Abstract
Introduction
and hypothesis.
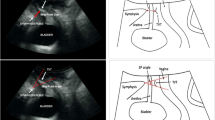
We evaluated different bladder parameters using Transperineal Ultrasound (TPUS) in patients with apical pelvic organ prolapse undergoing lateral suspension or sacropexy.
Methods
We included 73 cases with 37 cases in lateral suspension (LS) group and 36 cases in sacropexy group. We enrolled cases with apical prolapse stage 2 or higher according to Pelvic Organ Prolapse Quantification system (POP-Q). Evaluation done of all cases using TPUS preoperatively and at 6, 12 and 18 months follow-up visits.
Results
In LS group we found significant differences postoperatively in bladder neck height (Dy distance) at Valsalva and rest (P value < 0.001 in both) and in β angle at Valsalva and rest (P value < 0.001 in both). There was significant improvement in PVR (P value < 0.001). In sacropexy group we found no significant differences postoperatively in bladder neck height at Valsalva (P value 0.07) or in β angle at Valsalva (P value 0.097). There was significant improvement in PVR (P value 0.006). In between the 2 groups, there was better improvement in LS group than sacropexy group in bladder neck height at rest (P value 0.001) and in β angle both at Valsalva and rest (P value < 0.001 & 0.002 respectively). There was no significant difference in PVR, bladder wall thickness or bladder neck funnelling.
Conclusion
LS and sacropexy showed good postoperative improvement in some bladder parameters using TPUS with better improvement in bladder neck height in LS.
Clinical Trial Registration
Clinical trial ID: NCT03772691.


Similar content being viewed by others
References
Norton P, Brubaker L, Nager CW, et al. Pelvic organ prolapse in a cohort of women treated for stress urinary incontinence. Am J Obstet Gynecol. 2014;211:e1-5.
Olsen AL, Smith VJ, Bergstrom JO, et al. Epidemiology of surgically managed pelvic organ prolapse and urinary incontinence. Obstet Gynecol. 1997;89:501–6.
Abrams P, Cardozo L, Fall M et al. The standardisation of terminology in lower urinary tract function: report from the standardisation sub-committee of the International Continence Society. Urol J. 2003;61(1):37–49.
Summers A, Winkel LA, Hussain HK, et al. The relationship between anterior and apical compartment support. Am J Obstet Gynecol. 2006;194:1438–43.
Patel BN, Smith JJ, Badlani GH. Minimizing the cost of surgical correction of stress urinary incontinence and prolapse. Urology. 2009;74:762–4.
Amaral MOP, Coutinho EC, Nelas PAAB, et al. Risk factors associated with urinary incontinence in Portugal and the quality of life of affected women. Int J Gynecol Obstet. 2015;131:82–6.
Grzybowska ME, Wydra D, Smutek J. Analysis of the usage of continence pads and help-seeking behavior of women with stress urinary incontinence in Poland. BMC Womens Health. 2015;15:1–6.
Orietta D*, Pierpaolo C. Role of perineal ultrasound in the evaluation of urinary stress incontinence and pelvic organ prolapse: a systematic review. Neurourol Urodyn. 2006;25:301–306.
Tunn R, Schaer GN, Peschers UM et al. Updated recommendations on ultrasonography in urogynecology. Int Urogynecol J. 2005;16:236–41.
Chantarasorn V, Dietz HP. Diagnosis of cystocele type by clinical examination and pelvic floor ultrasound. Ultrasound Obstet Gynecol. 2012;39:710–4.
Nygaard IE, McCreery R, Brubaker L, et al. Pelvic floor disorders network. Abdominal sacrocolpopexy: A comprehensive review. Obstet Gynecol 2004; 104:805–23.
Wong V, Guzman Rojas R, Shek KL et al. Laparoscopic sacrocolpopexy: how low does the mesh go? Ultrasound Obstet Gynecol. 2017;49(3):404–8.
