Abstract
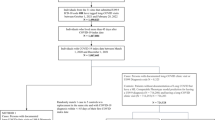
The administrative claims database of the Italian region Lombardy, the first in Europe to be hit by the SARS-CoV-2 pandemic, was employed to evaluate the impact on healthcare resource utilization following recovery from the second (mainly alpha-related variant) and third (delta-related) infection waves. 317,164 individuals recovered from the infection and became negative after the second wave, 271,180 after the third. Of them, 1571 (0.5%) and 1575 (0.6%) died in the first 6 post-negativization months. In the remaining cases (315,593 after the second wave and 269,605 after the third), hospitalizations, attendances to emergency rooms and outpatient visits were compared with those recorded in the same pre-pandemic time periods in 2019. Dispensation of drugs as well as of imaging, and functional and biochemical diagnostic tests were also compared as additional proxies of the healthcare impact of the SARS-CoV-2 infection waves. Following both waves, hospitalizations, attendances at emergency rooms, and outpatient visits were similar in number and rates to the pre-pandemic periods. However, there was an increased dispensation a number of drugs and diagnostic tests, particularly those addressing the cardiorespiratory and blood systems. In a large region such as Lombardy taken as a relevant model because early and severely hit by the SARS-CoV-2 pandemic, the post-COVID burden on healthcare facilities was mildly relevant in cases who recovered from the second and third infection waves regarding such pivotal events as deaths, hospitalizations, and need for emergency room and outpatient visits, but was high regarding the dispensation of some drug classes and types of diagnostic tests.
Similar content being viewed by others
Data availability
Only upon permission by the Lombardy Region.
References
Consolandi E (2021) Chapter 1.3—Evolution and intensity of infection in Lombardy. In: Casti E, Adobati F, Negri I (eds) Map** the epidemic: a systemic geography of COVID-19 in Italy, volume 9. https://www.sciencedirect.com/science/article/abs/pii/B9780323910613000089. Accessed Mar 2023
https://www.regione.lombardia.it/wps/portal/istituzionale/HP/vaccinazionicovid. Accessed Mar 2023
https://opendatamds.maps.arcgis.com/apps/dashboards/0f1c9a02467b45a7b4ca12d8ba296596. Accessed Mar 2023
Caramello V, Catalano A, Macciotta A, Dansero L, Sacerdote C, Costa G et al (2022) Improvements throughout the three waves of COVID-19 pandemic: results from 4 million inhabitants of North-West Italy. J Clin Med 11(15):4304
Mannucci PM, Galbussera AA, D’Avanzo B, Tettamanti M, Remuzzi G, Fortino I, Leoni O, Harari S, Nobili A (2023) Two years of SARS-CoV-2 pandemic and COVID-19 in Lombardy, Italy. Intern Emerg Med. https://doi.org/10.1007/s11739-023-03315-7
Havers FP, Pham H, Taylor CA, Whitaker M, Patel K, Anglin O et al (2022) COVID-19-associated hospitalizations among vaccinated and unvaccinated adults 18 years or older in 13 US States, January 2021 to April 2022. JAMA Intern Med 182(10):1071–1081
Taylor CA, Whitaker M, Anglin O, Milucky J, Patel K, Pham H et al (2022) COVID-19-associated hospitalizations among adults during SARS-CoV-2 delta and omicron variant predominance, by race/ethnicity and vaccination status—COVID-NET, 14 states, July 2021–January 2022. MMWR Morb Mortal Wkly Rep 71(12):466–473
Bobrovitz N, Ware H, Ma X, Li Z, Hosseini R, Cao C et al (2023) Protective effectiveness of previous SARS-CoV-2 infection and hybrid immunity against the omicron variant and severe disease: a systematic review and meta-regression. Lancet Infect Dis. https://doi.org/10.1016/S1473-3099(22)00801-5
Parums DV (2021) Editorial: long-COVID, or post-COVID syndrome, and the global impact on health care. Med Sci Monit 27:e933446
Sanchez-Ramirez DC, Normand K, Zhaoyun Y, Torres-Castro R (2021) Long-term impact of COVID-19: a systematic review of the literature and meta-analysis. Biomedicines. 9(8):900
Alkodaymi MS, Omrani OA, Fawzy NA, Shaar BA, Almamlouk R, Riaz M et al (2022) Prevalence of post-acute COVID-19 syndrome symptoms at different follow-up periods: a systematic review and meta-analysis. Clin Microbiol Infect 28(5):657–666
