th European Congress of Neurosurgery, Glasgow (UK), September 2–7, 2007: 655–9.
Peñarrocha M, Bagán JV, Alfaro A, Peñarrocha M. Acyclovir treatment in 2 patients with benign trigeminal sensory neuropathy. J Oral Maxillofac Surg. 2001;59(4):453–6. https://doi.org/10.1053/joms.2001.21887.
Zhou J, Li J, Ma L, Cao S. Zoster sine herpete: a review. Korean J Pain. 2020;33(3):208–15.
Ramos F, Monforte C, Luengo A. Acute sensory neuropathy associated with a varicella-zoster infection. Rev Neurol. 1999;28(11):1067–9.
Liu W, Pu B, Liu M, Zhang X, Zeng R. Down-regulation of MAPK pathway alleviates TRPV4-mediated trigeminal neuralgia by inhibiting the activation of histone acetylation. Exp Brain Res. 2021;239(11):3397–404. https://doi.org/10.1007/s00221-021-06194-6.
Stalker WH. Facial neuralgia associated with recurrent herpes simplex. Oral Surg Oral Med Oral Pathol. 1980;49(6):502–3.
Roullet E, Assuerus V, Gozlan J, Ropert A, Saïd G, Baudrimont M, et al. Cytomegalovirus multifocal neuropathy in AIDS: analysis of 15 consecutive cases. Neurology. 1994;44(11):2174–82. https://doi.org/10.1212/wnl.44.11.2174.
Farahani RM, Marsee DK, Baden LR, Woo SB, Treister NS. Trigeminal trophic syndrome with features of oral CMV disease. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2008;106(3):e15–8. https://doi.org/10.1016/j.tripleo.2008.05.002.
Hüfner K, Arbusow V, Himmelein S, Derfuss T, Sinicina I, Strupp M, et al. The prevalence of human herpesvirus 6 in human sensory ganglia and its co-occurrence with alpha-herpesviruses. J Neurovirol. 2007;13(5):462–7. https://doi.org/10.1080/13550280701447059.
Ptaszyńska-Sarosiek I, Dunaj J, Zajkowska A, Niemcunowicz-Janica A, Król M, Pancewicz S, et al. Post-mortem detection of six human herpesviruses (HSV-1, HSV-2, VZV, EBV, CMV, HHV-6) in trigeminal and facial nerve ganglia by PCR. PeerJ. 2019;6:e6095. https://doi.org/10.7717/peerj.6095.
Neroyev VV, Saakian SV, Miakoshina EB, Iurovskaia NN, Riabina MV, Zaĭtseva OV, Lysenko VS. Differential diagnosis of early central choroidal melanoma and late stage age-related macula degeneration. Vestn oftalmol. 2013;129(1):39–45.
Chan J, Bergstrom RT, Lanza DC, Oas JG. Lateral sinus thrombosis associated with zoster sine herpete. Am J Otolaryngol. 2004;25(5):357–60. https://doi.org/10.1016/j.amjoto.2004.03.007.
Nagel MA, Niemeyer CS, Bubak AN. Central nervous system infections produced by varicella zoster virus. Curr Opin Infect Dis. 2020;33(3):273–8. https://doi.org/10.1097/QCO.0000000000000647.
Wipfler P, Dunn N, Beiki O, et al. The viral hypothesis of mesial temporal lobe epilepsy—is human herpes virus-6 the missing link? A systematic review and meta-analysis Seizure. 2018;54:33–40.
Li CMF, Chu PPW, Hung PS, Mikulis D, Hodaie M. Standardizing T1-w/T2-w ratio images in trigeminal neuralgia to estimate the degree of demyelination in vivo. Neuroimage Clin. 2021;32:102798. https://doi.org/10.1016/j.nicl.2021.102798.
Saakyan SV, Zharua AA, Myakoshina EB, Lazareva LA, Yakovlev SB. Superselective intra-arterial chemotherapy treatment for resistant and severe retinoblastoma. Russ Pediatr Ophthalmol. 2013;1:31–4.
Saakyan SV, Myakoshina EB, Yurovskaya NN. Tumor-associated distant maculopathy caused by small uveal melanoma. Russ Ophthalmol J. 2011;4(2):41–5.
