Abstract
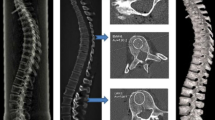
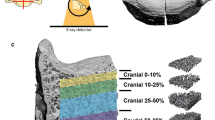
Trabecular structures in vertebral bodies are unequally distributed in the cervical, thoracic and lumbar spine, and also within individual vertebrae. Knowledge of the microstructure of these entities could influence our comprehension and treatment of osteoporotic fractures, and even surgical procedures. Appropriate investigations may clarify the pathomechanisms of various osteoporotic fractures (fish, wedge-shaped, and flat vertebrae). We obtained three cancellous bone cylinders from the centers and margins of cervical vertebra 3 to lumbar vertebra 5, and investigated these in regard of bone volume fraction, trabecular thickness, separation, trabecular number, trabecular bone pattern factor, connectivity density, and degree of anisotropy. Using a Jamshidi needle®, we obtained samples from three quadrants (QI: right-sided edge, QII: central, QIII: left-sided edge) of 242 prepared vertebrae, and investigated these on a micro-CT device. In all, 726 bone samples were taken from eleven body donors. Bone volume fraction, trabecular thickness, and the degree of anisotropy were significantly lower in QII than in QI and QIII. Trabecular pattern factor, however, was significantly higher in QII than in QI and QIII. The results helped to explain fish vertebrae. Wedge fractures and flat vertebrae are most likely caused by the complex destruction of trabecular and cortical structures. The higher bone volume fraction in the cervical spine compared to the thoracic and lumbar spine accounts for the small number of fractures in the cervical spine. The marked trabecular pattern factor in the center of thoracic and lumbar vertebrae could be a reason for the surgeon to use different screw designs for individual vertebrae.






Similar content being viewed by others
Data availability
The datasets used and/or analyzed in the current study are available from the corresponding author on reasonable request.
Abbreviations
- Al:
-
Aluminum
- BMD:
-
Bone mineral density
- BMI:
-
Body mass index
- BVF:
-
Bone volume fraction
- cm:
-
Centimeter
- Conn.D:
-
Connectivity density
- CS:
-
Cervical spine
- CT:
-
Computed tomography
- CV:
-
Cervical vertebra
- DA:
-
Degree of anisotropy
- Fig.:
-
Figure
- Fs:
-
Fractures
- g/cm3 :
-
Gram/cubic centimeter
- HU:
-
Hounsfield units
- kV:
-
Kilovolt
- LV:
-
Lumbar vertebrae
- LS:
-
Lumbar spine
- M:
-
Mean value
- mg/cm3 :
-
Milligram/cubic centimeter
- Micro-CT:
-
Micro-computed tomography
- Mio.:
-
Million
- ml:
-
Milliliter
- mm:
-
Millimeter
- OP:
-
Osteoporosis
- Q I:
-
Quadrant I
- Q II:
-
Quadrant II
- Q III:
-
Quadrant III
- QCT:
-
Quantitative computed tomography
- ROI:
-
Region of interest
- SD:
-
Standard deviation
- Tb.N:
-
Trabecular number
- Tb.Pf:
-
Trabecular pattern factor
- Tb.Sp:
-
Trabecular separation
- Tb.Th:
-
Trabecular thickness
- TS:
-
Thoracic spine
- TV:
-
Thoracic vertebra
- VFs:
-
Vertebral fractures
- µm:
-
Micrometer
- µA:
-
Microampere
References
Andresen R, Radmer S, Banzer D, Felsenberg D, Wolf KJ (1994) Quantitative Knochenmineralgehaltsbestimmung (QCT)–Systemvergleich baugleicher Computertomographen (The quantitative determination of bone mineral content–a system comparison of similarly built computed tomographs). Rofo 160:260–265. https://doi.org/10.1055/s-2008-1032417
Andresen R, Radmer S, Banzer D (1998) Bone mineral density and spongiosa architecture in correlation to vertebral body insufficiency fractures. Acta Radiol 39:538–542. https://doi.org/10.1080/02841859809172221
