Abstract
Purpose of Review
Over 50% of the infections in most ICUs in tertiary care centres in India are caused by difficult to treat (DTR) gram-negative bacteria. The options available for the treatment of these infections are quite limited. This review discusses the epidemiology of these DTR infections in India and explores the various treatment strategies for these infections which are relevant in an Indian setting.
Recent Findings
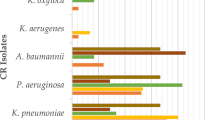
The most common organisms causing DTR infections in India are Klebsiella pneumoniae, Escherichia coli, Acinetobacter baumannii and Pseudomonas aeruginosa. The mechanisms of resistance in these organisms are not the same as those in DTR organisms prevalent in the western world. Treatment strategies recommended by western guidelines may not work in India. Management of these DTR organisms needs to be tailored to the situation in India.
Summary
Overuse of antibiotics has led to an alarming rate of DTR infections in Indian ICUs. The polymyxins are often the only drugs which are effective against many of these infections. Physicians in India and the government need to take urgent measures to control the spread of these organisms.
Key points
-
Antibiotic overuse has led to a situation where over 50% of infections in Indian ICUs are caused by DTR organisms.
-
Carbapenemase production is the primary mechanism of resistance in carbapenem-resistant Enterobacterales (CRE). Efflux pumps, altered outer membrane porin and production of carbapenemases are all implicated in DTR Pseudomonas aeruginosa and Acinetobacter baumannii.
-
KPC production is very uncommon in the CRE prevalent in India. Western guidelines may therefore not be relevant in India.
-
The polymyxins (in combination) and ceftazidime/avibactam with aztreonam are the drugs most often used to deal with DTR gram-negative bacteria in India.
-
Local delivery of antibiotics may be indicated in the management of these DTR infections in special sites like meningitis and pneumonia.


Similar content being viewed by others
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Kumar SG, Adithan C, Harish BN, Sujatha S, Roy G, Malini A. Antimicrobial resistance in India: a review. J Nat Sci Biol Med. 2013;4(2):286–91.
• Divatia JV, Mehta Y, Govil D, et al. the INDICAPS-II investigators. Intensive care in India in 2018–2019: the Second Indian Intensive Care Case Mix and Practice Patterns Study. Indian J Crit Care Med. 2021;25(10):1093–1107. A Bird’s eyeview of Intensive care in India.
Kadri SS, Lai YLE, Ricotta EE, et al. External validation of difficult-to-treat resistance prevalence and mortality risk in gram-negative bloodstream infection using electronic health record data from 140 US hospitals. Open Forum Infect Dis. 2019;6.
•• Annual report January 2021 to December 2021: Antimicrobial Resistance Research and Surveillance Network: Indian Council of Medical Research.
Breijyeh Z, Jubeh B, Karaman R. Resistance of gram-negative bacteria to current antibacterial agents and approaches to resolve it. Molecules. 2020;25(6):1340.
• Garg A, Garg J, Kumar S, Bhattacharya A, Agarwal S, Upadhyay GC. Molecular epidemiology & therapeutic options of carbapenem-resistant gram-negative bacteria. Indian J Med Res. 2019. Highlights differences between India and the West.
van Duin D, Doi Y. The global epidemiology of carbapenemase-producing Enterobacteriaceae. Virulence. 2017;8(4):460–469.
Paul M, Carrara E, Retamar P, Tängdén T, et al. European Society of Clinical Microbiology and Infectious Diseases (ESCMID) guidelines for the treatment of infections caused by multidrug-resistant gram-negative bacilli (endorsed by European Society of Intensive Care Medicine). Clin Microbiol Infect. 2022;28(4):521–47.
Tamma P, Aitken S, Bonomo R et al. Infectious Diseases Society of America 2023 guidance on the treatment of antimicrobial resistant gram-negative infections. Clin Infect Dis. 2023.
Tenover FC. Using molecular diagnostics to develop therapeutic strategies for carbapenem-resistant gram-negative infections. Front Cell Infect Microbiol. 2021;28:11.
Michalopoulos AS, Karatza DC. Multidrug-resistant gram-negative infections: the use of colistin. Expert Rev Anti Infect Ther. 2010;8:1009–17.
Nation RL, Velkov T, Li J. Colistin and polymyxin B: peas in a pod, or chalk and cheese? Clin Infect Dis. 2014;59(1):88–94.
GLASS (Global Antimicrobial Resistance and Use Surveillance System); The detection and reporting of colistin resistance; second edition; World Health Organisation.
Shirley M. Ceftazidime-avibactam: a review in the treatment of serious gram-negative bacterial infections. Drugs. 2018;78(6):675–92.
de Jonge BL, Karlowsky JA, Kazmierczak KM, et al. In vitro susceptibility to ceftazidime-avibactam of carbapenem-nonsusceptible Enterobacteriaceae isolates collected during the INFORM Global Surveillance Study (2012 to 2014). Antimicrob Agents Chemother. 2016;60(5):3163–9.