Rusbridge C. Neurobehavioral disorders: the corticolimbic system in health and disease. Vet Clin North Am Small Anim Pract. 2020;50(5):1157–81. https://doi.org/10.1016/j.cvsm.2020.06.009.
Alper J, Seifert AC, Verma G, Huang KH, Jacob Y, Al Qadi A, et al. Leveraging high-resolution 7-tesla MRI to derive quantitative metrics for the trigeminal nerve and subnuclei of limbic structures in trigeminal neuralgia. J Headache Pain. 2021;22(1):112. https://doi.org/10.1186/s10194-021-01325-4.
Engdahl E, Niehusmann P, Fogdell-Hahn A. The effect of human herpesvirus 6B infection on the MAPK pathway. Virus Res. 2018;256:134–41. https://doi.org/10.1016/j.virusres.2018.08.014.
Jacobs BM, Giovannoni G, Cuzick J, Dobson R. Systematic review and meta-analysis of the association between Epstein-Barr virus, multiple sclerosis and other risk factors. Mult Scler. 2020;26(11):1281–97. https://doi.org/10.1177/1352458520907901.
Pormohammad A, Azimi T, Falah F, Faghihloo E. Relationship of human herpes virus 6 and multiple sclerosis: a systematic review and meta-analysis. J Cell Physiol. 2018;233(4):2850–62. https://doi.org/10.1002/jcp.26000.
Spirin NN, Kiselev DV, Karpova MS. Neuropathic pain syndromes in patients with multiple sclerosis. Zh nevrol psikhiatr im SS Korsakova. 2021;121(7):22–30. https://doi.org/10.17116/jnevro202112107222.
Venâncio P, Brito MJ, Pereira G, Vieira JP. Anti-N-methyl-D-aspartate receptor encephalitis with positive serum antithyroid antibodies, IgM antibodies against mycoplasma pneumoniae and human herpesvirus 7 PCR in the CSF. Pediatr Infect Dis J. 2014;33(8):882–3.
Schwenkenbecher P, Skripuletz T, Lange P, Dürr M, Konen FF, Möhn N, et al. Intrathecal antibody production against epstein-barr, herpes simplex, and other neurotropic viruses in autoimmune encephalitis. Neurol Neuroimmunol Neuroinflamm. 2021;8(6): e1062. https://doi.org/10.1212/NXI.0000000000001062.
Magen E, Schlesinger M, David M, Ben-Zion I, Vardy D. Selective IgE deficiency, immune dysregulation, and autoimmunity. Allergy Asthma Proc. 2014;35(2):e27-33. https://doi.org/10.2500/aap.2014.35.3734.
Smith JK, Krishnaswamy GH, Dykes R, Reynolds S, Berk SL. Clinical manifestations of IgE hypogammaglobulinemia. Ann Allergy Asthma Immunol. 1997;78(3):313–8. https://doi.org/10.1016/S1081-1206(10)63188-2.
Gujadhur A, Thomson N, Aung AK, Catriona M, Solomon M. CMV sinusitis in a HIV-negative renal transplant recipient. Transplantation. 2014;97(9):e55–7. https://doi.org/10.1097/TP.0000000000000114.
Bogduk N, Gavind J. Cervicogenic headache: an assessment of the evidence on clinical diagnosis, invasive tests, and treatment. Lancet Neurol. 2009;8(10):959–68. https://doi.org/10.1016/S1474-4422(09)70209-1.
Mitrofanova LB, Mitrofanov NA, Shliakhto EV, Koval’skiĭ GB. Spinal osteochondrosis, mesenchymal dysplasia and herpes infection. Arkh Patol. 2006;68(6):23–5.
Vurdelja RB, Budincević H, Prvan MP. Central poststroke pain. Lijec Vjesn. 2008;130(7–8):191–5.
Pazos-Añón R, Machado-Costa C, Farto E, Abreu J. Ramsay-Hunt syndrome complicated with cerebral venous thrombosis in an HIV-1-infected patient. Enferm Infec Microbiol Clin. 2007;25(1):69–70. https://doi.org/10.1016/s0213-005x(07)74232-5.