Banse X, Devogelaer J, Munting E, Delloye C, Cornu O, Grynpas M (2001) Inhomogeneity of human vertebral cancellous bone: systematic density and structure patterns inside the vertebral body. Bone 28:563–571. https://doi.org/10.1016/S8756-3282(01)00425-2
Banzer D, Fabian C, Andresen R, Banzer JP, Felsenberg D, Reisinger W, Neher KM (1998) Knochendichte von Spongiosa und Kortikalis der Lendenwirbelsäule. Beziehungen zu Geschlecht, Alter und Wirbeldeformitäten in einem regionalen Kollektiv der europäischen Studie zur vertebralen Osteoporose (EVOS) (Bone density of spongiosa and cortical bone of the lumbar spine. Relations to sex, age and spinal deformities in a regional collective of the European Study of Vertebral Osteoporosis (EVOS)). Med Klin (Munich) 93(Suppl 2):56–65
Bässgen K, Westphal T, Haar P, Kundt G, Mittlmeier T, Schober H-C (2013) Population-based prospective study on the incidence of osteoporosis-associated fractures in a German population of 200,413 inhabitants. J Public Health (oxf) 35:255–261. https://doi.org/10.1093/pubmed/fds076
Blattert TR, Schnake KJ, Gonschorek O, Katscher S, Ullrich BW, Gercek E, Hartmann F, Mörk S, Morrison R, Müller ML, Partenheimer A, Piltz S, Scherer MA, Verheyden A, Zimmermann V (2019) Nichtoperative und operative Behandlung der osteoporotischen Wirbelkörperfraktur: Empfehlungen der Sektion Wirbelsäule der Deutschen Gesellschaft für Orthopädie und Unfallchirurgie (DGOU) (Nonsurgical and surgical management of osteoporotic vertebral body fractures: recommendations of the Spine Section of the German Society for Orthopaedics and Trauma (DGOU)). Orthopade 48:84–91. https://doi.org/10.1007/s00132-018-03666-6
Chen H, Kubo K-Y (2014) Bone three-dimensional microstructural features of the common osteoporotic fracture sites. World J Orthop 5:486–495. https://doi.org/10.5312/wjo.v5.i4.486
Chen H, Shoumura S, Emura S, Bunai Y (2008) Regional variations of vertebral trabecular bone microstructure with age and gender. Osteoporos Int 19:1473–1483. https://doi.org/10.1007/s00198-008-0593-3
Christiansen BA, Bouxsein ML (2010) Biomechanics of vertebral fractures and the vertebral fracture cascade. Curr Osteoporos Rep 8:198–204. https://doi.org/10.1007/s11914-010-0031-2
Crilly RG, Cox L (2013) A comparison of bone density and bone morphology between patients presenting with hip fractures, spinal fractures or a combination of the two. BMC Musculoskelet Disord 14:68. https://doi.org/10.1186/1471-2474-14-68
Ea H-K, Weber A-J, Yon F, Lioté F (2004) Osteoporotic fracture of the dens revealed by cervical manipulation. Joint Bone Spine 71:246–250. https://doi.org/10.1016/S1297-319X(03)00113-1
Engelke K, Adams JE, Armbrecht G, Augat P, Bogado CE, Bouxsein ML, Felsenberg D, Ito M, Prevrhal S, Hans DB, Lewiecki EM (2008) Clinical use of quantitative computed tomography and peripheral quantitative computed tomography in the management of osteoporosis in adults: the 2007 ISCD Official Positions. J Clin Densitom 11:123–162. https://doi.org/10.1016/j.jocd.2007.12.010
Feng H, Ma Y, Wang SJ, Zhang S, Li Z (2021) The correlation of regional microstructure and mechanics of the cervical articular process in adults. Materials (Basel). https://doi.org/10.3390/ma14216409
Follet H, Farlay D, Bala Y, Viguet-Carrin S, Gineyts E, Burt-Pichat B, Wegrzyn J, Delmas P, Boivin G, Chapurlat R (2013) Determinants of microdamage in elderly human vertebral trabecular bone. PLoS One 8:e55232. https://doi.org/10.1371/journal.pone.0055232
Genant HK, Wu CY, van Kuijk C, Nevitt MC (1993) Vertebral fracture assessment using a semiquantitative technique. J Bone Miner Res 8:1137–1148. https://doi.org/10.1002/jbmr.5650080915
Gong H, Zhang M, Yeung HY, Qin L (2005) Regional variations in microstructural properties of vertebral trabeculae with aging. J Bone Miner Metab 23:174–180. https://doi.org/10.1007/s00774-004-0557-4
