Abstract
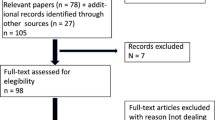
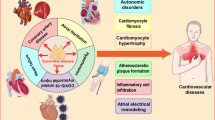
Epicardial adipose tissue (EAT) is a visceral fat depot located between the myocardium and visceral epicardium. Emerging evidence suggests that excessive EAT is linked to increased risk of cardiovascular conditions and other metabolic diseases. A literature search was conducted from the earliest studies to the 26th of November 2022 on PubMed, Embase, and the Cochrane. All the studies evaluating changes in EAT, pericardial adipose tissue (PAT), or total cardiac fat loss before and after BS were included. From 623 articles, 35 were eventually included in the systematic review. Twenty-one studies showed a significant reduction of EAT after BS, and only one study showed a non-significant reduction (p = 0.2).




Similar content being viewed by others
References
Wu FZ, Huang YL, Wu CC, et al. Differential effects of bariatric surgery versus exercise on excessive visceral fat deposits. Medicine (Baltimore). 2016;95(5):e2616.
Kokkinos A, Alexiadou K, Liaskos C, et al. Improvement in cardiovascular indices after Roux-en-Y gastric bypass or sleeve gastrectomy for morbid obesity. Obes Surg. 2013;23(1):31–8.
Sarmiento-Cobos M, Valera R, Botero Fonnegra C, et al. Ventricular conduction improvement after pericardial fat reduction triggered by rapid weight loss in subjects with obesity undergoing bariatric surgery. Surg Obes Relat Dis Off J Am Soc Bariatr Surg. 2022;18(2):288–94.
Gaborit B, Jacquier A, Kober F, et al. Effects of bariatric surgery on cardiac ectopic fat: lesser decrease in epicardial fat compared to visceral fat loss and no change in myocardial triglyceride content. J Am Coll Cardiol. 2012;60(15):1381–9.
Launbo N, Zobel EH, von Scholten BJ, et al. Targeting epicardial adipose tissue with exercise, diet, bariatric surgery or pharmaceutical interventions: A systematic review and meta-analysis. Obes Rev. 2021;22(1):e13136.
Secchi F, Asteria C, Monti CB, et al. Quantification of epicardial adipose tissue in obese patients using an open-bore MR scanner. Eur Radiol Exp. 2022;6(1):25.
Rabkin SW, Campbell H. Comparison of reducing epicardial fat by exercise, diet or bariatric surgery weight loss strategies: a systematic review and meta-analysis. Obes Rev. 2015;16(5):406–15.
Villasante Fricke AC, Iacobellis G. Epicardial adipose tissue: clinical biomarker of cardio-metabolic risk. Int J Mol Sci. 2019;20(23):5989.
Scarano Pereira JP, Owen E, Martinino A, et al. Epicardial adipose tissue, obesity, and the occurrence of atrial fibrillation: an overview of pathophysiology and treatment methods. Expert Rev Cardiovasc Ther. 2022;20(4):307–22.
Salman AA, Salman MA, Soliman A, et al. Changes of epicardial fat thickness after laparoscopic sleeve gastrectomy: a prospective study. Ann Med. 2021;53(1):523–30.
Packer M. Disease-treatment interactions in the management of patients with obesity and diabetes who have atrial fibrillation: the potential mediating influence of epicardial adipose tissue. Cardiovasc Diabetol. 2019;18(1):121.
Mahajan R, Wong CX. Obesity and metabolic syndrome in atrial fibrillation: cardiac and noncardiac adipose tissue in atrial fibrillation. Card Electrophysiol Clin. 2021;13(1):77–86.
Jones NR, Taylor KS, Clare JT, et al. Weight change and the risk of incident atrial fibrillation: a systematic review and meta-analysis. Heart. 2019;105(23):1799–805. https://heart.bmj.com/content/105/23/1799. Accessed 28 Nov 2022
Adami GF, Carbone F, Montecucco F, et al. Adipose tissue composition in obesity and after bariatric surgery. Obes Surg. 2019;29(9):3030–8.
Page MJ, McKenzie JE, Bossuyt PM, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;29(372):n71.
