Abstract
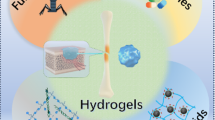
Bone tissue engineering has become a popular area of study for making biomimetic hydrogels to treat bone diseases. In this work, we looked at biocompatible hydrogels that can be injected into bone defects that require the smallest possible surgery. Mineral ions can be attached to polymer chains to make useful hydrogels that help bones heal faster. These ions are very important for the balance of the body. In the chemically-triggered sector, advanced hydrogels cross-linked by different molecular agents have many advantages, such as being selective, able to form gels, and having mechanical properties that can be modified. In addition, different photo-initiators can be used to make photo cross linkable hydrogels react quickly and moderately under certain light bands. Enzyme-triggered hydrogels are another type of hydrogel that can be used to repair bone tissue because they are biocompatible and gel quickly. We also look at some of the important factors mentioned above that could change how well bone tissue engineering works as a therapy. Finally, this review summarizes the problems that still need to be solved to make clinically relevant hydrogels.




Similar content being viewed by others
Abbreviations
- IL-1:
-
Interleukin-1
- TNF-α:
-
Tumor necrosis factor alpha
- TGF-β:
-
Transforming growth factor beta
- MSCs:
-
Mesenchymal stem cell
- MMPs:
-
Matrix metalloproteinases
- ECM:
-
Extracellular matrix
- BMSC:
-
Bone marrow-derived stem cell
- PLGA:
-
Poly(lactic-co-glycolic) acid
- PEG:
-
Polyethylene glycol
- PNIPAAm:
-
Poly(N-isopropylacrylamide)
- HA:
-
Hyaluronic acid
- RA:
-
Rheumatoid arthritis
- TA:
-
Tannic acid
- ROS:
-
Reactive oxygen species
- ALP:
-
Alkaline phosphatase
- BPNs:
-
Black phosphorus nanosheets
- PLA:
-
Poly caprolactone
- DDS:
-
Drug delivery system
References
Adil MM, Vazin T, Ananthanarayanan B, Rodrigues GM, Rao AT, Kulkarni RU et al (2017) Engineered hydrogels increase the post-transplantation survival of encapsulated hESC-derived midbrain dopaminergic neurons. Biomaterials 136:1–11. https://doi.org/10.1016/j.biomaterials.2017.05.008
Akhtar MF, Hanif M, Ranjha NM (2016) Methods of synthesis of hydrogels… a review. Saudi Pharm J 24(5):554–559. https://doi.org/10.1016/j.jsps.2015.03.022
Anjum F, Lienemann PS, Metzger S, Biernaskie J, Kallos MS, Ehrbar M (2016) Enzyme responsive GAG-based natural-synthetic hybrid hydrogel for tunable growth factor delivery and stem cell differentiation. Biomaterials 87:104–117. https://doi.org/10.1016/j.biomaterials.2016.01.050
Bai S, Zhang X, Lv X, Zhang M, Huang X, Shi Y et al (2020) Bioinspired mineral–organic bone adhesives for stable fracture fixation and accelerated bone regeneration. Adv Funct Mater 30(5):1908381. https://doi.org/10.1002/adfm.201908381
Balakrishnan B, Banerjee R (2011) Biopolymer-based hydrogels for cartilage tissue engineering. Chem Rev 111(8):4453–4474. https://doi.org/10.1021/cr100123h
Banimohamad-Shotorbani B, Karkan SF, Rahbarghazi R, Mehdipour A, Jarolmasjed S, Saghati S et al (2023) Application of mesenchymal stem cell sheet for regeneration of craniomaxillofacial bone defects. Stem Cell Res Ther 14(1):1–21. https://doi.org/10.1186/s13287-023-03309-4
Chan WP, Kung F-C, Kuo Y-L, Yang M-C, Lai W-FT. Alginate/poly (γ-glutamic acid) base biocompatible gel for bone tissue engineering. BioMed research international. 2015;2015. https://doi.org/10.1155/2015/185841
