Abstract
Background
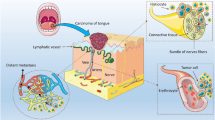
Perineural invasion (PNI) is recognized as a poor prognostic factor in oral squamous cell carcinoma (OSCC). However, the prognostic significance of further histologic subcategorization of PNI is inconclusive. In this study, we determined the prognostic relevance of histologic subcategories of PNI and their correlation with the presence of other clinical and pathological parameters
Methods
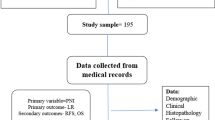
This is a retrospective study of 207 homogeneously treated OSCC patients with histologically documented PNI from a single center. Univariate and multivariate survival outcomes, namely, local recurrence-free survival (LRFS), disease-free survival (DFS), and overall survival (OS) of patients with various subcategories of PNI,namely- number of foci, size of the involved nerve, extratumoral or intratumoral extent, and intraneural or perineural location—were determined.
Results
Within the histologic subcategories of PNI, tongue primary and presence of lymph node metastasis correlated significantly with the number of nerves involved with PNI. Larger size of involved nerve correlated with advanced tumor stage. Number of foci, extent, and location of PNI were not prognostically significant except size of the involved nerve which showed an inverse correlation with disease outcome as involvement of larger nerves displayed better outcomes in terms of DFS and LRFS but not of OS on multivariate analysis. Addition of adjuvant chemotherapy to radiotherapy emerged as a significant predictor of improved LRFS, DFS, and OS.
Conclusions
Histologic subcategorization of PNI did not have prognostic relevance in our study. Involvement of even small nerves was associated with poor prognosis. Addition of chemoradiation was seen to improve prognosis.

Similar content being viewed by others
Data Availability
The data and material of this study are available from the corresponding author upon reasonable request.
Code Availability
Not applicable.
References
Binmadi NO, Basile JR. Perineural invasion in oral squamous cell carcinoma: a discussion of significance and review of the literature. Oral Oncol. 2011;47(11):1005–10. https://doi.org/10.1016/j.oraloncology.2011.08.002.
Haddad RI, Shin DM. Recent advances in head and neck cancer. N Engl J Med. 2008;359(11):1143–54. https://doi.org/10.1056/NEJMra0707975.
Chinn SB, Spector ME, Bellile EL, McHugh JB, Gernon TJ, Bradford CR, et al. Impact of perineural invasion in the pathologically N0 neck in oral cavity squamous cell carcinoma. Otolaryngology. 2013;149(6):893–9. https://doi.org/10.1177/0194599813506867.
Yang X, Tian X, Wu K, Liu W, Li S, Zhang Z, et al. Prognostic impact of perineural invasion in early stage oral tongue squamous cell carcinoma: Results from a prospective randomized trial. Surg Oncol. 2018;27(2):123–8. https://doi.org/10.1016/j.suronc.2018.02.005.
Brown B, Barnes L, Mazariegos J, Taylor F, Johnson J, Wagner RL. Prognostic factors in mobile tongue and floor of mouth carcinoma. Cancer. 1989;64(6):1195–202. https://doi.org/10.1002/1097-0142(19890915)64:6%3c1195::aid-cncr2820640606%3e3.0.co;2-7.
Rajappa SK, Ram D, Shukla H, Mandal G, Venkatasubramaniyan M, Dubey A, et al. Oncological benefits of postoperative radiotherapy in node-negative early stage cancer of the oral cavity with isolated perineural invasion. Br J Oral Maxillofac Surg. 2019;57(5):454–9. https://doi.org/10.1016/j.bjoms.2019.04.002.
Li J, Liu S, Li Z, Han X, Que L. Prognostic value of perineural invasion in oral tongue squamous cell carcinoma: a systematic review and meta-analysis. Front Oncol. 2021;11:683825. https://doi.org/10.3389/fonc.2021.683825.
Liao CT, Chang JT, Wang HM, Ng SH, Hsueh C, Lee LY, et al. Does adjuvant radiation therapy improve outcomes in pT1-3N0 oral cavity cancer with tumor-free margins and perineural invasion? Int J Radiat Oncol Biol Phys. 2008;71(2):371–6. https://doi.org/10.1016/j.ijrobp.2007.10.015.
Le Tourneau C, Jung GM, Borel C, Bronner G, Flesch H, Velten M. Prognostic factors of survival in head and neck cancer patients treated with surgery and postoperative radiation therapy. Acta Otolaryngol. 2008;128(6):706–12. https://doi.org/10.1080/00016480701675668.
Arun I, Maity N, Hameed S, Jain PV, Manikantan K, Sharan R, et al. Lymph node characteristics and their prognostic significance in oral squamous cell carcinoma. Head Neck. 2021;43(2):520–33. https://doi.org/10.1002/hed.26499.
Jain PV, Sharan R, Manikantan K, Clark GM, Chatterjee S, Mallick I, et al. Redefining adequate margins in oral squamous cell carcinoma: outcomes from close and positive margins. Eur Arch Oto-rhino-laryngol. 2020;277(4):1155–65. https://doi.org/10.1007/s00405-019-05779-w.
Jain PV, Sharan R, Manikantan K, Mallick I, Chatterjee S, Arun I, et al. Clinicopathologic determinants of outcome in pathologic T4a (pT4a) squamous cell carcinoma of the gingivobuccal subsite of the oral cavity. Indian J Surg Oncol. 2019;10(4):594–9. https://doi.org/10.1007/s13193-019-00950-5.