Lo CKL, Mertz D, Loeb M. Newcastle-Ottawa scale: comparing reviewers’ to authors’ assessments. BMC Med Res Methodol. 2014;1(14):45.
Su B, Qin W, Xue F, et al. The relation of passive smoking with cervical cancer. Medicine (Baltimore). 2018;97(46):e13061.
Abstracts of the 47th Annual Meeting of the EASD, Lisbon 2011. Diabetologia. 2011;54(1):1.
Vasques ACJ, Pareja JC, Souza JRM, et al. Epicardial and pericardial fat in type 2 diabetes: favourable effects of biliopancreatic diversion. Obes Surg. 2015;25(3):477–85.
van Schinkel LD, Sleddering MA, Lips MA, et al. Effects of bariatric surgery on pericardial ectopic fat depositions and cardiovascular function. Clin Endocrinol (Oxf). 2014;81(5):689–95.
Hunt SC, Davidson LE, Adams TD, et al. Associations of visceral, subcutaneous, epicardial, and liver fat with metabolic disorders up to 14 years after weight loss surgery. Metab Syndr Relat Disord. 2021;19(2):83–92.
Willens HJ, Byers P, Chirinos JA, et al. Effects of weight loss after bariatric surgery on epicardial fat measured using echocardiography. Am J Cardiol. 2007;99(9):1242–5.
Kaya BC, Elkan H. The impact of weight loss after laparoscopic sleeve gastrectomy on early markers of atherosclerotic vascular disease: a prospective study. Kardiologia Pol Pol Heart J. 2020;78(7–8):674–80.
Hannukainen JC, Lautamäki R, Pärkkä J, et al. Reversibility of myocardial metabolism and remodelling in morbidly obese patients 6 months after bariatric surgery. Diabetes Obes Metab. 2018;20(4):963–73.
Cekici Y, Kaya BC, Elkan H. The effect of laparoscopic sleeve gastrectomy on subclinical atherosclerosis in patients with severe obesity. Obes Surg. 2021;31(2):738–45.
Sarmiento-Cobos M, Aleman R, Gomez CO, et al. Weight loss following bariatric surgery decreases pericardial fat thickness lowering the risk of develo** coronary artery disease. Surg Obes Relat Dis. 2021;17(2):390–7.
Frea. Subclinical left ventricular dysfunction in severe obesity and reverse cardiac remodeling after bariatric surgery. 2022. https://www.jcecho.org/article.asp?issn=2211-4122;year=2020;volume=30;issue=1;spage=22;epage=28;aulast=Frea. Accessed 28 Nov 2022
Mikhalkova D, Holman SR, Jiang H, et al. Bariatric surgery–induced cardiac and lipidomic changes in obesity-related heart failure with preserved ejection fraction. Obesity. 2018;26(2):284–90.
Altin C, Erol V, Aydin E, et al. Impact of weight loss on epicardial fat and carotid intima media thickness after laparoscopic sleeve gastrectomy: a prospective study. Nutr Metab Cardiovasc Dis. 2018;28(5):501–9.
HIT Poster session 1. Eur Heart J Cardiovasc Imaging. 2017;18(suppl_3):iii21–5.
Integrated Physiology/Obesity. Diabetes. 2014;63(Supplement_1):A655–65.
Abstracts of the 49th Annual Meeting of the EASD. Diabetologia. 2013;56(1):1–566.
Kovac N, Grymyr LMD, Gerdts E, Nadirpour S, Nedrebø BG, Hjertaas JJ, et al. Markers of subclinical atherosclerosis in severe obesity and one year after bariatric surgery. J Clin Med. 2022;11(8):2237.
Schneiter S, Warrier R, Lefkovits L, et al. Effects of weight loss on left ventricle and pericardial fat assessed with cardiac magnetic resonance imaging in morbid obesity. Heart Lung Circ. 2010;1(19):S179.
Foppa M, Pond KK, Jones DB, et al. Subcutaneous fat thickness, but not epicardial fat thickness, parallels weight reduction three months after bariatric surgery: A cardiac magnetic resonance study. Int J Cardiol. 2013;168(4):4532–3.
Castillo A, Rivera E, Typhair C, et al. Echocardiographic assessment of epicardial fat pad and cardiac remodeling after bariatric surgery. J Am Coll Cardiol. 2021;77(18_Supplement_1):1342.