Chao Y, Ge Y, Chen Z, Cui X, Zhao C, Wang C et al (2021) One-pot hydrothermal synthesis of solution-processable MoS2/PEDOT: PSS composites for high-performance supercapacitors. ACS Appl Mater Interfaces 13(6):7285–7296. https://doi.org/10.1021/acsami.0c21439
Chaudhuri O, Gu L, Klumpers D, Darnell M, Bencherif SA, Weaver JC et al (2016) Hydrogels with tunable stress relaxation regulate stem cell fate and activity. Nat Mater 15(3):326–334. https://doi.org/10.1038/nmat4489
Chen L, Li M, Yang Z, Tao W, Wang P, Tian X et al (2020a) Gardenia jasminoides Ellis: ethnopharmacology, phytochemistry, and pharmacological and industrial applications of an important traditional Chinese medicine. J Ethnopharmacol 257:112829. https://doi.org/10.1016/j.jep.2020.112829
Chen M, Feng Z, Guo W, Yang D, Gao S, Li Y et al (2019) PCL-MECM-based hydrogel hybrid scaffolds and meniscal fibrochondrocytes promote whole meniscus regeneration in a rabbit meniscectomy model. ACS Appl Mater Interfaces 11(44):41626–41639. https://doi.org/10.1021/acsami.9b13611
Chen R, Chen H-B, Xue P-P, Yang W-G, Luo L-Z, Tong M-Q et al (2021) HA/MgO nanocrystal-based hybrid hydrogel with high mechanical strength and osteoinductive potential for bone reconstruction in diabetic rats. J Mater Chem B 9(4):1107–1122. https://doi.org/10.1039/D0TB02553D
Chen W, Xu Y, Li Y, Jia L, Mo X, Jiang G et al (2020b) 3D printing electrospinning fiber-reinforced decellularized extracellular matrix for cartilage regeneration. Chem Eng J 382:122986. https://doi.org/10.1016/j.cej.2019.122986
Cui Z-K, Kim S, Baljon JJ, Wu BM, Aghaloo T, Lee M (2019) Microporous methacrylated glycol chitosan-montmorillonite nanocomposite hydrogel for bone tissue engineering. Nat Commun 10(1):3523. https://doi.org/10.1038/s41467-019-11511-3
Dalby MJ, Gadegaard N, Tare R, Andar A, Riehle MO, Herzyk P et al (2007) The control of human mesenchymal cell differentiation using nanoscale symmetry and disorder. Nat Mater 6(12):997–1003. https://doi.org/10.1038/nmat2013
Das Mahapatra R, Imani KBC, Yoon J (2020) Integration of macro-cross-linker and metal coordination: a super stretchable hydrogel with high toughness. ACS Appl Mater Interfaces 12(36):40786–40793. https://doi.org/10.1021/acsami.0c11167
Dubin-Thaler BJ, Giannone G, Döbereiner H-G, Sheetz MP (2004) Nanometer analysis of cell spreading on matrix-coated surfaces reveals two distinct cell states and STEPs. Biophys J 86(3):1794–1806. https://doi.org/10.1016/S0006-3495(04)74246-0
Ekerdt BL, Fuentes CM, Lei Y, Adil MM, Ramasubramanian A, Segalman RA et al (2018) Thermoreversible hyaluronic Acid-PNIPAAm hydrogel systems for 3D stem cell culture. Adv Healthc Mater 7(12):1800225. https://doi.org/10.1002/adhm.201800225
Elkhoury K, Russell CS, Sanchez-Gonzalez L, Mostafavi A, Williams TJ, Kahn C et al (2019) Soft-nanoparticle functionalization of natural hydrogels for tissue engineering applications. Adv Healthc Mater 8(18):1900506. https://doi.org/10.1002/adhm.201900506
Fu S, Ni P, Wang B, Chu B, Zheng L, Luo F et al (2012) Injectable and thermo-sensitive PEG-PCL-PEG copolymer/collagen/n-HA hydrogel composite for guided bone regeneration. Biomaterials 33(19):4801–4809. https://doi.org/10.1016/j.biomaterials.2012.03.040
