Abstract
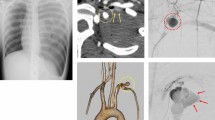
Atraumatic tension hemothorax is extremely rare. We report a case of 62-year-old woman presented with obstructive and hypovolemic shock status by tension hemothorax due to ruptured aneurysm of congenital intercostal artery–azygous fistula. Contrast-enhanced computed tomography and aortography revealed an aberrant 12th intercostal artery flowing into the aneurysm with a fistula draining into the azygous vein and the rupture of aneurysm. Our experience indicates that the rupture of congenital arteriovenous fistulas (AVFs) of systemic circulation in the thoracic cavity might cause not only hypovolemic shock but also atraumatic tension hemothorax. Surgery following preoperative endovascular embolization offers a feasible treatment strategy for ruptured aneurysms associated with AVFs.



Similar content being viewed by others
References
Hu H, Liu W, Tang J, et al. Aorto-azygous fistula complicated by arteriovenous aneurysm treated with video-assisted thoracic surgery. Ann Thorac Surg. 2015;99:e107–9.
Roth TC, Manness WK, Hershey BL, et al. Complex vertebral arteriovenous fistula and ruptured aneurysm in neurofibromatosis: a therapeutically challenging case. Skull Base Surg. 2000;10:35–41.
Kim SJ, Kim CW, Kim S, et al. Endovascular treatment of a ruptured internal thoracic artery pseudoaneurysm presenting as a massive hemothorax in a patient with type I neurofibromatosis. Cardiovasc Interv Radiol. 2005;28:818–21.
Sutton D, North EA. Unusual arteriovenous communications presenting as cardiac murmurs in infancy: report of three cases. Br J Radiol. 1977;50:871–5.
Soler P, Mehta AV, Garcia OL, et al. Congenital systemic arteriovenous fistula between the descending aorta, azygos vein, and superior vena cava. Chest. 1981;80:647–9.
Gamba PG, Longo M, Zanon GF, et al. Arteriovenous fistula between descending aorta and hemiazygos vein. Eur J Pediatr Surg. 1991;1:49–50.
Siddhartha W, Parmar H, Shrivastav M, et al. Endovascular glue embolisation of intercostal arteriovenous fistula: a non-surgical treatment option. J Postgrad Med. 2000;46:213–4.
Coulter TD, Maurer JR, Miller MT, et al. Chest wall arteriovenous fistula: an unusual complication after chest tube placement. Ann Thorac Surg. 1996;67:849–50.
Fukuda W, Taniguchi S, Fukuda I. Endovascular treatment of ruptured intercostal arteriovenous fistulas associated with neurofibromatosis type 1. Ann Vasc Dis. 2012;5:109–12.
Kim HJ, Seon HJ, Choi S, et al. Ruptured aneurysm of intercostal arteriovenous malformation associated with neurofibromatosis type 1: a case report. Cardiovasc Interv Radiol. 2011;34(Suppl 2):S74–7.
Yilmaz S, Atinkaya C, Aktas A, et al. Giant arteriovenous malformation located on the chest wall—diagnosis and endovascular treatment: report of a case. Surg Today. 2010;40:1164–8.
Grillo HC, Athanasoulis CA. Tracheal obstruction from mediastinal arteriovenous malformation. J Thorac Cardiovasc Surg. 2004;128:780–2.
Oto O, Metin SK, Guzeloglu M, et al. A congenital arteriovenous malformation originating from the aorta locating in the posterior mediastinum. Ann Thorac Cardiovasc Surg. 2012;18:387–90.
Acknowledgements
We thank Susan Furness, PhD, from Edanz Group (http://www.edanzediting.com/ac) for editing a draft of this manuscript and Satoshi Akagi for creating schemes.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Nakayama, T., Uehara, H., Osawa, M. et al. Atraumatic tension hemothorax associated with ruptured aneurysm of intercostal artery–azygous fistula: a case report. Gen Thorac Cardiovasc Surg 66, 552–555 (2018). https://doi.org/10.1007/s11748-018-0922-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11748-018-0922-1