Abstract
Background
Oral antibiotics (OAB) in colorectal surgery have been shown to reduce surgical site infections (SSIs) and possibly anastomotic leakage. However, evidence on long-term follow-up, reintervention rates and 5-year oncological follow-up is lacking. The current study aims at elucidating this knowledge gap.
Methods
This study evaluated the long-term effectiveness of perioperative ‘Selective decontamination of the digestive tract’ (SDD) in colorectal cancer surgery. The primary outcome was anastomotic leakage within 90 days, secondary outcomes included infectious complications, reinterventions, readmission, hospital stay, and 5-year overall and disease-free-survival. Statistical analysis including univariate and multivariate analysis was performed to identify predictors of 90-day outcomes, and Kaplan–Meier survival analysis was used for the 5-year survival outcomes.
Results
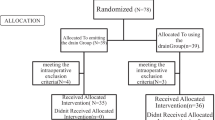
In total 455 patients were analyzed, 228 participants in the SDD group and 227 in the control group. Anastomotic leakage rate was not statistically different between the SDD and control group (6.6% versus 9.7%). One or more infectious complications occurred in 15.4% of patients in the SDD group and in 28.2% in the control group (OR 0.46, 95% C.I. 0.29 – 0.73). In the SDD group 8,8% of patients required a reintervention compared to 16,3% of patients in the control group (OR 0.47, 95% C.I. 0.26 – 0.84). After multivariable analysis SDD remained significant in reducing both infectious complications and reinterventions after 90-days follow-up. There was no difference between SDD and control group in 5-year overall survival and disease-free-survival.
Conclusion
SDD as OAB is effective in reducing 90-days postoperative infectious complications and reinterventions. As such, SDD as standard OAB in elective colorectal surgery is highly recommended.

Similar content being viewed by others
Data Availability
Data available on request from the corresponding author.
References
Abis, G.S.A., et al., Randomized clinical trial of selective decontamination of the digestive tract in elective colorectal cancer surgery (SELECT trial). Br J Surg, 2019. 106(4): p. 355-363.
Koskenvuo, L., et al., Mechanical and oral antibiotic bowel preparation versus no bowel preparation for elective colectomy (MOBILE): a multicentre, randomised, parallel, single-blinded trial. Lancet, 2019. 394(10201): p. 840-848.
Espin Basany, E., et al., Preoperative oral antibiotics and surgical-site infections in colon surgery (ORALEV): a multicentre, single-blind, pragmatic, randomised controlled trial. Lancet Gastroenterol Hepatol, 2020. 5(8): p. 729-738.
Yang, J., et al., The influence of anastomotic leakage for rectal cancer oncologic outcome: A systematic review and meta-analysis. J Surg Oncol, 2020. 121(8): p. 1283-1297.
Wang, S., et al., Adverse Effects of Anastomotic Leakage on Local Recurrence and Survival After Curative Anterior Resection for Rectal Cancer: A Systematic Review and Meta-analysis. World J Surg, 2017. 41(1): p. 277-284.
Zimlichman, E., et al., Health care-associated infections: a meta-analysis of costs and financial impact on the US health care system. JAMA Intern Med, 2013. 173(22): p. 2039-46.
Keenan, J.E., et al., Improving Outcomes in Colorectal Surgery by Sequential Implementation of Multiple Standardized Care Programs. J Am Coll Surg, 2015. 221(2): p. 404-14.e1.
Papp, G., et al., Systemic versus Oral and Systemic Antibiotic Prophylaxis (SOAP) study in colorectal surgery: prospective randomized multicentre trial. Br J Surg, 2021. 108(3): p. 271-276.
Rollins, K.E., et al., The Role of Oral Antibiotic Preparation in Elective Colorectal Surgery: A Meta-analysis. Ann Surg, 2019. 270(1): p. 43-58.
Grewal, S., et al., Oral Antibiotic Prophylaxis Reduces Surgical Site Infection and Anastomotic Leakage in Patients Undergoing Colorectal Cancer Surgery. Biomedicines, 2021. 9(9).
Morks, A.N., et al., Late anastomotic leakage in colorectal surgery: a significant problem. Colorectal Dis, 2013. 15(5): p. e271-5.
Tan, W.P., et al., Anastomotic leaks after colorectal anastomosis occurring more than 30 days postoperatively: a single-institution evaluation. Am Surg, 2014. 80(9): p. 868-72.
Borstlap, W.A.A., et al., Anastomotic Leakage and Chronic Presacral Sinus Formation After Low Anterior Resection: Results From a Large Cross-sectional Study. Ann Surg, 2017. 266(5): p. 870-877.
Roos, Daphne et al. “Perioperative selective decontamination of the digestive tract (SDD) in elective colorectal surgery.” Journal of gastrointestinal surgery : official journal of the Society for Surgery of the Alimentary Tract vol. 13,10 (2009): 1839-44.
Woodfield, J.C., et al., Strategies for Antibiotic Administration for Bowel Preparation Among Patients Undergoing Elective Colorectal Surgery: A Network Meta-analysis. JAMA Surg, 2021.
Bona, S., et al., Introducing an enhanced recovery after surgery program in colorectal surgery: a single center experience. World J Gastroenterol, 2014. 20(46): p. 17578-87.