Gabarin N, Gavish H, Muhlrad A, Chen YC, Namdar-Attar M, Nissenson RA et al (2001) Mitogenic Gi protein-MAP kinase signaling cascade in MC3T3-E1 osteogenic cells: activation by C-terminal pentapeptide of osteogenic growth peptide [OGP (10–14)] and attenuation of activation by cAMP. J Cell Biochem 81(4):594–603. https://doi.org/10.1002/jcb.1083
Gauvin R, Chen Y-C, Lee JW, Soman P, Zorlutuna P, Nichol JW et al (2012) Microfabrication of complex porous tissue engineering scaffolds using 3D projection stereolithography. Biomaterials 33(15):3824–3834. https://doi.org/10.1016/j.biomaterials.2012.01.048
Ghorbani F, Ghalandari B, Khajehmohammadi M, Bakhtiary N, Tolabi H, Sahranavard M et al (2023) Photo-cross-linkable hyaluronic acid bioinks for bone and cartilage tissue engineering applications. Int Mater Rev 1-42. https://doi.org/10.1080/09506608.2023.2167559
He Y, Liang L, Luo C, Zhang Z-Y, Huang J (2023) Strategies for in situ tissue engineering of vascularized bone regeneration. Biomed Rep 18(6):1–13. https://doi.org/10.3892/br.2023.1625
Henkel J, Woodruff MA, Epari DR, Steck R, Glatt V, Dickinson IC et al (2013) Bone regeneration based on tissue engineering conceptions—a 21st century perspective. Bone Res 1(1):216–248. https://doi.org/10.4248/BR201303002
Hu W, Wang Z, **ao Y, Zhang S, Wang J (2019) Advances in crosslinking strategies of biomedical hydrogels. Biomater Sci 7(3):843–855. https://doi.org/10.1039/C8BM01246F
Hu X, Cheng W, Shao Z, **n L (2015) Synthesis and characterization of temperature-sensitive hydrogels. e-Polymers 15(5):353–360. https://doi.org/10.1515/epoly-2015-0157
Huang K, Wu J, Gu Z (2018) Black phosphorus hydrogel scaffolds enhance bone regeneration via a sustained supply of calcium-free phosphorus. ACS Appl Mater Interfaces 11(3):2908–2916. https://doi.org/10.1021/acsami.8b21179
Khajouei S, Ravan H, Ebrahimi A (2020) Develo** a colorimetric nucleic acid-responsive DNA hydrogel using DNA proximity circuit and catalytic hairpin assembly. Anal Chim Acta 1137:1–10. https://doi.org/10.1016/j.aca.2020.08.059
Kirillova A, Yeazel TR, Asheghali D, Petersen SR, Dort S, Gall K et al (2021) Fabrication of biomedical scaffolds using biodegradable polymers. Chem Rev 121(18):11238–11304. https://doi.org/10.1021/acs.chemrev.0c01200
Lee CS, Hwang HS, Kim S, Fan J, Aghaloo T, Lee M (2020a) Inspired by nature: facile design of nanoclay–organic hydrogel bone sealant with multifunctional properties for robust bone regeneration. Adv Funct Mater 30(43):2003717. https://doi.org/10.1002/adfm.202003717
Lee M, Rizzo R, Surman F, Zenobi-Wong M (2020b) Guiding lights: tissue bioprinting using photoactivated materials. Chem Rev 120(19):10950–11027. https://doi.org/10.1021/acs.chemrev.0c00077
Li J, Wang B, Lin J, Cheng D, Lu Y (2018) Multifunctional surface modification of mulberry silk fabric via PNIPAAm/chitosan/PEO nanofibers coating and cross-linking technology. Coatings 8(2):68. https://doi.org/10.3390/coatings8020068
Li Q, Barrett DG, Messersmith PB, Holten-Andersen N (2016) Controlling hydrogel mechanics via bio-inspired polymer–nanoparticle bond dynamics. ACS Nano 10(1):1317–1324. https://doi.org/10.1021/acsnano.5b06692
Li X, Chen L, Lin H, Cao L, Ja C, Dong J et al (2017a) Efficacy of poly (D, L-lactic acid-co-glycolic acid)-poly (ethylene glycol)-poly (D, L-lactic acid-co-glycolic acid) thermogel as a barrier to prevent spinal epidural fibrosis in a postlaminectomy rat model. Clinical Spine. Surgery 30(3):E283–EE90. https://doi.org/10.1097/BSD.0000000000000221