Leruth J, Fillet M, Waltregny D. Incidence and risk factors of postoperative stress urinary incontinence following laparoscopic sacrocolpopexy in patients with negative preoperative prolapse reduction stress testing. Int Urogynecol J. 2013;24(3):485–91.
Veit-Rubin N, Dubuisson J-B, Lange S et al.. Uterus-preserving laparoscopic lateral suspension with mesh for pelvic organ prolapse: a patient-centered outcome report and video of a continuous series of 245 patients. Int Urogynecol J. 2016;27:491–3.
Isenlik BS, Aksoy O, Erol O, et al. Comparison of laparoscopic lateral suspension and laparoscopic sacrocolpopexy with concurrent total laparoscopic hysterectomy for the treatment of pelvic organ prolapse: a randomized controlled clinical trial. Int Urogynecol J. 2023;34(1):231–8.
Price N, Jackson S, Avery KNL, et al. Development and psychometric evaluation of the ICIQ Vaginal Symptoms Questionnaire: the ICIQ‐VS. BJOG Int J Obstet Gynaecol. 2006;113.
Brookes S, Donovan JL, Wright M, et al. A scored form of the Bristol Female Lower Urinary Tract Symptoms questionnaire: data from a randomized controlled trial of surgery for women with stress incontinence. Am J Obstet Gynecol. 2004;191(1):73–82.
Schaer GN, Koechli OR, Schuessler B, et al. Perineal ultrasound for evaluating the bladder neck in urinary stress incontinence. Obstet Gynecol. 1995;85:220–4.
Li YQ, Geng J, Tan C et al. Diagnosis and classification of female stress urinary incontinence by transperineal two dimensional ultrasound. Technol Health Care. 2017;25:859–66.
Shek KL, Pirpiris A, Dietz HP. Does levator avulsion increase urethral mobility? Eur J Obstet Gynecol Reprod Biol. 2010;153:215–9.
Pirpiris A, Shek KL, Dietz HP. Urethral mobility and urinary incontinence. Ultrasound Obstet Gynecol. 2010;36:507–11.
Yassa M, Tug N. Uterus-preserving laparoscopic lateral suspension with mesh operation in pelvic organ prolapse: initial experience in a single tertiary center with a median 24-month follow-up. Geburtshilfe Frauenheilkd. 2019;79(9):983–92.
Huang WC, Yang SH, Yang JM. Clinical importance and surgical outcomes of green type III cystocele in women with anterior vaginal prolapse. J Ultrasound Med 2015; 34(12):2279–85.
Funding
No funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were consistent with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its comparable ethical standards. Ethics approval: approved by the Ethical Review Committee of Faculty of Medicine Asyut University with IRB number 17200283.
Consent for publication
Authors state that the work described has not been published before, it is not under consideration for publication anywhere else and its publication has been approved by all co-authors. All authors agreed with the content and that all gave explicit consent to submit and that they obtained consent from the responsible authorities at the institute/organization where the work has been carried out. All authors (1) made substantial contributions to the conception or design of the work; or the acquisition, analysis, or interpretation of data; or the creation of new software used in the work; (2) drafted the work or revised it critically for important intellectual content; (3) approved the version to be published; and (4) agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Informed Consent
Informed consent was obtained from all participants included in the study. Written consent is taken before operations.
Point of Transparency
Authors state that this work is based on earlier work.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Ezzat Sayed is a Professor, Abubakr Mitwally is a Professor, Ahmed Abdelmagied is a Professor, Ahmed Fetih is a Professor, Mohamed Fekry is a Master degree Urogynaecology, Assistant Lecturer.
Appendix
Appendix
CONSORT Flow diagram
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sayed, E., Mitwally, A., Abdelmagied, A. et al. Transperineal Ultrasound Evaluation of Bladder Parameters in Patients with Apical Prolapse Undergoing Lateral Suspension or Sacropexy. J Obstet Gynecol India 74, 170–175 (2024). https://doi.org/10.1007/s13224-023-01912-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13224-023-01912-2