Grote HJ, Amling M, Vogel M, Hahn M, Pösl M, Delling G (1995) Intervertebral variation in trabecular microarchitecture throughout the normal spine in relation to age. Bone 16:301–308. https://doi.org/10.1016/8756-3282(94)00042-5
Harvey NC, Glüer CC, Binkley N, McCloskey EV, Brandi M-L, Cooper C, Kendler D, Lamy O, Laslop A, Camargos BM, Reginster J-Y, Rizzoli R, Kanis JA (2015) Trabecular bone score (TBS) as a new complementary approach for osteoporosis evaluation in clinical practice. Bone 78:216–224. https://doi.org/10.1016/j.bone.2015.05.016
** Y, Zhang T, Cheung JPY, Wong TM, Feng X, Sun T, Zu H, Sze KY, Lu WW (2020) A novel mechanical parameter to quantify the microarchitecture effect on apparent modulus of trabecular bone: A computational analysis of ineffective bone mass. Bone 135:115314
Johnell O, Kanis JA (2006) An estimate of the worldwide prevalence and disability associated with osteoporotic fractures. Osteoporos Int 17:1726–1733. https://doi.org/10.1007/s00198-006-0172-4
Kanis JA, Norton N, Harvey NC, Jacobson T, Johansson H, Lorentzon M, McCloskey EV, Willers C, Borgström F (2021) SCOPE 2021: a new scorecard for osteoporosis in Europe. Arch Osteoporos 16:82. https://doi.org/10.1007/s11657-020-00871-9
Kendler DL, Bauer DC, Davison KS, Dian L, Hanley DA, Harris ST, McClung MR, Miller PD, Schousboe JT, Yuen CK, Lewiecki EM (2016) Vertebral fractures: clinical importance and management. Am J Med 129:221.e1–10. https://doi.org/10.1016/j.amjmed.2015.09.020
Kinney JH, Ladd AJ (1998) The relationship between three-dimensional connectivity and the elastic properties of trabecular bone. J Bone Miner Res 13:839–845. https://doi.org/10.1359/jbmr.1998.13.5.839
Maquer G, Musy SN, Wandel J, Gross T, Zysset PK (2015) Bone volume fraction and fabric anisotropy are better determinants of trabecular bone stiffness than other morphological variables. J Bone Miner Res 30:1000–1008. https://doi.org/10.1002/jbmr.2437
McDonnell P, McHugh PE, O’Mahoney D (2007) Vertebral osteoporosis and trabecular bone quality. Ann Biomed Eng 35:170–189. https://doi.org/10.1007/s10439-006-9239-9
Möller G, Andresen R, Banzer D (2011) Shape model-based semi-automatic morphometric assessment of vertebral deformities in clinical practice. Osteologie 20:239–247. https://doi.org/10.1055/s-0037-1620000
Mosekilde L (1988) Age-related changes in vertebral trabecular bone architecture—assessed by a new method. Bone 9:247–250. https://doi.org/10.1016/8756-3282(88)90038-5
Ostrowski C, Ronan L, Sheridan R, Pearce V (2013) An osteoporotic fracture mimicking cervical dystonia in idiopathic Parkinson’s disease. Age Ageing 42:658–659. https://doi.org/10.1093/ageing/aft050
Popp AW, Buffat H, Eberli U, Lippuner K, Ernst M, Richards RG, Stadelmann VA, Windolf M (2014) Microstructural parameters of bone evaluated using HR-pQCT correlate with the DXA-derived cortical index and the trabecular bone score in a cohort of randomly selected premenopausal women. PLoS One 9:e88946. https://doi.org/10.1371/journal.pone.0088946
Resnick D, Niwayama G (1976) Radiographic and pathologic features of spinal involvement in diffuse idiopathic skeletal hyperostosis (DISH). Radiology 119:559–568. https://doi.org/10.1148/119.3.559
Schreiber JJ, Anderson PA, Rosas HG, Buchholz AL, Au AG (2011) Hounsfield units for assessing bone mineral density and strength: a tool for osteoporosis management. J Bone Joint Surg Am 93:1057–1063. https://doi.org/10.2106/JBJS.J.00160
Schröder G, Wendig D, Jabke B, Schulze M, Wree A, Kundt G, Manhart J, Martin H, Sahmel O, Andresen R, Schober H-C (2019) Vergleich der Spongiosamorphologie aus humaner Halswirbelsäule (HWS), Brustwirbelsäule (BWS) und Lendenwirbelsäule (LWS) einer 102-jährigen Körperspenderin. Osteologie 28:283–288. https://doi.org/10.1055/a-0997-8059