Tokhi B, Humphrey T, Harris E, et al. Effects of bariatric surgery on epicardial fat pat remodeling. J Am Coll Cardiol. 2020;75(11, Supplement 1):1597.
Abdesselam I, Dutour A, Kober F, et al. Time course of change in ectopic fat stores after bariatric surgery. J Am Coll Cardiol. 2016;67(1):117–9.
Luaces M, Cachofeiro V, Pedrazo JC, et al. Quantification of epicardial adipose tissue in morbidly obese patients before and after bariatric surgery. J Cardiovasc Magn Reson. 2014;16(1):P281.
Luaces M, Paiva M, Secades Gonzalez S, et al. Long-term changes in epicardial adipose tissue after bariatric surgery: a CMR study. J Am Coll Cardiol. 2013;61(10, Supplement):E1286.
Graziani F, Leone AM, Cialdella P, et al. Effects of bariatric surgery on cardiac remodeling: clinical and pathophysiologic implications. Int J Cardiol. 2013;168(4):4277–9.
Oral Sessions. Obes Facts. 2012;5(Suppl. 1):32–54.
Henry JA, Abdesselam I, Sorimachi H, et al. 13 The long-term effects of adipose depot change following bariatric surgery on cardiac geometry. Heart. 2022;108(Suppl 1):A11.
2019 Scientific Session of the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES), Baltimore, Maryland, USA, 3–6 April 2019: 2019 Posters. Surg Endosc. 2019;33(1):130–413.
Daud A, Dranow E, Ibrahim M. Effect of weight loss surgery on pericardial fat volume assessed by chest computed tomography. J Am Coll Cardiol. 2021;77(18_Supplement_1):1364.
Sarmiento-Cobos M, Cogollo VJ, Rivera CE, et al. Cardio-metabolic impact of bariatric surgery and its allometric effect on the heart’s shape, Anatomy, and Physiology. J Am Coll Surg. 2020;231(4, Supplement 2):e71.
Cobos MS, Rivera CE, Montorfano L, et al. Improvement in ventricular conduction after reduction in pericardial fat triggered by rapid weight loss in severely obese patients undergoing bariatric intervention. J Am Coll Surg. 2019;229(4):S24.
Zhou M, Wang H, Chen J. Epicardial adipose tissue and atrial fibrillation: possible mechanisms, potential therapies, and future directions. Pacing Clin Electrophysiol. 2020;43(1):133–45.
Can we decrease epicardial and pericardial fat in patients with diabetes? - Emir M. Muzurović, Snežana Vujošević, Dimitri P. Mikhailidis, 2021 https://journals.sagepub.com/doi/10.1177/10742484211006997. Accessed 28 Nov 2022
Scarano-Pereira JP, Martinino A, Manicone F, et al. Response to: ‘recent advances in the mechanisms underlying the beneficial effects of bariatric and metabolic surgery’. Surg Obes Relat Dis. 2021;S1550-7289(21):00494–9.
Author information
Authors and Affiliations
Contributions
Initial idea: JPSP, SP
Literature search and data collection: JPSP, MC, AM, SP
Data analysis: JPSP, MC, AM, SP
Writing of the paper: JPSP, MC, AM, DR, CS, CP, SW, LD, TH, OW, SP
Final approval: JPSP, MC, AM, DR, CS, CP, SW, LD, TH, OW, SP
Corresponding author
Ethics declarations
Ethical Approval
Not applicable
Informed Consent
Not applicable.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key Points
- Epicardial adipose tissue (EAT) is a visceral fat depot located between the myocardium and visceral epicardium.
- Excessive EAT is linked to increased risk of cardiovascular conditions and other metabolic diseases.
- Our systematic review showed that a significant reduction of EAT after bariatric surgery is seen.
- This indicates a beneficial effect of bariatric surgery on EAT.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Pereira, J.P.S., Calafatti, M., Martinino, A. et al. Epicardial Adipose Tissue Changes After Bariatric and Metabolic Surgery: a Systematic Review and Meta-analysis. OBES SURG 33, 3636–3648 (2023). https://doi.org/10.1007/s11695-023-06848-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-023-06848-0