Brandwein-Gensler M, Teixeira MS, Lewis CM, Lee B, Rolnitzky L, Hille JJ, et al. Oral squamous cell carcinoma: histologic risk assessment, but not margin status, is strongly predictive of local disease-free and overall survival. Am J Surg Pathol. 2005;29(2):167–78. https://doi.org/10.1097/01.pas.0000149687.90710.21.
Woolgar JA. Histopathological prognosticators in oral and oropharyngeal squamous cell carcinoma. Oral Oncol. 2006;42(3):229–39. https://doi.org/10.1016/j.oraloncology.2005.05.008.
da Silva SD, Kowalski LP. Perineural invasion in oral cancer: challenges, controversies and clinical impact. Chin Clin Oncol. 2019;8(S1):S5. https://doi.org/10.21037/cco.2018.11.04.
Network NCC: Head and Neck Cancer ( Version 1.2022). https://www.nccn.org/professionals/physician_gls/pdf/head-and-neck.pdf (2022). Accessed March,22,2022.
Tim Helliwell JW: Dataset for histopathology reporting of mucosal malignancies of the oral cavity. https://www.rcpath.org/uploads/assets/c4a9faf7-393a-4ba8-9532f719d8cdff3b/Dataset-for-histopathology-reporting-of-mucosal-malignancies-of-the-oral-cavity.pdf (2013). Accessed 15 May 2022.
Raja R Seethala: Protocol for the Examination of Specimens from Patients with Cancers of the Oral Cavity. https://documents.cap.org/protocols/HN.Oral_4.1.1.0.REL_CAPCP.pdf Accessed Version: 4.1.1.0.
Müller S BS, Day TA, Magliocca K, Richardson MS, Sloan P, Tilakaratne WM, Zain RB, Thompson LDR. Carcinomas of the Oral Cavity, Histopathology Reporting Guide. 1st edition ed. Sydney, Australia: International Collaboration on Cancer Reporting; 2018.
Miller ME, Palla B, Chen Q, Elashoff DA, Abemayor E, St John MA, et al. A novel classification system for perineural invasion in noncutaneous head and neck squamous cell carcinoma: histologic subcategories and patient outcomes. Am J Otolaryngol. 2012;33(2):212–5. https://doi.org/10.1016/j.amjoto.2011.06.003.
Aivazian K, Ebrahimi A, Low TH, Gao K, Clifford A, Shannon K, et al. Perineural invasion in oral squamous cell carcinoma: quantitative subcategorisation of perineural invasion and prognostication. J Surg Oncol. 2015;111(3):352–8. https://doi.org/10.1002/jso.23821.
Liebig C, Ayala G, Wilks JA, Berger DH, Albo D. Perineural invasion in cancer: a review of the literature. Cancer. 2009;115(15):3379–91. https://doi.org/10.1002/cncr.24396.
Hasmat S, Ebrahimi A, Gao K, Low TH, Palme C, Gupta R, et al. Multifocal perineural invasion is a better prognosticator than depth of invasion in oral squamous cell carcinoma. Head Neck. 2019;41(11):3992–9. https://doi.org/10.1002/hed.25940.
Fagan JJ, Collins B, Barnes L, D’Amico F, Myers EN, Johnson JT. Perineural invasion in squamous cell carcinoma of the head and neck. Arch Otolaryngol. 1998;124(6):637–40. https://doi.org/10.1001/archotol.124.6.637.
Cracchiolo JR, Xu B, Migliacci JC, Katabi N, Pfister DG, Lee NY, et al. Patterns of recurrence in oral tongue cancer with perineural invasion. Head Neck. 2018;40(6):1287–95. https://doi.org/10.1002/hed.25110.
Wei PY, Li WY, Tai SK. Discrete Perineural Invasion Focus Number in Quantification for T1–T2 Oral Squamous Cell Carcinoma. Otolaryngology. 2019;160(4):635–41. https://doi.org/10.1177/0194599818808510.
Acknowledgements
The authors would like to thank Mr. Surajit Bag and Mr. Debabrata Das for technical assistance.
Funding
This study was not supported by any funding. The authors have no relevant financial or non-financial interests to disclose.
Author information
Authors and Affiliations
Contributions
IA: study design, data collection, histopathological analysis, and manuscript writing. PR: data collection, histopathological analysis, and manuscript review. PJ: data collection and manuscript review. SH: data collection and manuscript review. KM: data collection and manuscript review. PA: concept, study design, statistical analysis, and manuscript writing.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical Approval
Ethical approval was obtained from the Institutional Review Board (IRB) at our institute for this study (No.EC/WV/TMC/48/20).
Informed Consent
Not applicable. This study has obtained Institutional Review Board (IRB) at our institute and the need for informed consent was waived.
Consent for Publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Supplementary Figure. Survival analysis: PNI subcategories. Kaplan–Meier Curves comparing LRFS (Panel A), DFS (Panel B), and OS (Panel C) between various PNI subcategories. p values within the graphs indicate the log-rank statistic. None of the PNI subcategories demonstrated a significant difference in either LRFS, DFS, or OS on univariate analysis. Abbreviations: LRFS-Locoregional recurrence-free Survival; DFS-Disease-free survival; OS-Overall survival.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Arun, I., Roy, P., Jain, P.V. et al. Subcategorization of Perineural Invasion and Its Impact on Survival in Patients with Oral Squamous Cell Carcinoma. Head and Neck Pathol 17, 383–392 (2023). https://doi.org/10.1007/s12105-022-01512-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12105-022-01512-y