Abstract
Introduction
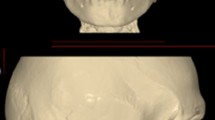
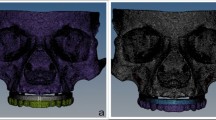
The residual post-COVID maxillary mucormycosis defect (PCMMD) were extensive, due to unilateral or bilateral maxillectomies. The Goal of rehabilitation of PCMMD is to deliver a prosthetically driven reconstruction. FEA was to evaluate the biomechanical response of PSI struts (PSI 1), PSI Screw retained (PSI 2) and QZI to masticatory load on virtual simulation to improve accuracy and enhance the design.
Aim
To validate and compare the Biomechanical benefit of the PSI struts, PSI Screw retained, QZI in a case of rehabilitation of post-COVID maxillary mucormycosis defect (PCMMD) by FEA study.
Methodology
The result of stress to masticatory load on virtual simulation for (1) Maximum and minimum stress (Von Mises stress); (2) the Displacement (in three positions) and (3) the Deformation (Plastic strain) was compared on virtual simulation for PSI 1 and PSI 2 and QZI.
Conclusion
The FEA and comparative evaluation of PSI 1, PSI 2 and QZI showed a good resistance to displacement. The stress and strain values are low and acceptable. In comparison QZI shows more stress in the anterior region.





Similar content being viewed by others
Abbreviations
- PSI:
-
Patient specific implants
- QZI:
-
Quad zygoma implant
- PCMMD:
-
Post-COVID maxillary mucormycosis defect
- FEA:
-
Finite element analysis
References
Ali IE, Chugh A, Cheewin T, Hattori M, Sumita YI (2022) The rising challenge of mucormycosis for maxillofacial prosthodontists in the covid-19 pandemic: a literature review. J Prosthodont Res. https://doi.org/10.2186/jpr.JPR_D_21_00264
Rattan V, Rai S, Jolly SS, Meena VK (2019) Maxillofacial reconstruction with Patient-specific Implants. J Postgrad Med Educ Res 53(1):34–37
Soltanzadeh P, Su JM, Habibabadi SR, Kattadiyil MT (2019) Obturator fabrication incorporating computer-aided design and 3-dimensional printing technology: a clinical report. J Prosthet Dent 121(4):694–697
Vega LG, Gielincki W, Fernandes RP (2013) Zygoma implants reconstruction of acquired maxillary bony defects. Oral Maxillofac Surg Clin North Am 25(2):223–239
Rathee M, Singh S, Malik S, Divakar S, Alam M (2022) Reconstruction and rehabilitation of maxillary defects secondary to mucormycosis. Saudi J Oral Dent Res 7(1):1–7. https://doi.org/10.36348/sjodr.2022.v07i01.001
Zhong S, Shi Q, Van Dessel J, Gu Y, Sun Y, Yang S, Politis C (2022) Biomechanical validation of structural optimized patient-specific mandibular reconstruction plate orienting additive manufacturing. Comput Methods Programs Biomed 1(224):107023
Rotaru H, Schumacher R, Kim SG, Dinu C (2015) Selective laser melted titanium implants: a new technique for the reconstruction of extensive zygomatic complex defects. Maxillofac Plast Recon Surg 37:1–4
Melville JC, Manis CS, Shum JW, Alsuwied D (2019) Single-unit 3D-printed titanium reconstruction plate for maxillary reconstruction: the evolution of surgical reconstruction for maxillary defects—a case report and review of current techniques. J Oral Maxillofac Surg 77(4):874-e1
Glas HH, Vosselman N, de Visscher SA (2020) The use of 3D virtual surgical planning and computer aided design in reconstruction of maxillary surgical defects. Curr Opin Otolaryngol Head Neck Surg 28(2):122–8
Schmidt BL, Pogrel MA, Young CW, Sharma A (2004) Reconstruction of extensive maxillary defects using zygomaticus implants. J Oral Maxillofac Surg 62:82–89
Romeed SA, Malik R, Dunne SM (2014) Zygomatic implants: the impact of zygoma bone support on biomechanics. J Oral Implantol 40(3):231–7
Korkmaz FM, Korkmaz YT, Yaluğ S, Korkmaz T (2012) Impact of dental and zygomatic implants on stress distribution in maxillary defects: a 3-dimensional finite element analysis study. J Oral Implantol 38(5):557–67
Wen H, Guo W, Liang R, **ang L, Long G, Wang T, Deng M, Tian W (2014) Finite element analysis of three zygomatic implant techniques for the severely atrophic edentulous maxilla. J Prosthet Dent 111(3):203–15
Gaur V, Patel K, Palka L (2021) An implant-supported prosthetic rehabilitation of a patient with a bilateral subtotal maxillectomy defect secondary to rhino-orbital-cerebral mucormycosis: a clinical report of a graftless approach. J Prosthet Dent. https://doi.org/10.1016/j.prosdent.2020.12.022
Freytag M, Shapiro V, Tsukanov I (2011) Finite element analysis in situ. Finite Elem Anal Des 47(9):957–972
Biegler M, Marko A, Graf B, Rethmeier M (2018) Finite element analysis of in-situ distortion and bulging for an arbitrarily curved additive manufacturing directed energy deposition geometry. Addit Manuf 24:264–272
Mommaerts MY (2018) Evolutionary steps in the design and biofunctionalization of the additively manufactured sub-periosteal jaw implant ‘AMSJI’ for the maxilla. Int J Oral Maxillofac Surg. https://doi.org/10.1016/j.ijom.2018.08.001
Kaman S et al (2017) Stress analysis of zygomatic implants on the augmented maxillary sinus: is it necessary to graft? Implant Dent 26:1–8
Demenko V, Linetskiy I, Linetska L, Yefremov O (2019) Load-carrying capacity of short implants in edentulous posterior maxilla: a finite element study. Med Eng Phys 71:30–37
Liu X et al (2019) Effects of different positions and angles of implants in maxillary edentulous jaw on surrounding bone stress under dynamic loading: a three-dimensional finite element analysis. Comput Math Methods Med 23:56. https://doi.org/10.1155/2019/8074096
Saini H, Ackland DC, Gong L, Cheng LK, Röhrle O (2020) Occlusal load modelling significantly impacts the predicted tooth stress response during biting: a simulation study. Comput Methods Biomech Biomed Eng 23(7):261–270
Miyamoto S, Ujigawa K, Kizu Y, Tonogi M, Yamane GY (2010) Biomechanical threedimensional finite-element analysis of maxillary prostheses with implants. Design of number and position of implants for maxillary prostheses after hemimaxillectomy. Int J Oral Maxillofac Surg 39:1120–1126
Carnicero A, Peláez A, Restoy-Lozano A, Jacquott I, Perera R (2021) Improvement of an additively manufactured subperiosteal implant structure design by finite elements based topological optimization. Sci Rep 11(1):1–9
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Manekar, V.S., Datarkar, A.N., Ghormode, A. et al. Comparison of Two Types of Patient Specific Implants (PSI) and Quad Zygoma Implant (QZI) for Rehabilitation of Post-COVID Maxillary Mucormycosis Defect (PCMMD): Finite Element Analysis. J. Maxillofac. Oral Surg. 22, 688–694 (2023). https://doi.org/10.1007/s12663-023-01950-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12663-023-01950-3