Li Y, **ao Y, Liu C (2017b) The horizon of materiobiology: a perspective on material-guided cell behaviors and tissue engineering. Chem Rev 117(5):4376–4421. https://doi.org/10.1021/acs.chemrev.6b00654
Lin Z, Wu J, Qiao W, Zhao Y, Wong KH, Chu PK et al (2018) Precisely controlled delivery of magnesium ions thru sponge-like monodisperse PLGA/nano-MgO-alginate core-shell microsphere device to enable in-situ bone regeneration. Biomaterials 174:1–16. https://doi.org/10.1016/j.biomaterials.2018.05.011
Liu M, Zeng X, Ma C, Yi H, Ali Z, Mou X et al (2017) Injectable hydrogels for cartilage and bone tissue engineering. Bone Res 5(1):1–20. https://doi.org/10.1038/boneres.2017.14
Lu Y, Li L, Zhu Y, Wang X, Li M, Lin Z et al (2018) Multifunctional copper-containing carboxymethyl chitosan/alginate scaffolds for eradicating clinical bacterial infection and promoting bone formation. ACS Appl Mater Interfaces 10(1):127–138. https://doi.org/10.1021/acsami.7b13750
Lu Z, Liu S, Le Y, Qin Z, He M, Xu F et al (2019) An injectable collagen-genipin-carbon dot hydrogel combined with photodynamic therapy to enhance chondrogenesis. Biomaterials 218:119190. https://doi.org/10.1016/j.biomaterials.2019.05.001
Matai I, Kaur G, Seyedsalehi A, McClinton A, Laurencin CT (2020) Progress in 3D bioprinting technology for tissue/organ regenerative engineering. Biomaterials 226:119536. https://doi.org/10.1016/j.biomaterials.2019.119536
Morais D, Rodrigues M, Silva T, Lopes M, Santos M, Santos J et al (2013) Development and characterization of novel alginate-based hydrogels as vehicles for bone substitutes. Carbohydr Polym 95(1):134–142. https://doi.org/10.1016/j.carbpol.2013.02.067
Nabavi MH, Salehi M, Ehterami A, Bastami F, Semyari H, Tehranchi M et al (2020) A collagen-based hydrogel containing tacrolimus for bone tissue engineering. Drug Deliv Transl Res 10:108–121. https://doi.org/10.1007/s13346-019-00666-7
Neves MI, Araújo M, Moroni L, da Silva RM, Barrias CC (2020) Glycosaminoglycan-inspired biomaterials for the development of bioactive hydrogel networks. Molecules 25(4):978. https://doi.org/10.3390/molecules25040978
Ni P, Ding Q, Fan M, Liao J, Qian Z, Luo J et al (2014) Injectable thermosensitive PEG–PCL–PEG hydrogel/acellular bone matrix composite for bone regeneration in cranial defects. Biomaterials 35(1):236–248. https://doi.org/10.1016/j.biomaterials.2013.10.016
Nonoyama T, Lee YW, Ota K, Fujioka K, Hong W, Gong JP (2020) Instant thermal switching from soft hydrogel to rigid plastics inspired by thermophile proteins. Adv Mater 32(4):1905878. https://doi.org/10.1002/adma.201905878
Obata A, Ogasawara T, Kasuga T (2019) Combinatorial effects of inorganic ions on adhesion and proliferation of osteoblast-like cells. J Biomed Mater Res Part A 107(5):1042–1051. https://doi.org/10.1002/jbm.a.36623
Oryan A, Kamali A, Moshiri A, Baharvand H, Daemi H (2018) Chemical crosslinking of biopolymeric scaffolds: current knowledge and future directions of crosslinked engineered bone scaffolds. Int J Biol Macromol 107:678–688. https://doi.org/10.1016/j.ijbiomac.2017.08.184
Pan H, Gao H, Li Q, Lin Z, Feng Q, Yu C et al (2020) Engineered macroporous hydrogel scaffolds via pickering emulsions stabilized by MgO nanoparticles promote bone regeneration. J Mater Chem B 8(28):6100–6114. https://doi.org/10.1039/D0TB00901F
Piluso S, Gomez DF, Dokter I, Texeira LM, Li Y, Leijten J et al (2020) Rapid and cytocompatible cell-laden silk hydrogel formation via riboflavin-mediated crosslinking. J Mater Chem B 8(41):9566–9575. https://doi.org/10.1039/D0TB01731K