Betrosian AP, Frantzeskaki F, Xanthaki A, Douzinas EE. Efficacy and safety of high-dose ampicillin/sulbactam vs. colistin as monotherapy for the treatment of multidrug resistant Acinetobacter baumannii ventilator-associated pneumonia. J Infect. 2008;56:432–6.
Taha R, Kader O, Shawky S, et al. Ceftazidime-avibactam plus aztreonam synergistic combination tested against carbapenem-resistant Enterobacterales characterized phenotypically and genotypically: a glimmer of hope. Ann Clin Microbiol Antimicrob. 2023;22:21.
Veeraraghavan B, Bakthavatchalam YD, Soman R, et al. Management of serious infections caused by metallo β-lactamases with or without OXA-48-like expressing Enterobacterales with aztreonam and ceftazidime/avibactam combination: dosing strategy for better clinical outcome. Indian J Med Microbiol. 2021;39(3):286–8.
Falagas ME, Karageorgopoulos DE, Dimopoulos G. Clinical significance of the pharmacokinetic and pharmacodynamic characteristics of tigecycline. Curr Drug Metab. 2009;10(1):13–21.
Zha L, Pan L, Guo J, French N, Villanueva EV, Tefsen B. Effectiveness and safety of high dose tigecycline for the treatment of severe infections: a systematic review and metaanalysis. Adv Ther. 2020;37(3):1049–64.
Lashinsky JN, Henig O, Pogue JM, Kaye KS. Minocycline for the treatment of multidrug and extensively drug-resistant A. baumannii: a review. Infect Dis Ther. 2017 Jun;6(2):199–211.
Hashemian SMR, Farhadi Z, Farhadi T. Fosfomycin: the characteristics, activity, and use in critical care. Ther Clin Risk Manag. 2019;15:525–30.
•• Guidance on diagnosis, management of carbapenem resistant gram-negative infections. Division of Epidemiology & Communicable Diseases, Indian Council of Medical Research, New Delhi. 2022. Comprehensive Guidelines relevant to the Indian situation.
Yamamoto M, Pop-Vicas AE. Treatment for infections with carbapenem-resistant Enterobacteriaceae: what options do we still have? Crit Care. 2014;18:229.
•• Veeraraghavan B, Pragasam AK, Bakthavatchalam YD, et al. Colistin-sparing approaches with newer antimicrobials to treat carbapenem-resistant organisms: current evidence and future prospects. Indian J Med Microbiol. 2019;37:72–90. Discusses the various options available to Indian physicians.
Bakthavatchalam YD, Walia K, Veeraraghavan B. Susceptibility testing for aztreonam plus ceftazidime/avibactam combination: a general guidance for clinical microbiology laboratories in India. Indian J Med Microbiol. 2022;40(1):3–6.
van Duin D, Lok JJ, Earley M, et al. Antibacterial Resistance Leadership Group. Colistin versus ceftazidime-avibactam in the treatment of infections due to carbapenem-resistant Enterobacteriaceae. Clin Infect Dis. 2018;66(2):163–171.
Hakeam HA, Alsahli H, et al. Effectiveness of ceftazidime–avibactam versus colistin in treating carbapenem-resistant Enterobacteriaceae bacteremia. Int J Infect Dis. 2021;109: 1–7.
Pragasam AK, Veeraraghavan B, Nalini E, et al. An update on antimicrobial resistance and the role of newer antimicrobial agents for Pseudomonas aeruginosa. Indian J Med Microbiol. 2018;36:303–16.
Zhu Y, Monsel A, Roberts JA, et al. European Investigator Network for Nebulized Antibiotics in Ventilator-Associated Pneumonia (ENAVAP). Nebulized colistin in ventilator-associated pneumonia and tracheobronchitis: historical background, pharmacokinetics and perspectives. Microorganisms. 2021;9(6):1154.
Karaiskos I, Galani L, Baziaka F, Giamarellou H. Intraventricular and intrathecal colistin as the last therapeutic resort for the treatment of multidrug-resistant and extensively drug-resistant Acinetobacter baumannii ventriculitis and meningitis: a literature review. Int J Antimicrob Agents. 2013;41(6):499–508.
Author information
Authors and Affiliations
Contributions
NB did a literature search and summarised important sections of each article. AH prepared a rough draft of the final article. FNK wrote the final draft and added the section on individual antibiotics. All 3 authors reviewed the final manuscript. FNK and NB prepared the figures and tables. AH made the modifications suggested by the reviewer.
Corresponding author
Ethics declarations
Conflict of Interest
Dr. HEGDE reports personal fees from Glenmark Pharmaceutical, personal fees from Pfizer Pharmaceutical, personal fees from Alkem Pharmaceutical , personal fees from Sanofi Pharmaceutical, outside the submitted work; . Dr Kapadia & Dr Bannore have no conflict of interest
Human and Animal Rights and Informed Concent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Bannore, N., Kapadia, F. & Hegde, A. Difficult to Treat Gram-Negative Bacteria—The Indian Scenario. Curr Infect Dis Rep 26, 69–77 (2024). https://doi.org/10.1007/s11908-024-00834-y
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11908-024-00834-y