Primrose, John N et al. “Effect of 3 to 5 years of scheduled CEA and CT follow-up to detect recurrence of colorectal cancer: the FACS randomized clinical trial.” JAMA vol. 311,3 (2014): 263-70. doi:https://doi.org/10.1001/jama.2013.285718
Henneman, Daniel et al. “Safety of elective colorectal cancer surgery: non-surgical complications and colectomies are targets for quality improvement.” Journal of surgical oncology vol. 109,6 (2014): 567-73. doi:https://doi.org/10.1002/jso.23532
Yang, S.Y., et al., Late anastomotic leakage after anal sphincter saving surgery for rectal cancer: is it different from early anastomotic leakage? Int J Colorectal Dis, 2020. 35(7): p. 1321-1330.
Ju, H.E., et al., High incidence rate of late anastomosis leakage in patients for rectal cancer after neoadjuvant chemoradiotherapy: A comparative study. Asian J Surg, 2021.
Kverneng Hultberg, D., et al., The Impact of Anastomotic Leakage on Long-term Function After Anterior Resection for Rectal Cancer. Dis Colon Rectum, 2020. 63(5): p. 619-628.
Mirnezami, A., et al., Increased local recurrence and reduced survival from colorectal cancer following anastomotic leak: systematic review and meta-analysis. Ann Surg, 2011. 253(5): p. 890-9.
Koedam, T.W.A., et al., Oncological Outcomes After Anastomotic Leakage After Surgery for Colon or Rectal Cancer: Increased Risk of Local Recurrence. Ann Surg, 2020.
Kulu, Y., et al., Anastomotic leakage is associated with impaired overall and disease-free survival after curative rectal cancer resection: a propensity score analysis. Ann Surg Oncol, 2015. 22(6): p. 2059-67.
Bogner, A., et al., Selective decontamination of the digestive tract in colorectal surgery reduces anastomotic leakage and costs: a propensity score analysis. Langenbecks Arch Surg, 2022.
McDermott, F.D., et al., Systematic review of preoperative, intraoperative and postoperative risk factors for colorectal anastomotic leaks. Br J Surg, 2015. 102(5): p. 462-79.
Huisman, D.E., et al., LekCheck: A Prospective Study to Identify Perioperative Modifiable Risk Factors for Anastomotic Leakage in Colorectal Surgery. Ann Surg, 2022. 275(1): p. e189-e197.
Shobar, R.M., et al., The Effects of Bowel Preparation on Microbiota-Related Metrics Differ in Health and in Inflammatory Bowel Disease and for the Mucosal and Luminal Microbiota Compartments. Clin Transl Gastroenterol, 2016. 7: p. e143.
Cong, J., et al., A Pilot Study: Changes of Gut Microbiota in Post-surgery Colorectal Cancer Patients. Front Microbiol, 2018. 9: p. 2777.
Taur, Y., et al., Intestinal domination and the risk of bacteremia in patients undergoing allogeneic hematopoietic stem cell transplantation. Clin Infect Dis, 2012. 55(7): p. 905-14.
Shogan, B.D., et al., Collagen degradation and MMP9 activation by Enterococcus faecalis contribute to intestinal anastomotic leak. Sci Transl Med, 2015. 7(286): p. 286ra68.
Olivas, A.D., et al., Intestinal tissues induce an SNP mutation in Pseudomonas aeruginosa that enhances its virulence: possible role in anastomotic leak. PLoS One, 2012. 7(8): p. e44326.
Gaines, S., et al., Gut microbiome influences on anastomotic leak and recurrence rates following colorectal cancer surgery. Br J Surg, 2018. 105(2): p. e131-e141.
Hyoju, S.K., et al., Oral Polyphosphate Suppresses Bacterial Collagenase Production and Prevents Anastomotic Leak Due to Serratia marcescens and Pseudomonas aeruginosa. Ann Surg, 2018. 267(6): p. 1112-1118.
Shakhsheer, B.A., et al., Morphine Promotes Colonization of Anastomotic Tissues with Collagenase - Producing Enterococcus faecalis and Causes Leak. J Gastrointest Surg, 2016. 20(10): p. 1744-51.
Reuvers, J.R.D., et al., Gut Proteobacteria levels and colorectal surgical infections: SELECT trial. Br J Surg, 2022.
Acknowledgements
Collaborators (alphabetical order)
Members of the SELECT trial study group: G. S. A. Abis1, Y. I. Z. Acherman2, F. C. den Boer3, H. J. Bonjer4, M. van Egmond4, G. Kazemier4, N. de Korte2, S. J. Oosterling2, J. R. D. Reuvers2, J. Scholten2, D. J. A. Sonneveld5, H. B. A. C. Stockmann2, K. van Stralen2, J. B. Tuynman4.
Meander Medisch Centrum, Amersfoort
Spaarne Gasthuis, Haarlem/Hoofddorp
Zaans Medisch Centrum, Zaandam
Amsterdam University Medical Centers, AUMC, Amsterdam
Dijklander Ziekenhuis, Hoorn
Funding
This study was funded by the Dutch Digestive Foundation, Spaarne Gasthuis Academy Fund. The funder had no role in study design, data collection, data analysis, data interpretation or writing of the report.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Disclosure
The authors declare no conflict of interest.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Members of the SELECT trial study group can be found under the heading Collaborators.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Scholten, J., Reuvers, J.R.D., Stockmann, H.B.A.C. et al. Selective Decontamination with Oral Antibiotics in Colorectal Surgery: 90-day Reintervention Rates and Long-term Oncological Follow-up. J Gastrointest Surg 27, 1685–1693 (2023). https://doi.org/10.1007/s11605-023-05746-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-023-05746-1