Pontremoli C, Boffito M, Fiorilli S, Laurano R, Torchio A, Bari A et al (2018) Hybrid injectable platforms for the in situ delivery of therapeutic ions from mesoporous glasses. Chem Eng J 340:103–113. https://doi.org/10.1016/j.cej.2018.01.073
Qiao Y, Liu X, Zhou X, Zhang H, Zhang W, **ao W et al (2020) Gelatin templated polypeptide co-cross-linked hydrogel for bone regeneration. Adv Healthc Mater 9(1):1901239. https://doi.org/10.1002/adhm.201901239
Rahman MM, Karim MR, Alharbi HF, Aldokhayel B, Uzzaman T, Zahir H (2021) Cadmium selenide quantum dots for solar cell applications: a review. Chem Asian J 16(8):902–921. https://doi.org/10.1002/asia.202001369
Rauner N, Meuris M, Zoric M, Tiller JC (2017) Enzymatic mineralization generates ultrastiff and tough hydrogels with tunable mechanics. Nature 543(7645):407–410. https://doi.org/10.1038/nature21392
Rezaei H, Shahrezaee M, Jalali Monfared M, Fathi Karkan S, Ghafelehbashi R (2021) Simvastatin-loaded graphene oxide embedded in polycaprolactone-polyurethane nanofibers for bone tissue engineering applications. J Polym Eng 41(5):375–386. https://doi.org/10.1515/polyeng-2020-0301
Ryu JH, Messersmith PB, Lee H (2018) Polydopamine surface chemistry: a decade of discovery. ACS Appl Mater Interfaces 10(9):7523–7540. https://doi.org/10.1021/acsami.7b19865
Salhotra A, Shah HN, Levi B, Longaker MT (2020) Mechanisms of bone development and repair. Nat Rev Mol Cell Biol 21(11):696–711. https://doi.org/10.1038/s41580-020-00279-w
Schröter L, Kaiser F, Stein S, Gbureck U, Ignatius A (2020) Biological and mechanical performance and degradation characteristics of calcium phosphate cements in large animals and humans. Acta Biomater 117:1–20. https://doi.org/10.1016/j.actbio.2020.09.031
Shang F, Yu Y, Liu S, Ming L, Zhang Y, Zhou Z et al (2021) Advancing application of mesenchymal stem cell-based bone tissue regeneration. Bioact Mater 6(3):666–683. https://doi.org/10.1016/j.bioactmat.2020.08.014
Singh BN, Veeresh V, Mallick SP, Sinha S, Rastogi A, Srivastava P (2020) Generation of scaffold incorporated with nanobioglass encapsulated in chitosan/chondroitin sulfate complex for bone tissue engineering. Int J Biol Macromol 153:1–16. https://doi.org/10.1016/j.ijbiomac.2020.02.173
Stolzing A, Jones E, Mcgonagle D, Scutt A (2008) Age-related changes in human bone marrow-derived mesenchymal stem cells: consequences for cell therapies. Mech Ageing Dev 129(3):163–173. https://doi.org/10.1016/j.mad.2007.12.002
Sun Z, Song C, Wang C, Hu Y, Wu J (2019) Hydrogel-based controlled drug delivery for cancer treatment: a review. Mol Pharm 17(2):373–391. https://doi.org/10.1021/acs.molpharmaceut.9b01020
Sung H-W, Huang R-N, Huang LL, Tsai C-C (1999) In vitro evaluation of cytotoxicity of a naturally occurring cross-linking reagent for biological tissue fixation. J Biomater Sci Polym Ed 10(1):63–78. https://doi.org/10.1163/156856299X00289
Tang G, Liu Z, Liu Y, Yu J, Wang X, Tan Z et al (2021) Recent trends in the development of bone regenerative biomaterials. Front Cell Dev Biol 9:665813. https://doi.org/10.3389/fcell.2021.665813
Tomaszewska E, Dobrowolski P, Kwiecień M, Winiarska-Mieczan A, Tomczyk A, Muszyński S (2017) The influence of the dietary cu-glycine complex on the histomorphology of cancellous bone, articular cartilage, and growth plate as well as bone mechanical and geometric parameters is dose dependent. Biol Trace Elem Res 178:54–63. https://doi.org/10.1007/s12011-016-0894-x