Bussani R, Zentilin L, Correa R, Colliva A, Silvestri F, Zacchigna S et al (2023) Persistent SARS-CoV-2 infection in patients seemingly recovered from COVID-19. J Pathol 259(3):254–263
Mannucci PM, Nobili A, Tettamanti M, D’Avanzo B, Galbussera AA, Remuzzi G et al (2022) Impact of the post-COVID-19 condition on health care after the first disease wave in Lombardy. J Intern Med 292(3):450–462
Mannucci PM, Nobili A, Tettamanti M, D’Avanzo B, Galbussera AA, Remuzzi G et al (2022) Progressive decrease of the healthcare impact of the post-COVID condition after the first disease wave in Lombardy, Italy. J Intern Med 292(6):961–964
ATC/DDD Index 2021. https://www.whocc.no/atc_ddd_index/. Accessed Mar 2023
McNaughton CD, Austin PC, Sivaswamy A, Fang J, Abdel-Qadir H, Daneman N et al (2022) Post-acute health care burden after SARS-CoV-2 infection: a retrospective cohort study. CMAJ 194(40):E1368–E1376
Peter RS, Nieters A, Kräusslich HG, Brockmann SO, Göpel S, Kindle G et al (2022) Post-acute sequelae of covid-19 six to 12 months after infection: population based study. BMJ 379:e071050
Tsioutis C, Tofarides A, Spernovasilis N (2022) Transition beyond the acute phase of the COVID-19 pandemic: need to address the long-term health impacts of COVID-19. World J Clin Cases 10(27):9967–9969
Paterson C, Davis D, Roche M, Bissett B, Roberts C, Turner M et al (2022) What are the long-term holistic health consequences of COVID-19 among survivors? An umbrella systematic review. J Med Virol 94(12):5653–5668
Global Burden of Disease Long COVID Collaborators (2022) Estimated global proportions of individuals with persistent fatigue, cognitive, and respiratory symptom clusters following symptomatic COVID-19 in 2020 and 2021. JAMA 328(16):1604–1605
Rapin A, Boyer FC, Mourvillier B, Giordano Orsini G, Launois C et al (2022) Post-intensive care syndrome prevalence six months after critical COVID-19: comparison between first and second waves. J Rehabil Med 54:jrm00339. https://doi.org/10.2340/jrm.v54.4363
https://www.istat.it/it/files/2020/03/tabella-regionale-decessi-totali-14022023-1.xlsx. Accessed Mar 2023
WHO Coronavirus (COVID-19) Dashboard. https://covid19.who.int/. Accessed Mar 2023
WHO Coronavirus (COVID-19) Italy. https://covid19.who.int/region/euro/country/it. Accessed Mar 2023
Acknowledgements
The authors would like to thank Giuseppe Preziosi, Monica Arivetti, and Giovanna Rigotti from ARIA S.p.A, Alfredo Bevilacqua from Laife Reply S.p.A., Marco D. Forlani from T Bridge—BV Tech S.p.A, and Igor Monti from Istituto di Ricerche Farmacologiche Mario Negri IRCCS who kindly assisted us with data collection. The authors would also like to thank Regione Lombardia, under Grant/Award No. DGR n. 3375—July 14, 2020, and Health Ministry of the Lombardy, under Grant/Award No. EPIFARM-Pharmaco-epidemiology.
Funding
This work was supported by Regione Lombardia, under Grant/Award No. DGR n. 3375—July 14, 2020, and Health Ministry of the Lombardy, under Grant/Award No. EPIFARM-Pharmaco-epidemiology.
Author information
Authors and Affiliations
Contributions
SH, PMM, AN, MT, GR, BDA, and AAG: study concept and design; IF and OL: acquisition of data; SH, PMM, AN, MT, BDA, and AAG: analysis and interpretation of data; SH, PMM, AN, BDA, and MT: drafting of the manuscript. All authors were involved in the critical revision of the manuscript for important intellectual content. All authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
None of the authors declares to have conflict of interest.
Human and animal rights
This study was conducted according to the principles expressed in the Declaration of Helsinki and its later amendments, and approved by local Institutional Review Board (0051814/19).
Informed consent
Being a retrospective study performed on an administrative database of anonymized patients, patient informed consent was waived.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Harari, S., Mannucci, P.M., Nobili, A. et al. Post-recovery impact of the second and third SARS-CoV-2 infection waves on healthcare resource utilization in Lombardy, Italy. Intern Emerg Med 18, 2011–2018 (2023). https://doi.org/10.1007/s11739-023-03396-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11739-023-03396-4