Farooqi AA, Gulnara K, Mukhanbetzhanovna AA, Datkhayev U, Kussainov AZ, Adylova A. Regulation of RUNX proteins by long non-coding RNAs and circular RNAs in different cancers. Noncoding RNA Res. 2021;6(2):100–6. https://doi.org/10.1016/j.ncrna.2021.05.001.
Egoshin VL, Ivanov SV, Savvina NV, Kapanova GZ, Grjibovski AM. Basic principles of biomedical data analysis in R. Ekologiya cheloveka (Human Ecol). 2018;7:55–64.
Miranda CM, Torres TJP, Larrañaga LC, Acuña LG. Meningomyelitis associated with infection by human herpes virus 7: report of two cases. Rev Med Chil. 2011;139(12):1588–91.
Galin P, Galyaveeva A, Bataev H, Safonov V. The role of micronutrients and vitamins in the prevention and remote treatment of heart failure. Rev Latinoam de Hipertens. 2020;15(1):26–32.
Merigan TC, Gallagher JG, Pollard RB, Arvin AM. Short-course human leukocyte interferon in treatment of herpes zoster in patients with cancer. Antimicrob Agents Chemother. 1981;19(1):193–5. https://doi.org/10.1128/AAC.19.1.193.
Biron CA, Byron KS, Sullivan JL. Severe herpesvirus infections in an adolescent without natural killer cells. N Engl J Med. 1989;320(26):1731–5. https://doi.org/10.1056/NEJM198906293202605.
Banovic T, Yanilla M, Simmons R, Robertson I, Schroder WA, Raffelt NC, et al. Disseminated varicella infection caused by varicella vaccine strain in a child with low invariant natural killer T cells and diminished CD1d expression. J Infect Dis. 2011;204(12):1893–901. https://doi.org/10.1093/infdis/jir660.
Almerigogna F, Fassio F, Giudizi MG, Biagiotti R, Manuelli C, Chiappini E, et al. Natural killer cell deficiencies in a consecutive series of children with herpetic encephalitis. Int J Immunopathol Pharmacol. 2011;24(1):231–8. https://doi.org/10.1177/039463201102400128.
Kallio-Laine K, Seppänen M, Aittoniemi J, Kautiainen H, Seppälä I, Valtonen V, et al. HLA-DRB1*01 allele and low plasma immunoglobulin G1 concentration may predispose to herpes-associated recurrent lymphocytic meningitis. Hum Immunol. 2010;71(2):179–81. https://doi.org/10.1016/j.humimm.2009.10.014.
Picado C, de Landazuri IO, Vlagea A, Bobolea I, Arismendi E, Amaro R. Spectrum of disease manifestations in patients with selective immunoglobulin E deficiency. J Clin Med. 2021;10(18):4160. https://doi.org/10.3390/jcm10184160.
Yoshikawa T, Ihira M, Asano Y, et al. Fatal adult case of severe lymphocytopenia associated with reactivation of human herpesvirus 6. J Med Virol. 2002;66(1):82–5.
Backström E, Chambers BJ, Ho EL, Naidenko OV, Mariotti R, Fremont DH, et al. Natural killer cell-mediated lysis of dorsal root ganglia neurons via RAE1/NKG2D interactions. Eur J Immunol. 2003;33(1):92–100. https://doi.org/10.1002/immu.200390012.
Acknowledgements
Not applicable.
Funding
The study was performed as a fragment of scientific work commissioned by the Ministry of Health of Ukraine, grant No. 0121U107940.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by DM. The first draft of the manuscript was written by VF. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics approval
The research complies with the guidelines for human studies and was conducted ethically in accordance with the World Medical Association Declaration of Helsinki. The author declares that the work is written with due consideration of ethical standards. The study was conducted in accordance with the ethical principles approved by the Human Experiments Ethics Committee of O'Bogomolets National Medical University (protocol No. 140, 21.12.2020).
Consent to publish
Not applicable.
Informed consent
The written informed consent was obtained from participants.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Maltsev, D., Fedirko, V. Refractory atypical trigeminal neuralgia associated with reactivated herpesvirus infection: pathogenetic link and efficacy of combination antiviral therapy. VirusDis. 33, 155–165 (2022). https://doi.org/10.1007/s13337-022-00769-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13337-022-00769-9