Schröder G, Jabke B, Schulze M, Wree A, Martin H, Sahmel O, Doerell A, Kullen CM, Andresen R, Schober H-C (2021a) A comparison, using X-ray micro-computed tomography, of the architecture of cancellous bone from the cervical, thoracic and lumbar spine using 240 vertebral bodies from 10 body donors. Anat Cell Biol 54:25–34. https://doi.org/10.5115/acb.20.269
Schröder G, Hiepe L, Moritz M, Vivell L-M, Schulze M, Martin H, Götz A, Andresen JR, Kullen C-M, Andresen R, Schober H-C (2021) Warum sich in der Halswirbelsäule auch bei Osteoporose nur selten Insuffizienzfrakturen finden (why insufficiency fractures are rarely found in the cervical spine, even with osteoporosis). Z Orthop Unfall. https://doi.org/10.1055/a-1647-3914
Schröder G, Reichel M, Spiegel S, Schulze M, Götz A, Bugaichuk S, Andresen JR, Kullen CM, Andresen R, Schober H-C (2022a) Breaking strength and bone microarchitecture in osteoporosis: a biomechanical approximation based on load tests in 104 human vertebrae from the cervical, thoracic, and lumbar spines of 13 body donors. J Orthop Surg Res 17:228. https://doi.org/10.1186/s13018-022-03105-5
Schröder G, Flachsmeyer D, Kullen CM, Andresen JR, Schulze M, Hiepe L, Schober H-C, Andresen R (2022b) Insuffizienzfrakturen der Wirbelsäule in Abhängigkeit von der spongiösen Knochendichte: Eine in-vitro-Studie (Insufficiency fractures of the spine in relation to cancellous bone density: an in vitro study). Orthopadie (Heidelb) 51:547–555. https://doi.org/10.1007/s00132-022-04261-6
Waterloo S, Ahmed LA, Center JR, Eisman JA, Morseth B, Nguyen ND, Nguyen T, Sogaard AJ, Emaus N (2012) Prevalence of vertebral fractures in women and men in the population-based Tromsø Study. BMC Musculoskelet Disord 13:3. https://doi.org/10.1186/1471-2474-13-3
Willers C, Norton N, Harvey NC, Jacobson T, Johansson H, Lorentzon M, McCloskey EV, Borgström F, Kanis JA (2022) Osteoporosis in Europe: a compendium of country-specific reports. Arch Osteoporos. https://doi.org/10.1007/s11657-021-00969-8
Zanker J, Duque G (2019) Osteoporosis in older persons: old and new players. J Am Geriatr Soc 67:831–840. https://doi.org/10.1111/jgs.15716
Acknowledgements
The authors sincerely thank those who donated their bodies to science and their gesture in promoting anatomical research. Results from such research could potentially enhance our overall knowledge and thus improve patient care. We express our utmost gratitude to these donors and their families.
Funding
Not applicable.
Author information
Authors and Affiliations
Contributions
GS and HCS contributed to conceptualization. MS, LH, AMB and MM were involved in data acquisition. GS, RA, SB, AMB, HM and JRA contributed to data analysis or interpretation. GS, RA, and HCS were involved in drafting the manuscript. GS, RA, and HCS contributed to critical revisions of the manuscript. All authors approved the final version.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The study was performed in accordance with the principles of the Declaration of Helsinki—Ethical Principles for Medical Research Involving Human Subjects—and was approved by the local ethics committees of the participating universities.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Schröder, G., Baginski, A.M., Schulze, M. et al. Regional variations in the intra- and intervertebral trabecular microarchitecture of the osteoporotic axial skeleton. Anat Sci Int 98, 566–579 (2023). https://doi.org/10.1007/s12565-023-00726-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12565-023-00726-6