Unagolla JM, Jayasuriya AC (2020) Hydrogel-based 3D bioprinting: a comprehensive review on cell-laden hydrogels, bioink formulations, and future perspectives. Appl Mater Today 18:100479. https://doi.org/10.1016/j.apmt.2019.100479
Utari TR, Ana ID, Pudyani PS, Asmara W (2021) The intrasulcular application effect of bisphosphonate hydrogel toward osteoclast activity and relapse movement. Saudi Dent J 33(5):292–298. https://doi.org/10.1016/j.sdentj.2020.03.003
Wang C, Huang W, Zhou Y, He L, He Z, Chen Z et al (2020c) 3D printing of bone tissue engineering scaffolds. Bioact Mater 5(1):82–91. https://doi.org/10.1016/j.bioactmat.2020.01.004
Wang C, Lai J, Li K, Zhu S, Lu B, Liu J et al (2021) Cryogenic 3D printing of dual-delivery scaffolds for improved bone regeneration with enhanced vascularization. Bioact Mater 6(1):137–145. https://doi.org/10.1016/j.bioactmat.2020.07.007
Wang G, Zhu J, Chen X, Dong H, Li Q, Zeng L et al (2018) Alginate based antimicrobial hydrogels formed by integrating Diels–Alder “click chemistry” and the thiol–ene reaction. RSC Adv 8(20):11036–11042. https://doi.org/10.1039/C8RA00668G
Wang Y, Li L, Ma Y, Tang Y, Zhao Y, Li Z et al (2020b) Multifunctional supramolecular hydrogel for prevention of epidural adhesion after laminectomy. ACS Nano 14(7):8202–8219. https://doi.org/10.1021/acsnano.0c01658
Wang Y, Xue Y, Wang J, Zhu Y, Zhu Y, Zhang X et al (2019) A composite hydrogel with high mechanical strength, fluorescence, and degradable behavior for bone tissue engineering. Polymers 11(7):1112. https://doi.org/10.3390/polym11071112
Wang Z, Liu H, Luo W, Cai T, Li Z, Liu Y et al (2020a) Regeneration of skeletal system with genipin crosslinked biomaterials. J Tissue Eng 11:2041731420974861. https://doi.org/10.1177/2041731420974861
Webber MJ (2016) Engineering responsive supramolecular biomaterials: tToward smart therapeutics. Bioeng Transl Med 1(3):252–266. https://doi.org/10.1002/btm2.10031
Wu H, Wang K, Wang H, Chen F, Huang W, Chen Y et al (2017) Novel self-assembled tacrolimus nanoparticles cross-linking thermosensitive hydrogels for local rheumatoid arthritis therapy. Colloids Surf B Biointerfaces 149:97–104. https://doi.org/10.1016/j.colsurfb.2016.10.013
**an S, Webber MJ (2020) Temperature-responsive supramolecular hydrogels. J Mater Chem B 8(40):9197–9211. https://doi.org/10.1039/D0TB01814G
Xu C, Chen J, Li L, Pu X, Chu X, Wang X et al (2018) Promotion of chondrogenic differentiation of mesenchymal stem cells by copper: implications for new cartilage repair biomaterials. Mater Sci Eng C 93:106–114. https://doi.org/10.1016/j.msec.2018.07.074
Xu M, Qin M, Zhang X, Zhang X, Li J, Hu Y et al (2020) Porous PVA/SA/HA hydrogels fabricated by dual-crosslinking method for bone tissue engineering. J Biomater Sci Polym Ed 31(6):816–831. https://doi.org/10.1080/09205063.2020.1720155
Yang R, Li G, Zhuang C, Yu P, Ye T, Zhang Y et al (2021b) Gradient bimetallic ion–based hydrogels for tissue microstructure reconstruction of tendon-to-bone insertion. Sci Adv 7(26):eabg3816. https://doi.org/10.1126/sciadv.abg3816
Yang Z, Zhao F, Zhang W, Yang Z, Luo M, Liu L et al (2021a) Degradable photothermal bioactive glass composite hydrogel for the sequential treatment of tumor-related bone defects: from anti-tumor to repairing bone defects. Chem Eng J 419:129520. https://doi.org/10.1016/j.cej.2021.129520
