Abstract
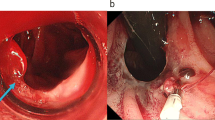
An 80-year old man with myelofibrosis and chronic renal disease was admitted to our hospital because of severe anemia and gastrointestinal bleeding. Although no bleeding was observed by upper or lower endoscopy, contrast-enhanced computed tomography revealed an enhanced area in the small intestinal wall that was suspected of being the bleeding site, and was confirmed by double-balloon endoscopy. Based on endoscopic findings, it was difficult to differentiate between variceal rupture and collapse of a submucosal tumor. We performed segmental resection of the small intestine to make a definitive diagnosis and achieve reliable hemostasis. The gross findings confirmed a variceal rupture from the small intestine. His gastrointestinal bleeding stopped and his anemia improved following surgery. Although some cases of portal hypertension in association with myelofibrosis have been reported, we are aware of no prior reports of variceal rupture in the small intestine. To our knowledge, this is the first reported case of ectopic jejunal varices in a patient with myelofibrosis.



Similar content being viewed by others
References
Ward HP, Block MH. The natural history of agnogenic myeloid metaplasia (AMM) and a critical evaluation of its relationship with the myeloproliferative syndrome. Medicine (Baltimore). 1971;50:357–420.
Sullivan A, Rheinlander H, Weintraub LR. Esophageal varices in agnogenic myeloid metaplasia: disappearance after splenectomy A case report. Gastroenterology. 1974;66:429–32.
Tokai K, Miyatani H, Yoshida Y, et al. Multiple esophageal variceal ruptures with massive ascites due to myelofibrosis-induced portal hypertension. World J Gastroenterol. 2012;18:3770–4.
Takasaki M, Takahashi I, Takamatsu M, et al. Endoscopic injection sclerotherapy for esophageal variceal hemorrhage in a patient with idiopathic myelofibrosis. J Gastroenterol. 1996;31:260–2.
Kasper P, Schramm C, Jaspers N, et al. Jejunal varices as a rare cause of recurrent gastrointestinal bleeding in a 74-year-old man with extrahepatic portal hypertension after pancreato-biliary surgery. BMJ Case Rep. 2019; 12. e228527.
Saeki Y, Ide K, Kakizawa H, et al. Controlling the bleeding of jejunal varices formed at the site of choledochojejunostomy: report of 2 cases and a review of the literature. Surg Today. 2013;43:550–5.
Levine RL, Wadleigh M, Cools J, et al. Activating mutation in the tyrosine kinase JAK2 in polycythemia vera, essential thrombocythemia, and myeloid metaplasia with myelofibrosis. Cancer Cell. 2005;7:387–97.
Pereira A, Bruguera M, Cervantes F, et al. Liver involvement at diagnosis of primary myelofibrosis: a clinicopathological study of twenty-two cases. Eur J Haematol. 1988;40:355–61.
Wanless IR, Peterson P, Das A, et al. Hepatic vascular disease and portal hypertension in polycythemia vera and agnogenic myeloid metaplasia: a clinicopathological study of 145 patients examined at autopsy. Hepatology. 1990;12:1166–74.
Dubois A, Dauzat M, Pignodel C, et al. Portal hypertension in lymphoproliferative and myeloproliferative disorders: hemodynamic and histological correlations. Hepatology. 1993;17:246–50.
Jacobs P, Maze S, Toyob F, et al. Myelofibrosis, splenomegaly, and portal hypertension. Acta Hematologica. 1985;74:45–8.
Silverstein MN, Wollaeger EE, Baggenstoss AH. Gastrointestinal and abdominal manifestations of agnogenic myeloid metaplasia. Arch Intern Med. 1973;131:532–7.
Ligumski M, Polliack A, Benbassat J. Nature and incidence of liver involvement in agnogenic myeloid metaplasia. Scand J Haematol. 1978;21:81–93.
Yan M, Geyer H, Mesa R, et al. Clinical features of patients with Philadelphia-negative myeloproliferative neoplasms complicated by portal hypertension. Clin Lymphoma Myeloma Leuk. 2015;15:e1-5.
Reilly CR, Babushok DV, Martin K, et al. Multicenter analysis of the use of transjugular intrahepatic portosystemic shunt for management of MPN-associated portal hypertension. Am J Hematol. 2017;92:909–14.
Blackburn CRB. Acquired portal-pulmonary venous anastomosis complicating partial esophago-gastrectomy in a patient with portal hypertension. Thorax. 1956;11:30–5.
Watanabe N, Toyonaga A, Kojima S, et al. Current status of ectopic in Japan: results of a survey by the Japan Society for Portal Hypertension. Hepatol Res. 2010;40:763–76.
Norton ID, Andrews JC, Kamath PS. Management of ectopic varices. Hepatology. 1998;28:1154–8.
Sakuma Y, Yazumi S, Fukunaga T, et al. Melena from jejunal mucosal varices caused by esophageal variceal sclerotherapy-induced splenic arteriovenous fistula. Gastrointest Endosc. 2011;74:404–6.
Masuda K, Takenaga S, Ashida H, et al. Variceal bleeding in the small intestine successfully treated with balloon-occluded retrograde transvenous obliteration using N-butyl-2-cyanoacrylate: a case report. Radiol Case Rep. 2018;6(13):400–3.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Tomonori Wada, Yoshihiko Yano, Atsushi Yamamoto, Masato Kinoshita, Eiichiro Yasutomi, Yuri Hatazawa, Hiroki Hayashi, Yuuki Shiomi, Kimihiro Yamashita, Yoshihide Ueda and Yuzo Kodama declare that they have no conflict of interest.
Human rights
All procedures followed have been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments.
Informed consent
Informed consent was obtained from all patients for being included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wada, T., Yano, Y., Yamamoto, A. et al. Jejunal variceal rupture in a patient with myelofibrosis: a case report. Clin J Gastroenterol 14, 542–545 (2021). https://doi.org/10.1007/s12328-021-01373-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12328-021-01373-y