Zafeiris K, Brasinika D, Karatza A, Koumoulos E, Karoussis I, Kyriakidou K et al (2021) Additive manufacturing of hydroxyapatite–chitosan–genipin composite scaffolds for bone tissue engineering applications. Mater Sci Eng C 119:111639. https://doi.org/10.1016/j.msec.2020.111639
Zhang J, Zhou H, Yang K, Yuan Y, Liu C (2013) RhBMP-2-loaded calcium silicate/calcium phosphate cement scaffold with hierarchically porous structure for enhanced bone tissue regeneration. Biomaterials 34(37):9381–9392. https://doi.org/10.1016/j.biomaterials.2013.08.059
Zhang K, Feng Q, Fang Z, Gu L, Bian L (2021c) Structurally dynamic hydrogels for biomedical applications: pursuing a fine balance between macroscopic stability and microscopic dynamics. Chem Rev 121(18):11149–11193. https://doi.org/10.1021/acs.chemrev.1c00071
Zhang Y, Cao Y, Zhao H, Zhang L, Ni T, Liu Y et al (2020) An injectable BMSC-laden enzyme-catalyzed crosslinking collagen-hyaluronic acid hydrogel for cartilage repair and regeneration. J Mater Chem B 8(19):4237–4244. https://doi.org/10.1039/D0TB00291G
Zhang Y, Chen H, Zhang T, Zan Y, Ni T, Cao Y et al (2019) Injectable hydrogels from enzyme-catalyzed crosslinking as BMSCs-laden scaffold for bone repair and regeneration. Mater Sci Eng C 96:841–849. https://doi.org/10.1016/j.msec.2018.12.014
Zhang Z, Jia B, Yang H, Han Y, Wu Q, Dai K et al (2021a) Biodegradable ZnLiCa ternary alloys for critical-sized bone defect regeneration at load-bearing sites: in vitro and in vivo studies. Bioact Mater 6(11):3999–4013. https://doi.org/10.1016/j.bioactmat.2021.03.045
Zhang Z, Jia B, Yang H, Han Y, Wu Q, Dai K et al (2021b) Zn0. 8Li0. 1Sr—a biodegradable metal with high mechanical strength comparable to pure Ti for the treatment of osteoporotic bone fractures: In vitro and in vivo studies. Biomaterials 275:120905. https://doi.org/10.1016/j.biomaterials.2021.120905
Zheng L, Liu S, Cheng X, Qin Z, Lu Z, Zhang K et al (2019) Intensified stiffness and photodynamic provocation in a collagen-based composite hydrogel drive chondrogenesis. Adv Sci 6(16):1900099. https://doi.org/10.1002/advs.201900099
Zhu H, Yang H, Ma Y, Lu TJ, Xu F, Genin GM et al (2020) Spatiotemporally controlled photoresponsive hydrogels: design and predictive modeling from processing through application. Adv Funct Mater 30(32):2000639. https://doi.org/10.1002/adfm.202000639
Zohreband Z, Adeli M, Zebardasti A (2021) Self-healable and flexible supramolecular gelatin/MoS2 hydrogels with molecular recognition properties. Int J Biol Macromol 182:2048–2055. https://doi.org/10.1016/j.ijbiomac.2021.05.106
Funding
Self-funded by the authors.
Author information
Authors and Affiliations
Contributions
Zahra Ebrahimvand Dibazar: conceptualization, investigation, and writing—original draft. Hadi Kokabi, Mehdi Shahgolzari, Meysam Mohammadikhah, Shamam Kareem Oudah, and Milad Elyasi: investigation and writing—original/revised draft. Mahdi Azizy, Hadi Kokabi, and Leila Delnabi Asl: writing—review and editing, visualization, supervision, and project administration. All co-authors approved the final version of the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Dibazar, Z.E., Zarei, M., Mohammadikhah, M. et al. Crosslinking strategies for biomimetic hydrogels in bone tissue engineering. Biophys Rev 15, 2027–2040 (2023). https://doi.org/10.1007/s12551-023-01141-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12551-023-01141-x